12 Knuckle and Joint Appearance Changes Linked to Inflammatory Conditions
The human hand serves as a remarkable diagnostic window into systemic inflammatory conditions, with knuckles and joints acting as early indicators of underlying pathological processes. When inflammatory diseases take hold, they often manifest through subtle yet distinctive changes in joint appearance that can precede more severe symptoms by months or even years. These visual transformations—ranging from subtle swelling and discoloration to dramatic deformities—represent the body's inflammatory response gone awry, affecting the delicate balance of synovial fluid, cartilage integrity, and surrounding soft tissues. Understanding these twelve key appearance changes not only empowers individuals to seek timely medical intervention but also provides healthcare professionals with crucial visual clues for accurate diagnosis and treatment planning. From the characteristic swan-neck deformities of rheumatoid arthritis to the tophi deposits of gout, each inflammatory condition leaves its unique signature on the joints, creating a complex but decipherable pattern that reflects the underlying disease process and its progression over time.
1. Synovial Swelling - The First Warning Sign

Synovial swelling represents one of the earliest and most common visual indicators of joint inflammation, occurring when the synovial membrane becomes thickened and produces excess fluid in response to inflammatory triggers. This swelling typically manifests as a soft, boggy enlargement around the affected joints, particularly noticeable in the proximal interphalangeal (PIP) and metacarpophalangeal (MCP) joints of the fingers. The swelling often has a characteristic spongy feel when palpated and may fluctuate in severity throughout the day, frequently being most pronounced in the morning hours due to overnight fluid accumulation. Research indicates that synovial swelling can precede other inflammatory symptoms by several weeks, making it a crucial early warning system for conditions such as rheumatoid arthritis, psoriatic arthritis, and systemic lupus erythematosus. The appearance may range from subtle puffiness that obscures normal joint contours to dramatic enlargement that significantly alters hand function and grip strength, often accompanied by warmth and tenderness that reflects the active inflammatory process occurring within the joint capsule.
2. Erythema and Skin Discoloration - Visual Markers of Inflammation
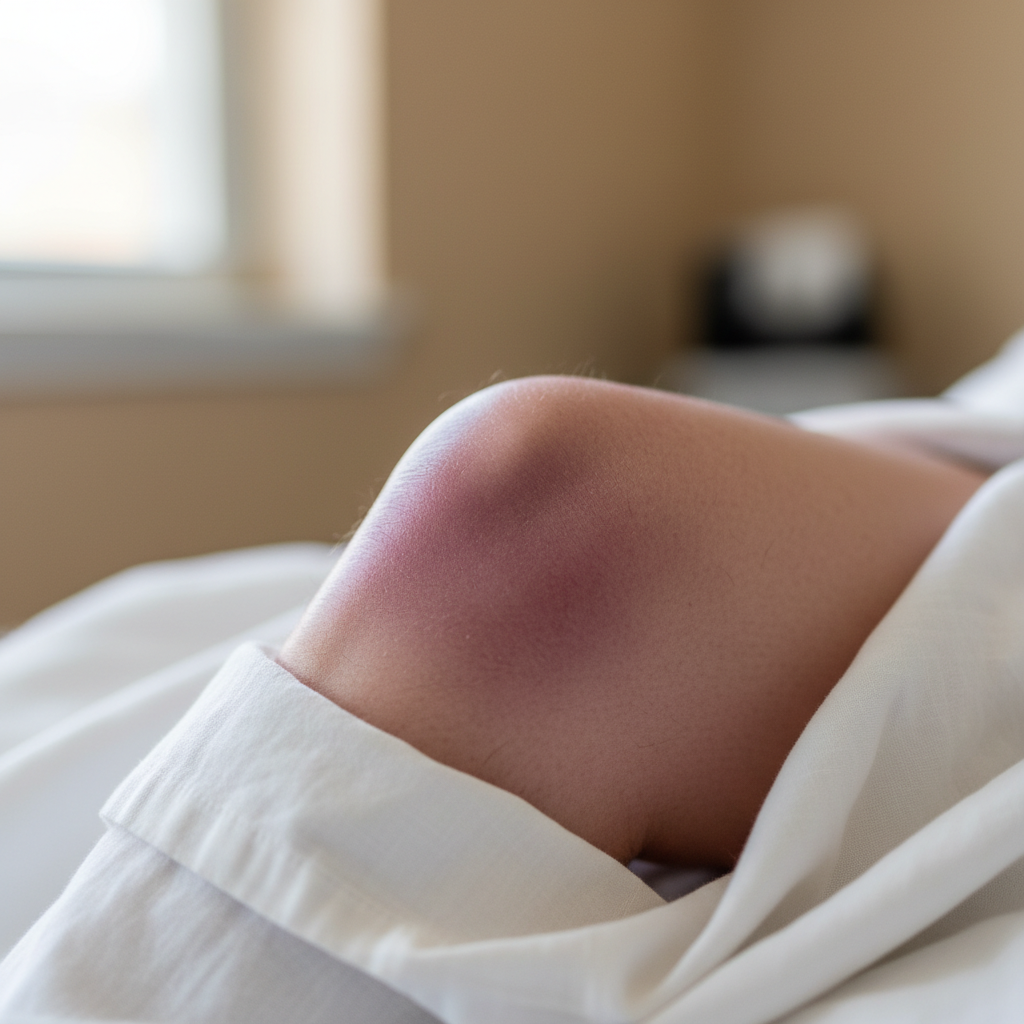
The skin overlying inflamed joints frequently displays characteristic color changes that serve as external manifestations of internal inflammatory processes, with erythema being the most common presentation. This reddening occurs due to vasodilation and increased blood flow to the affected area, creating a warm, flushed appearance that may extend beyond the immediate joint boundaries. In acute inflammatory conditions like gouty arthritis, the erythema can be particularly intense, sometimes appearing almost purple or burgundy in color, while chronic conditions may present with a more subtle, persistent pink or salmon-colored