10 Neck Appearance Changes Associated With Thyroid and Lymph Node Issues
The human neck serves as a remarkable diagnostic window, offering visible clues to underlying thyroid and lymphatic system dysfunction that can significantly impact overall health and well-being. This complex anatomical region houses critical structures including the thyroid gland, numerous lymph node clusters, major blood vessels, and essential muscles that work in harmony to support vital physiological functions. When thyroid disorders such as hyperthyroidism, hypothyroidism, goiter, or thyroid cancer develop, or when lymphatic issues including infections, autoimmune conditions, or malignancies arise, the neck often displays characteristic physical changes that trained healthcare professionals and informed individuals can recognize. These visible manifestations range from subtle swelling and texture alterations to dramatic enlargements and color changes that may indicate serious underlying pathology. Understanding these ten key appearance changes—including thyroid gland enlargement, lymph node swelling, skin texture modifications, vascular prominence, muscle weakness effects, postural changes, breathing-related visible strain, swallowing difficulties, voice-related physical signs, and systemic manifestations—empowers individuals to seek timely medical evaluation and enables healthcare providers to make more accurate preliminary assessments. Early recognition of these neck appearance changes can be crucial for prompt diagnosis and treatment, potentially preventing complications and improving long-term health outcomes for patients experiencing thyroid or lymphatic system disorders.
1. Thyroid Gland Enlargement (Goiter) - The Most Recognizable Sign

Thyroid gland enlargement, medically termed goiter, represents perhaps the most immediately recognizable neck appearance change associated with thyroid dysfunction, manifesting as a visible swelling in the lower front portion of the neck that can range from barely perceptible to dramatically prominent. This enlargement occurs when the thyroid gland increases in size due to various underlying causes including iodine deficiency, autoimmune conditions like Hashimoto's thyroiditis or Graves' disease, thyroid nodules, or malignant growths within the gland tissue. The appearance of goiter can vary significantly depending on the underlying cause and duration of the condition, with some presenting as smooth, uniform enlargements while others display irregular, nodular surfaces that create an uneven neck contour. In cases of diffuse goiter, the entire thyroid gland enlarges symmetrically, creating a butterfly-shaped swelling that moves up and down with swallowing, while multinodular goiter produces a more irregular, bumpy appearance that may be more prominent on one side of the neck. The size of goiter can progress gradually over months or years, or in some cases, develop rapidly, particularly in instances of thyroid inflammation or malignancy. Patients may notice that clothing feels tighter around the neck area, or that necklaces and collared shirts become uncomfortable as the enlargement progresses. The visibility of goiter can also be affected by body habitus, neck length, and the position of the thyroid gland, with some individuals showing more obvious signs than others despite similar degrees of gland enlargement.
2. Lymph Node Swelling (Lymphadenopathy) - Immune System Indicators
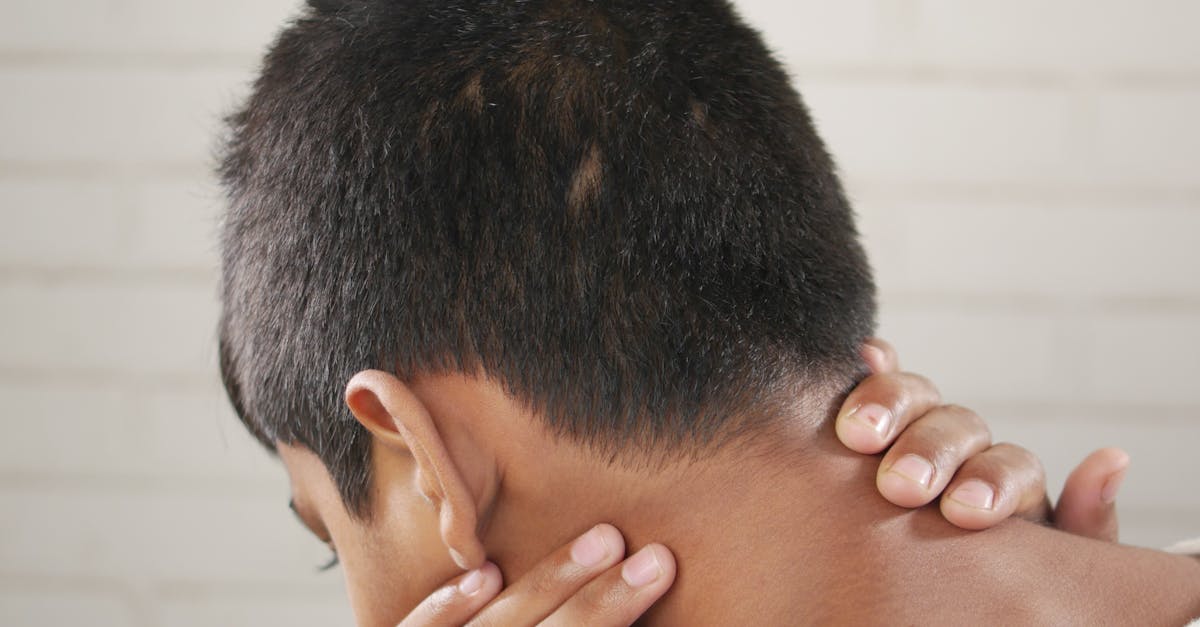
