10 Lip and Mouth Changes That Signal Nutritional Deficiencies
The human mouth serves as one of the most revealing indicators of overall nutritional status, offering healthcare professionals and individuals alike a readily accessible window into the body's internal health. The lips, tongue, gums, and oral tissues are among the fastest-regenerating structures in the human body, making them exquisitely sensitive to nutritional imbalances and deficiencies. When the body lacks essential vitamins, minerals, or other crucial nutrients, these oral tissues often manifest the earliest and most visible signs of distress. From subtle changes in lip texture and color to more pronounced alterations in tongue appearance and gum health, the mouth's response to nutritional inadequacy follows predictable patterns that have been documented extensively in medical literature. Understanding these oral manifestations empowers individuals to recognize potential deficiencies early, before more serious systemic complications develop. This comprehensive exploration examines ten specific lip and mouth changes that serve as reliable indicators of nutritional deficiencies, providing detailed insights into the underlying mechanisms, associated symptoms, and practical solutions for addressing these important health signals.
1. Cracked and Fissured Lips - The B-Vitamin Connection
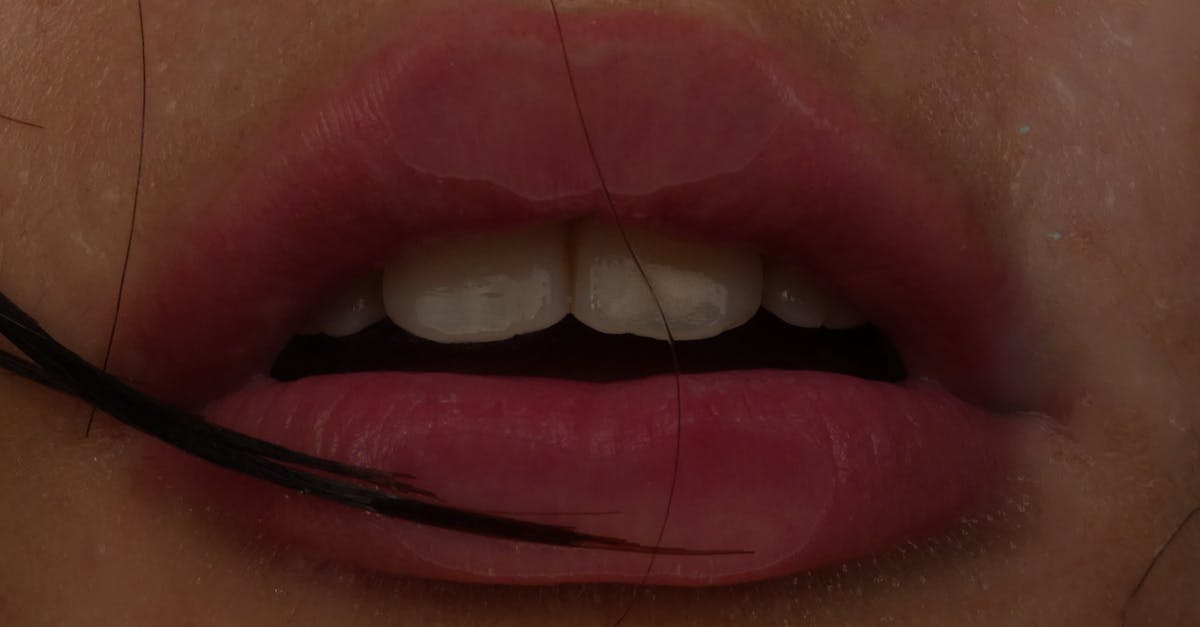
Angular cheilitis, characterized by painful cracks and fissures at the corners of the mouth, represents one of the most common oral manifestations of B-vitamin deficiencies, particularly riboflavin (B2), niacin (B3), and vitamin B12. These water-soluble vitamins play crucial roles in cellular metabolism and tissue repair, making their deficiency particularly evident in rapidly regenerating oral tissues. When riboflavin levels drop below optimal ranges, the delicate skin at the lip corners becomes vulnerable to breakdown, creating painful fissures that may bleed, crust over, or become secondarily infected with bacteria or fungi. The condition often begins as subtle dryness or tightness at the mouth corners, progressing to visible cracks that worsen with mouth opening, eating, or exposure to environmental factors. Research indicates that angular cheilitis affects up to 0.7% of the general population, with higher prevalence among elderly individuals, vegetarians, and those with malabsorption disorders. The healing process requires adequate B-vitamin restoration through dietary modifications or supplementation, typically showing improvement within 2-4 weeks of addressing the underlying deficiency. Foods rich in riboflavin include dairy products, eggs, leafy greens, and fortified cereals, while niacin sources encompass meat, fish, nuts, and whole grains.