discoloration. Certain inflammatory arthritides produce distinctive color patterns, such as the violaceous discoloration seen in dermatomyositis or the characteristic "heliotrope" rash that may accompany joint involvement. The intensity and distribution of skin discoloration often correlate with disease activity levels, providing clinicians with a visual gauge of inflammatory burden. Additionally, some patients may experience livedo reticularis, a net-like pattern of skin discoloration that can indicate underlying vasculitis or autoimmune conditions affecting both joints and vascular structures.
3. Joint Deformities - Structural Consequences of Chronic Inflammation

Prolonged inflammatory processes can lead to irreversible structural changes in joint architecture, resulting in characteristic deformities that vary depending on the underlying condition and affected anatomical structures. The swan-neck deformity, commonly associated with rheumatoid arthritis, involves hyperextension of the PIP joint combined with flexion of the distal interphalangeal (DIP) joint, creating a distinctive curved appearance reminiscent of a swan's neck. Boutonnière deformities present with the opposite pattern, featuring flexion of the PIP joint and extension of the DIP joint, often resulting from damage to the central slip of the extensor tendon mechanism. Ulnar deviation of the fingers at the MCP joints represents another hallmark of advanced rheumatoid arthritis, occurring when inflammatory damage weakens the supporting ligaments and allows the fingers to drift toward the ulnar side of the hand. These deformities not only create distinctive visual appearances but also significantly impact hand function, grip strength, and the ability to perform activities of daily living, making early recognition and intervention crucial for preventing permanent disability.
4. Nodular Formations - Inflammatory Deposits and Growths

Various inflammatory conditions produce characteristic nodular formations around joints, each with distinct appearances that can aid in differential diagnosis and disease monitoring. Rheumatoid nodules, perhaps the most well-known of these formations, typically appear as firm, non-tender subcutaneous masses that develop over pressure points such as the extensor surfaces of the forearms and hands. These nodules, which occur in approximately 20-30% of patients with rheumatoid arthritis, are composed of central areas of fibrinoid necrosis surrounded by inflammatory cells and can range in size from a few millimeters to several centimeters in diameter. Gouty tophi represent another distinctive type of nodular formation, consisting of crystalline uric acid deposits that appear as white or yellowish lumps beneath the skin, often with a chalky appearance when they ulcerate through the surface. Heberden's and Bouchard's nodes, associated with osteoarthritis, present as bony enlargements at the DIP and PIP joints respectively, creating a knobby appearance that reflects underlying osteophyte formation. These nodular changes not only provide diagnostic clues but also serve as markers of disease progression and treatment response.