Lymph node enlargement in the neck region, known as cervical lymphadenopathy, creates distinctive appearance changes that can indicate various underlying conditions affecting the immune system, ranging from benign infections to serious malignancies requiring immediate medical attention. The neck contains multiple lymph node chains including the submandibular, submental, anterior cervical, posterior cervical, and supraclavicular groups, each of which can become enlarged and visible under different pathological circumstances. When lymph nodes swell due to infection, autoimmune conditions, or malignant infiltration, they typically appear as firm, rounded masses beneath the skin that may be mobile or fixed to surrounding tissues depending on the underlying cause. Reactive lymphadenopathy, commonly seen with upper respiratory infections, tends to produce tender, mobile nodes that feel soft to rubbery in consistency, while malignant involvement often creates harder, fixed masses that may be painless and continue growing despite treatment of apparent infections. The pattern of lymph node enlargement can provide important diagnostic clues, with bilateral involvement often suggesting systemic conditions like viral infections or autoimmune disorders, while unilateral enlargement may indicate localized infection or regional malignancy. In some cases, enlarged lymph nodes can become visible as obvious bumps or swellings along the sides of the neck, particularly in thin individuals or when the enlargement is significant. The skin overlying enlarged lymph nodes may appear normal, reddened, or even develop a stretched appearance when the nodes reach considerable size, and in cases of infection, the overlying skin might feel warm to the touch.
3. Skin Texture and Color Changes - Metabolic Manifestations
Thyroid dysfunction profoundly affects skin appearance throughout the body, with the neck region often displaying particularly noticeable changes in texture, color, and overall appearance that reflect the underlying metabolic disturbances characteristic of hyper- or hypothyroidism. In hyperthyroid conditions, the neck skin typically becomes warm, moist, and flushed due to increased metabolic rate and enhanced blood circulation, often displaying a smooth, almost velvety texture with increased sweating that may be particularly noticeable during physical examination or in warm environments. Conversely, hypothyroidism frequently produces cool, dry, and pale neck skin with a coarse, rough texture that may appear slightly thickened or puffy, particularly around the lower neck and supraclavicular areas where fluid retention commonly occurs. Patients with severe hypothyroidism may develop a characteristic yellowish tint to their skin due to carotenemia, a condition where beta-carotene accumulates in the skin when thyroid hormone deficiency impairs the conversion of carotene to vitamin A. Additionally, some individuals with autoimmune thyroid conditions may develop vitiligo, appearing as patches of depigmented skin that can be particularly noticeable on the neck due to the contrast with surrounding normal skin tone. The skin may also show signs of accelerated or delayed healing, with hyperthyroid patients experiencing faster wound healing but increased fragility, while hypothyroid individuals may notice slower healing and increased susceptibility to skin infections. In cases of thyroid storm or severe thyrotoxicosis, the neck skin may appear markedly flushed and feel extremely warm to the touch, while severe myxedema can produce a characteristic non-pitting edema that gives the skin a waxy, thickened appearance.
