8 Skin Texture Changes Linked to Thyroid Function
The intricate relationship between thyroid function and skin health represents one of dermatology's most fascinating yet underappreciated connections. Your thyroid gland, a butterfly-shaped organ nestled in your neck, produces hormones that regulate virtually every cellular process in your body, including the complex mechanisms governing skin texture, moisture, and appearance. When thyroid function becomes disrupted—whether through hypothyroidism, hyperthyroidism, or autoimmune conditions like Hashimoto's thyroiditis—the skin often serves as an early warning system, manifesting subtle yet telling changes that can precede more obvious systemic symptoms by months or even years. Research has consistently demonstrated that thyroid hormones T3 and T4 directly influence collagen synthesis, sebaceous gland activity, hair follicle cycling, and dermal hydration levels, making skin texture alterations not merely cosmetic concerns but valuable diagnostic indicators. Understanding these eight distinct skin texture changes can empower both patients and healthcare providers to recognize thyroid dysfunction earlier, leading to more timely interventions and better long-term outcomes for overall health and skin vitality.
1. Dry, Rough, and Scaly Skin - The Hypothyroid Signature
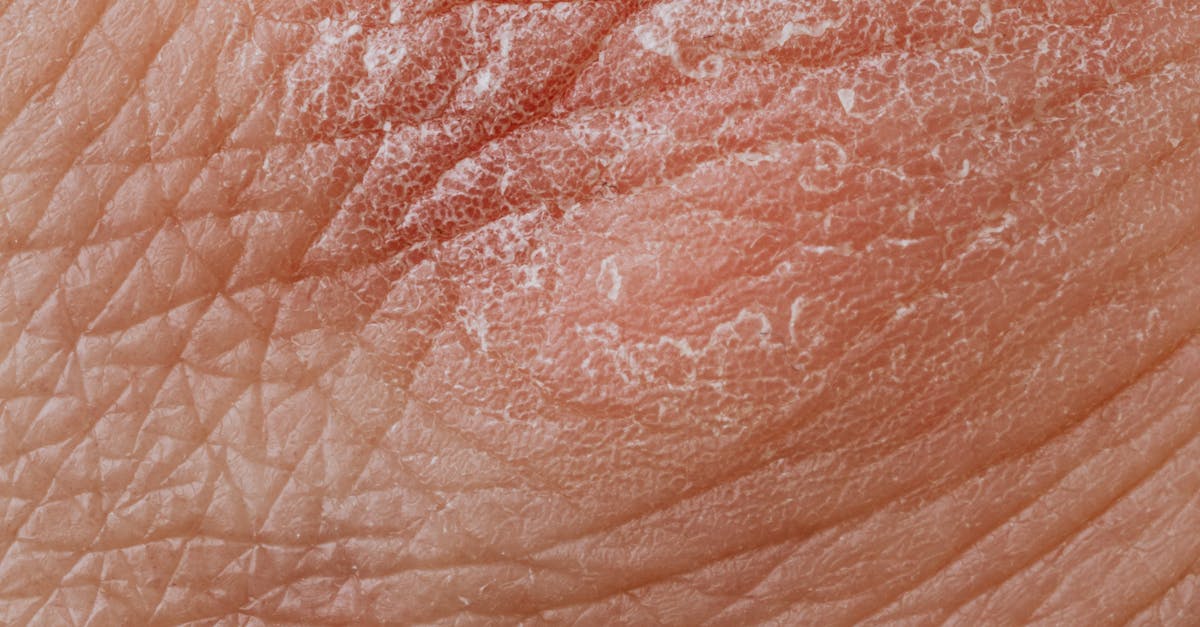
Perhaps the most recognizable skin manifestation of thyroid dysfunction is the development of persistently dry, rough, and scaly skin texture, particularly associated with hypothyroidism or underactive thyroid function. This condition, medically termed xerosis, occurs when decreased thyroid hormone levels significantly reduce the skin's natural oil production and impair the barrier function of the stratum corneum, the outermost layer of skin. Research published in the Journal of Clinical Endocrinology demonstrates that hypothyroid patients show measurably decreased sebum production, reduced ceramide levels, and compromised skin barrier integrity compared to healthy controls. The skin becomes noticeably coarse to the touch, often developing a sandpaper-like texture that's most pronounced on the shins, forearms, and elbows. Unlike temporary dryness from environmental factors, thyroid-related skin changes persist despite aggressive moisturizing efforts and tend to worsen gradually over time. The scaling can become so pronounced that it resembles fish scales, a condition called ichthyosis, which affects up to 30% of individuals with severe hypothyroidism. This texture change often accompanies other thyroid-related skin symptoms like yellowing of the palms and soles, and typically begins to improve within 6-8 weeks of initiating appropriate thyroid hormone replacement therapy.
