12 Pain Referral Patterns the Body Uses as Warning Signals
The human body operates as an intricate communication network, where pain serves as a sophisticated alarm system designed to protect us from harm and signal underlying dysfunction. Pain referral patterns represent one of the most fascinating aspects of this biological warning system, where discomfort manifests in locations distant from the actual source of injury or disease. This phenomenon occurs because our nervous system processes sensory information through complex pathways that can create misleading signals, causing us to feel pain in areas that may seem completely unrelated to the underlying problem. Understanding these referral patterns is crucial for both healthcare professionals and individuals seeking to interpret their body's warning signals accurately. The convergence of nerve pathways, shared embryological origins of tissues, and the interconnected nature of our fascial and muscular systems all contribute to these sometimes puzzling pain presentations. From the classic example of heart attack pain radiating to the left arm, to the lesser-known phenomenon of gallbladder pain presenting as right shoulder discomfort, these patterns have evolved as part of our body's ancient warning mechanisms. By recognizing and understanding twelve key pain referral patterns, we can better decode what our bodies are trying to tell us and respond more effectively to potential health threats before they become serious complications.
1. Cardiac Pain Referral - When the Heart Speaks Through the Arm
The most well-documented and clinically significant pain referral pattern involves cardiac issues manifesting as discomfort in the left arm, jaw, neck, or even the back. This phenomenon occurs because the heart and these distant areas share similar nerve pathways through the sympathetic nervous system, specifically through the cardiac plexus and the upper thoracic sympathetic chain. During a myocardial infarction or angina episode, the heart's distress signals travel along these shared neural highways, creating the sensation of pain in areas far removed from the actual cardiac tissue. The left arm is particularly common because both the heart and the left upper extremity receive innervation from the same spinal cord segments (T1-T5), causing the brain to misinterpret the source of the painful stimulus. This referral pattern serves as a crucial early warning system, often alerting individuals to cardiac problems before more obvious symptoms like chest pain become apparent. Women, in particular, may experience atypical cardiac symptoms with pain referring to the jaw, back, or right arm rather than the classic left arm presentation. Understanding this pattern has saved countless lives by encouraging people to seek immediate medical attention when experiencing unexplained arm or jaw pain, especially when accompanied by other cardiac risk factors. The evolutionary advantage of this referral system likely stems from the need to create unmistakable warning signals that would prompt immediate behavioral changes to protect the vital cardiac muscle from further damage.
2. Gallbladder Pain Referral - The Right Shoulder Connection
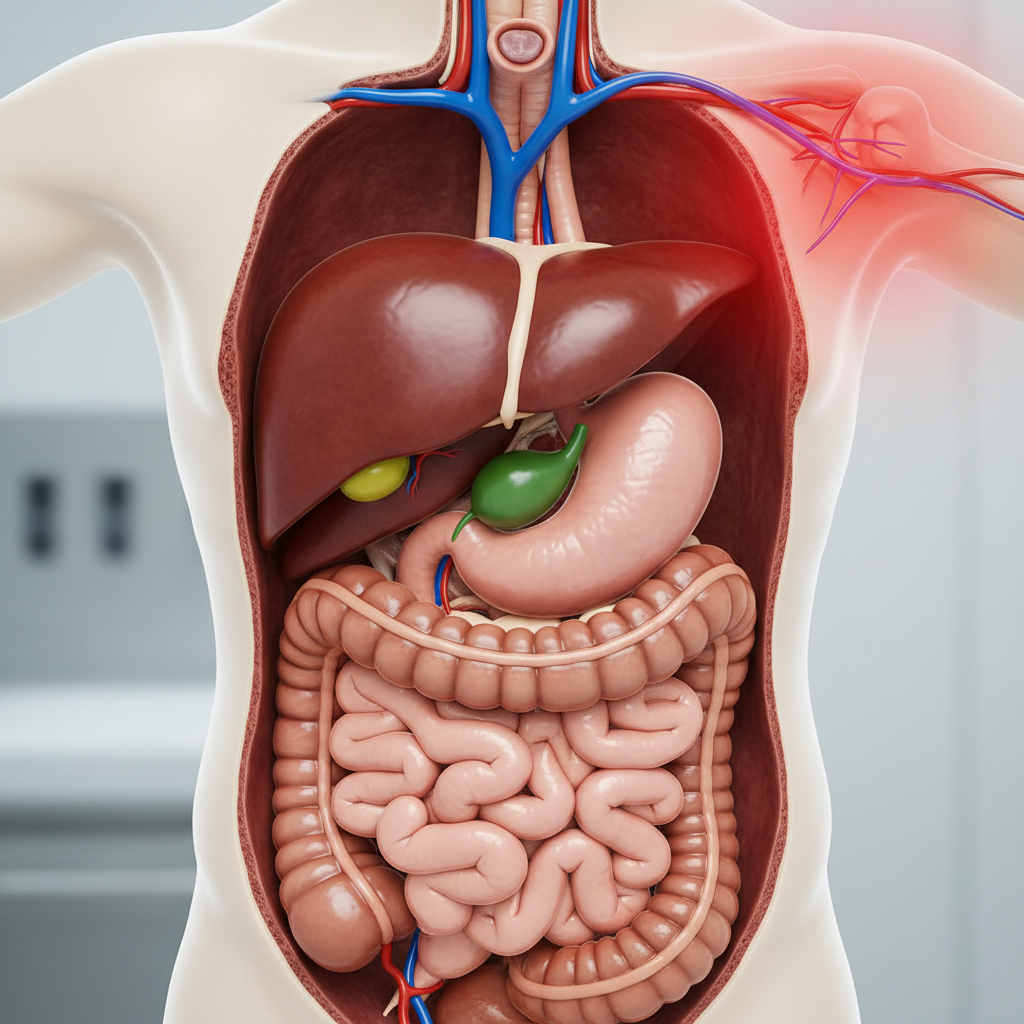