4. Vascular Prominence - Circulation and Pressure Effects
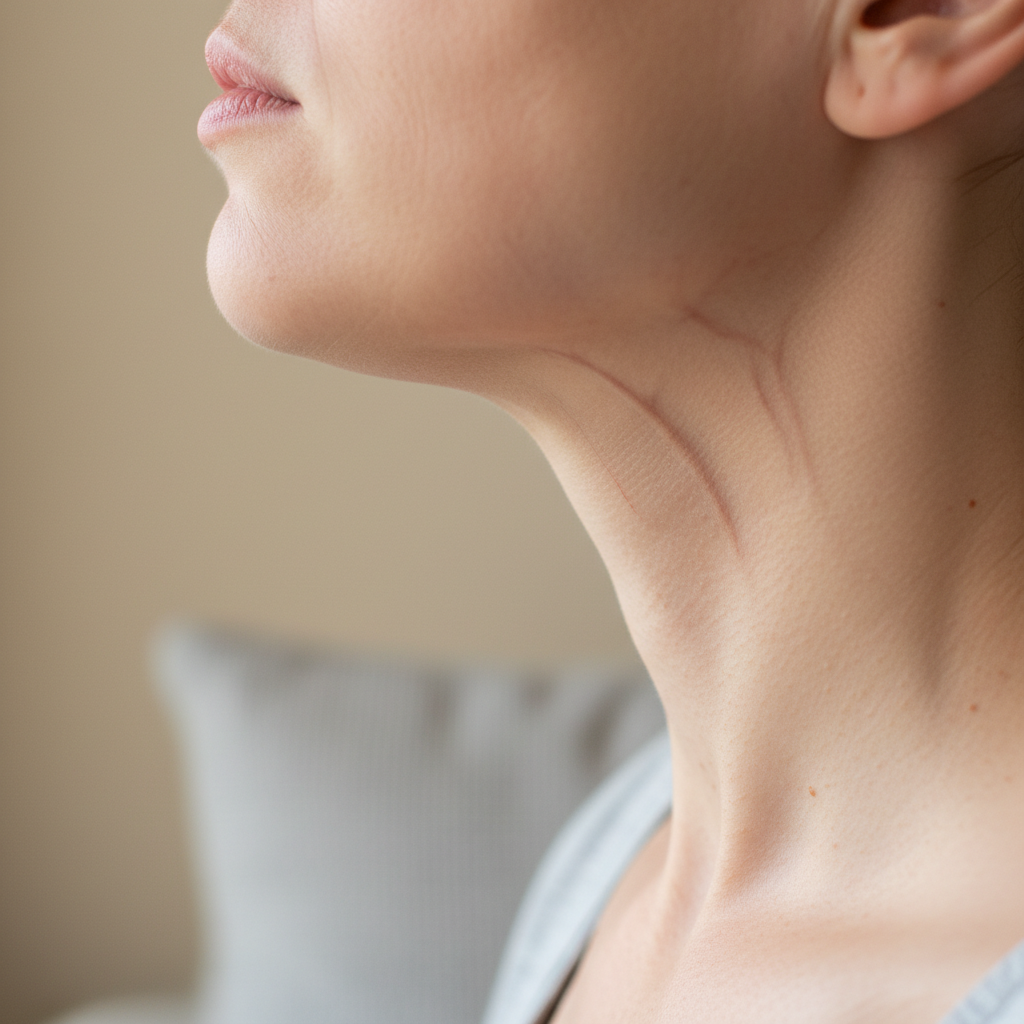
Thyroid disorders and lymphatic system dysfunction can create dramatic changes in neck vascular appearance, with blood vessels becoming more prominent, distended, or displaying abnormal pulsation patterns that reflect underlying circulatory and pressure changes within the neck region. In hyperthyroid conditions, increased cardiac output and enhanced circulation often make neck veins more visible and prominent, particularly the external jugular veins, which may appear engorged and pulsatile even when the patient is in an upright position. This vascular prominence results from the increased blood volume and enhanced cardiac contractility characteristic of thyrotoxicosis, combined with peripheral vasodilation that makes superficial vessels more apparent beneath the skin. Large goiters or significantly enlarged lymph node masses can compress major neck vessels, leading to venous congestion that manifests as distended, tortuous veins visible on the neck surface, particularly when the patient performs maneuvers that increase intrathoracic pressure such as coughing or straining. Superior vena cava syndrome, though rare, can occur with large thyroid masses or extensive lymphadenopathy, producing dramatic neck vein distension, facial swelling, and a characteristic plethoric appearance that represents a medical emergency requiring immediate intervention. The carotid arteries may also become more prominent in hyperthyroid patients due to increased stroke volume and pulse pressure, creating visible pulsations in the neck that may be accompanied by audible bruits during auscultation. In some cases, arteriovenous malformations or increased vascularity associated with thyroid cancer can create unusual vascular patterns or pulsatile masses that alter the normal neck contour and require careful evaluation to distinguish from other causes of neck swelling.