2. Smooth, Velvety, and Warm Skin - Hyperthyroid Manifestations
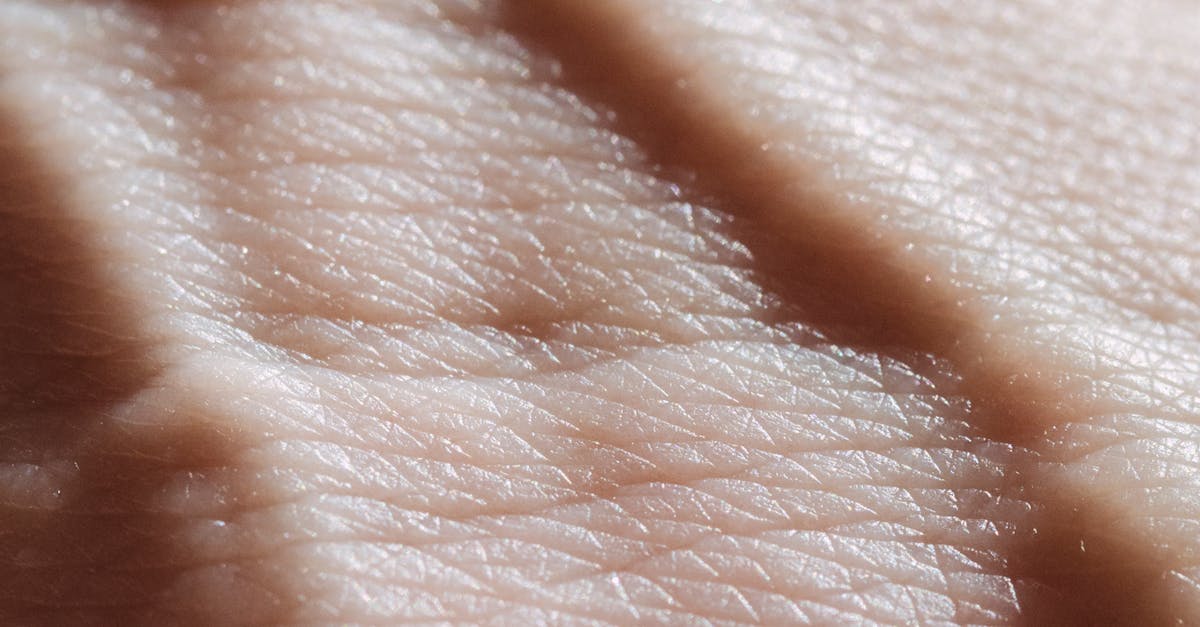
In stark contrast to the dry, rough texture associated with hypothyroidism, hyperthyroidism or overactive thyroid function produces distinctly smooth, velvety, and unusually warm skin that feels almost silky to the touch. This dramatic textural change results from the accelerated metabolic processes triggered by excess thyroid hormones, which increase blood flow to the skin, enhance sebaceous gland activity, and accelerate cellular turnover rates. Clinical studies have shown that hyperthyroid patients exhibit skin temperatures 2-3 degrees higher than normal, creating the characteristic warm, moist feeling that accompanies the smooth texture. The increased circulation gives the skin a healthy, almost luminous appearance, but this seemingly positive change often masks underlying health concerns. The velvety texture is most noticeable on the face, neck, and hands, where increased oil production creates an almost poreless appearance that many initially mistake for improved skin health. However, this hyperstimulated state is unsustainable and can lead to premature aging once thyroid levels normalize. The smooth texture may be accompanied by increased sweating, flushing, and a tendency toward heat intolerance. Interestingly, this skin change often appears before other classic hyperthyroid symptoms like weight loss or heart palpitations, making it a valuable early diagnostic indicator that healthcare providers should not overlook during routine examinations.
