12 Skin Color Changes Doctors Use as Diagnostic Clues
The human skin serves as far more than a protective barrier against the external environment; it functions as a sophisticated diagnostic canvas that reveals critical information about our internal health status. Medical professionals have long recognized that changes in skin coloration can provide invaluable clues about underlying systemic conditions, metabolic disorders, and disease processes occurring within the body. From the subtle yellowing associated with liver dysfunction to the distinctive blue-gray discoloration of certain genetic conditions, skin color variations represent a complex interplay of physiological factors including blood circulation, oxygen saturation, pigment production, and cellular metabolism. This comprehensive exploration delves into twelve specific skin color changes that serve as essential diagnostic tools in modern medicine, examining the underlying pathophysiology, clinical significance, and diagnostic implications of each condition. Understanding these dermatological manifestations enables healthcare providers to make more accurate diagnoses, initiate appropriate treatments, and potentially identify serious medical conditions before they progress to more advanced stages.
1. Jaundice - The Yellow Warning Signal
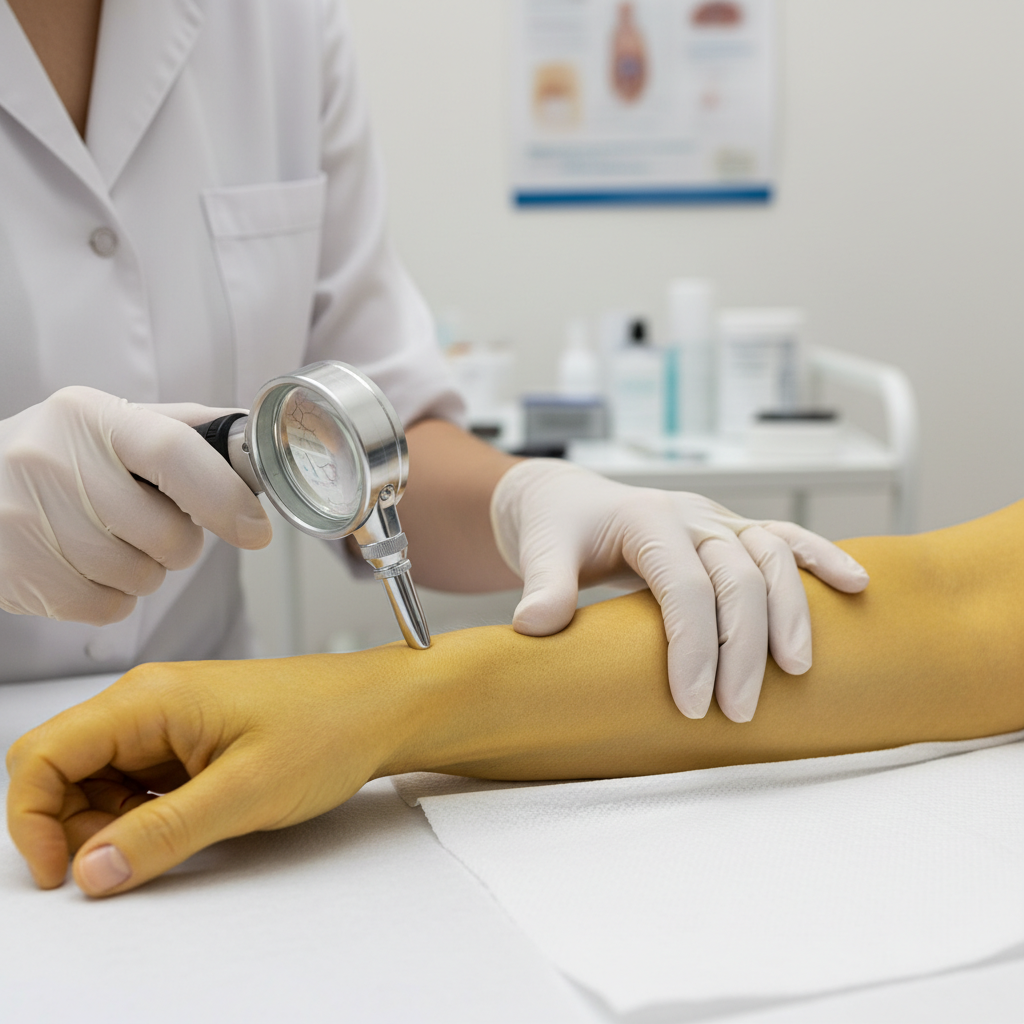
Jaundice represents one of the most recognizable and clinically significant skin color changes in medical practice, characterized by a distinctive yellow discoloration of the skin, sclera, and mucous membranes. This condition results from elevated levels of bilirubin in the bloodstream, a yellow pigment produced during the normal breakdown of red blood cells. When bilirubin accumulates beyond the body's capacity to process and eliminate it, the excess pigment deposits in tissues, creating the characteristic golden-yellow appearance that medical professionals immediately recognize as a potential indicator of serious underlying pathology. The causes of jaundice are broadly categorized into three main types: pre-hepatic (related to excessive red blood cell destruction), hepatic (involving liver dysfunction or disease), and post-hepatic (caused by bile duct obstruction). Pre-hepatic jaundice may result from conditions such as hemolytic anemia, malaria, or certain genetic disorders affecting red blood cell stability. Hepatic jaundice commonly occurs in cases of viral hepatitis, alcoholic liver disease, cirrhosis, or drug-induced liver toxicity. Post-hepatic jaundice typically stems from gallstones, pancreatic cancer, or bile duct strictures that prevent normal bile flow. The intensity and distribution of jaundice can provide additional diagnostic clues, with mild jaundice often appearing first in the sclera before becoming visible in the skin, while severe cases may present with a deep orange-yellow coloration throughout the body.