5. Morning Stiffness and Joint Rigidity Patterns
The temporal pattern of joint stiffness, particularly the characteristic morning stiffness associated with inflammatory arthritis, creates distinctive visual presentations that can be observed through limited range of motion and altered hand positioning. Morning stiffness in inflammatory conditions typically lasts for more than one hour and affects multiple joints simultaneously, causing patients to hold their hands in protective positions that minimize discomfort. This prolonged stiffness results from overnight accumulation of inflammatory mediators and edema within the joint space, creating a gel-like consistency in the synovial fluid that requires time and movement to return to normal viscosity. The visual impact of morning stiffness includes clenched or partially flexed fingers, reduced finger extension, and difficulty with fine motor tasks such as buttoning clothes or writing. Unlike the brief stiffness associated with mechanical joint problems, inflammatory morning stiffness improves with activity and movement, creating a characteristic pattern where joints appear more mobile and functional as the day progresses. The severity and duration of morning stiffness often correlate with disease activity levels, making it both a diagnostic tool and a marker for monitoring treatment effectiveness.
6. Skin Texture Changes and Thickening
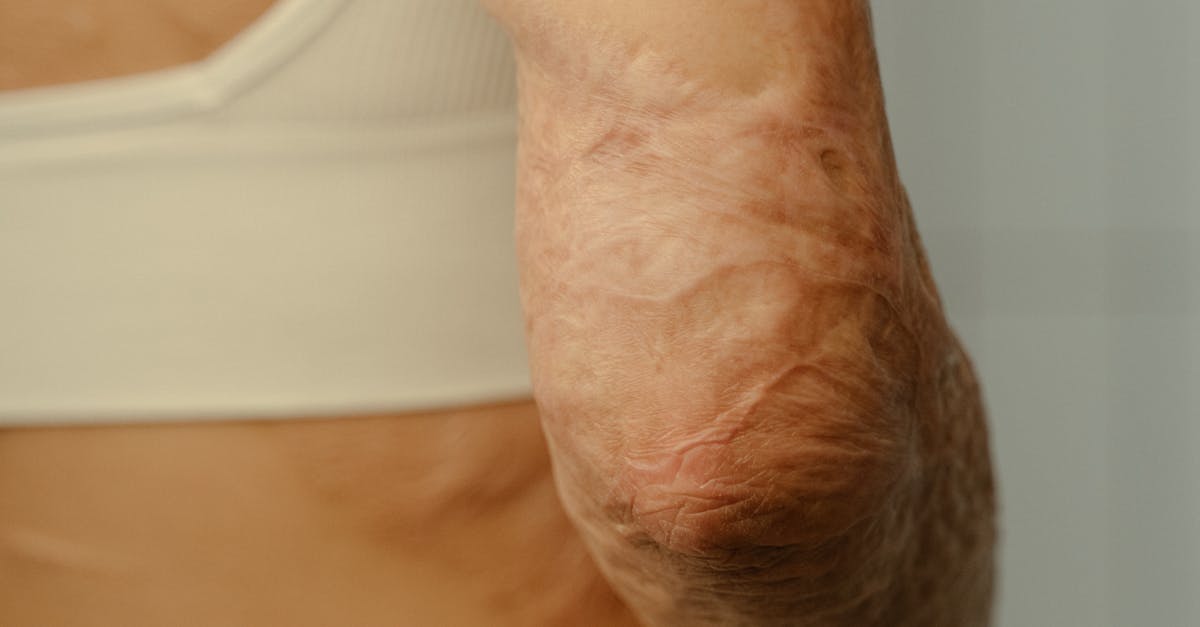
Inflammatory conditions affecting joints frequently produce distinctive changes in skin texture and thickness that extend beyond simple color alterations, creating characteristic tactile and visual presentations. Scleroderma, or systemic sclerosis, produces perhaps the most dramatic skin changes, with affected areas becoming tight, shiny, and bound down to underlying structures, creating a mask-like appearance in facial involvement and claw-like positioning of the fingers. The skin may develop a waxy, porcelain-like quality with loss of normal skin folds and creases, particularly noticeable over the knuckles and finger joints. Psoriatic arthritis often presents with characteristic silvery, scaly plaques over the extensor surfaces of joints, creating raised, well-demarcated lesions that may crack or bleed with movement. Dermatomyositis produces distinctive skin changes including Gottron's papules, which appear as raised, violaceous lesions over the knuckles and other bony prominences. These skin texture changes not only provide diagnostic clues but also impact joint mobility and function, as thickened or tight skin can restrict normal range of motion and contribute to the development of contractures over time.