3. Thickened, Waxy Skin - Myxedema and Advanced Hypothyroidism

One of the most distinctive yet concerning skin texture changes associated with severe hypothyroidism is the development of thickened, waxy skin known as myxedema, a condition that represents the accumulation of mucopolysaccharides in the dermal layer. This unique texture change occurs when prolonged thyroid hormone deficiency leads to the deposition of hyaluronic acid and other glycosaminoglycans in the skin's deeper layers, creating a characteristic non-pitting swelling that gives the skin a doughy, waxy consistency. Unlike typical edema that leaves an indentation when pressed, myxedematous skin maintains its shape, feeling firm and almost leather-like to the touch. Research from the American Thyroid Association indicates that this condition affects approximately 5-10% of patients with severe, untreated hypothyroidism, most commonly appearing on the face, particularly around the eyes and cheeks, as well as on the hands and feet. The affected skin often takes on a yellowish hue due to carotenemia, another common feature of advanced hypothyroidism. The waxy texture can be so pronounced that facial features appear puffy and mask-like, with the skin losing its natural elasticity and becoming difficult to pinch or manipulate. This condition requires immediate medical attention, as it indicates severe thyroid hormone deficiency that can lead to life-threatening complications if left untreated, though the skin changes are typically reversible with appropriate hormone replacement therapy over several months.
4. Thinning, Fragile Skin - Hyperthyroid Complications
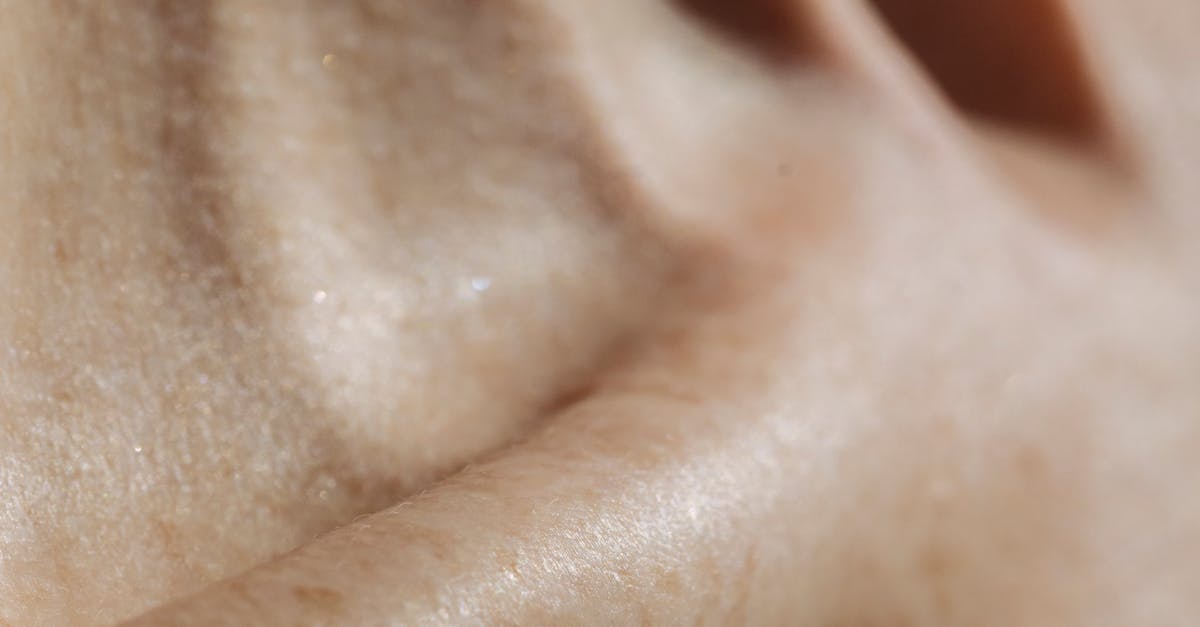
Extended periods of hyperthyroidism can lead to significant skin thinning and increased fragility, creating a texture that feels almost paper-thin and tears easily with minimal trauma. This concerning change occurs because excess thyroid hormones accelerate protein breakdown while simultaneously impairing collagen synthesis, leading to