12 Skin Itching Patterns That Correspond to Liver, Kidney, and Blood Disorders
The human skin serves as a remarkable diagnostic window into the body's internal health, particularly when it comes to itching patterns that may signal underlying liver, kidney, and blood disorders. Medical professionals have long recognized that pruritus, or chronic itching, often represents more than just a superficial skin condition—it can be a crucial early warning system for serious systemic diseases. When the liver struggles to process toxins, the kidneys fail to filter waste products effectively, or blood disorders disrupt normal cellular function, the skin frequently responds with distinctive itching patterns that trained healthcare providers can interpret like a medical roadmap. These patterns range from generalized itching without visible rash to specific regional distributions that correlate with particular organ dysfunctions. Understanding these connections between skin symptoms and internal organ health has revolutionized diagnostic approaches in modern medicine, allowing for earlier detection and treatment of potentially life-threatening conditions. The following exploration will examine twelve specific itching patterns that serve as reliable indicators of liver dysfunction, kidney disease, and various blood disorders, providing both medical professionals and patients with valuable insights into the body's interconnected warning systems.
1. Cholestatic Pruritus - The Liver's Distress Signal
Cholestatic pruritus represents one of the most distinctive and well-documented forms of itching associated with liver dysfunction, occurring when bile acids accumulate in the bloodstream due to impaired bile flow. This condition typically manifests as intense, generalized itching that begins on the palms and soles before spreading throughout the body, often becoming more severe during nighttime hours when patients attempt to rest. The underlying mechanism involves elevated levels of bile salts that deposit in skin tissues, triggering inflammatory responses and activating itch-sensitive nerve fibers. Patients with primary biliary cholangitis, primary sclerosing cholangitis, or drug-induced cholestasis frequently experience this debilitating symptom, which can significantly impact quality of life and sleep patterns. The itching associated with cholestatic conditions is characteristically described as deep, burning, and impossible to satisfy through scratching, often leading to secondary skin damage from persistent scratching attempts. Laboratory findings typically reveal elevated alkaline phosphatase, gamma-glutamyl transferase, and direct bilirubin levels, confirming the cholestatic nature of the liver dysfunction. Treatment approaches focus on addressing the underlying bile flow obstruction while providing symptomatic relief through bile acid sequestrants, rifampicin, or specialized anti-pruritic medications that target the specific pathways involved in cholestatic itching.
2. Uremic Pruritus - Kidney Failure's Uncomfortable Warning

Uremic pruritus affects approximately 80% of patients with chronic kidney disease, representing a complex syndrome that emerges when the kidneys can no longer effectively filter metabolic waste products from the bloodstream. This condition typically develops when kidney function declines below 30% of normal capacity, causing uremic toxins to accumulate in tissues and trigger inflammatory cascades that stimulate itch receptors throughout the skin. The itching pattern in uremic pruritus is characteristically generalized but often shows predilection for the back, abdomen, and extremities, with many patients reporting that the sensation feels like "crawling insects" beneath the skin surface. Unlike other forms of pruritus, uremic itching tends to be more severe during dialysis sessions and immediately afterward, as rapid fluid and electrolyte shifts can temporarily worsen the inflammatory response. The pathophysiology involves multiple mechanisms including elevated phosphorus levels, secondary hyperparathyroidism, chronic inflammation, and accumulation of middle molecular weight toxins that normal kidneys would eliminate. Patients often develop characteristic scratch marks and lichenification from chronic scratching, particularly on easily accessible areas like the arms and legs. Management strategies include optimizing dialysis adequacy, controlling phosphorus levels through dietary restrictions and phosphate binders, addressing secondary hyperparathyroidism with vitamin D analogs, and utilizing targeted anti-pruritic therapies such as gabapentin or topical capsaicin preparations.
