8 Chest Symptom Variations That Differ from Classic Heart Attack Signs
When most people envision a heart attack, they picture the dramatic Hollywood portrayal: a person clutching their chest in excruciating pain before collapsing. However, medical research reveals that cardiac events present with far more complexity and variation than popular culture suggests. While the classic symptoms of crushing chest pain, left arm pain, and shortness of breath remain important warning signs, numerous atypical presentations can signal serious cardiac conditions that require immediate attention. These alternative chest symptoms often masquerade as less serious conditions, leading to delayed diagnosis and treatment. Understanding these variations is crucial because they frequently affect specific populations differently, including women, elderly patients, diabetics, and individuals with certain medical conditions. The chest cavity houses multiple organs and systems beyond the heart, and symptoms originating from cardiac distress can manifest in unexpected ways that don't fit the traditional heart attack narrative. This comprehensive exploration examines eight distinct chest symptom variations that diverge from classic heart attack presentations, providing essential knowledge that could prove life-saving when conventional warning signs are absent or subtle.
1. Silent Chest Pressure - The Subtle Squeeze

Silent chest pressure represents one of the most dangerous variations of cardiac symptoms because it lacks the dramatic intensity typically associated with heart attacks. This condition manifests as a gradual, persistent feeling of heaviness or tightness across the chest that patients often describe as wearing a tight vest or having someone sitting on their chest. Unlike the sharp, stabbing pain of classic presentations, silent chest pressure develops slowly and may fluctuate in intensity throughout the day. Research indicates that this symptom is particularly common among diabetic patients, whose nerve damage can diminish pain sensation, and elderly individuals whose pain perception may be altered by age-related changes. The pressure sensation often extends beyond the traditional left-sided chest pain, potentially affecting the entire chest wall or even presenting primarily on the right side. Patients frequently dismiss this symptom as muscle strain, stress, or indigestion, especially when it occurs without accompanying shortness of breath or sweating. However, studies show that silent chest pressure can indicate significant coronary artery blockages and may precede more obvious cardiac events. The gradual onset and persistent nature of this symptom require careful attention, particularly when it worsens with physical activity or emotional stress and improves with rest.
2. Burning Sensations and Acid-Like Pain

Chest burning sensations present a particularly challenging diagnostic scenario because they closely mimic gastroesophageal reflux disease (GERD) and other gastrointestinal conditions. This cardiac symptom variation manifests as a searing, acid-like pain that typically originates in the central chest and may radiate upward toward the throat or downward toward the stomach. The burning quality often leads patients and even healthcare providers to initially consider digestive causes, potentially delaying crucial cardiac evaluation. Research demonstrates that approximately 30% of patients experiencing cardiac events report burning chest pain as their primary symptom, with the sensation sometimes accompanied by a bitter taste in the mouth or feeling of food stuck in the throat. The pain pattern may worsen after meals or when lying down, further reinforcing the gastrointestinal misinterpretation. However, cardiac-related burning differs from typical heartburn in several key ways: it often occurs with physical exertion, may be accompanied by subtle shortness of breath or fatigue, and typically doesn't respond to antacids or acid-reducing medications. Women are statistically more likely to experience this burning variation compared to men, and the symptom may be more prominent during hormonal fluctuations. The challenge lies in distinguishing between benign digestive burning and potentially life-threatening cardiac burning, requiring careful attention to timing, triggers, and associated symptoms.
3. Sharp, Stabbing Chest Pains

Sharp, stabbing chest pains represent a counterintuitive cardiac symptom that contradicts the common belief that heart-related pain is always dull and crushing. These sudden, knife-like sensations can occur anywhere in the chest and may last from seconds to several minutes before subsiding completely. The intermittent nature of stabbing chest pain often leads patients to dismiss it as muscle strain, especially if it seems to worsen with movement or deep breathing. However, research indicates that certain cardiac conditions, particularly those involving the pericardium (heart's outer lining) or coronary artery spasms, can produce these sharp, piercing sensations. Young adults and individuals with a history of viral infections may be particularly susceptible to pericarditis-related stabbing pain, which often worsens when lying flat and improves when sitting forward. The pain may be accompanied by a friction rub sound audible through a stethoscope, though patients themselves rarely detect this. Coronary artery spasms, another cause of stabbing chest pain, can occur even in individuals with relatively healthy coronary arteries and may be triggered by stress, cold exposure, or certain medications. The challenge with stabbing chest pain lies in its similarity to musculoskeletal conditions, lung problems, or even anxiety-related symptoms. However, when stabbing pain occurs repeatedly, is associated with exertion, or is accompanied by other cardiac symptoms like palpitations or lightheadedness, it warrants immediate medical evaluation.