5. Muscle Weakness and Atrophy - Structural Support Changes
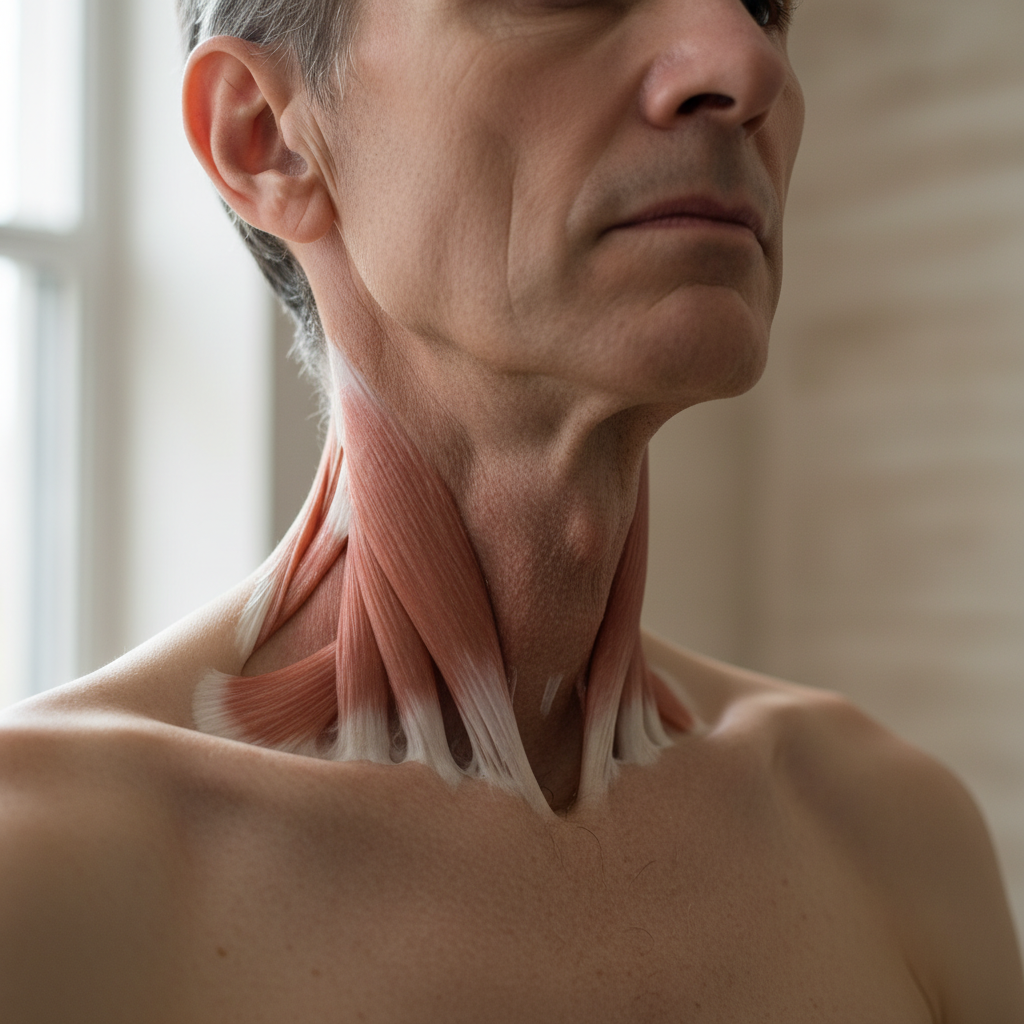
Thyroid dysfunction significantly impacts neck muscle strength, tone, and mass, creating visible changes in neck contour and support that can affect both appearance and function in ways that may be subtle initially but become increasingly apparent as the condition progresses. Hyperthyroidism commonly produces muscle weakness and wasting, particularly affecting the sternocleidomastoid muscles and other neck stabilizers, leading to a more prominent appearance of underlying bony structures and a general loss of the normal rounded neck contour. This muscle atrophy can create a more angular, defined appearance to the neck, with increased visibility of the clavicles, cervical spine processes, and other skeletal landmarks that are normally softened by adequate muscle mass. In severe cases of thyrotoxic myopathy, patients may develop significant weakness of the neck flexor and extensor muscles, leading to difficulty holding the head in normal positions and creating compensatory postural changes that further alter neck appearance. Hypothyroidism can produce the opposite effect, with muscle stiffness, cramping, and pseudohypertrophy that may initially make muscles appear larger but actually represent decreased functional capacity and altered muscle composition. The platysma muscle, which forms part of the superficial neck musculature, may become more prominent or develop unusual banding patterns in thyroid disease, particularly when patients experience weight loss or muscle wasting associated with hyperthyroidism. Additionally, chronic lymphadenopathy or large thyroid masses can compress or displace neck muscles, creating asymmetrical contours and altered muscle function that may be visible during neck movement or when patients attempt to turn their heads or swallow.