2. Cyanosis - When Oxygen Levels Drop
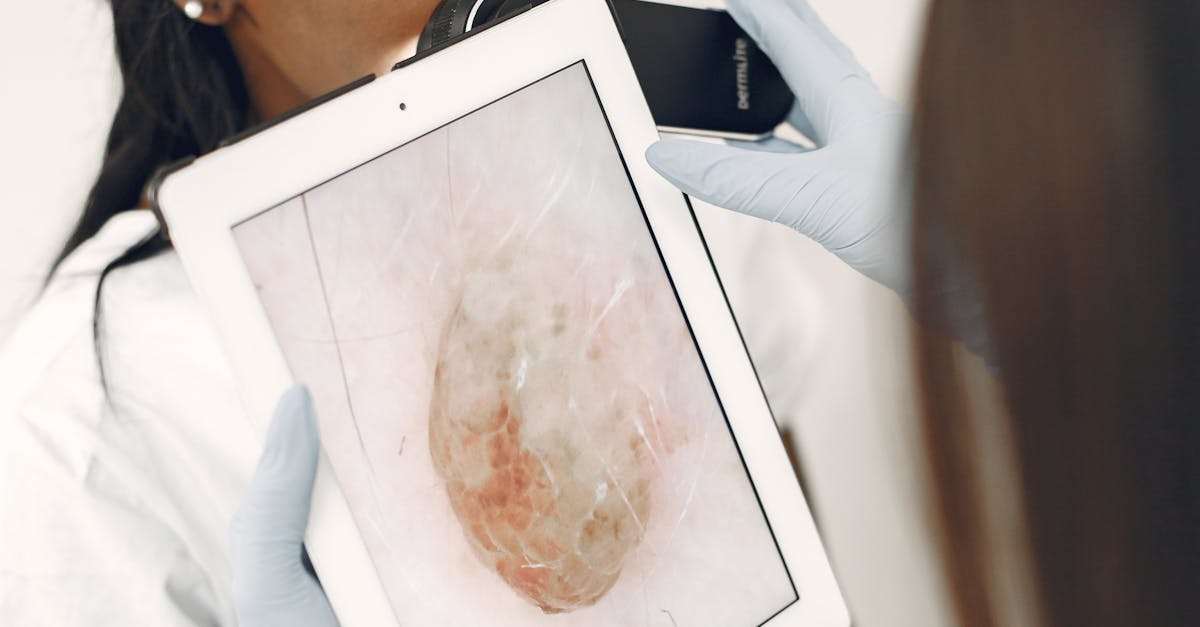
Cyanosis manifests as a blue or purple discoloration of the skin and mucous membranes, serving as a critical visual indicator of inadequate oxygen saturation in the blood or poor circulation. This distinctive coloration occurs when deoxygenated hemoglobin levels exceed approximately 5 grams per deciliter in the capillary blood, creating the characteristic blue-tinged appearance that immediately alerts healthcare providers to potential respiratory or cardiovascular emergencies. Central cyanosis affects the core areas of the body, including the lips, tongue, and mucous membranes, typically indicating serious systemic hypoxemia caused by conditions such as severe pneumonia, pulmonary edema, congenital heart defects, or chronic obstructive pulmonary disease. Peripheral cyanosis, conversely, affects the extremities like fingers and toes, often resulting from reduced blood flow due to cold exposure, peripheral vascular disease, or shock states. The clinical significance of cyanosis cannot be overstated, as it frequently represents a medical emergency requiring immediate intervention to restore adequate oxygenation and prevent organ damage. Healthcare providers must distinguish between true cyanosis and pseudocyanosis, which can result from certain medications, dyes, or heavy metal poisoning that may create similar discoloration without actual oxygen deficiency. The assessment of cyanosis also requires consideration of factors such as ambient lighting, skin pigmentation, and the presence of anemia, which can mask or alter the typical presentation of this important diagnostic sign.