4. Chest Tightness Without Pain
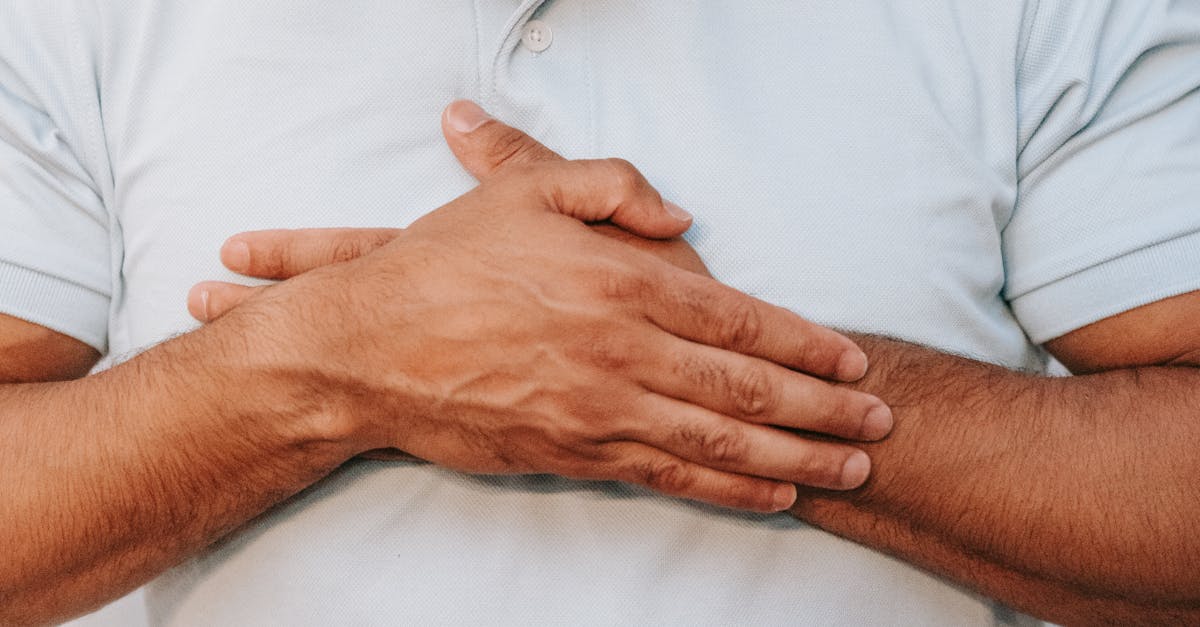
Chest tightness without accompanying pain presents a subtle but significant cardiac symptom that many patients struggle to articulate effectively to healthcare providers. This sensation is often described as feeling like the chest is being squeezed in a vice, wrapped tightly with bandages, or compressed from the inside, yet without the sharp or aching pain typically associated with cardiac events. The absence of pain can be particularly misleading, as patients may not recognize the severity of their condition or may attribute the sensation to anxiety, asthma, or physical fitness issues. Research shows that chest tightness is frequently reported by women experiencing cardiac events, and it may be the predominant symptom in up to 40% of female heart attack patients. The tightness often develops gradually and may be accompanied by a feeling of breathlessness or the inability to take a deep, satisfying breath. Unlike anxiety-related chest tightness, cardiac-origin tightness typically correlates with physical exertion and may be accompanied by subtle fatigue or a sense of impending doom. The symptom may also present with radiation patterns, extending to the shoulders, back, or jaw, though patients may not initially connect these sensations to their chest tightness. Athletes and physically active individuals may be particularly prone to dismissing chest tightness as exercise-related muscle tension, potentially delaying critical diagnosis and treatment of underlying cardiac conditions.