6. Postural and Alignment Changes - Compensatory Adaptations

Thyroid and lymphatic disorders often necessitate compensatory postural changes that create distinctive alterations in neck alignment, head position, and overall cervical spine posture that can be readily observed and may significantly impact both appearance and comfort. Large goiters, particularly those with substernal extension, commonly force patients to adopt a characteristic head-extended, chin-elevated posture to maintain adequate airway clearance and reduce the sensation of throat fullness or compression. This compensatory positioning creates an elongated neck appearance with increased cervical lordosis and may lead to secondary muscle tension and discomfort in the upper trapezius and suboccipital regions. Patients with significant lymphadenopathy may unconsciously tilt their heads away from the affected side to reduce pressure on enlarged nodes or to accommodate asymmetrical swelling, creating a characteristic head tilt that becomes more pronounced over time. In cases where thyroid masses or enlarged lymph nodes compress the trachea or esophagus, patients may adopt forward head posture with slight neck flexion to optimize breathing and swallowing function, though this positioning can create a hunched appearance and contribute to secondary musculoskeletal problems. Thyroid eye disease, commonly associated with Graves' disease, can indirectly affect neck posture as patients attempt to compensate for diplopia or visual disturbances by altering head position, creating unusual neck angles that may appear abnormal to observers. The weight and mass effect of large thyroid glands can also create a forward-pulling sensation that encourages forward head posture and rounded shoulders, fundamentally altering the normal cervical spine alignment and creating a characteristic appearance that experienced clinicians can recognize from a distance.
7. Breathing-Related Visible Changes - Respiratory Compensation
Thyroid enlargement and lymphatic masses in the neck can significantly impact respiratory function, creating visible changes in breathing patterns, neck muscle recruitment, and overall respiratory effort that become increasingly apparent as airway compromise progresses. Large goiters, particularly those with retrosternal extension, may compress the trachea and create inspiratory stridor that is accompanied by visible supraclavicular and intercostal retractions during inspiration, giving the neck a characteristic "sucked-in" appearance during breathing efforts. Patients with significant airway compression often develop accessory muscle breathing patterns that make the sternocleidomastoid muscles more prominent during inspiration, creating a rope-like appearance along the sides of the neck that becomes more pronounced with physical exertion or when lying flat. The presence of tracheal deviation, commonly seen with large unilateral thyroid masses or asymmetrical lymphadenopathy, may be visible as an apparent shift in the normal midline neck structures, particularly noticeable when patients extend their necks or during deep inspiration. In severe cases of airway compromise, patients may exhibit paradoxical breathing patterns where the neck muscles work against the diaphragm, creating unusual movement patterns that are visible during respiratory cycles and may be accompanied by cyanosis around the lips and nail beds. Chronic airway compression can lead to the development of collateral circulation and venous congestion that becomes more apparent during respiratory effort, with neck veins becoming more distended during inspiration rather than the normal pattern of collapse. Additionally, patients may unconsciously adopt specific neck positions that optimize airway patency, such as the "sniffing position" with slight neck extension and chin elevation, which can become a habitual posture that alters the normal neck appearance even when not actively experiencing respiratory distress.