The gallbladder's pain referral pattern to the right shoulder and scapular region represents one of the most consistent and diagnostically valuable examples of visceral referred pain. This phenomenon occurs through the phrenic nerve pathway, where the gallbladder shares sensory innervation with the diaphragm via the celiac plexus, and the diaphragm's phrenic nerve (C3-C5) also supplies sensory fibers to the shoulder region. When the gallbladder becomes inflamed, distended, or obstructed by stones, the resulting visceral pain signals travel along these shared neural pathways, creating the characteristic right shoulder blade pain that many patients describe as a deep, aching sensation. This referral pattern is so reliable that healthcare providers often use right shoulder pain as a key diagnostic indicator when evaluating patients for cholecystitis or cholelithiasis. The pain typically intensifies after consuming fatty meals, as the gallbladder contracts more vigorously to release bile for fat digestion, increasing pressure within an already compromised organ. Patients frequently describe the shoulder pain as more bothersome than any abdominal discomfort, leading some to initially seek treatment for what they assume is a musculoskeletal shoulder problem. This referral mechanism serves as an early warning system, alerting individuals to gallbladder dysfunction before more serious complications like perforation or pancreatitis can develop. The consistency of this pattern across different populations suggests it represents a fundamental aspect of human neuroanatomy that has remained unchanged throughout our evolutionary history.
3. Kidney Stone Pain Referral - The Flank to Groin Journey
Kidney stone pain follows a distinctive referral pattern that traces the anatomical course of the ureter, creating a characteristic pain pathway from the flank to the groin that serves as a reliable diagnostic indicator. This referral occurs because the ureters, kidneys, and associated structures share sensory innervation through the renal plexus and sympathetic fibers from T10-L1 spinal segments, which also supply sensation to the skin and muscles along the lateral abdomen, groin, and inner thigh. As a kidney stone travels down the ureter, the pain referral pattern typically follows this anatomical journey, beginning in the costovertebral angle and radiating anteriorly around the flank, then descending toward the inguinal region and sometimes extending into the testicles in men or labia in women. The intensity and location of the referred pain often correlate with the stone's position within the ureter, providing healthcare providers with valuable information about the stone's likely location and progression. This pain is typically described as excruciating and colicky, coming in waves that correspond to ureteral contractions attempting to move the obstructing stone. The referral pattern serves multiple biological purposes: it creates an unmistakable warning signal that demands immediate attention, helps localize the problem for potential medical intervention, and may even influence behavior in ways that could facilitate stone passage, such as increased fluid intake and movement. Understanding this referral pattern helps distinguish kidney stone pain from other conditions like appendicitis, ovarian cysts, or musculoskeletal problems that might present with similar regional discomfort.