5. Chest Fluttering and Palpitation-Related Discomfort

Chest fluttering and palpitation-related discomfort represent cardiac symptoms that patients often describe as feeling like butterflies, fish flopping, or hummingbirds trapped within their chest cavity. These sensations stem from irregular heart rhythms or arrhythmias that can range from benign to life-threatening, making proper evaluation crucial. The fluttering sensation may be accompanied by a feeling of the heart skipping beats, racing unexpectedly, or beating so hard that it seems to shake the entire chest wall. Research indicates that while many palpitations are harmless, those accompanied by chest discomfort, shortness of breath, or lightheadedness may signal serious cardiac conditions requiring immediate attention. The timing and triggers of chest fluttering provide important diagnostic clues: symptoms occurring with caffeine consumption or stress may indicate different conditions than those appearing during rest or sleep. Some patients experience a combination of fluttering and chest pressure, creating a unique symptom complex that doesn't fit typical heart attack presentations but may indicate conditions like atrial fibrillation, ventricular tachycardia, or coronary artery disease. The sensation may be intermittent, lasting only seconds, or sustained for hours, with the duration and frequency helping healthcare providers determine the underlying cause. Young adults may experience chest fluttering related to structural heart abnormalities, while older patients may develop these symptoms secondary to coronary artery disease or heart failure, emphasizing the importance of age-appropriate evaluation and treatment strategies.
6. Chest Numbness and Tingling Sensations
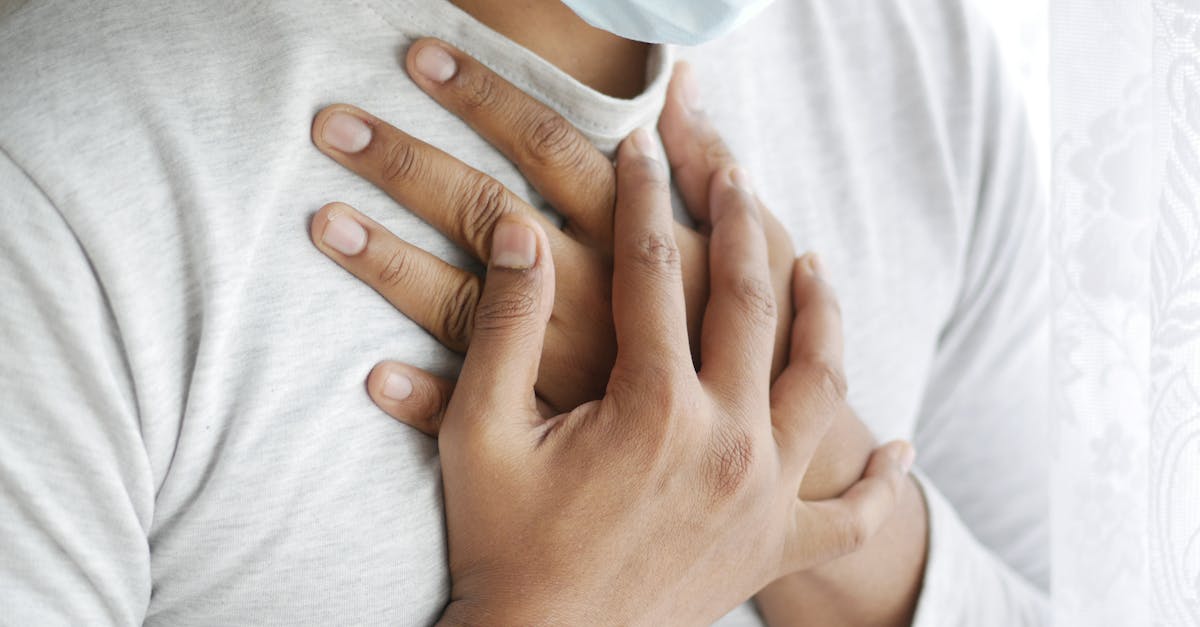
Chest numbness and tingling sensations represent an often-overlooked category of cardiac symptoms that patients may dismiss as nerve-related or musculoskeletal in origin. These sensations can manifest as areas of decreased feeling across the chest wall, pins-and-needles sensations similar to a limb "falling asleep," or electric-like tingling that may come and go unpredictably. The numbness may be localized to specific areas of the chest or may involve larger regions, sometimes extending to the arms, shoulders, or upper back. Research suggests that chest numbness can occur in conjunction with reduced blood flow to the heart muscle, particularly in cases where smaller coronary arteries are affected or when circulation is compromised by conditions like diabetes or peripheral vascular disease. The tingling component often results from nerve irritation caused by inflammation around the heart or changes in blood chemistry during cardiac stress. Patients with diabetes are particularly susceptible to these sensations due to their increased risk of both cardiac disease and neuropathy, making it challenging to distinguish between diabetic nerve damage and cardiac-related symptoms. The numbness may be accompanied by weakness in the chest muscles or difficulty with fine motor control in the hands and arms. Unlike typical heart attack pain, these sensations may persist for extended periods and may not correlate directly with physical activity, though they often worsen during times of cardiac stress or when circulation is further compromised by position changes or environmental factors.