3. Polycythemia Vera Aquagenic Pruritus - Blood Disorder's Unique Signature
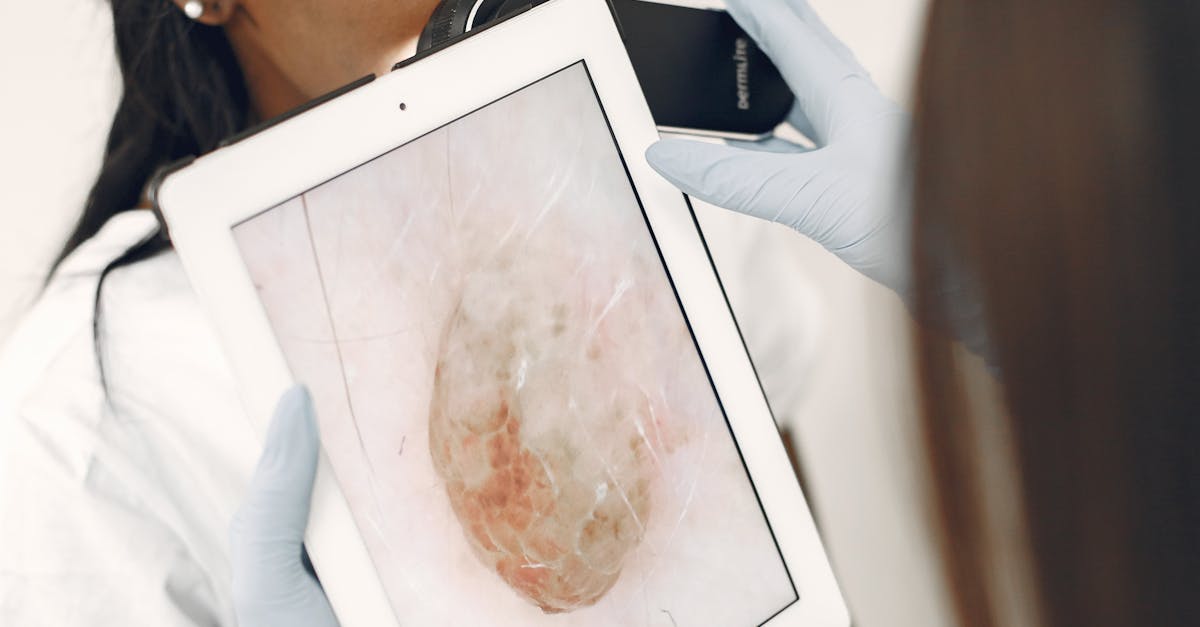
Aquagenic pruritus associated with polycythemia vera represents one of the most specific and diagnostically valuable itching patterns in hematologic medicine, occurring in approximately 70% of patients with this myeloproliferative disorder. This distinctive condition manifests as intense, burning, or prickling sensations that develop within minutes of contact with water of any temperature, typically lasting 30-60 minutes after water exposure ends. The underlying mechanism involves abnormal histamine release from increased numbers of basophils and mast cells, which are characteristic features of polycythemia vera's altered blood cell production. Patients often describe the sensation as feeling like "needles and pins" or "electric shocks" spreading across water-exposed skin areas, leading many to avoid bathing, swimming, or even washing dishes. The itching pattern is remarkably consistent and reproducible, making it an important diagnostic clue when evaluating patients with unexplained pruritus. Laboratory investigations typically reveal elevated hematocrit levels, increased red blood cell mass, and often accompanying thrombocytosis or leukocytosis. The JAK2 V617F mutation, present in over 95% of polycythemia vera cases, provides molecular confirmation of the diagnosis when aquagenic pruritus is present. Treatment approaches include therapeutic phlebotomy to reduce blood viscosity, hydroxyurea to control cell proliferation, and antihistamines or selective serotonin reuptake inhibitors to manage the pruritic symptoms, with many patients experiencing significant improvement once the underlying blood disorder is adequately controlled.
