12 Fingertip and Palm Changes That Doctors Note During Physical Examinations
The human hand serves as a remarkable diagnostic window into overall health, offering physicians invaluable insights that extend far beyond orthopedic concerns. During comprehensive physical examinations, experienced clinicians meticulously observe fingertips and palms for subtle yet significant changes that can indicate underlying systemic diseases, nutritional deficiencies, circulatory disorders, and metabolic conditions. These dermatological and structural manifestations often precede more obvious symptoms, making hand examination a crucial component of early disease detection. From the characteristic clubbing of fingertips that signals respiratory or cardiac pathology to the distinctive palmar creases associated with genetic disorders, each change tells a story about the body's internal state. Modern medical practice recognizes that the hands, with their rich vascular supply, sensitive nerve endings, and constant exposure to environmental factors, serve as sensitive barometers of health. This comprehensive exploration delves into twelve specific fingertip and palm changes that astute physicians routinely assess, examining their clinical significance, underlying pathophysiology, and diagnostic implications. Understanding these manifestations empowers healthcare providers to make more accurate diagnoses while highlighting the sophisticated interconnectedness of human anatomy and the body's remarkable ability to communicate distress through visible signs.
1. Digital Clubbing - Windows to Respiratory and Cardiac Health
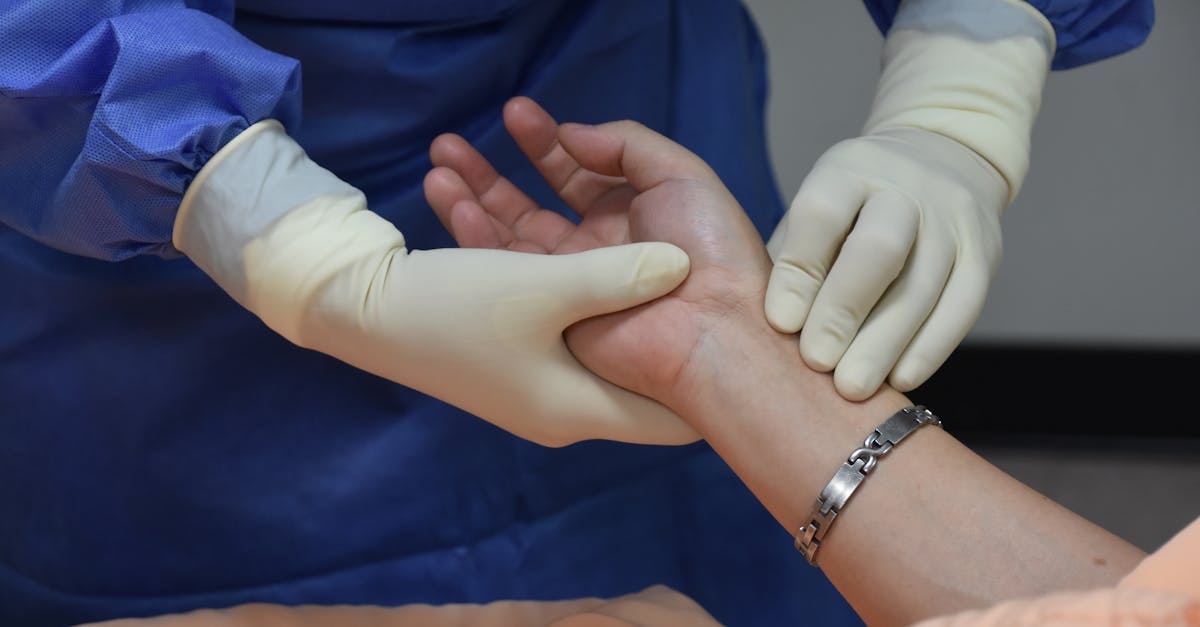
Digital clubbing represents one of the most clinically significant fingertip changes that physicians encounter during physical examinations, characterized by the distinctive enlargement and rounding of fingertip soft tissues accompanied by nail changes. This phenomenon occurs when chronic hypoxemia or other pathological processes trigger increased vascular proliferation and connective tissue growth in the distal digits. The classic presentation includes loss of the normal angle between the nail and nail bed (Lovibond's angle), increased nail curvature both longitudinally and transversely, and a spongy feel to the nail bed upon palpation. Clubbing typically develops gradually over months to years and most commonly indicates underlying pulmonary conditions such as lung cancer, chronic obstructive pulmonary disease, pulmonary fibrosis, or bronchiectasis. However, cardiovascular causes including congenital heart disease with right-to-left shunting, infective endocarditis, and certain congenital cardiac malformations can also produce this finding. Additionally, gastrointestinal disorders like inflammatory bowel disease, liver cirrhosis, and malabsorption syndromes may manifest with digital clubbing. The degree of clubbing often correlates with disease severity and duration, making it not only a diagnostic tool but also a marker for monitoring disease progression and treatment response.