4. Liver Pain Referral - The Right Shoulder and Back Signal
The liver's pain referral pattern primarily manifests in the right shoulder, right scapular region, and sometimes the right side of the neck, creating a diagnostic signature that reflects the organ's extensive neural connections and embryological development. This referral occurs through the hepatic plexus and phrenic nerve pathways, where liver inflammation or distension stimulates visceral afferent fibers that converge with somatic sensory neurons at the spinal cord level, particularly at C3-C5 segments that also innervate the shoulder region. The liver's large size and rich nerve supply mean that various hepatic conditions, including hepatitis, liver congestion, or hepatic abscess, can trigger this characteristic referral pattern. Patients often describe the referred pain as a deep, aching sensation in the right shoulder blade that may worsen with deep breathing or movement, sometimes leading to initial misdiagnosis as a musculoskeletal problem. The referral pattern becomes particularly pronounced when the liver capsule is stretched due to inflammation or rapid enlargement, as the capsule contains numerous pain-sensitive nerve endings. This warning system serves a crucial protective function by alerting individuals to liver dysfunction before more obvious symptoms like jaundice or abdominal swelling become apparent. The consistency of this referral pattern across different liver pathologies suggests it represents a fundamental aspect of hepatic innervation that healthcare providers can rely upon for diagnostic purposes. Additionally, the referral to the shoulder region may have evolutionary advantages, as shoulder discomfort naturally limits upper body movement and activity, potentially allowing the liver time to recover from whatever insult is causing the inflammation or dysfunction.
5. Appendicitis Pain Referral - The Periumbilical to Right Lower Quadrant Migration

Appendicitis presents a unique and diagnostically valuable pain referral pattern that typically begins as vague periumbilical discomfort before migrating to the right lower quadrant, reflecting the appendix's dual innervation and embryological origins. Initially, the visceral pain from appendiceal inflammation travels through sympathetic fibers that accompany the superior mesenteric artery, converging at the T10 spinal level, which corresponds to the periumbilical region where patients first experience the characteristic dull, cramping sensation. As inflammation progresses and involves the parietal peritoneum surrounding the appendix, somatic pain fibers are activated, creating the sharp, localized pain in the right iliac fossa known as McBurney's point. This evolution from referred visceral pain to localized somatic pain represents one of the most reliable diagnostic sequences in medicine, helping healthcare providers distinguish appendicitis from other causes of abdominal pain. The referral pattern serves as an early warning system, with the initial periumbilical pain alerting individuals to seek medical attention before the appendix reaches the point of perforation. The migration of pain from the umbilical region to the right lower quadrant typically occurs over 12-24 hours, providing a temporal framework that aids in diagnosis and treatment timing. This pattern is so consistent that deviations from it often suggest alternative diagnoses or anatomical variants, such as a retrocecal appendix position. The biological advantage of this referral system lies in its ability to create progressively more specific and intense warning signals as the condition becomes more serious, encouraging appropriate medical intervention before life-threatening complications develop.