a net loss of structural skin proteins that maintain thickness and resilience. Dermatological research has documented that chronic hyperthyroid patients show measurably reduced dermal thickness on ultrasound imaging, with some individuals experiencing up to a 40% reduction in skin thickness compared to healthy controls. The thinning is most noticeable on areas already prone to delicate skin, such as the eyelids, backs of the hands, and forearms, where blood vessels become increasingly visible through the translucent skin. This fragility manifests as easy bruising from minor bumps, spontaneous tearing from normal activities like removing adhesive bandages, and delayed wound healing that can lead to persistent skin breakdown. The texture feels almost crepe-like, lacking the normal plumpness and elasticity of healthy skin. Additionally, the thinned skin provides less protection against UV radiation, making hyperthyroid patients more susceptible to sun damage and premature aging. This condition can be particularly distressing for patients, as the visible changes often persist for months after thyroid hormone levels normalize, requiring patience and protective skincare measures during the recovery period.
5. Coarse, Pebbled Texture - Thyroid-Related Keratosis
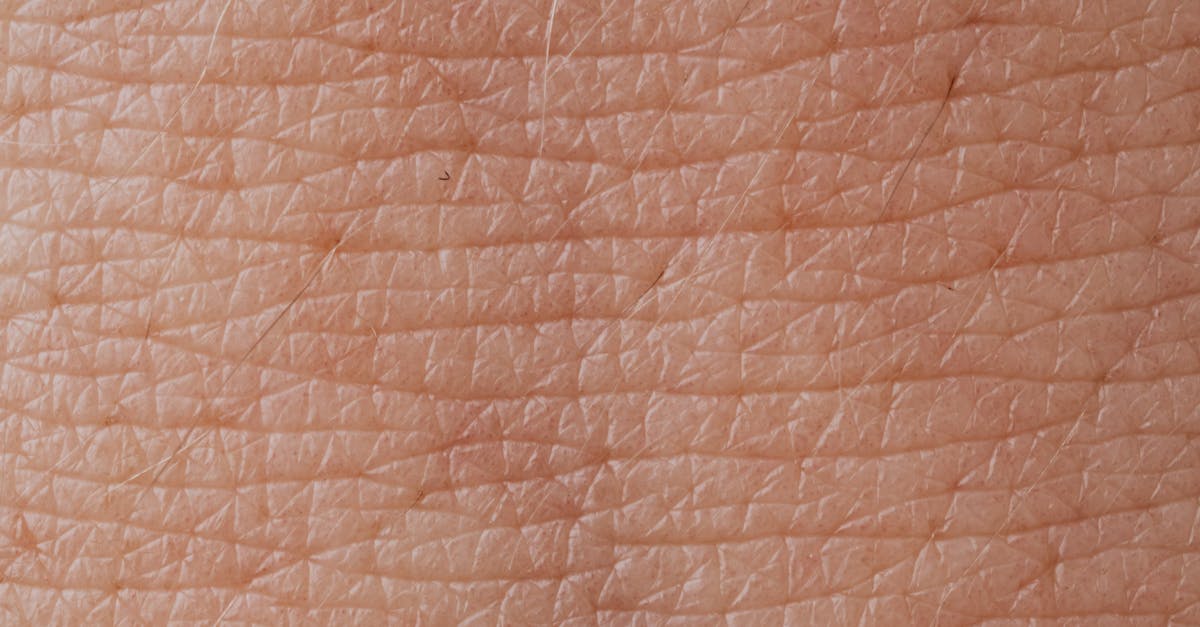
A lesser-known but significant skin texture change associated with thyroid dysfunction is the development of coarse, pebbled skin that resembles the texture of an orange peel or goose bumps that never resolve. This condition, often called keratosis pilaris-like changes, occurs when altered thyroid hormone levels disrupt normal keratinocyte turnover and follicular keratinization processes, leading to the accumulation of keratin plugs in hair follicles and surrounding skin. Clinical observations have shown that this pebbled texture most commonly affects the upper arms, thighs, and buttocks of hypothyroid patients, though it can appear anywhere on the body where hair follicles are present. The affected