2. Cyanosis - Revealing Oxygenation and Circulation Issues

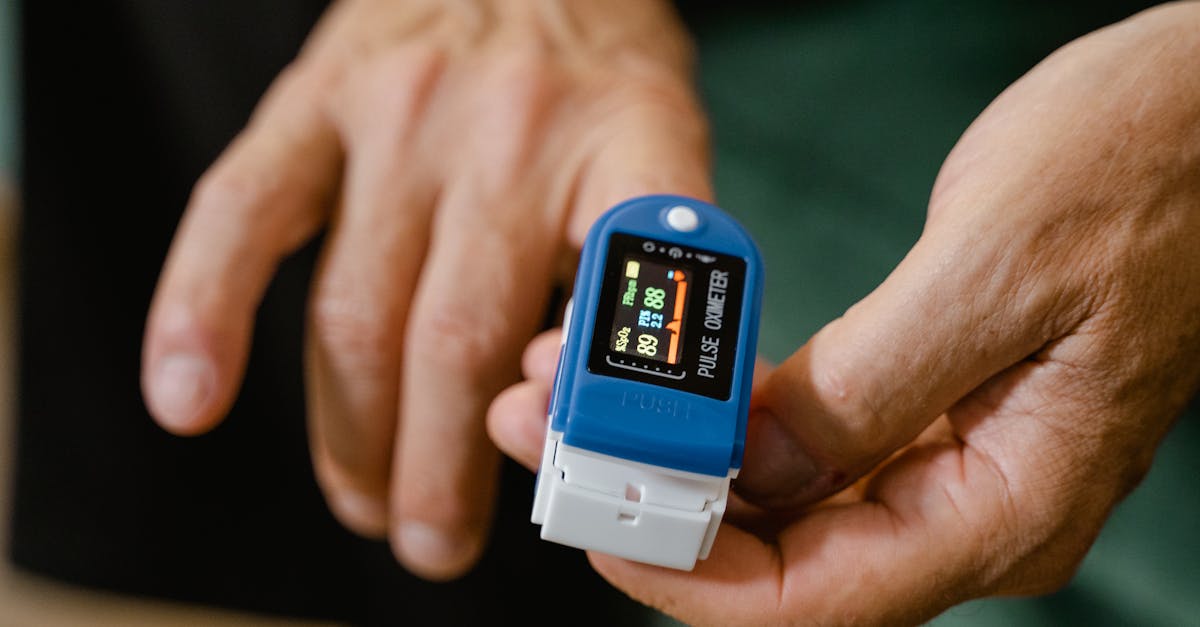
Cyanosis of the fingertips and nail beds provides immediate visual evidence of compromised oxygenation or circulation, appearing as a bluish or purplish discoloration that skilled physicians can detect even in subtle presentations. This color change results from increased concentrations of deoxygenated hemoglobin in the blood, typically becoming visible when deoxygenated hemoglobin levels exceed 5 grams per deciliter. Central cyanosis, affecting the entire body including fingertips, indicates serious systemic hypoxemia often caused by pulmonary diseases, congenital heart defects, or high-altitude exposure. Peripheral cyanosis, localized to extremities including fingertips, suggests reduced blood flow due to vasoconstriction, heart failure, or vascular disease. Temperature plays a crucial role in assessment, as cold-induced vasoconstriction can cause physiological peripheral cyanosis in healthy individuals. Physicians must differentiate between pathological and physiological cyanosis by considering patient history, ambient temperature, and associated symptoms. Chronic cyanosis may lead to compensatory polycythemia, further complicating the clinical picture. The rapid recognition of cyanosis during examination can prompt immediate interventions, particularly in acute settings where it may indicate respiratory failure, cardiac arrest, or severe circulatory compromise. Modern pulse oximetry complements visual assessment, but experienced clinicians understand that cyanosis can be detected before oxygen saturation measurements become critically low.