6. Pancreatic Pain Referral - The Epigastric to Back Radiation
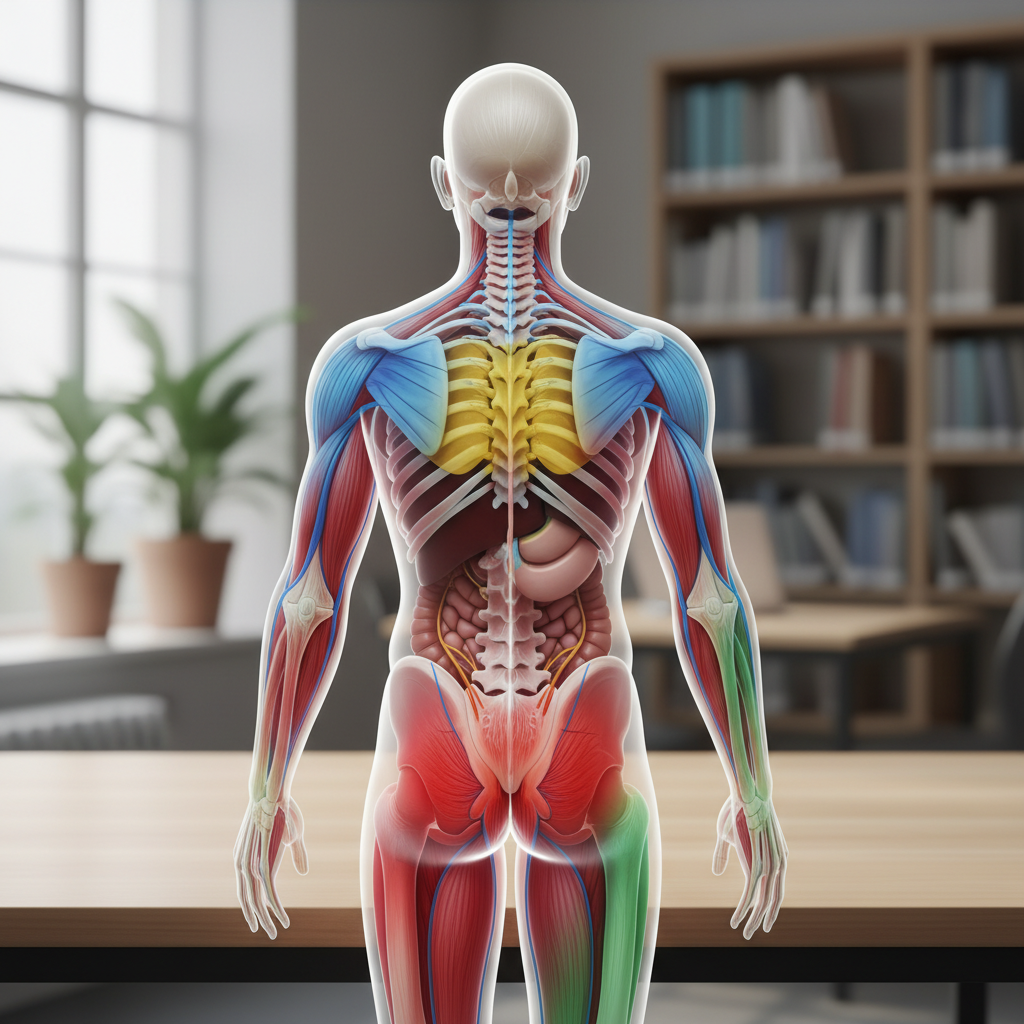
Pancreatic pain demonstrates a characteristic referral pattern that radiates from the epigastric region straight through to the back, creating a distinctive "boring" or "drilling" sensation that reflects the organ's retroperitoneal location and complex innervation. This referral occurs because the pancreas receives sensory innervation from both the celiac and superior mesenteric plexuses, with nerve fibers that travel alongside the splanchnic nerves to converge at the T6-T10 spinal cord levels, which also receive sensory input from the corresponding dermatomes on the back. The pancreas's deep retroperitoneal position means that inflammatory conditions like pancreatitis or pancreatic cancer often create pressure against the posterior abdominal wall and surrounding structures, contributing to the characteristic back pain that patients describe as penetrating and unrelenting. This referral pattern is particularly pronounced in acute pancreatitis, where patients often find temporary relief by leaning forward or assuming a fetal position, positions that may reduce pressure on the inflamed organ and surrounding neural structures. The referred back pain typically occurs at the level of the T8-T10 vertebrae, corresponding to the pancreas's anatomical position and nerve supply distribution. This warning system serves a crucial protective function, as pancreatic conditions can rapidly become life-threatening without appropriate medical intervention. The intensity and persistence of the referred back pain often correlates with the severity of pancreatic inflammation or damage, providing healthcare providers with valuable information about disease progression. Understanding this referral pattern helps distinguish pancreatic pain from other causes of epigastric discomfort, such as peptic ulcer disease or gastroesophageal reflux, which typically do not produce the characteristic through-and-through pain pattern.