2. Pale and Colorless Lips - Iron Deficiency Anemia Indicators

The natural pink or red coloration of healthy lips depends heavily on adequate blood flow and optimal hemoglobin levels, making lip pallor one of the earliest visible signs of iron deficiency anemia. Iron serves as the central component of hemoglobin, the protein responsible for oxygen transport throughout the body, and when iron stores become depleted, the resulting decrease in red blood cell production and hemoglobin concentration manifests prominently in the lips' appearance. Normally vibrant lips may gradually fade to pale pink, white, or even grayish hues as iron deficiency progresses from mild depletion to frank anemia. This color change typically accompanies other systemic symptoms including fatigue, weakness, shortness of breath, and cold intolerance, though lip pallor often appears before individuals recognize these more subtle internal symptoms. The condition affects approximately 25% of the global population, with particularly high prevalence among menstruating women, vegetarians, and individuals with gastrointestinal disorders that impair iron absorption. Diagnosis requires comprehensive blood testing including complete blood count, serum ferritin, and transferrin saturation levels to accurately assess iron status. Treatment involves identifying and addressing underlying causes of iron loss while implementing iron-rich dietary sources such as lean meats, seafood, beans, and fortified cereals, often supplemented with oral iron preparations under medical supervision.
3. Smooth, Red Tongue - Vitamin B12 and Folate Deficiency

A smooth, red, and often painful tongue condition known as glossitis serves as a hallmark sign of vitamin B12 and folate deficiencies, representing one of the most diagnostically significant oral manifestations of these crucial nutrient inadequacies. Under normal circumstances, the tongue surface features numerous small projections called papillae that give it a slightly rough texture and house taste buds essential for flavor perception. However, when B12 or folate levels drop significantly, these papillae gradually atrophy and disappear, leaving behind a characteristically smooth, shiny, and often bright red or magenta-colored tongue surface. This transformation typically occurs gradually over weeks to months, initially presenting as subtle changes in tongue texture before progressing to the classic smooth appearance that may be accompanied by burning sensations, altered taste perception, or difficulty eating certain foods. Vitamin B12 deficiency affects approximately 6% of adults under 60 years and up to 20% of those over 60, while folate deficiency remains common in areas with limited access to fortified foods or fresh vegetables. The condition frequently coexists with megaloblastic anemia, where both nutrients are essential for proper DNA synthesis and red blood cell formation. Treatment requires addressing the underlying cause, whether dietary inadequacy, malabsorption, or medication interference, followed by appropriate supplementation and regular monitoring to ensure adequate tissue healing and symptom resolution.