3. Pallor - The Pale Complexion Mystery
Pallor describes an abnormal paleness or loss of normal skin coloration that can indicate various underlying medical conditions, ranging from simple fatigue to serious systemic diseases. This condition occurs when there is reduced blood flow to the skin, decreased red blood cell count, or diminished hemoglobin levels, resulting in a noticeably lighter complexion than the individual's baseline skin tone. Healthcare providers assess pallor by examining areas with minimal pigmentation and good vascular supply, such as the conjunctiva, nail beds, palms, and mucous membranes, where changes in blood perfusion become most apparent. Acute pallor may develop suddenly due to conditions like severe bleeding, shock, or acute heart failure, while chronic pallor typically evolves gradually in association with conditions such as iron-deficiency anemia, chronic kidney disease, or malnutrition. The underlying mechanisms causing pallor include vasoconstriction of cutaneous blood vessels, reduced cardiac output, decreased blood volume, or diminished oxygen-carrying capacity of the blood. Anemia represents one of the most common causes of pallor, with different types producing varying degrees of skin color changes depending on the severity and underlying etiology. Iron-deficiency anemia often presents with a characteristic pale, almost translucent appearance, while chronic disease-related anemia may produce a more subtle pallor accompanied by other systemic symptoms. Healthcare providers must differentiate between pathological pallor and normal variations in skin pigmentation, considering factors such as genetic background, sun exposure history, and individual baseline coloration when making clinical assessments.
4. Erythema - The Red Flag of Inflammation
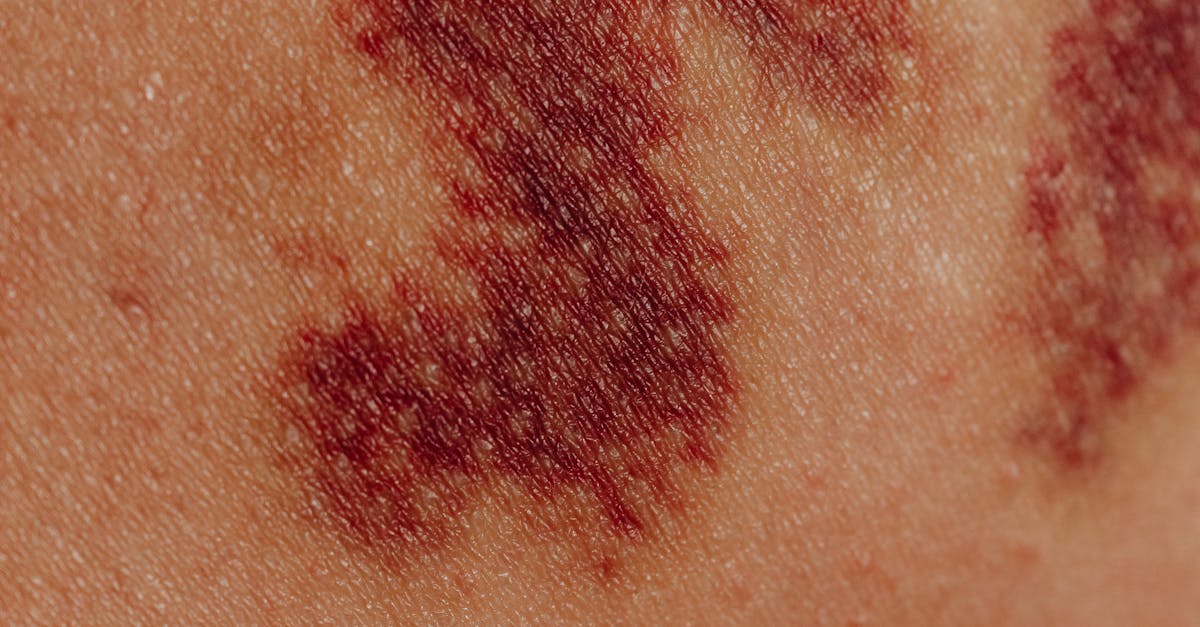
Erythema presents as abnormal redness of the skin caused by increased blood flow to the superficial capillaries, serving as a fundamental indicator of inflammation, infection, or vascular changes within affected tissues. This distinctive red discoloration occurs when arterioles and capillaries dilate in response to various stimuli, including inflammatory mediators, heat, mechanical irritation, or immune system activation. The clinical assessment of erythema involves evaluating its distribution, intensity, associated symptoms, and response to pressure, with blanching erythema (which temporarily disappears with pressure) indicating vasodilation, while non-blanching erythema may suggest more serious conditions involving bleeding into the skin. Localized erythema commonly accompanies skin infections such as cellulitis, where bacterial invasion triggers an intense inflammatory response characterized by warmth, swelling, and tenderness in addition to the characteristic redness. Systemic conditions can also manifest with widespread erythema, including autoimmune disorders like systemic lupus erythematosus, which may present with the classic butterfly rash across the cheeks and nose bridge. Drug reactions frequently cause erythematous eruptions ranging from mild skin redness to severe, life-threatening conditions like Stevens-Johnson syndrome or toxic epidermal necrolysis. Healthcare providers must carefully evaluate the pattern and progression of erythema, as certain distributions can provide specific diagnostic clues, such as the photosensitive distribution seen in lupus or the characteristic pattern of erythema migrans associated with Lyme disease. The temporal relationship between erythema onset and potential triggers, including medications, infections, or environmental exposures, provides crucial information for accurate diagnosis and appropriate treatment planning.