7. Ovarian Pain Referral - The Pelvic to Thigh Connection
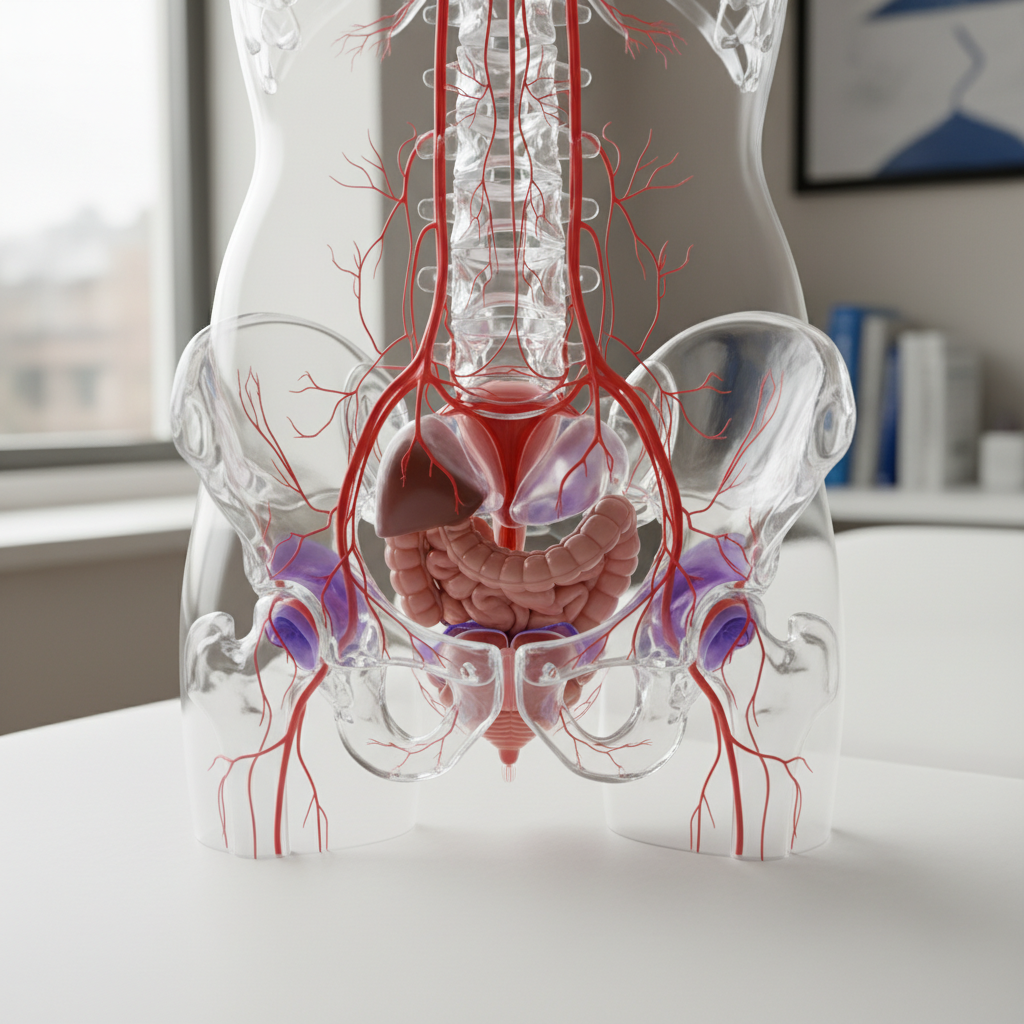
Ovarian pain referral follows the distribution of the ovarian nerve pathways, creating characteristic patterns that extend from the pelvis to the inner thigh and sometimes the lower back, reflecting the complex innervation of female reproductive organs. The ovaries receive dual innervation through both the sympathetic nervous system via the ovarian plexus (originating from T10-T11 spinal levels) and parasympathetic fibers from the pelvic splanchnic nerves, creating multiple potential pathways for referred pain. Ovarian cysts, torsion, or other pathology can trigger pain that radiates along the genitofemoral nerve distribution, causing discomfort in the inguinal region, upper thigh, and sometimes the lower abdomen in patterns that may initially suggest musculoskeletal or urological problems. The referral pattern becomes particularly pronounced during ovarian torsion, where the twisting of the ovary and its vascular supply creates intense visceral pain that often refers to the ipsilateral thigh and groin region. Ovulation pain (mittelschmerz) also follows these referral pathways, typically creating a characteristic monthly pattern of pelvic discomfort that may extend to the thigh or lower back. The referral system serves as an important warning mechanism, alerting women to ovarian dysfunction that might require medical intervention, particularly in cases of ovarian torsion where rapid treatment is essential to preserve organ viability. Healthcare providers rely on understanding these referral patterns to differentiate ovarian pathology from other causes of pelvic pain, such as appendicitis, kidney stones, or musculoskeletal problems. The evolutionary significance of this referral system likely relates to reproductive health protection, ensuring that ovarian problems generate unmistakable warning signals that would prompt behavioral changes to protect fertility and overall reproductive function.
