12 Lower Leg Skin Changes That Reflect Vascular and Circulatory Health
9. Arterial Ulcers - Ischemic Tissue Death
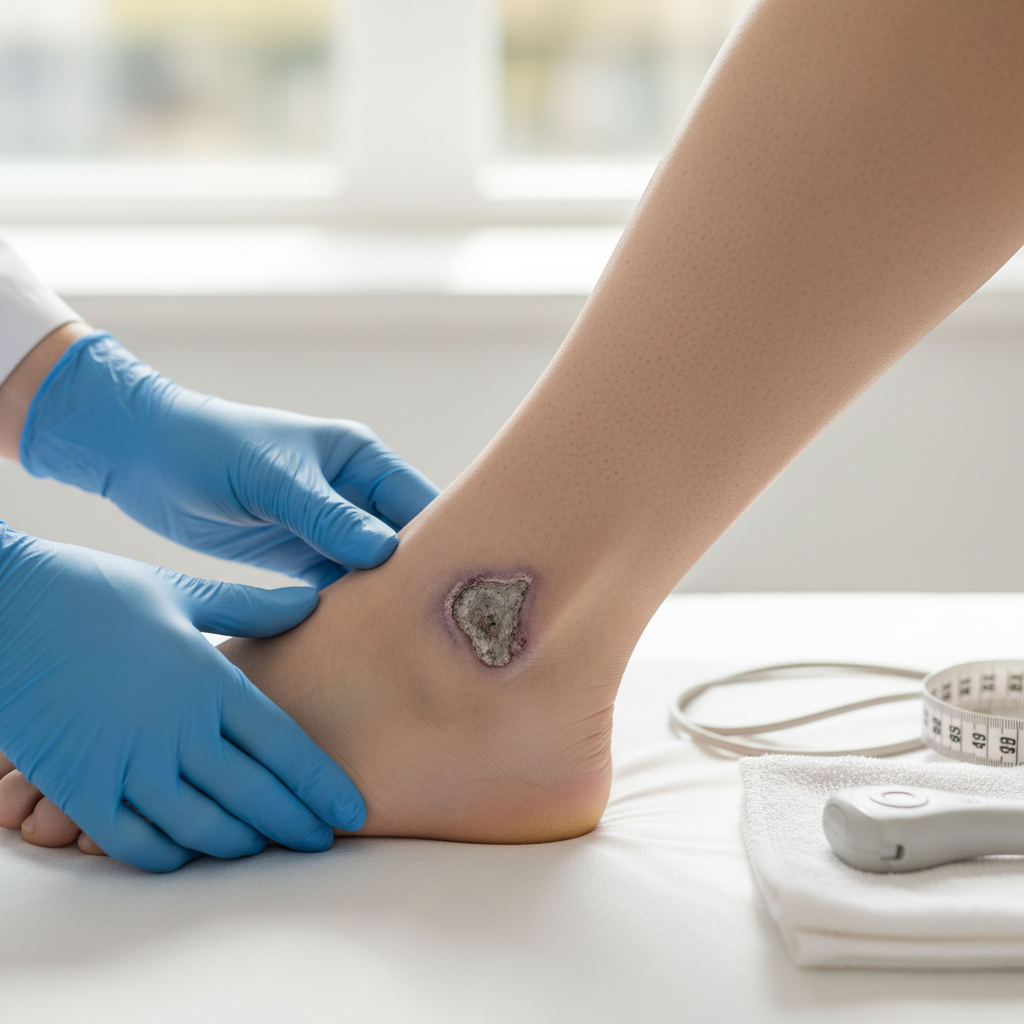
Arterial ulcers develop as a consequence of severe arterial insufficiency where tissue perfusion becomes inadequate to maintain cellular viability, resulting in ischemic necrosis and subsequent ulceration that reflects the critical nature of the underlying vascular compromise. These ulcers typically appear on pressure points such as the toes, heels, and lateral malleoli, where the combination of reduced blood flow and mechanical stress creates conditions conducive to tissue breakdown. Unlike venous ulcers, arterial ulcers characteristically have well-defined, "punched-out" margins with a pale or necrotic base that may contain black eschar, reflecting the ischemic nature of the tissue death. The surrounding skin shows classic signs of arterial insufficiency including pallor, coolness, hair loss, and nail dystrophy, providing important diagnostic clues to the underlying etiology. Pain is a prominent feature of arterial ulcers, often described as severe, constant, and worse at night when cardiac output naturally decreases, leading many patients to sleep with their legs dependent to maximize gravitational assistance to perfusion. The healing capacity of arterial ulcers is severely compromised due to the inadequate blood supply, with many ulcers remaining static or enlarging despite appropriate wound care unless arterial circulation is restored. The development of arterial ulcers indicates critical limb ischemia that requires urgent vascular evaluation and intervention to prevent limb loss. Treatment focuses primarily on revascularization through surgical or endovascular procedures, as topical wound care alone is insufficient when tissue perfusion is critically compromised.