skin feels rough and bumpy to the touch, with small, hard bumps that may be flesh-colored or slightly darker than the surrounding skin. Unlike typical keratosis pilaris, which is primarily a cosmetic concern, thyroid-related keratosis often covers larger areas and may be accompanied by inflammation and itching. Research suggests that this texture change results from the combination of decreased skin cell turnover, altered sebum composition, and impaired barrier function that characterizes hypothyroid skin. The pebbled appearance can be particularly pronounced in areas where clothing creates friction, and unlike environmental or genetic causes of similar skin textures, thyroid-related keratosis typically improves significantly once optimal thyroid hormone levels are achieved and maintained, though improvement may take several months to become apparent.
6. Puffy, Swollen Texture - Thyroid-Related Edema
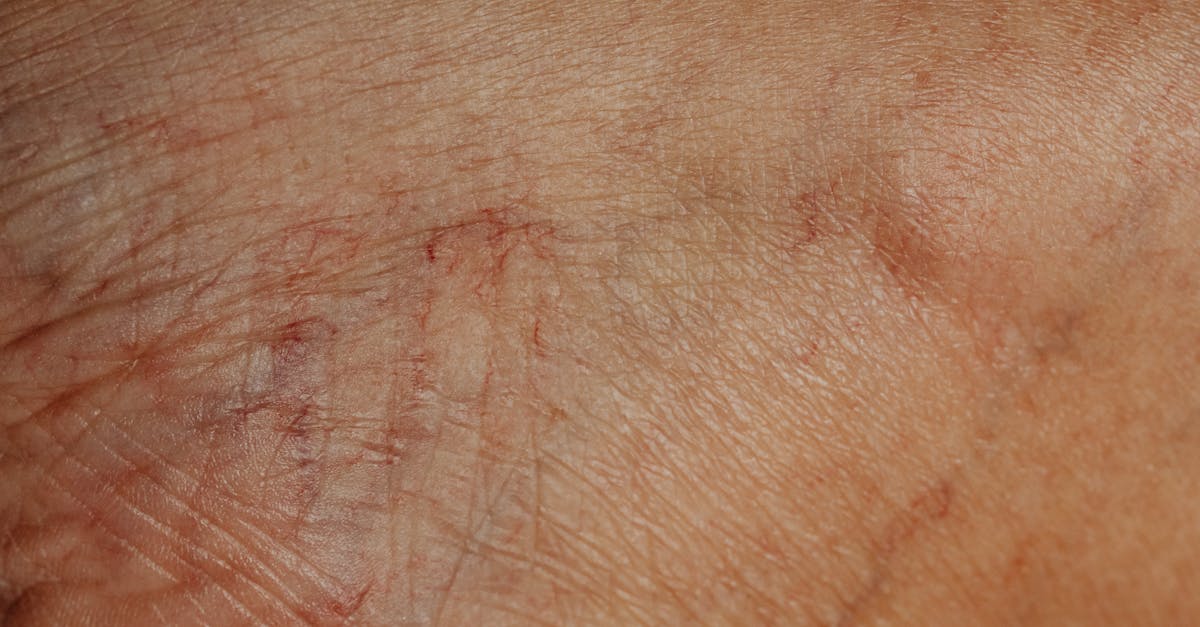
Thyroid dysfunction frequently manifests as distinctive puffy, swollen skin texture that differs significantly from typical fluid retention, creating areas that feel spongy and maintain indentations when pressed. This unique textural change, most commonly associated with hypothyroidism, results from the accumulation of protein-rich fluid in the interstitial spaces of the skin, combined with the deposition of mucopolysaccharides that characterize myxedematous changes. Unlike cardiac or renal edema, thyroid-related skin swelling typically affects specific areas including the face (particularly around the eyes), hands, and feet, creating a characteristic puffy appearance that patients often describe as feeling "stuffed" or "bloated." Endocrinological studies have demonstrated that this swelling results from increased capillary permeability and altered sodium-potassium pump function caused by thyroid hormone deficiency, leading to fluid accumulation that gives the skin a distinctly soft, doughy texture. The affected areas may feel cool to the touch and appear