8. Diaphragmatic Pain Referral - The Shoulder Tip Phenomenon
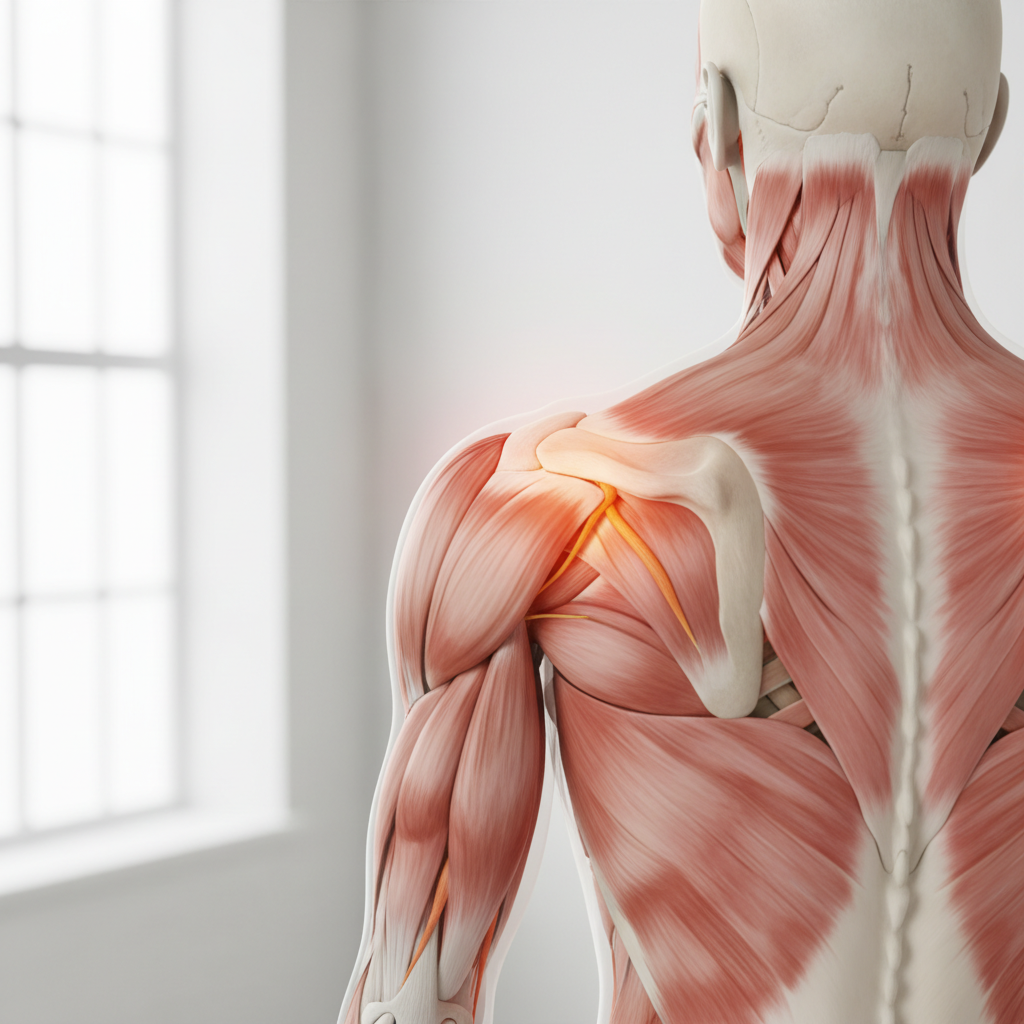
Diaphragmatic irritation creates one of the most distinctive and diagnostically valuable referral patterns in medicine, manifesting as sharp pain at the tip of the shoulder that reflects the unique embryological development and innervation of this crucial respiratory muscle. The diaphragm receives sensory innervation from the phrenic nerve, which originates from the C3, C4, and C5 nerve roots—the same spinal segments that provide sensory innervation to the shoulder region through the supraclavicular nerves. This shared neural pathway explains why diaphragmatic irritation, whether from blood, infection, or inflammation in the peritoneal cavity, consistently refers pain to the ipsilateral shoulder tip. The phenomenon is particularly common in conditions such as ruptured ectopic pregnancy, splenic rupture, or liver laceration, where blood or other irritating substances come into contact with the diaphragmatic surface. Patients typically describe the referred shoulder pain as sharp, stabbing, and distinctly different from typical musculoskeletal shoulder discomfort, often noting that the pain worsens with deep breathing or certain positional changes. This referral pattern serves as a crucial early warning system for potentially life-threatening intra-abdominal conditions, often appearing before other more obvious signs of internal bleeding or organ damage become apparent. The reliability of this referral pattern has made it an important diagnostic tool in emergency medicine, where shoulder tip pain in the appropriate clinical context can indicate the need for immediate surgical intervention. The evolutionary advantage of this system likely stems from the diaphragm's critical role in respiration, ensuring that any threat to this vital muscle generates unmistakable warning signals that would prompt immediate protective responses and medical attention.
9. Cervical Spine Pain Referral - The Neck to Arm and Head Pattern