4. Hepatitis C-Associated Cryoglobulinemic Vasculitis Itching
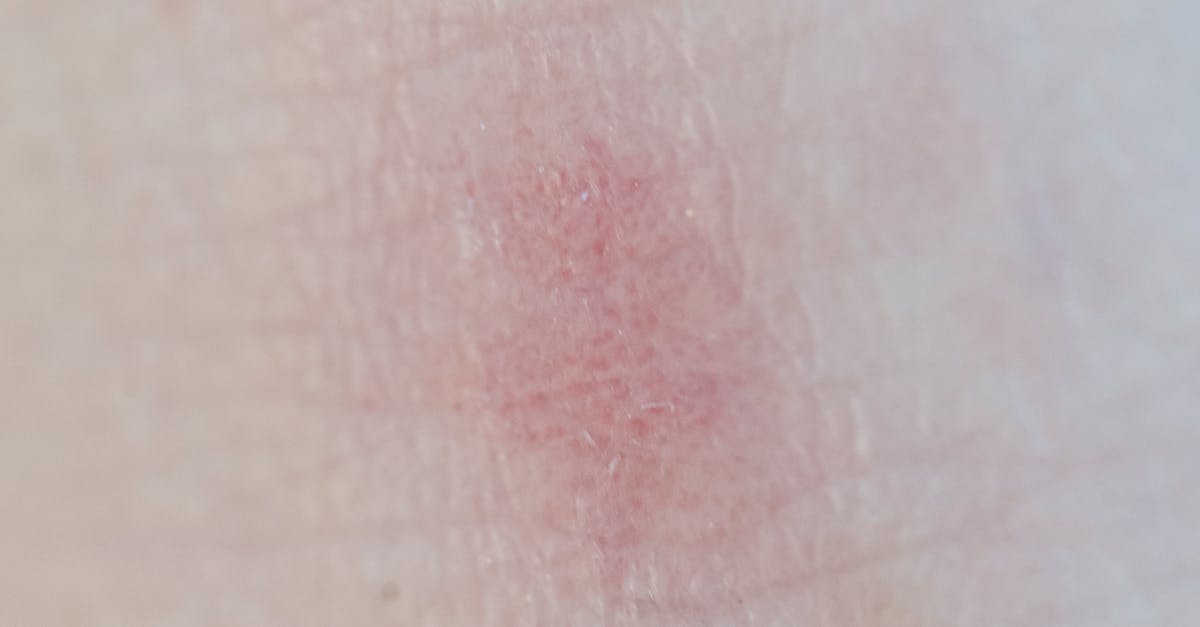
Hepatitis C virus infection can trigger a unique form of itching through the development of mixed cryoglobulinemia, a condition where abnormal proteins precipitate in cold temperatures and cause small vessel inflammation throughout the body. This particular itching pattern typically affects the lower extremities initially, presenting as intense pruritus associated with palpable purpura, skin ulcerations, and sometimes livedo reticularis in a distinctive reticular pattern. The pathophysiology involves immune complex formation between hepatitis C viral antigens and host antibodies, creating cryoglobulins that deposit in small blood vessels and activate complement cascades, leading to vasculitic inflammation and associated neurogenic itching. Patients often report that the itching worsens with cold exposure and improves in warm environments, reflecting the temperature-dependent nature of cryoglobulin precipitation. The condition affects approximately 40-60% of patients with chronic hepatitis C infection, though symptomatic cryoglobulinemia develops in only 5-10% of cases. Diagnosis requires demonstration of serum cryoglobulins, often accompanied by low complement levels, positive rheumatoid factor, and evidence of hepatitis C viral replication. The itching associated with this condition is particularly challenging to treat because it stems from both viral-induced liver inflammation and immune-mediated vascular damage. Effective management typically requires antiviral therapy to eliminate hepatitis C virus, immunosuppressive medications to control the vasculitic component, and symptomatic treatments including topical corticosteroids and systemic antihistamines to address the persistent pruritic symptoms.
5. Iron Deficiency Anemia Restless Leg Syndrome Itching

Iron deficiency anemia can manifest with a distinctive pattern of itching and uncomfortable sensations primarily affecting the lower extremities, often overlapping with restless leg syndrome in a condition that significantly impacts sleep quality and daily functioning. This form of pruritus typically presents as deep, aching, crawling sensations in the legs that worsen during periods of rest and improve with movement, creating an irresistible urge to move or scratch the affected areas. The underlying mechanism involves iron's crucial role in dopamine synthesis and neuronal function, with iron deficiency leading to altered neurotransmitter metabolism in brain regions responsible for motor control and sensory processing. Patients frequently describe the sensation as "bugs crawling under the skin" or "electric currents" running through their legs, with symptoms typically worsening in the evening and nighttime hours. The condition affects approximately 25% of individuals with iron deficiency anemia, particularly women of reproductive age who experience heavy menstrual bleeding or individuals with chronic gastrointestinal blood loss. Laboratory findings reveal low serum iron, decreased ferritin levels, elevated total iron-binding capacity, and characteristic microcytic, hypochromic red blood cells on peripheral blood smear examination. The itching pattern often shows a clear circadian rhythm, with minimal symptoms during morning hours and progressive worsening throughout the day, reaching peak intensity during attempted sleep periods. Treatment focuses on iron replacement therapy through oral or intravenous supplementation, dietary modifications to enhance iron absorption, and identification of underlying causes of iron loss, with most patients experiencing significant symptom improvement within 4-6 weeks of achieving adequate iron repletion.