pale or slightly yellow-tinged, with the skin surface showing a subtle dimpled or orange-peel appearance when examined closely. This puffy texture is often most noticeable in the morning upon waking and may fluctuate throughout the day, though it rarely completely resolves without thyroid hormone treatment. The swelling can be so pronounced that it affects facial features, making the eyes appear smaller and the cheeks fuller, changes that can significantly impact a person's appearance and self-confidence until proper thyroid treatment is established.
7. Rough, Sandpaper-Like Patches - Localized Thyroid Skin Changes
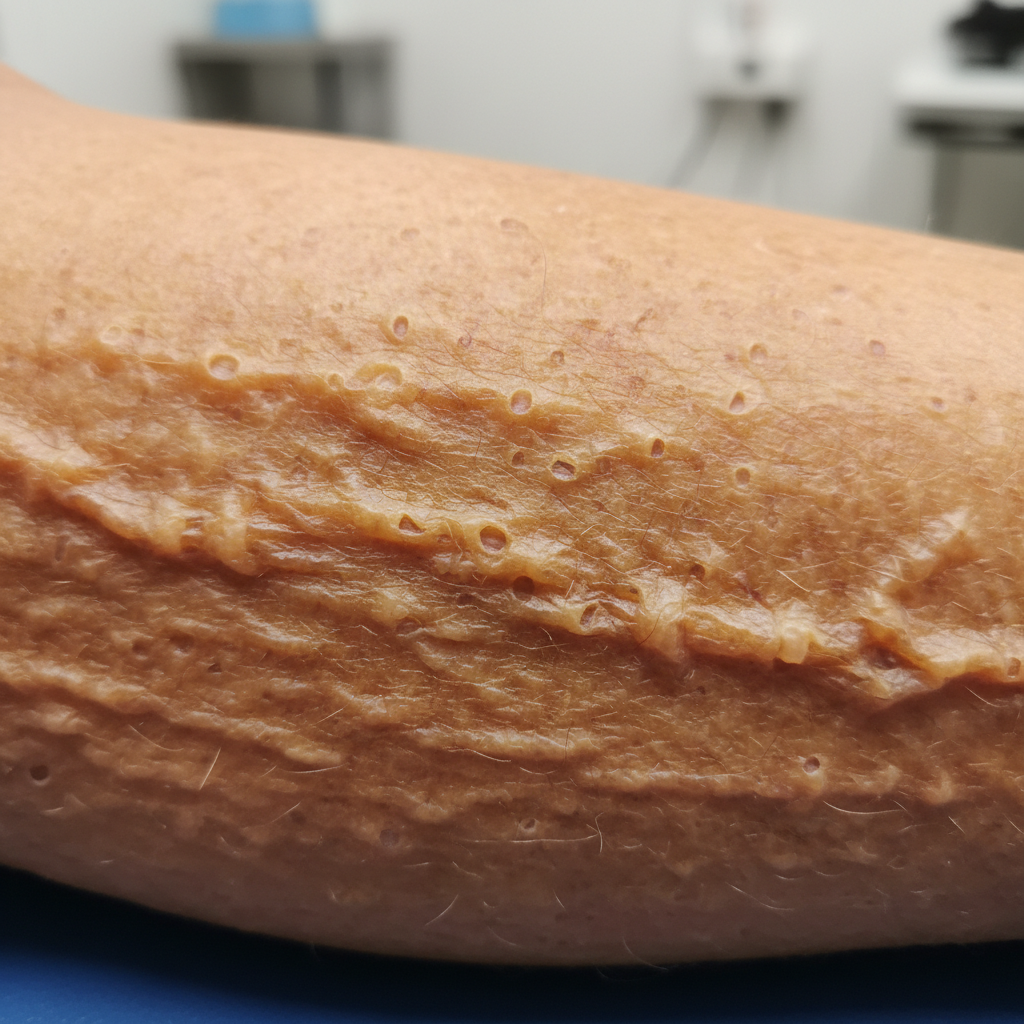
Thyroid dysfunction can manifest as distinctly rough, sandpaper-like patches of skin that appear in localized areas, creating texture changes that feel dramatically different from the surrounding normal skin. These patches, medically termed hyperkeratotic lesions, develop when thyroid hormone imbalances disrupt the normal process of skin cell renewal, causing excessive accumulation of dead skin cells in specific areas rather than the generalized dryness seen in other thyroid-related skin conditions. Research has identified that these rough patches most commonly appear on the elbows, knees, and heels of hypothyroid patients, though they can develop anywhere on the body where skin experiences regular friction or pressure. The affected areas feel distinctly gritty and may appear darker than surrounding skin due to the thickened keratin layer that creates shadows and traps environmental particles. Unlike calluses or corns that develop from external pressure, thyroid-related rough patches can appear on areas with minimal friction and tend to be more widespread and persistent. Dermatological examination often reveals that these patches have poorly defined borders and may be accompanied by fine scaling or flaking that becomes more pronounced in dry weather. The texture can be so rough that it catches on clothing or bedding, and attempts to smooth