3. Koilonychia - Spoon-Shaped Nails and Systemic Deficiencies

Koilonychia, commonly known as spoon nails, presents as a distinctive concave deformity of the fingernails that creates a characteristic spoon-like appearance capable of holding a drop of water. This nail dystrophy represents one of the most recognizable signs of iron deficiency anemia, though it can also indicate other systemic conditions affecting nail matrix function. The pathophysiology involves disrupted keratin synthesis and nail plate formation due to inadequate iron availability for cellular metabolism and protein production. While mild koilonychia may occur normally in infants and young children due to soft nail plates, persistent or severe spooning in adults warrants investigation for underlying iron deficiency, chronic blood loss, malabsorption disorders, or dietary insufficiency. Beyond iron deficiency, koilonychia can accompany other conditions including hemochromatosis (paradoxically), Raynaud's disease, systemic lupus erythematosus, and certain occupational exposures to petroleum products or strong detergents. The severity of spooning often correlates with the duration and extent of iron deficiency, with mild cases showing subtle flattening progressing to pronounced concavity in severe deficiency. Physicians assess koilonychia by observing the nail contour from multiple angles and may perform the water drop test to confirm the diagnosis. Treatment involves addressing the underlying cause, typically iron supplementation for deficiency states, with nail morphology gradually normalizing over several months as new nail growth replaces the affected tissue.
4. Palmar Erythema - Vascular Changes and Liver Function
Palmar erythema manifests as distinctive reddening of the palms, particularly prominent over the thenar and hypothenar eminences, representing an important clinical sign that physicians associate with various systemic conditions, most notably liver disease. This vascular phenomenon results from increased blood flow through dilated capillaries and arteriovenous anastomoses in the palmar skin, creating the characteristic warm, red appearance that blanches with pressure. The pathophysiology involves altered estrogen metabolism and increased circulating vasodilatory substances, explaining why palmar erythema commonly occurs in liver cirrhosis where hepatic clearance of hormones and vasoactive compounds becomes impaired. However, physicians must consider other causes including pregnancy, hyperthyroidism, rheumatoid arthritis, chronic obstructive pulmonary disease, and certain medications such as albuterol or cholestyramine. Physiological palmar erythema can occur during pregnancy due to increased estrogen levels and enhanced cardiac output, typically resolving postpartum. The intensity and distribution of erythema may correlate with disease severity, particularly in liver disease where it often accompanies other stigmata of chronic liver dysfunction such as spider angiomata, gynecomastia, and testicular atrophy. Careful examination requires adequate lighting and comparison with normal skin areas, as subtle erythema may be missed in poor lighting conditions. The presence of palmar erythema should prompt comprehensive evaluation of liver function, thyroid status, and other potential underlying conditions, making it a valuable screening tool during routine physical examinations.
5. Dupuytren's Contracture - Fascial Changes and Genetic Predisposition
Dupuytren's contracture represents a progressive fibroproliferative disorder of the palmar fascia that physicians can detect in its early stages through careful palpation and observation of subtle skin changes and nodule formation. This condition begins with the development of small, firm nodules in the palm, typically near the base of the ring and little fingers, progressing to form thick, cord-like bands that gradually contract and pull affected fingers into flexion. The pathophysiology involves abnormal proliferation and contraction of myofibroblasts within the palmar aponeurosis, leading to excessive collagen deposition and tissue remodeling. While the exact etiology remains unclear, strong genetic predisposition exists, particularly among individuals of Northern European descent, with additional risk factors including diabetes mellitus, alcohol consumption, smoking, and certain occupational exposures involving repetitive trauma or vibration. Early detection proves crucial as the condition typically progresses slowly over years, but the rate of progression varies significantly among individuals. Physicians assess the degree of contracture using standardized measurements and functional tests, documenting the angle of metacarpophalangeal and proximal interphalangeal joint flexion. The presence of Dupuytren's disease may indicate increased risk for similar fibromatoses affecting other body parts, including Peyronie's disease and plantar fibromatosis. Treatment options range from observation in mild cases to surgical intervention for severe contractures that significantly impair hand function, making early recognition and appropriate referral essential components of comprehensive hand examination.