6. Primary Biliary Cholangitis Palmoplantar Pruritus
Primary biliary cholangitis, an autoimmune liver disease primarily affecting middle-aged women, produces a characteristic itching pattern that begins specifically on the palms and soles before progressing to generalized pruritus throughout the body. This distinctive distribution pattern occurs because palmoplantar skin contains higher concentrations of bile acid receptors and has increased sensitivity to circulating pruritogenic substances that accumulate when intrahepatic bile ducts become progressively destroyed. The itching typically starts as mild irritation during early disease stages but can progress to severe, debilitating pruritus that significantly impacts sleep, work productivity, and overall quality of life as the condition advances. Patients often describe the sensation as deep, burning discomfort that cannot be relieved through conventional scratching, leading to secondary skin changes including excoriation, lichenification, and sometimes bacterial superinfection from persistent manipulation. The palmoplantar predilection is so characteristic that its presence in a middle-aged woman with elevated alkaline phosphatase levels should prompt immediate evaluation for primary biliary cholangitis through antimitochondrial antibody testing and liver biopsy if indicated. The severity of itching often correlates with disease progression and can serve as an important clinical marker for monitoring treatment response and disease activity over time. Histological examination reveals characteristic florid duct lesions with lymphocytic infiltration and progressive bile duct destruction, confirming the autoimmune nature of the condition. Management strategies include ursodeoxycholic acid as first-line therapy to improve bile flow, obeticholic acid for patients with inadequate response, and symptomatic treatments such as cholestyramine, rifampicin, or naltrexone to address the persistent pruritic symptoms that can dominate the clinical presentation.
7. Chronic Kidney Disease Mineral Bone Disorder Itching
Chronic kidney disease mineral bone disorder represents a complex syndrome that includes distinctive itching patterns related to disturbed calcium, phosphorus, and parathyroid hormone metabolism that occurs as kidney function progressively declines. This condition typically manifests as generalized pruritus with particular intensity over bony prominences such as the spine, shoulders, and hips, where altered mineral metabolism most significantly affects underlying bone and soft tissue structures. The pathophysiology involves multiple interconnected mechanisms including elevated serum phosphorus levels that deposit in skin tissues, secondary hyperparathyroidism causing increased calcium-phosphorus product precipitation, and chronic inflammation from uremic toxin accumulation. Patients often report that the itching has a deep, aching quality that seems to emanate from beneath the skin surface, making it particularly difficult to obtain relief through topical treatments or superficial scratching. The condition affects approximately 60-90% of patients with stage 4-5 chronic kidney disease, with severity often correlating with degree of mineral metabolism disturbance rather than absolute kidney function levels. Laboratory abnormalities typically include elevated serum phosphorus, inappropriately normal or low serum calcium, markedly elevated parathyroid hormone levels, and decreased 25-hydroxyvitamin D concentrations. The itching pattern often shows temporal relationships with dietary phosphorus intake and dialysis schedules in patients receiving renal replacement therapy, with many experiencing temporary relief following effective dialysis sessions. Treatment approaches focus on controlling serum phosphorus through dietary restriction and phosphate binders, managing secondary hyperparathyroidism with vitamin D analogs or calcimimetics, optimizing dialysis adequacy, and utilizing targeted anti-pruritic medications such as gabapentin or pregabalin that address the neuropathic component of uremic itching.