the area with pumice stones or exfoliating treatments often provide only temporary relief. These localized texture changes typically begin to improve within 2-3 months of initiating appropriate thyroid hormone replacement therapy, though complete resolution may take 6-12 months as the skin gradually returns to normal cellular turnover patterns.
8. Smooth, Shiny, and Tight Skin - Pretibial Myxedema
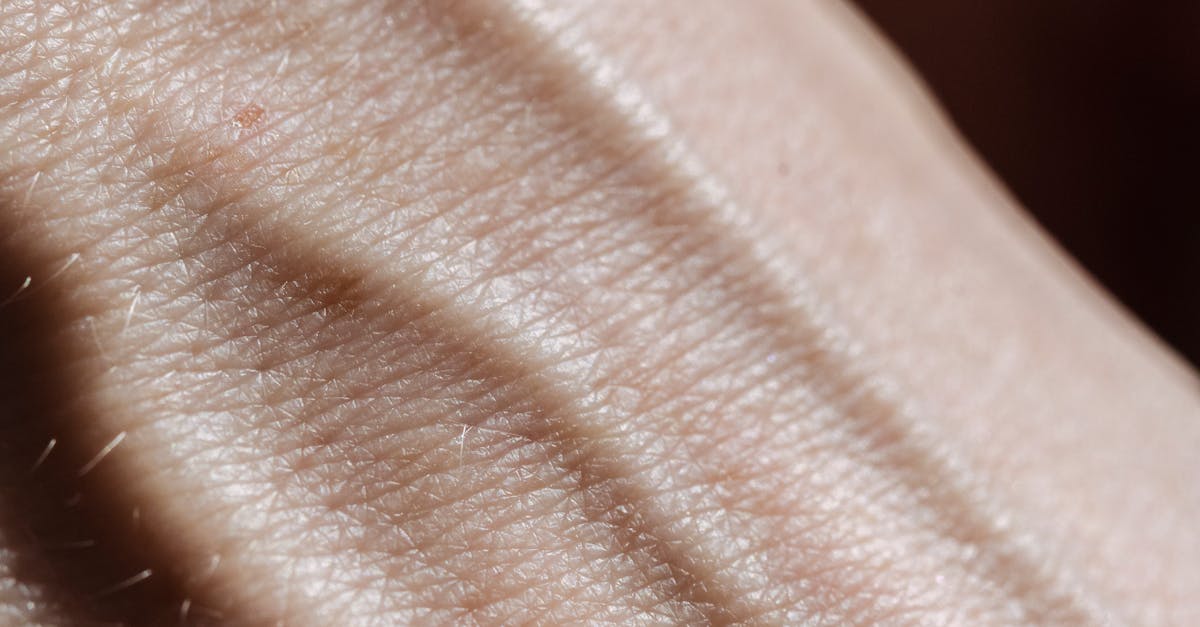
A rare but distinctive skin texture change associated with thyroid dysfunction is the development of smooth, shiny, and abnormally tight skin, most commonly seen in a condition called pretibial myxedema, which paradoxically occurs in some patients with hyperthyroidism, particularly those with Graves' disease. This unique texture change affects the front of the lower legs, creating skin that appears almost plastic-like in its smoothness and reflective quality, while simultaneously feeling tight and non-elastic when touched. The affected skin loses its normal texture completely, becoming so smooth that it appears almost artificial, with a waxy sheen that reflects light in an unnatural way. Clinical studies have shown that this condition results from the deposition of hyaluronic acid and other mucopolysaccharides in the dermis, triggered by thyroid-stimulating immunoglobulins that cross-react with tissues outside the thyroid gland. The skin becomes progressively tighter over time, sometimes restricting movement and causing discomfort, particularly when walking or bending the legs. Unlike the puffy myxedema seen in hypothyroidism, pretibial myxedema creates a firm, almost board-like texture that doesn't indent when pressed. The affected areas may also develop a distinctive orange-peel appearance around the edges, where the abnormal skin meets normal tissue. This condition can be particularly challenging to treat, as it may persist or even worsen despite normalization of thyroid hormone levels, requiring specialized treatments including topical corticosteroids, compression therapy, or in severe cases, surgical intervention to restore normal skin texture and function.