6. Splinter Hemorrhages - Microvascular Clues to Systemic Disease

Splinter hemorrhages appear as thin, linear, reddish-brown streaks running longitudinally under the fingernails, representing microbleeds within the nail bed capillaries that provide important diagnostic clues about underlying vascular and systemic conditions. These distinctive lesions result from damage to the delicate capillary network beneath the nail plate, causing extravasation of blood that becomes trapped and visible through the translucent nail. While minor trauma represents the most common cause of isolated splinter hemorrhages, their presence in multiple nails or in patients without obvious trauma history should prompt investigation for more serious underlying conditions. Infective endocarditis classically produces splinter hemorrhages as part of its constellation of peripheral embolic phenomena, along with Osler nodes, Janeway lesions, and Roth spots. However, physicians must consider other causes including vasculitis, antiphospholipid syndrome, systemic lupus erythematosus, rheumatoid arthritis, and malignant hypertension. The location of splinter hemorrhages provides diagnostic information, with those near the nail base more likely indicating systemic disease, while distal lesions often result from trauma. Subacute bacterial endocarditis may produce subtle splinter hemorrhages that develop gradually, contrasting with the acute presentation of other embolic phenomena. Drug-induced causes include anticoagulant therapy, chemotherapy agents, and certain antibiotics that affect platelet function or vascular integrity. Careful documentation of the number, location, and appearance of splinter hemorrhages, combined with appropriate clinical correlation, helps physicians differentiate between benign traumatic causes and serious systemic diseases requiring immediate intervention.
7. Janeway Lesions - Embolic Phenomena and Cardiac Pathology
Janeway lesions manifest as small, painless, hemorrhagic macules on the palms and soles that represent pathognomonic signs of infective endocarditis, providing physicians with crucial diagnostic evidence of septic embolic phenomena. These distinctive lesions appear as flat, reddish or brownish spots measuring typically 1-4 millimeters in diameter, distinguished from other embolic manifestations by their painless nature and specific anatomical distribution. The pathophysiology involves septic emboli originating from infected cardiac valves that lodge in small arteries and capillaries of the hands and feet, causing localized infarction and hemorrhage without the intense inflammatory response seen in other embolic lesions. Named after Edward Janeway, who first described them in 1899, these lesions represent microabscesses within the skin and are considered pathognomonic for acute bacterial endocarditis, particularly when caused by highly virulent organisms such as Staphylococcus aureus. The presence of Janeway lesions indicates significant cardiac involvement and active bacterial seeding, often accompanying other major criteria for endocarditis diagnosis including positive blood cultures and echocardiographic evidence of vegetation. Physicians must differentiate Janeway lesions from Osler nodes, which are typically painful, raised, and located on finger pads, representing immune complex vasculitis rather than septic emboli. The transient nature of Janeway lesions, often lasting only days to weeks, requires prompt recognition during physical examination. Their identification should trigger immediate evaluation for endocarditis, including blood cultures, echocardiography, and comprehensive cardiac assessment, as they indicate active infection requiring urgent antibiotic therapy and potential surgical intervention.
8. Osler Nodes - Immunological Responses in Fingertip Pathology
Osler nodes present as painful, tender, raised lesions on the fingertips and toe pads that represent immune-mediated vasculitic phenomena associated with subacute bacterial endocarditis and other systemic conditions. These distinctive nodules, typically measuring 2-15 millimeters in diameter, appear as erythematous to violaceous raised lesions that are exquisitely tender to palpation, distinguishing them from other embolic manifestations by their prominent pain and specific anatomical location on the pulp of digits. The pathophysiology involves immune complex deposition and subsequent vasculitis rather than direct septic embolization, explaining their painful nature and longer duration compared to Janeway lesions. Originally described by Sir William Osler in his classic descriptions of endocarditis, these lesions typically occur in subacute endocarditis caused by organisms of lower virulence such as viridans group streptococci or HACEK organisms. The immune-mediated nature of Osler nodes means they may persist for days to weeks, providing a longer diagnostic window compared to other transient embolic phenomena. Beyond endocarditis, physicians must consider other causes of similar lesions including systemic lupus erythematosus, antiphospholipid syndrome, cholesterol emboli syndrome, and certain vasculitic conditions. The bilateral and multiple occurrence of Osler nodes increases their diagnostic significance, particularly when accompanied by other clinical features suggestive of endocarditis such as fever, new heart murmur, or positive blood cultures. Careful palpation technique is essential for detection, as the tenderness may cause patients to withdraw their hands during examination. The presence of Osler nodes should prompt comprehensive evaluation for endocarditis and other systemic inflammatory conditions, including detailed cardiac assessment and laboratory investigation for autoimmune disorders.