8. Hodgkin Lymphoma Paraneoplastic Pruritus

Hodgkin lymphoma frequently presents with a distinctive paraneoplastic pruritus that can precede other clinical manifestations by months or even years, making it an important early diagnostic clue in the evaluation of unexplained chronic itching. This condition typically manifests as intense, generalized itching without primary skin lesions, often described by patients as burning or stinging sensations that worsen at night and can be triggered by alcohol consumption or heat exposure. The underlying mechanism involves cytokine release from malignant Reed-Sternberg cells and reactive inflammatory cells within lymph nodes, particularly interleukin-31, which directly activates itch-specific sensory neurons throughout the skin. Patients frequently report that the itching has an unusual quality that differs from common skin conditions, often describing it as originating from deep within tissues rather than from the skin surface itself. The pruritus associated with Hodgkin lymphoma affects approximately 30% of patients at diagnosis and can be so severe that it leads to sleep deprivation, depression, and significant functional impairment before the underlying malignancy is identified. The itching pattern often shows a characteristic response to alcohol consumption, with many patients experiencing immediate worsening of symptoms after drinking even small amounts of alcoholic beverages, a phenomenon known as alcohol-induced pain or pruritus. Diagnosis requires comprehensive evaluation including detailed physical examination for lymphadenopathy, computed tomography imaging of chest, abdomen, and pelvis, and ultimately lymph node biopsy to identify characteristic Reed-Sternberg cells and determine specific Hodgkin lymphoma subtype. Treatment of the underlying lymphoma with combination chemotherapy or radiation therapy typically results in complete resolution of the paraneoplastic pruritus, though symptomatic management with antihistamines, topical corticosteroids, or systemic immunomodulators may be necessary during the treatment period.
9. Autoimmune Hepatitis Systemic Pruritus
Autoimmune hepatitis can produce a distinctive pattern of systemic pruritus that reflects the complex interplay between liver inflammation, immune system dysfunction, and altered bile acid metabolism characteristic of this chronic inflammatory liver disease. This condition typically presents as generalized itching that may fluctuate in intensity corresponding to periods of disease activity, often accompanied by fatigue, joint pain, and other systemic symptoms that reflect the autoimmune nature of the underlying condition. The pathophysiology involves multiple mechanisms including direct hepatocellular damage from autoimmune inflammation, altered bile acid synthesis and transport, and systemic release of inflammatory mediators that can sensitize peripheral itch receptors throughout the body. Patients often describe the itching as having a burning or tingling quality that can be particularly bothersome during disease flares, when liver inflammation is most active and systemic symptoms are most pronounced. The condition predominantly affects young women and can present with either acute hepatitis-like symptoms or insidious onset of chronic liver disease, with pruritus being reported in approximately 20-30% of cases at initial presentation. Laboratory findings typically reveal elevated aminotransferases, hypergammaglobulinemia, and positive autoantibodies including antinuclear antibodies, anti-smooth muscle antibodies, or anti-liver kidney microsome antibodies depending on the specific autoimmune hepatitis subtype. The severity of itching often correlates with degree of liver inflammation as measured by aminotransferase levels and histological activity scores on liver biopsy examination. Treatment with immunosuppressive therapy including corticosteroids and azathioprine typically results in improvement of both liver inflammation and associated pruritic symptoms, though symptomatic management may be necessary during the initial treatment period while waiting for immunosuppression to take effect.
10. Thrombocythemia Essential Erythromelalgia Itching
Essential thrombocythemia, a myeloproliferative disorder characterized by excessive platelet production, can manifest with a unique form of itching associated with erythromelalgia, a condition involving painful, red, warm extremities that burn and itch intensely. This distinctive syndrome typically affects the hands and feet, presenting as episodes of severe burning pain accompanied by intense itching, erythema, and increased skin temperature that can last from minutes to hours. The underlying mechanism involves abnormal platelet aggregation in small blood vessels, leading to microvascular occlusion, inflammation, and activation of pain and itch receptors in affected tissues. Patients often describe the sensation as feeling like their hands or feet are "on fire" with accompanying intense itching that cannot be relieved through conventional means, often requiring cooling measures such as cold water immersion for symptomatic relief. The condition affects approximately 25-30% of patients with essential thrombocythemia and can be one of the presenting symptoms that leads to diagnosis of the underlying blood disorder. Episodes are frequently triggered by heat exposure, exercise, or prolonged standing, and characteristically improve with cooling and elevation of affected extremities. Laboratory evaluation reveals markedly elevated platelet counts, often exceeding 600,000-800,000 per microliter, along with evidence of abnormal platelet function studies and frequently the presence of JAK2, CALR, or MPL gene mutations that confirm the myeloproliferative nature of the disorder. The itching and burning associated with erythromelalgia can be particularly challenging to treat because conventional antihistamines and topical preparations are generally ineffective against this microvascular-mediated symptom complex. Management approaches include platelet reduction therapy with hydroxyurea or anagrelide, low-dose aspirin to prevent platelet aggregation, and symptomatic treatments such as cooling measures, topical anesthetics, or systemic medications including gabap