5. Hyperpigmentation - When Skin Darkens
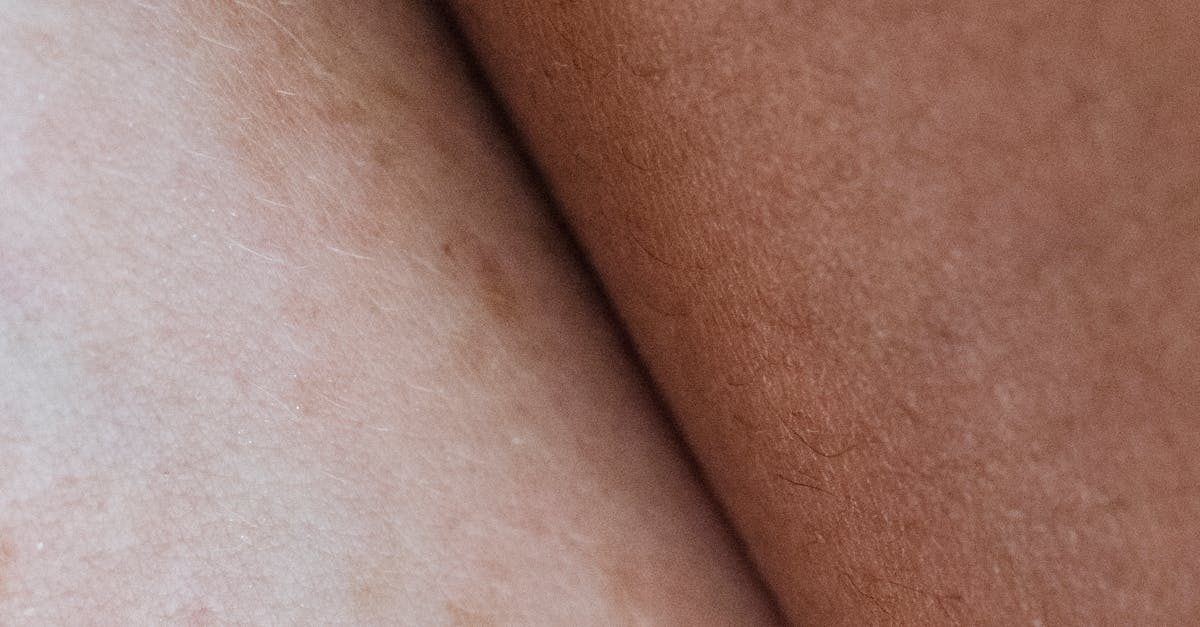
Hyperpigmentation encompasses various conditions characterized by abnormal darkening of the skin due to increased melanin production, melanin deposition, or accumulation of other pigmented substances within the dermis or epidermis. This complex group of conditions can result from multiple mechanisms, including post-inflammatory changes, hormonal influences, genetic factors, medication effects, or underlying systemic diseases that affect melanocyte function or pigment metabolism. Melasma, commonly known as the "mask of pregnancy," represents one of the most frequent forms of hyperpigmentation, typically affecting women during pregnancy or while taking hormonal contraceptives, creating symmetric brown patches on the face due to increased estrogen and progesterone levels stimulating melanin production. Post-inflammatory hyperpigmentation frequently develops following skin injury, acne, eczema, or other inflammatory conditions, particularly in individuals with darker skin types who have a greater tendency to produce excess melanin in response to tissue damage. Certain medications can induce hyperpigmentation through various mechanisms, including antimalarial drugs that deposit in the skin, chemotherapy agents that affect melanocyte function, or antibiotics like minocycline that can cause distinctive blue-gray discoloration. Addison's disease, a condition involving adrenal insufficiency, characteristically produces diffuse hyperpigmentation due to elevated levels of adrenocorticotropic hormone (ACTH), which stimulates melanin production and creates a bronze-like skin coloration that often appears first in areas exposed to friction or pressure. Healthcare providers must distinguish between benign hyperpigmentation and potentially serious conditions like melanoma, which can present as irregularly pigmented lesions requiring immediate evaluation and possible biopsy for definitive diagnosis.