4. Burning Mouth Syndrome - Multiple Nutrient Deficiencies
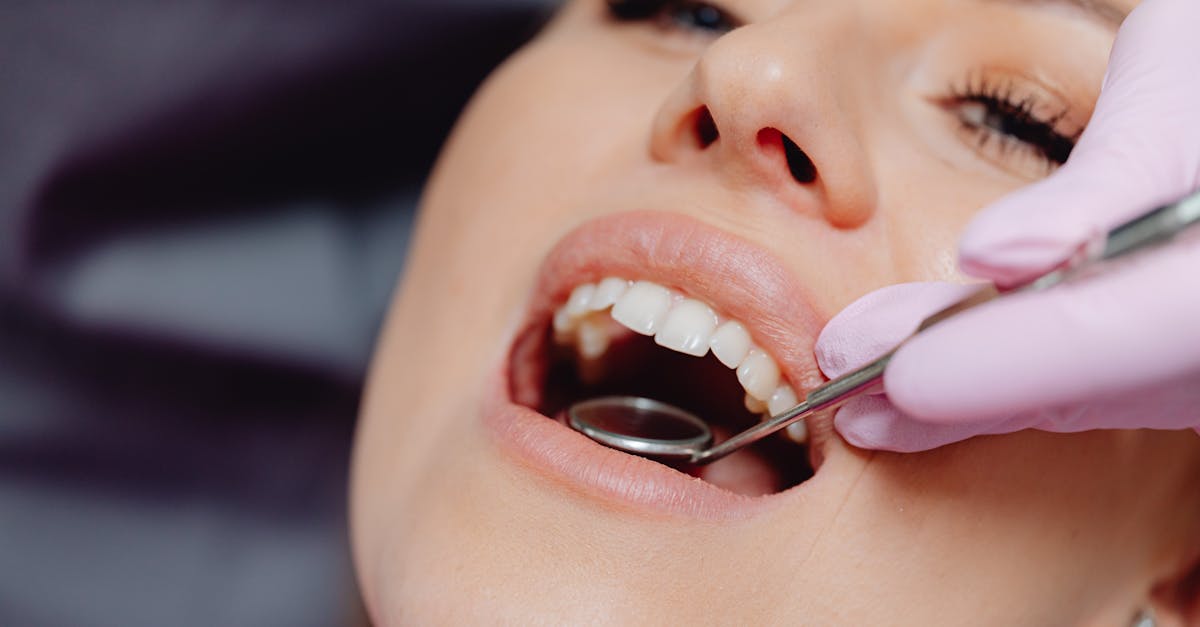
Burning mouth syndrome presents as a complex oral condition characterized by persistent burning, scalding, or tingling sensations affecting the lips, tongue, and oral mucosa, often indicating multiple overlapping nutritional deficiencies rather than a single nutrient inadequacy. This challenging condition most commonly affects postmenopausal women and has been linked to deficiencies in B-complex vitamins (particularly B1, B2, B6, and B12), iron, zinc, and folate, suggesting that optimal oral comfort requires a delicate balance of multiple essential nutrients working synergistically. The burning sensation typically intensifies throughout the day, often described as similar to having consumed very hot food or beverages, and may be accompanied by dry mouth, altered taste perception, and increased thirst. Research indicates that approximately 0.7-3.7% of the population experiences burning mouth syndrome, with the condition often misdiagnosed or attributed solely to psychological factors before underlying nutritional causes are identified. The pathophysiology involves compromised nerve function and altered oral tissue metabolism resulting from inadequate nutrient availability for cellular repair and neurotransmitter synthesis. Comprehensive nutritional assessment becomes essential for proper diagnosis, requiring detailed dietary analysis, blood testing for multiple vitamins and minerals, and careful evaluation of absorption capacity. Treatment typically involves a multifaceted approach combining targeted supplementation, dietary modifications to include nutrient-dense foods, and addressing any underlying conditions that may impair nutrient absorption or utilization.