7. Chest Heaviness and Fatigue-Related Symptoms

Chest heaviness combined with overwhelming fatigue represents a particularly insidious cardiac symptom complex that often develops gradually over days or weeks, making it easy to attribute to stress, aging, or general health decline. This symptom variation manifests as a persistent feeling of weight or burden in the chest, as if carrying heavy objects, combined with unusual tiredness that doesn't improve with rest. The heaviness may be most noticeable during routine activities that previously caused no discomfort, such as climbing stairs, carrying groceries, or even walking short distances. Research indicates that this symptom combination is frequently the primary presentation of heart failure, coronary artery disease, or cardiomyopathy, particularly in older adults and individuals with multiple cardiovascular risk factors. The fatigue component often extends beyond normal tiredness, affecting cognitive function, motivation, and the ability to perform daily activities. Patients may notice that they need to rest more frequently during routine tasks or that they feel exhausted after minimal exertion. The chest heaviness may fluctuate throughout the day, often worsening in the evening or after periods of activity, and may be accompanied by subtle swelling in the legs or ankles. Women are more likely to experience this symptom complex compared to men, and it may be particularly prominent in the weeks following what appears to be a minor illness or during periods of emotional stress. The gradual onset and non-specific nature of these symptoms often lead to delayed medical evaluation, emphasizing the importance of recognizing this pattern as potentially cardiac in origin.
8. Temperature-Related Chest Sensations
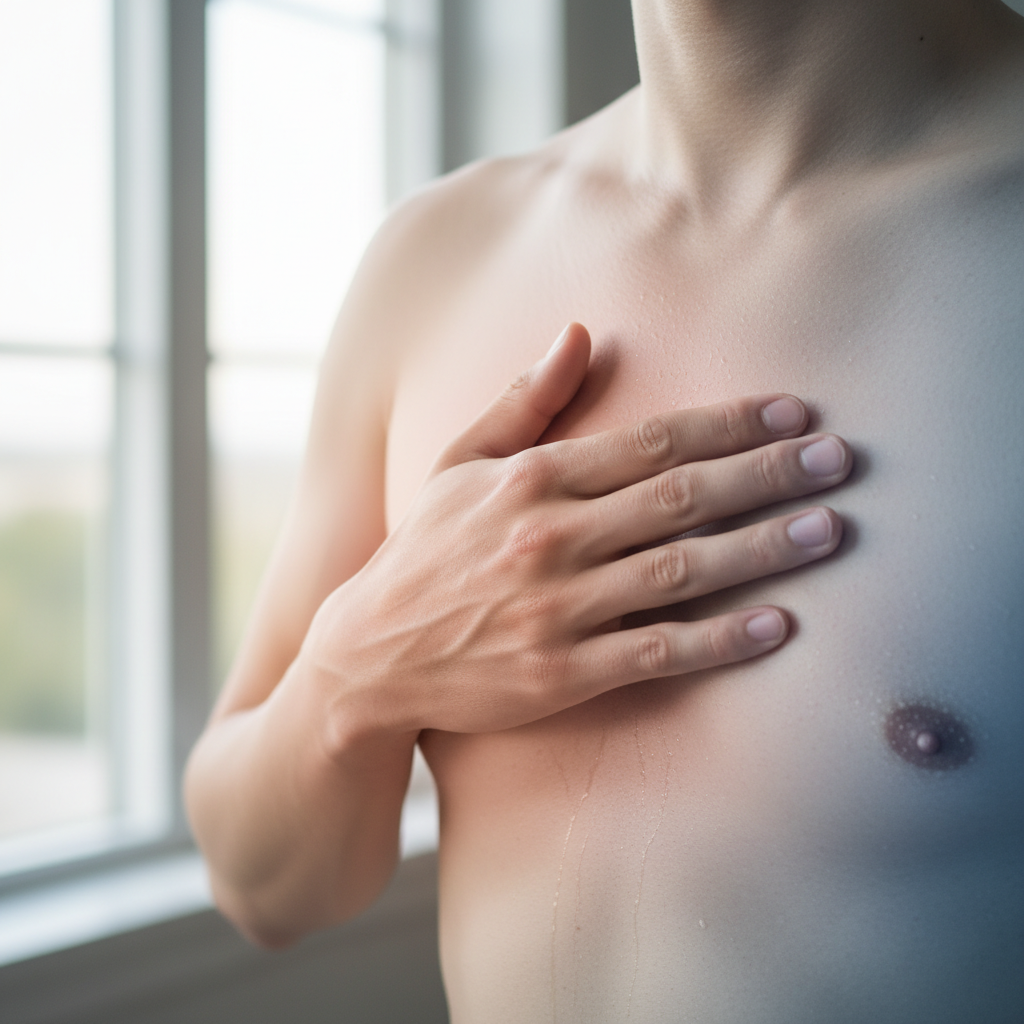
Temperature-related chest sensations encompass a range of unusual thermal experiences that can signal cardiac distress, including feelings of intense heat, cold, or alternating temperature changes within the chest cavity. These sensations often puzzle patients because they don't align with typical expectations of cardiac symptoms, leading to misinterpretation as fever, anxiety, or environmental factors. The heat sensation may manifest as a burning warmth that spreads across the chest, distinct from the acid-like burning associated with reflux-type symptoms, and may be accompanied by actual skin warmth or flushing. Conversely, some patients experience intense cold sensations in the chest, describing feelings of ice water flowing through their chest or a deep, penetrating chill that doesn't