6. Vitiligo - The Loss of Color
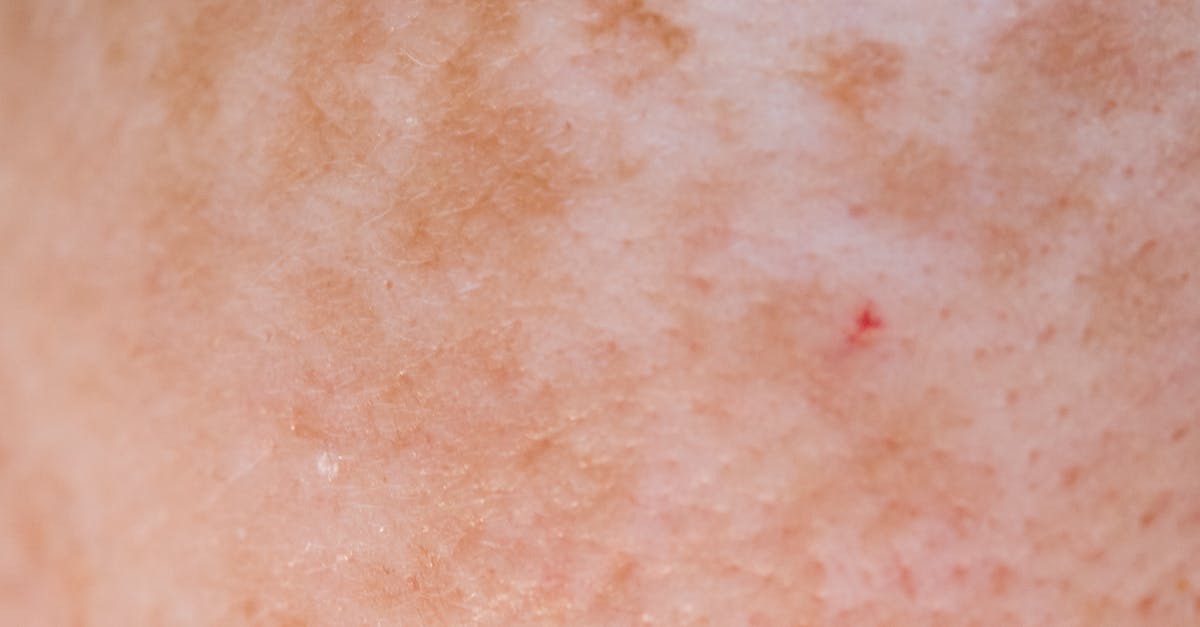
Vitiligo represents a distinctive autoimmune condition characterized by the progressive loss of skin pigmentation, resulting in well-demarcated white or depigmented patches that can appear anywhere on the body but commonly affect areas around body openings, joints, and sites of previous injury. This condition occurs when the immune system mistakenly attacks and destroys melanocytes, the specialized cells responsible for producing melanin pigment, leading to complete absence of coloration in affected areas. The clinical presentation of vitiligo varies significantly among individuals, with some experiencing limited, stable patches while others develop extensive, rapidly progressive depigmentation that can affect large portions of the body surface. Segmental vitiligo typically affects one side of the body in a dermatomal distribution and tends to stabilize after initial progression, while non-segmental vitiligo presents with symmetric patches that may continue expanding over time. The psychological impact of vitiligo can be profound, particularly when it affects visible areas like the face and hands, leading to significant emotional distress and social anxiety that healthcare providers must address as part of comprehensive patient care. Associated autoimmune conditions frequently accompany vitiligo, including thyroid disorders, type 1 diabetes, pernicious anemia, and Addison's disease, necessitating regular screening and monitoring for these related conditions. The diagnosis of vitiligo is primarily clinical, based on the characteristic appearance of depigmented patches, but Wood's lamp examination can help identify subtle lesions and assess the extent of involvement, particularly in fair-skinned individuals where contrast may be less apparent. Treatment options for vitiligo include topical corticosteroids, calcineurin inhibitors, phototherapy, and newer targeted therapies, with the choice depending on factors such as lesion location, extent of involvement, patient age, and individual response to previous treatments.