5. Swollen and Bleeding Gums - Vitamin C Deficiency (Scurvy)
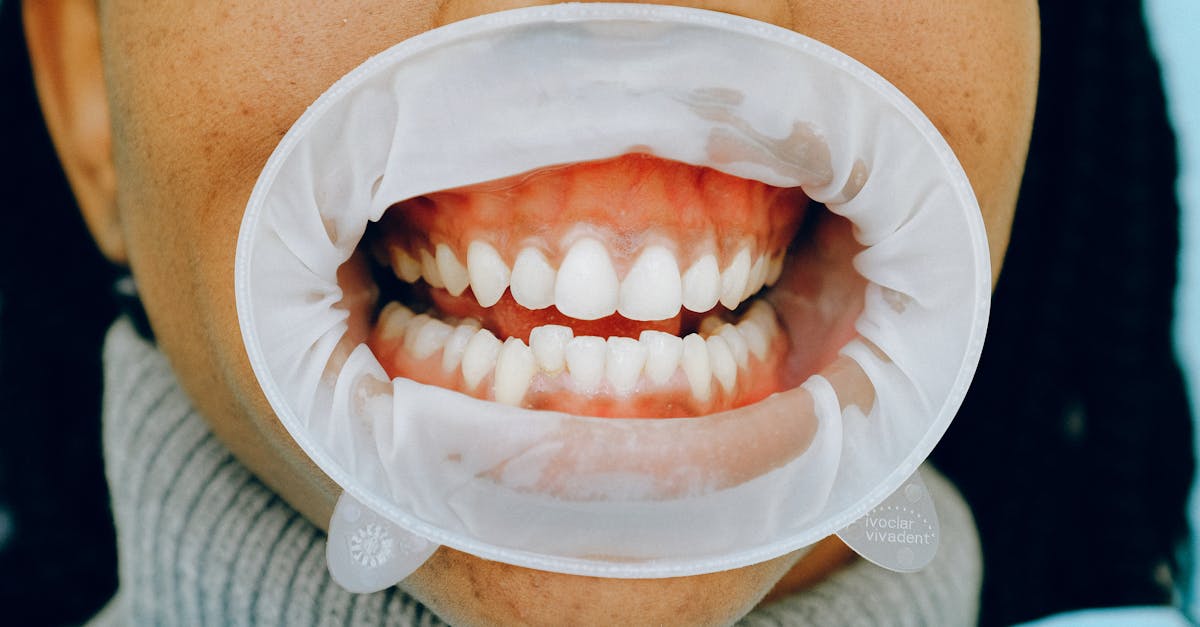
Swollen, bleeding, and tender gums represent the classic oral manifestation of vitamin C deficiency, historically known as scurvy, demonstrating the critical role of ascorbic acid in maintaining healthy connective tissue throughout the oral cavity. Vitamin C serves as an essential cofactor for collagen synthesis, the primary structural protein that provides strength and integrity to gums, blood vessel walls, and other connective tissues. When vitamin C intake falls below adequate levels, typically less than 10 mg daily for extended periods, the body's ability to maintain and repair gum tissue becomes severely compromised, leading to characteristic changes that progress from subtle inflammation to severe tissue breakdown. Initial symptoms include gum tenderness and slight bleeding during brushing or flossing, which many individuals mistakenly attribute to aggressive oral hygiene rather than nutritional deficiency. As the condition progresses, gums become increasingly swollen, purple or red in color, and may bleed spontaneously or with minimal provocation. Advanced cases can result in tooth loosening, gum recession, and secondary bacterial infections that further complicate the clinical picture. While frank scurvy remains relatively rare in developed countries due to food fortification and availability of fresh produce, subclinical vitamin C deficiency affects significant portions of certain populations, particularly elderly individuals, smokers, and those with limited access to fresh fruits and vegetables. Treatment requires immediate vitamin C supplementation combined with dietary modifications to include citrus fruits, berries, leafy greens, and other ascorbic acid-rich foods, typically resulting in noticeable gum improvement within days to weeks of adequate intake restoration.