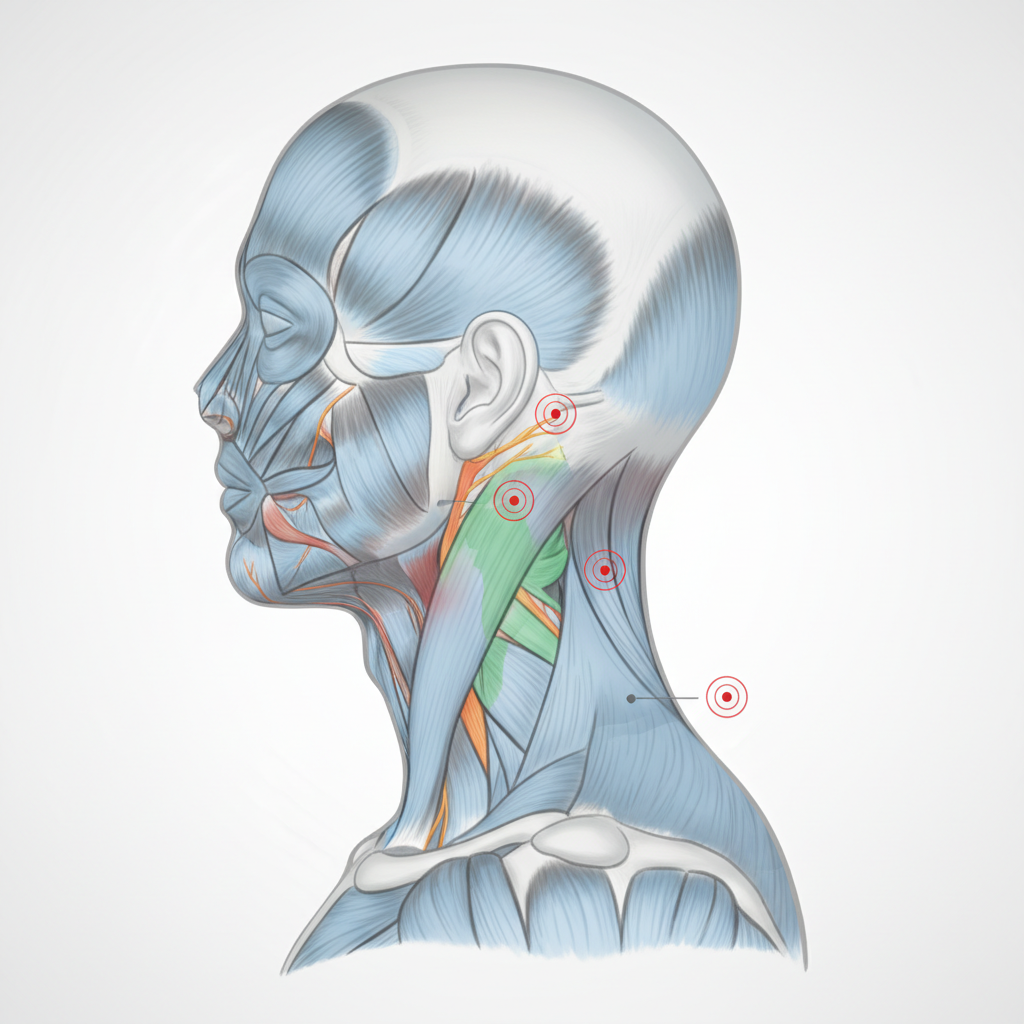
Cervical spine dysfunction creates complex referral patterns that can manifest as pain, numbness, or weakness throughout the upper extremities and head region, reflecting the intricate neural networks that emerge from the cervical spinal cord. The cervical nerve roots (C1-C8) form the brachial plexus and provide both motor and sensory innervation to the arms, shoulders, and parts of the head and neck, creating multiple pathways for referred pain when these structures are compressed or irritated. Cervical radiculopathy, whether from disc herniation, stenosis, or degenerative changes, can refer pain along specific dermatome patterns, with C6 nerve root irritation typically causing pain that radiates from the neck through the shoulder and down the lateral arm to the thumb, while C7 involvement often refers pain to the middle finger and posterior arm. The referral patterns are so consistent that healthcare providers can often predict which cervical nerve root is involved based solely on the distribution of referred symptoms. Cervical facet joint dysfunction can create different referral patterns, typically causing pain that radiates from the neck into the occipital region, temporal area, or upper trapezius muscle, depending on which joint levels are affected. These referral patterns serve as important warning systems, alerting individuals to cervical spine problems before more serious neurological complications develop, such as myelopathy or permanent nerve damage. The complexity of cervical referral patterns reflects the evolutionary importance of protecting the cervical spinal cord and nerve roots, which control many vital functions including breathing, upper extremity function, and sensory perception. Understanding these patterns helps distinguish cervical spine problems from other conditions that might cause similar symptoms, such as cardiac issues, thoracic outlet syndrome, or peripheral nerve entrapments.
10. Hip Joint Pain Referral - The Groin, Thigh, and Knee Connection