7. Bronze Discoloration - Hemochromatosis and Iron Overload

Bronze skin discoloration represents a pathognomonic sign of hereditary hemochromatosis and other iron overload disorders, creating a distinctive metallic bronze or slate-gray appearance that results from excessive iron deposition in the skin and other organs throughout the body. This characteristic coloration develops gradually as iron accumulates beyond the body's normal storage capacity, with the excess metal binding to proteins and depositing in various tissues, including the dermis where it creates the unmistakable bronze hue that gives hemochromatosis its historical nickname of "bronze diabetes." Hereditary hemochromatosis, the most common genetic disorder affecting people of Northern European descent, results from mutations in genes regulating iron absorption, leading to progressive iron accumulation that can cause irreversible organ damage if left untreated. The bronze discoloration typically becomes apparent when total body iron stores reach 15-40 grams, compared to the normal 3-4 grams, and often appears first on sun-exposed areas before becoming more generalized as the condition progresses. Secondary iron overload can also produce similar skin changes and may result from repeated blood transfusions, certain types of anemia requiring frequent transfusions, chronic liver disease, or excessive dietary iron intake, particularly in individuals with underlying genetic predispositions to iron accumulation. The clinical significance of bronze discoloration extends far beyond its cosmetic appearance, as it indicates substantial iron overload that may be associated with serious complications including liver cirrhosis, diabetes mellitus, cardiomyopathy, arthritis, and increased risk of hepatocellular carcinoma. Healthcare providers must recognize that the bronze coloration may be subtle in early stages and can be masked by concurrent conditions affecting skin pigmentation, making biochemical testing essential for definitive diagnosis through measurement of serum ferritin, transferrin saturation, and genetic testing for common hemochromatosis mutations.
8. Gray-Blue Discoloration - Argyria and Metal Deposition
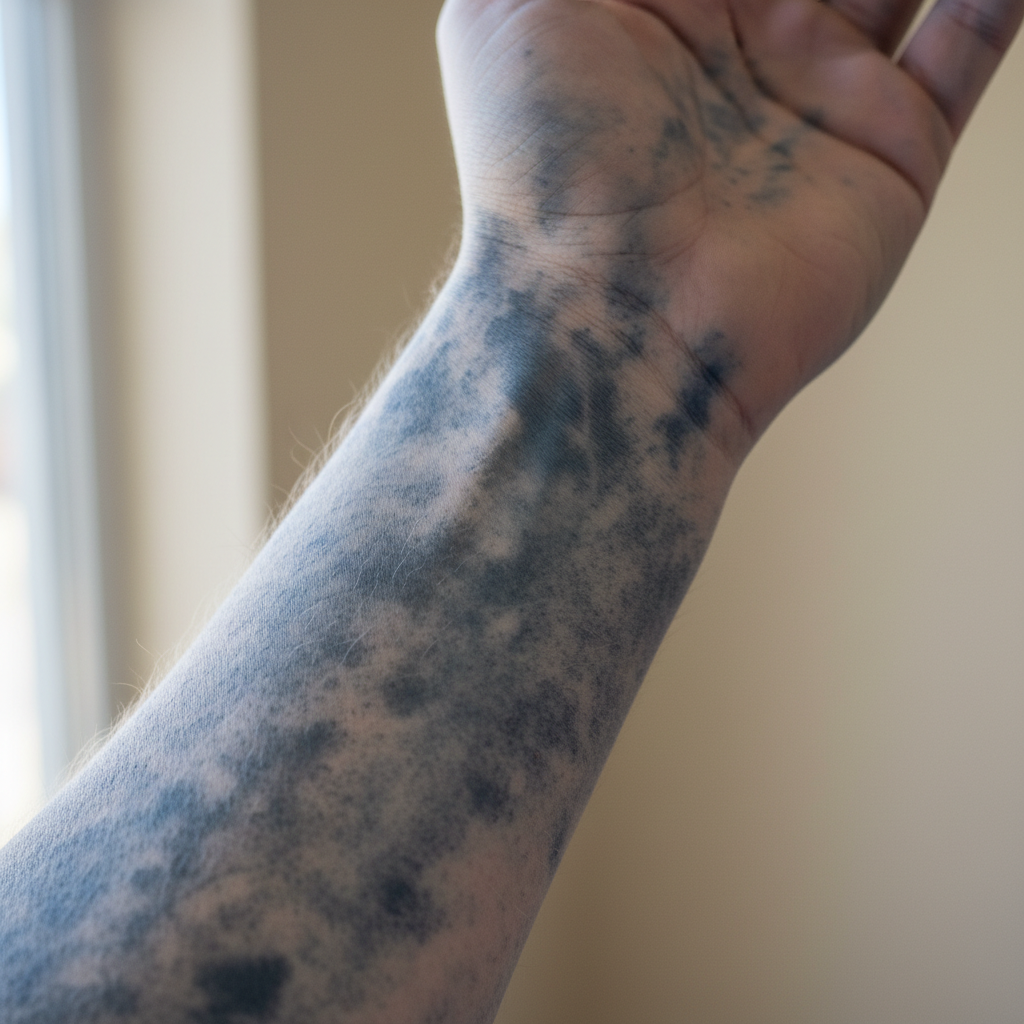
Gray-blue skin discoloration, most notably seen in argyria, represents a permanent cosmetic change resulting from silver deposition in the dermis and other tissues, creating a distinctive blue-gray metallic appearance that serves as a visible marker of chronic silver exposure. This irreversible condition develops when silver particles accumulate in the skin following prolonged exposure to silver-containing compounds, including colloidal silver supplements, silver-based medications, or occupational exposure to silver dust or solutions. The pathophysiology of argyria involves the reduction of silver ions to metallic silver particles within dermal tissues, where they become permanently deposited and create the characteristic discoloration that typically affects sun-exposed areas most prominently due to photochemical reactions that enhance silver particle formation. Localized argyria may develop from topical silver applications, such as silver nitrate used for medical procedures or silver-containing wound dressings, while generalized argyria results from systemic silver absorption through ingestion or inhalation of silver compounds over extended periods. Similar gray-blue