respond to external warming. Research suggests that these temperature sensations may result from changes in blood flow patterns, inflammatory responses around the heart, or autonomic nervous system dysfunction during cardiac stress. The alternating hot and cold sensations may occur in waves, sometimes correlating with heart rhythm changes or blood pressure fluctuations. These symptoms are particularly common in patients experiencing unstable angina or during the early phases of heart attack, when blood flow to the heart muscle is intermittently compromised. The temperature sensations may be accompanied by sweating, chills, or skin color changes, providing additional clues to their cardiac origin. Patients with diabetes or peripheral vascular disease may be more susceptible to these temperature-related symptoms due to their altered circulation and nerve function, making recognition and proper evaluation crucial for timely intervention.
9. Recognizing the Full Spectrum of Cardiac Symptoms

The exploration of these eight chest symptom variations reveals the complex and often misleading nature of cardiac presentations that diverge from classic heart attack signs. Understanding this broader spectrum of symptoms is essential for both patients and healthcare providers, as early recognition and intervention can significantly impact outcomes in cardiac emergencies. The subtle nature of many atypical symptoms means that individuals must become more attuned to their bodies and more willing to seek medical evaluation for seemingly minor or unusual chest sensations, particularly when they occur in patterns or are accompanied by other concerning signs. Healthcare systems must also adapt to recognize these variations, ensuring that emergency departments, primary care providers, and urgent care facilities are equipped to evaluate and respond appropriately to non-traditional cardiac presentations. The demographic variations in symptom presentation highlight the importance of personalized medicine approaches, with particular attention to how age, gender, diabetes status, and other medical conditions influence symptom manifestation. Education and awareness campaigns should expand beyond traditional heart attack symptoms to include these atypical presentations, potentially saving lives by encouraging earlier medical intervention. As medical research continues to refine our understanding of cardiac symptom variations, the integration of this knowledge into clinical practice and public health education becomes increasingly critical for improving cardiovascular outcomes across diverse patient populations.