7. Nail Changes and Periungual Involvement

The nails and surrounding tissues frequently reflect systemic inflammatory processes, producing characteristic changes that can precede or accompany joint involvement in various arthritides. Nail pitting, characterized by small punctate depressions in the nail plate, occurs in approximately 80% of patients with psoriatic arthritis and represents one of the strongest predictors of joint involvement in psoriasis patients. Oil drop or salmon patch discoloration appears as yellowish-brown spots beneath the nail plate, creating a distinctive appearance that correlates with the severity of underlying joint disease. Nail fold capillaroscopy may reveal characteristic patterns of capillary dilation, dropout, and hemorrhages that indicate underlying vasculitis or connective tissue diseases. Periungual erythema and swelling often accompany active inflammatory arthritis, creating a red, puffy appearance around the nail beds that may be particularly pronounced during disease flares. Onycholysis, or separation of the nail plate from the nail bed, can occur in psoriatic arthritis and other inflammatory conditions, creating a characteristic lifting appearance at the free edge of the nail. These nail changes not only provide diagnostic information but also serve as easily monitored markers of disease activity and treatment response.
8. Vascular Changes and Circulation Patterns
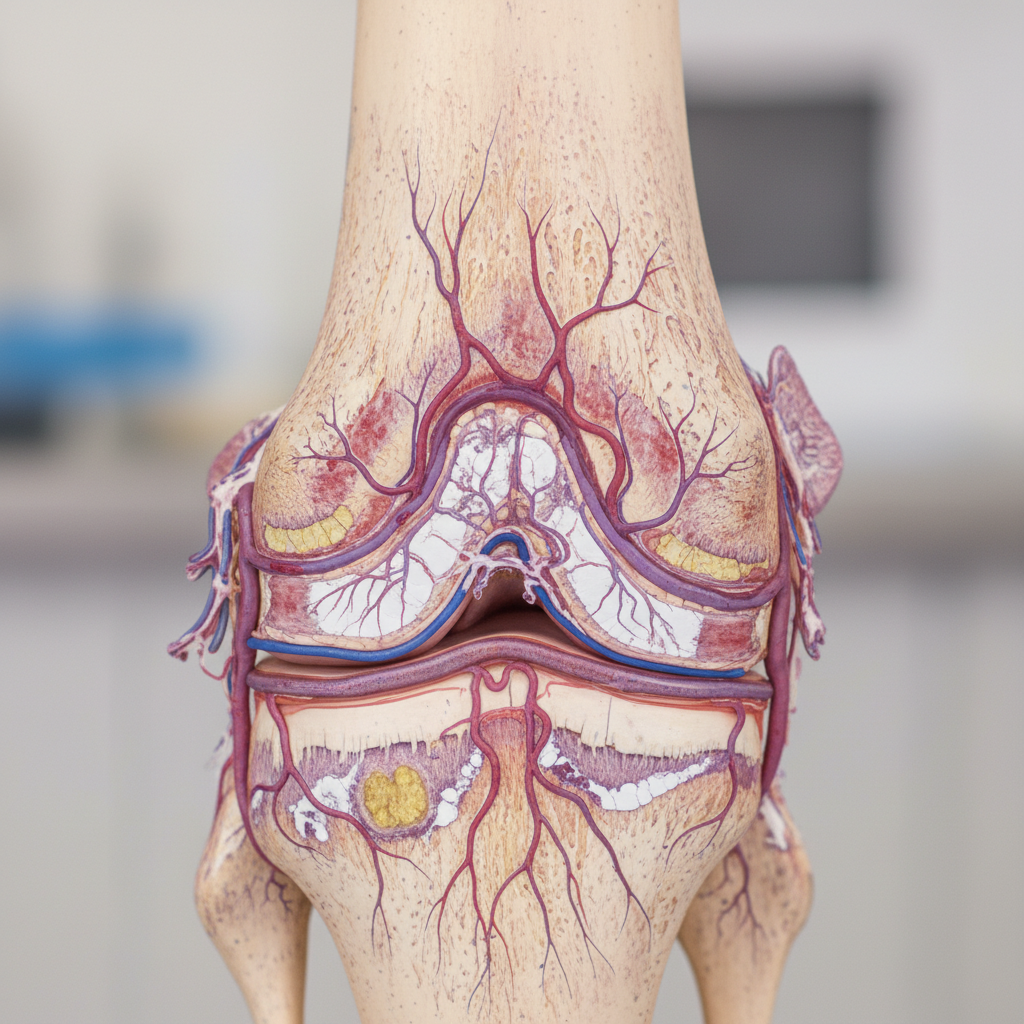
Inflammatory arthritis frequently affects the microvasculature around joints, producing distinctive vascular changes that can be observed through various visual manifestations and circulation patterns. Raynaud's phenomenon, characterized by episodic color changes in response to cold or stress, affects up to 90% of patients with systemic sclerosis and creates a characteristic triphasic color pattern of white (ischemia), blue (cyanosis), and red (reperfusion). Digital ulcerations may develop as a consequence of severe vascular involvement, appearing as painful, punched-out lesions typically located over the fingertips or knuckles, often with surrounding erythema and potential for secondary infection. Splinter