discoloration can occur with other heavy metals, including lead, bismuth, and gold, each producing slightly different hues and distribution patterns that can provide diagnostic clues about the specific metal involved and route of exposure. The clinical importance of recognizing metal-induced skin discoloration extends beyond the cosmetic concerns, as it may indicate significant systemic metal burden that could potentially affect other organ systems, although argyria itself is generally considered benign from a health perspective. Healthcare providers must obtain detailed exposure histories when evaluating patients with unexplained gray-blue skin discoloration, including questions about dietary supplements, occupational exposures, medications, and alternative medicine practices that might involve metal-containing compounds. The diagnosis of argyria can be confirmed through skin biopsy, which reveals characteristic silver deposits in the dermis, and may be supported by elevated silver levels in blood or urine samples, though these may normalize despite persistent skin discoloration.
9. Carotenemia - The Orange Glow
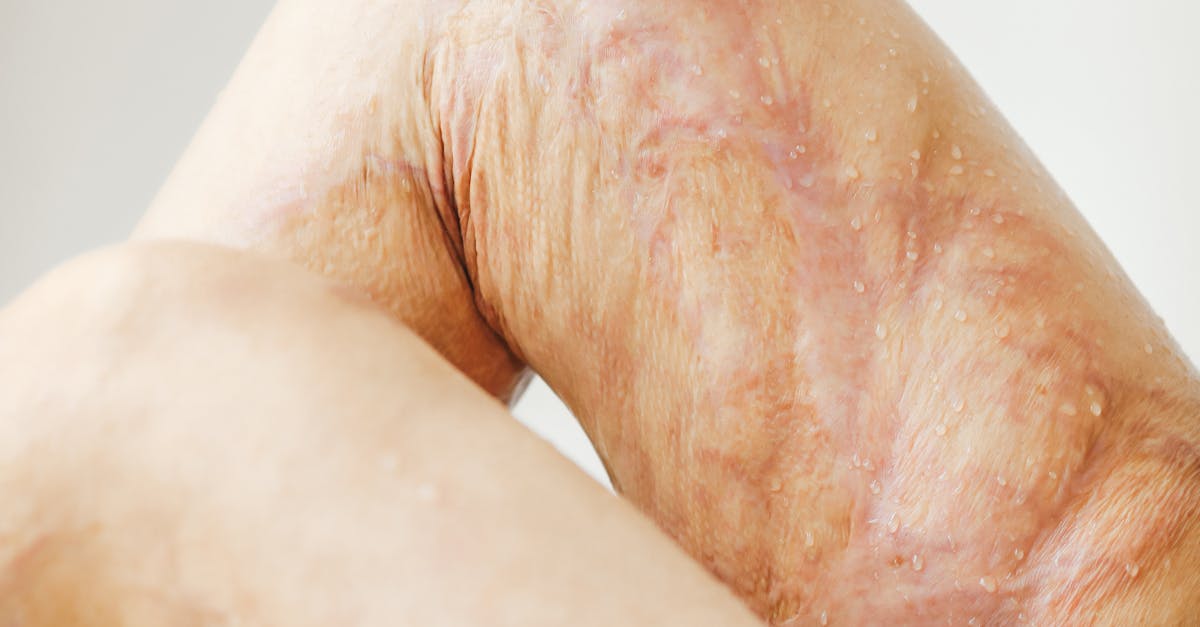
Carotenemia presents as a distinctive yellow-orange discoloration of the skin, particularly noticeable on the palms, soles, and nasolabial folds, resulting from elevated levels of carotenoids in the blood due to excessive dietary intake of carotenoid-rich foods or impaired carotenoid metabolism. This benign condition most commonly occurs in individuals who consume large quantities of orange and yellow vegetables such as carrots, sweet potatoes, squash, and leafy green vegetables, leading to carotenoid accumulation in adipose tissue and the stratum corneum of the skin. The clinical presentation of carotenemia differs significantly from jaundice in that the sclera remains clear and white, providing a crucial diagnostic distinction that helps healthcare providers differentiate between benign dietary carotenemia and potentially serious conditions causing hyperbilirubinemia. Carotenemia can also develop in association with certain medical conditions that affect carotenoid metabolism, including diabetes mellitus, hypothyroidism, liver disease, and kidney disease, where impaired conversion of carotenoids to vitamin A or altered lipid metabolism may contribute to carotenoid accumulation. Infants and young children may develop carotenemia more readily than adults due to their smaller body size and tendency to consume carotenoid-rich baby foods, particularly those containing carrots, sweet potatoes, or squash as primary ingredients. The condition is entirely reversible with dietary modification, typically resolving within several weeks to months after reducing carotenoid intake, making it important for healthcare providers to reassure patients about the benign nature of this cosmetic change. Healthcare providers should consider carotenemia in the differential diagnosis of yellow skin discoloration, particularly in health-conscious individuals following diets high in fruits and vegetables, vegetarians, or those taking carotenoid supplements for their antioxidant properties. The recognition of carotenemia prevents unnecessary laboratory testing and patient anxiety while providing an opportunity to discuss balanced nutrition and the potential for even beneficial nutrients to cause visible changes when consumed in excessive quantities.