Hip joint pathology demonstrates characteristic referral patterns that commonly manifest as pain in the groin, anterior thigh, and surprisingly often the knee, creating diagnostic challenges that reflect the complex innervation of this ball-and-socket joint. The hip joint receives sensory innervation from multiple nerve sources, including the femoral nerve, obturator nerve, and branches of the sciatic nerve, which also provide sensory input to various regions of the lower extremity. Hip arthritis, labral tears, or other joint pathology frequently refer pain along the distribution of the obturator nerve, creating the classic pattern of groin pain that may extend down the medial thigh toward the knee. The knee referral is particularly noteworthy because many patients with hip problems initially seek treatment for what they perceive as a knee issue, not realizing that their knee pain originates from the hip joint above. This referral pattern occurs because both the hip and knee joints receive sensory innervation from the same spinal cord segments (L2-L4), causing the brain to mislocalize the source of pain signals. The anterior thigh referral follows the femoral nerve distribution, while posterior hip pain may refer along sciatic nerve pathways into the buttock and posterior thigh. These referral patterns serve as important early warning systems, alerting individuals to hip joint dysfunction before more obvious symptoms like limited range of motion or obvious joint deformity become apparent. The evolutionary significance of this referral system likely relates to the hip joint's crucial role in locomotion and weight-bearing, ensuring that joint problems generate widespread warning signals that would encourage protective behaviors and appropriate medical attention. Healthcare providers must maintain high clinical suspicion for hip pathology in patients presenting with groin, thigh, or knee pain, particularly in older adults or those with risk factors for hip joint disease.