9. Integration and Clinical Significance - Recognizing the Complete Picture

Understanding these eight distinct skin texture changes linked to thyroid function provides invaluable insight into the complex interplay between endocrine health and dermatological manifestations, emphasizing the importance of viewing skin changes as potential windows into systemic health rather than isolated cosmetic concerns. The recognition that thyroid dysfunction can present through such diverse skin texture alterations—from the dry, scaly skin of hypothyroidism to the smooth, velvety texture of hyperthyroidism, and the more complex changes like pretibial myxedema—underscores the need for healthcare providers to maintain high clinical suspicion when evaluating patients with persistent or unusual skin texture changes. Research consistently demonstrates that skin manifestations often precede other thyroid symptoms by months, making dermatological awareness crucial for early diagnosis and intervention. The reversible nature of most thyroid-related skin changes offers hope for patients, though the timeline for improvement varies significantly depending on the severity and duration of thyroid dysfunction, with some changes resolving within weeks of treatment initiation while others may require months or years for complete resolution. For patients experiencing these texture changes, maintaining detailed photographic records and working closely with both dermatologists and endocrinologists can optimize treatment outcomes and monitor progress effectively. The integration of skin texture assessment into routine thyroid evaluation protocols could significantly improve diagnostic accuracy and patient outcomes, while patient education about these connections empowers individuals to seek appropriate medical attention when they notice persistent skin texture changes that don't respond to conventional skincare approaches.