hemorrhages, visible as dark lines beneath the nail plates, can indicate underlying vasculitis or embolic phenomena associated with inflammatory conditions. Livedo reticularis presents as a net-like pattern of skin discoloration that may indicate underlying vasculitis or antiphospholipid syndrome. Capillary nail fold changes, observable through dermoscopy or simple magnification, may reveal enlarged, tortuous capillaries, areas of capillary dropout, or microhemorrhages that reflect systemic vascular involvement. These vascular manifestations not only contribute to the overall clinical picture but also may indicate more severe systemic involvement requiring aggressive treatment intervention.
9. Temperature Variations and Heat Distribution

The thermal characteristics of inflamed joints create distinctive patterns of heat distribution that can be observed through visual inspection and palpation, providing valuable diagnostic and monitoring information. Acute inflammatory conditions such as gouty arthritis or septic arthritis typically produce intense local heat that may be visible as erythema and palpable as increased skin temperature over the affected joint. Infrared thermography studies have demonstrated that inflamed joints consistently show elevated surface temperatures compared to unaffected areas, with temperature differences often correlating with disease activity levels and inflammatory burden. The pattern of heat distribution can help differentiate between various inflammatory conditions, as some diseases produce diffuse warmth across multiple joints while others create focal hot spots over specific anatomical locations. Chronic inflammatory conditions may show less dramatic temperature elevation but often maintain a persistent low-grade warmth that reflects ongoing inflammatory activity. The temporal pattern of temperature changes throughout the day can also provide diagnostic clues, with some conditions showing peak warmth during morning hours while others demonstrate increased heat with activity or stress. These thermal patterns not only aid in diagnosis but also serve as non-invasive markers for monitoring treatment response and disease progression.