8. Swallowing Difficulties and Visible Effects - Digestive Function Impact

Thyroid disorders and neck lymphadenopathy frequently impair swallowing function, creating visible changes in neck movement patterns, muscle coordination, and compensatory behaviors that can be observed during eating, drinking, or even routine saliva management. Large thyroid masses, particularly those with posterior extension, can compress the esophagus and create mechanical obstruction that forces patients to adopt unusual head and neck positions during swallowing, often tilting the head back or to one side to facilitate food passage. This compensation creates characteristic movement patterns that may include multiple swallowing attempts, visible neck muscle strain, and prolonged elevation of the larynx during the swallowing process, all of which can be observed by careful observers during meals or when patients drink liquids. Patients with significant dysphagia may develop visible muscle tension in the neck during swallowing attempts, with prominent contraction of the platysma muscle creating characteristic neck banding or "cording" that becomes more apparent with age or weight loss. The normal smooth, coordinated movement of the hyoid bone and larynx during swallowing may become jerky, incomplete, or asymmetrical when thyroid masses or enlarged lymph nodes interfere with normal anatomy, creating visible irregularities in the swallowing process that can be concerning to both patients and observers. In some cases, patients may develop visible pooling of saliva or food particles in the pyriform sinuses or valleculae, creating subtle fullness or asymmetry in the lower neck region that becomes more apparent after eating or drinking. Chronic swallowing difficulties can also lead to compensatory behaviors such as frequent throat clearing, visible coughing episodes, or the need to drink liquids with every bite of solid food, all of which create observable changes in normal eating and drinking patterns that may alert others to underlying neck pathology.
9. Voice-Related Physical Manifestations - Laryngeal Function Changes
Thyroid and lymphatic disorders can significantly impact voice production and laryngeal function, creating visible physical manifestations in the neck region that reflect underlying changes in vocal cord function, laryngeal positioning, and respiratory support for speech production. Recurrent laryngeal nerve involvement, commonly seen with thyroid cancer or large goiters, can produce vocal cord paralysis that manifests as visible strain in the neck muscles during speaking attempts, with patients often displaying prominent sternocleidomastoid muscle contraction and neck vein distension as they work harder to produce audible voice. The loss of normal vocal cord adduction creates compensatory behaviors that are visible during speech, including increased respiratory effort with visible chest and neck muscle recruitment, frequent pausing to take breaths during conversation, and characteristic head and neck positioning to optimize voice production. Patients with vocal cord paralysis may unconsciously turn their heads slightly to one side or adopt a chin-down posture to improve vocal cord approximation, creating asymmetrical neck positioning that becomes habitual over time. Laryngeal edema associated with thyroid inflammation or lymphatic obstruction can create visible fullness in the anterior neck region, particularly around the thyroid cartilage prominence, and may be accompanied by visible swelling that fluctuates with voice use or time of day. In cases of bilateral vocal cord paralysis, patients may develop visible respiratory distress during speech attempts, with prominent accessory muscle use and possible cyanosis that creates a dramatic change in neck appearance during voice production efforts. The chronic strain of compensating for voice changes can also lead to secondary muscle tension and visible muscle hypertrophy in the neck region, particularly affecting the extrinsic laryngeal muscles that work overtime to maintain voice function despite underlying pathology.
10. Systemic Manifestations in the Neck Region - Whole-Body Effects

Thyroid disorders create systemic effects that manifest prominently in the neck region, producing visible changes that reflect the widespread impact of thyroid hormone imbalance on multiple body systems and metabolic processes. Severe hypothyroidism can produce characteristic myxedema that is particularly noticeable in the neck and face, creating a puffy, non-pitting edema that gives the neck a thickened, swollen appearance with loss of normal anatomical definition and contours. This myxedematous change is often accompanied by a characteristic waxy, pale appearance of the skin and may be associated with thinning of the lateral eyebrows and coarse, brittle hair that extends into the neck region. Hyperthyroidism frequently produces visible signs of increased sympathetic nervous system activity in the neck region, including prominent carotid pulsations, visible tremor that may be apparent in the neck muscles during fine motor tasks, and increased sweating that may be particularly noticeable around the neck and collar area. Thyroid storm, a life-threatening complication of hyperthyroidism, can produce dramatic neck changes including severe flushing, profuse sweating, prominent vascular engorgement, and visible agitation that may include tremor affecting the entire neck and head region. Autoimmune thyroid conditions may be associated with other autoimmune manifestations that appear in the neck region, such as vitiligo creating patchy depigmentation, or dermatomy