12 Lower Leg Skin Changes That Reflect Vascular and Circulatory Health
10. Mixed Arterial-Venous Ulcers - The Complex Challenge
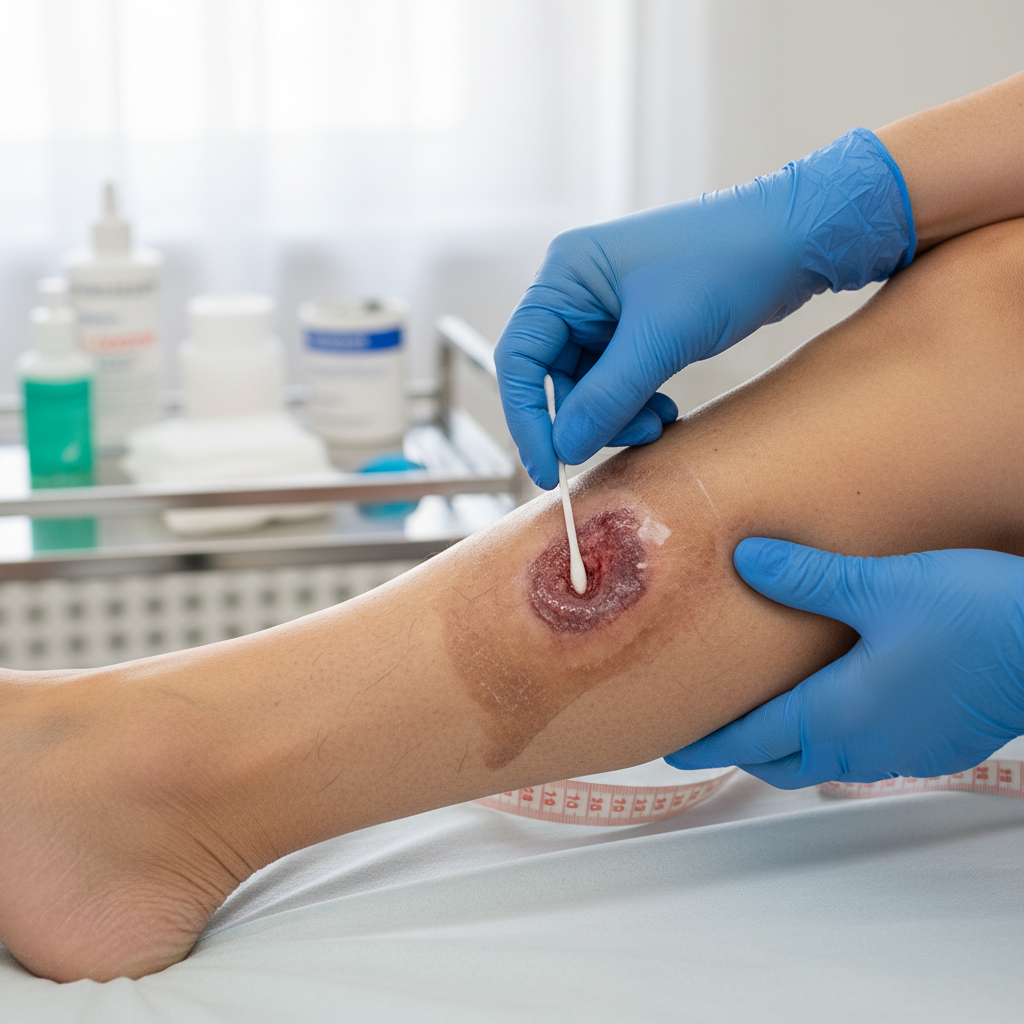
Mixed arterial-venous ulcers present a particularly challenging clinical scenario where both arterial insufficiency and venous disease contribute to ulcer development and impaired healing, creating a complex pathophysiology that requires careful evaluation and nuanced treatment approaches. These ulcers typically occur in patients with long-standing venous disease who have developed concurrent arterial compromise, often related to diabetes, smoking, or advanced age. The clinical presentation combines features of both arterial and venous ulceration, with irregular margins typical of venous disease but with poor granulation tissue and signs of ischemia characteristic of arterial insufficiency. The surrounding skin may show mixed findings including hemosiderin staining and lipodermatosclerosis from venous disease alongside pallor, coolness, and hair loss from arterial compromise. Pain characteristics can be variable, sometimes showing the severe pain typical of arterial ulcers but potentially modified by the presence of venous disease. The diagnostic challenge lies in determining the relative contribution of arterial versus venous pathology, as this significantly impacts treatment decisions, particularly regarding the use of compression therapy which is beneficial for venous disease but potentially harmful in the presence of significant arterial compromise. Ankle-brachial index measurements and additional vascular studies are essential for proper evaluation and treatment planning. Management requires addressing both components of the disease process, often necessitating arterial revascularization before aggressive venous treatment can be safely implemented. The prognosis for mixed ulcers is generally poorer than for pure venous or arterial ulcers, with higher rates of complications and limb loss.