10. Functional Limitations and Movement Restrictions

The visual assessment of hand and finger function provides crucial insights into the impact of inflammatory joint changes on daily activities and quality of life. Grip strength limitations become visually apparent through compensatory movements and altered hand positioning during functional tasks, with patients often developing characteristic adaptive strategies to accommodate joint pain and stiffness. Pinch grip dysfunction manifests as difficulty with precision tasks, observable through tremor, instability, or complete inability to perform fine motor activities such as picking up small objects or writing. Range of motion restrictions create distinctive visual patterns, with affected joints showing limited excursion during active movement and characteristic positioning at rest to minimize discomfort. The inability to make a complete fist or fully extend the fingers creates easily recognizable visual signs that correlate with underlying joint pathology and inflammation severity. Functional deformities may develop as patients unconsciously position their hands to avoid painful movements, leading to secondary contractures and further limitation of normal joint mechanics. These functional limitations not only impact quality of life but also provide objective measures for assessing disease progression and treatment effectiveness, making careful observation of movement patterns an essential component of comprehensive joint evaluation.
11. Asymmetric Patterns and Distribution Variations
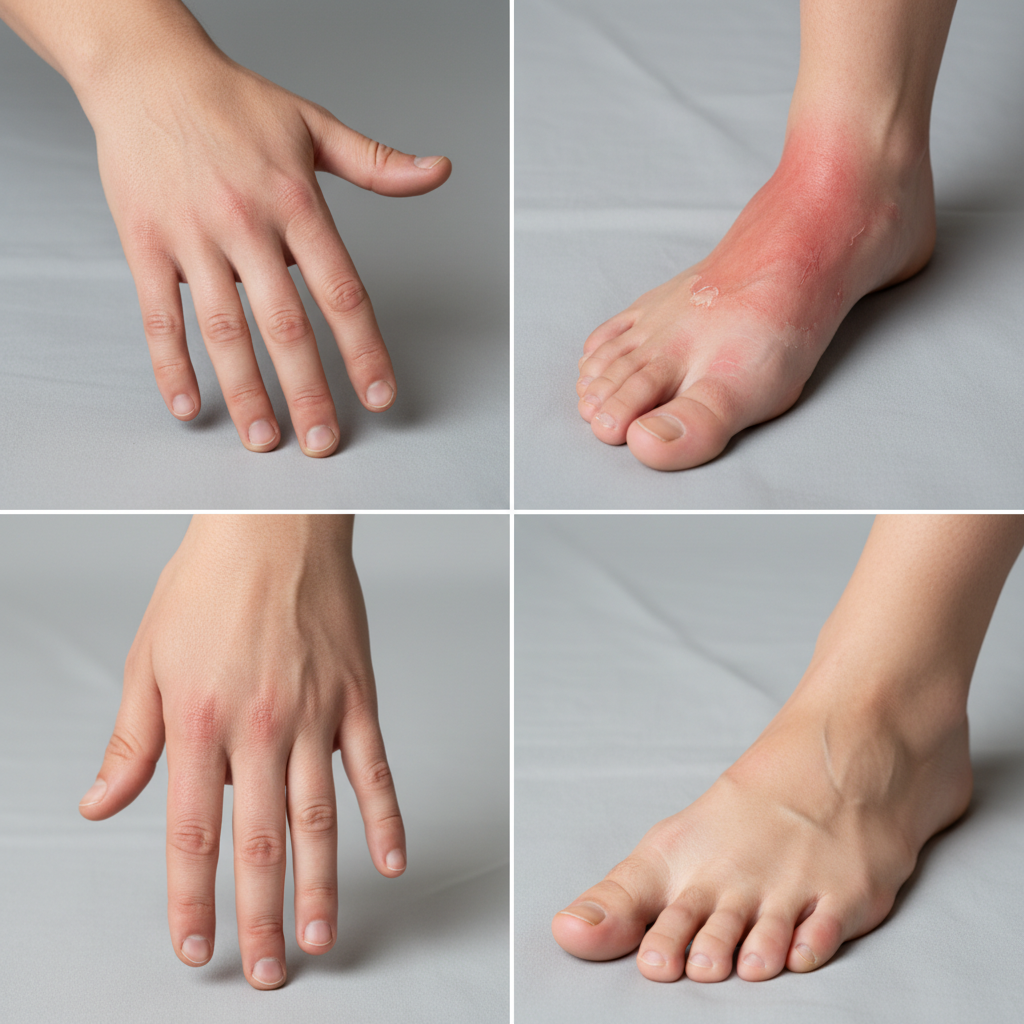
The pattern and distribution of joint involvement in inflammatory conditions create characteristic asymmetric presentations that provide valuable diagnostic information and help differentiate between various arthritides. Rheumatoid arthritis typically demonstrates a symmetric pattern of involvement, affecting corresponding joints on both sides of the body, while psoriatic arthritis often shows an asymmetric, oligoarticular pattern that may involve only one or a few joints on one side. The ray pattern of involvement, where all joints within a single finger are affected simultaneously, creates a distinctive "sausage digit" appearance characteristic of spondyloarthropathies. Distal interphalangeal joint predominance suggests psoriatic arthritis or osteoarthritis, while proximal interphalangeal and metacarpophalangeal involvement points toward rheumatoid arthritis or other inflammatory conditions. The temporal pattern of joint involvement also provides diagnostic clues, with some conditions showing additive patterns where new joints become involved over time, while others demonstrate a migratory pattern with inflammation moving from joint to joint. These distribution patterns not only aid in differential diagnosis but also help predict disease progression and guide treatment strategies, making careful documentation of involvement patterns essential for optimal patient management.
12. Progressive Changes and Disease Evolution