9. Terry's Nails - Systemic Disease Indicators in Nail Bed Changes
Terry's nails represent a distinctive nail abnormality characterized by a white or pale nail bed with a narrow band of normal pink coloration at the distal tip, creating a pathognomonic appearance that alerts physicians to potential underlying systemic diseases. This nail dystrophy affects the majority of the nail bed, typically involving 80% or more of the nail surface, with only a thin rim of 1-2 millimeters of normal pink nail bed visible near the free edge. The pathophysiology involves decreased vascularity and increased connective tissue in the nail bed, resulting from various systemic conditions that affect microcirculation and tissue perfusion. Liver cirrhosis represents the most common association with Terry's nails, occurring in approximately 80% of patients with advanced hepatic disease, making this finding a valuable clinical marker for hepatic dysfunction. However, physicians must consider other systemic conditions including congestive heart failure, diabetes mellitus, chronic kidney disease, malnutrition, and aging, all of which can produce similar nail bed changes through different pathophysiological mechanisms. The bilateral and symmetric presentation of Terry's nails increases their diagnostic significance, as unilateral changes more commonly result from local trauma or infection. Age-related changes can produce similar appearances in elderly patients without underlying disease, requiring careful clinical correlation and consideration of other systemic symptoms. The presence of Terry's nails should prompt comprehensive evaluation of liver function, cardiac status, renal function, and nutritional status, particularly when accompanied by other clinical signs of systemic disease. Unlike other nail abnormalities that may resolve with treatment of underlying conditions, Terry's nails often persist even after successful treatment of the associated systemic disease, reflecting permanent structural changes in the nail bed architecture.
10. Muehrcke's Lines - Protein Status and Renal Function Indicators
Muehrcke's lines manifest as distinctive paired white horizontal bands across the fingernails that provide physicians with valuable insights into protein metabolism and renal function, representing one of the most specific nail signs associated with hypoalbuminemia. These characteristic lines appear as narrow, white, transverse bands that typically occur in pairs and extend across the entire width of the nail, distinguished from other nail abnormalities by their specific appearance and association with serum albumin levels. The pathophysiology involves altered nail bed perfusion and protein synthesis related to hypoalbuminemia, with the lines representing areas of decreased nail bed vascularity that appear white against the normal pink background. Named after Robert Muehrcke, who first described them in 1956, these lines most commonly occur when serum albumin levels fall below 2.2 g/dL, making them reliable indicators of significant protein deficiency or loss. Nephrotic syndrome represents the classic association with Muehrcke's lines, where massive proteinuria leads to severe hypoalbuminemia and the characteristic nail changes. However, physicians must consider other causes of hypoalbuminemia including liver disease, malnutrition, inflammatory conditions, and protein-losing enteropathy. The reversible nature of Muehrcke's lines distinguishes them from other nail abnormalities, as they typically disappear when serum albumin levels normalize with appropriate treatment. Unlike Beau's lines, which represent grooves in the nail plate itself, Muehrcke's lines affect only the nail bed and disappear when pressure is applied to the nail, helping physicians differentiate between these conditions during examination. The presence of Muehrcke's lines should prompt immediate evaluation of protein status, renal function, and liver function, as they may indicate serious underlying conditions requiring prompt intervention.
11. Raynaud's Phenomenon - Vascular Reactivity in Digital Circulation

Raynaud's phenomenon presents as episodic color changes in the fingertips triggered by cold exposure or emotional stress, providing physicians with important information about vascular reactivity and potential underlying connective tissue diseases. This distinctive vascular response typically follows a characteristic triphasic color pattern: initial pallor (white) due to vasospasm and cessation of blood flow, followed by cyanosis