10. Purpura - Purple Patches and Bleeding Disorders
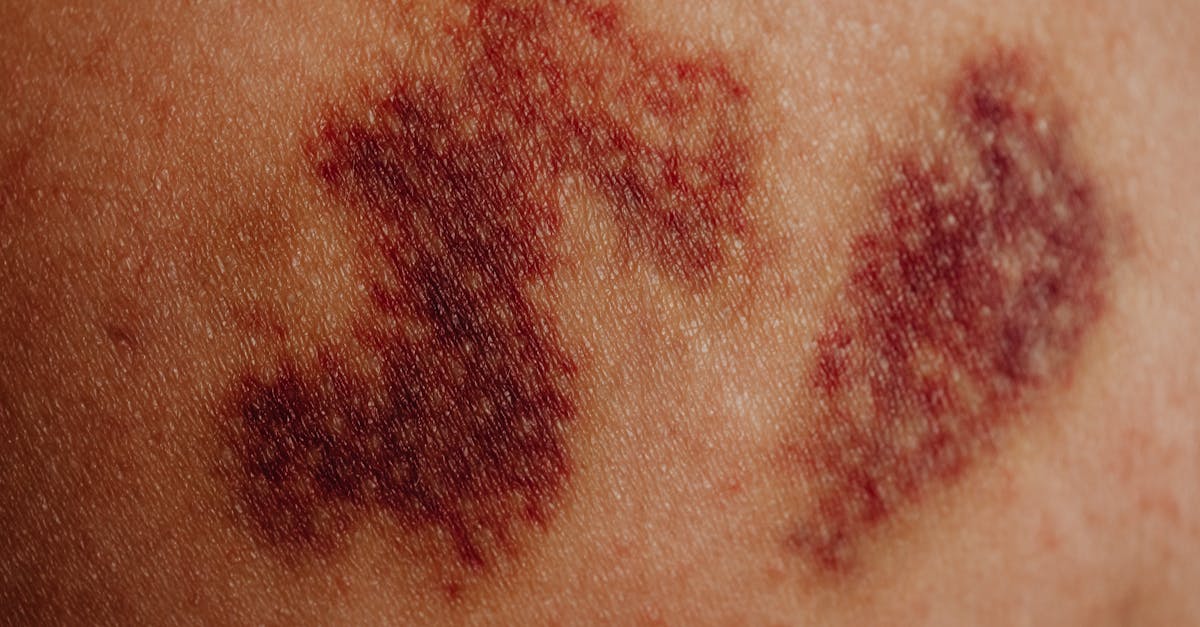
Purpura manifests as purple or reddish-brown discoloration of the skin resulting from bleeding into the dermis or subcutaneous tissues, serving as a crucial indicator of various bleeding disorders, vascular abnormalities, or platelet dysfunction that requires careful medical evaluation. This non-blanching discoloration occurs when red blood cells extravasate from damaged or fragile blood vessels into surrounding tissues, creating characteristic purple patches that can range from small pinpoint lesions called petechiae to larger areas of discoloration known as ecchymoses or bruises. The clinical assessment of purpura involves evaluating the size, distribution, and associated symptoms to help determine the underlying cause, with petechiae typically indicating platelet disorders or capillary fragility, while larger purpuric lesions may suggest coagulation defects or more significant vascular damage. Thrombocytopenic purpura results from decreased platelet counts due to conditions such as idiopathic thrombocytopenic purpura, drug-induced thrombocytopenia, or bone marrow disorders, typically presenting with widespread petechiae and easy bruising that may be accompanied by bleeding from mucous membranes. Non-thrombocytopenic purpura can occur in conditions affecting platelet function despite normal platelet counts, such as aspirin use, uremia, or inherited platelet disorders, or may result from vascular abnormalities including vasculitis, scurvy, or age-related capillary fragility.