The evolution of joint appearance changes over time provides crucial insights into disease progression and treatment effectiveness, with certain inflammatory conditions showing characteristic patterns of advancement. Early inflammatory changes typically begin with subtle swelling and erythema that may be intermittent and easily overlooked, gradually progressing to more persistent and obvious visual manifestations as the disease becomes established. The transition from reversible inflammatory changes to irreversible structural damage represents a critical threshold in disease progression, with early intervention being essential for preventing permanent deformity and functional loss. Photographic documentation of joint changes over time has become an invaluable tool for tracking disease progression and treatment response, allowing for objective comparison of appearance changes that might otherwise be difficult to quantify. Certain conditions show predictable patterns of progression, such as the characteristic sequence of joint involvement in rheumatoid arthritis or the typical evolution of tophi formation in chronic gout. The rate of progression varies significantly between individuals and conditions, with some patients showing rapid advancement over months while others maintain stable appearance for years. Understanding these progressive patterns helps clinicians anticipate future changes, adjust treatment strategies proactively, and counsel patients about expected disease course and prognosis.
13. Clinical Significance and Diagnostic Implications
The recognition and interpretation of knuckle and joint appearance changes carry profound clinical significance for early diagnosis, treatment planning, and long-term disease management in inflammatory conditions. These visual manifestations often represent the earliest detectable signs of systemic inflammatory diseases, providing opportunities for intervention before irreversible damage occurs and significantly impacting long-term patient outcomes. The specificity of certain appearance changes for particular conditions enables clinicians to narrow differential diagnoses and pursue targeted diagnostic testing, reducing the time to accurate diagnosis and appropriate treatment initiation. The correlation between visual changes and disease activity levels makes joint appearance assessment a valuable tool for monitoring treatment response and adjusting therapeutic interventions, particularly in resource-limited settings where sophisticated laboratory testing may not be readily available. Patient education regarding these appearance changes empowers individuals to recognize early warning signs and seek timely medical attention, potentially preventing disease progression and preserving joint function. The integration of joint appearance assessment with other clinical findings, laboratory results, and imaging studies creates a comprehensive diagnostic approach that maximizes accuracy and guides evidence-based treatment decisions. Furthermore, the documentation and tracking of these visual changes over time provides valuable prognostic information and helps establish realistic treatment goals and expectations for both patients and healthcare providers, ultimately contributing to improved quality of life and functional outcomes in individuals living with inflammatory joint conditions.