6. White Patches and Oral Thrush - Zinc and Immune Deficiency
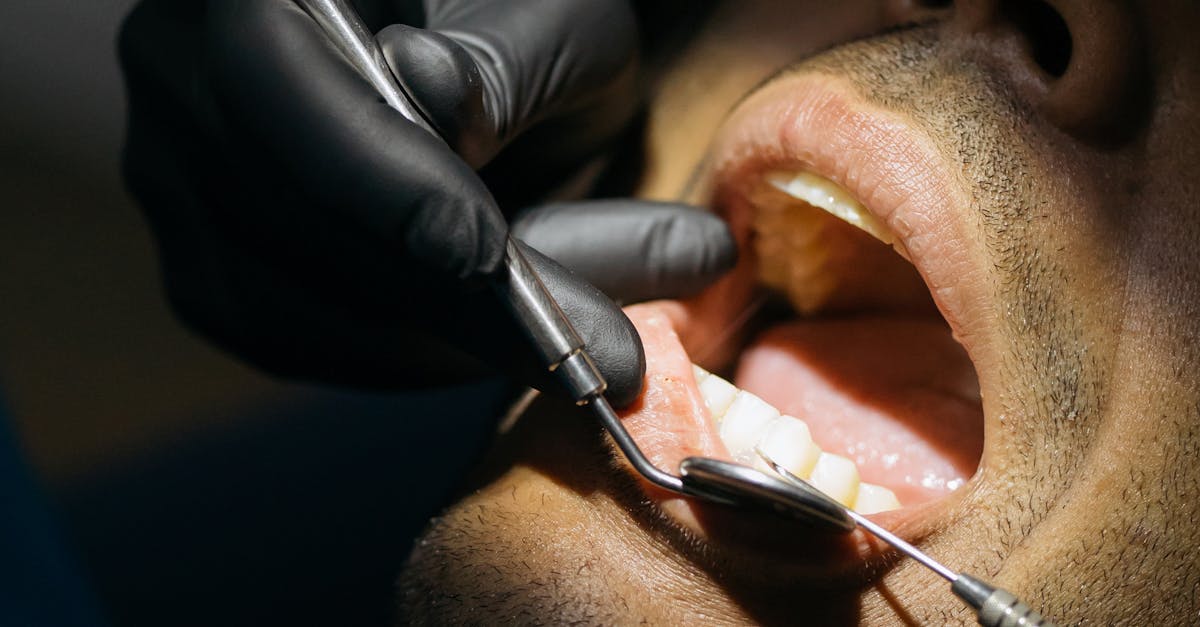
The development of white, cottage cheese-like patches on the tongue, inner cheeks, and oral tissues, known as oral thrush or candidiasis, often signals underlying zinc deficiency that compromises immune function and allows opportunistic fungal infections to establish themselves in the mouth. Zinc plays a fundamental role in immune system regulation, wound healing, and maintenance of healthy oral mucosa, making its deficiency particularly problematic for oral health maintenance. When zinc levels drop below optimal ranges, the body's natural defense mechanisms against Candida albicans and other opportunistic organisms become impaired, creating an environment conducive to fungal overgrowth and infection. These white patches typically appear as removable plaques that, when wiped away, reveal red, raw, or bleeding tissue underneath, often accompanied by burning sensations, altered taste perception, and difficulty swallowing. Zinc deficiency affects an estimated 17% of the global population, with higher prevalence among elderly individuals, vegetarians, pregnant women, and those with gastrointestinal disorders that impair mineral absorption. The condition frequently occurs alongside other signs of zinc inadequacy including delayed wound healing, hair loss, skin problems, and increased susceptibility to infections. Risk factors include inadequate dietary intake, malabsorption syndromes, chronic kidney disease, and certain medications that interfere with zinc metabolism. Treatment involves addressing the underlying zinc deficiency through dietary modifications emphasizing zinc-rich foods such as oysters, beef, pumpkin seeds, and legumes, often combined with zinc supplementation under medical supervision to restore adequate tissue levels and immune function.
7. Geographic Tongue - Nutritional Imbalances and Stress

Geographic tongue, medically termed benign migratory glossitis, presents as irregular, map-like patches of smooth, red areas surrounded by white or yellow borders that appear to migrate across the tongue surface over time, often indicating complex nutritional imbalances involving B-vitamins, zinc, and iron. This benign but often concerning condition affects approximately 1-3% of the population and demonstrates the intricate relationship between nutritional status, stress levels, and oral tissue health. The characteristic appearance results from localized loss of papillae in affected areas, creating the smooth, red patches that contrast sharply with the normal tongue texture, while the white borders represent areas of thickened tissue attempting to regenerate. Research suggests that geographic tongue frequently correlates with deficiencies in vitamin B12, folate, riboflavin, and zinc, nutrients essential for proper cellular turnover and tissue maintenance in rapidly regenerating oral structures. The condition often fluctuates in severity and location, with stress, hormonal changes, and dietary factors influencing the extent and activity of the lesions. While generally painless, some individuals experience burning or stinging sensations, particularly when consuming acidic, spicy, or hot foods and beverages. The condition shows strong associations with other oral health issues including fissured tongue, oral lichen planus, and increased susceptibility to oral infections. Management focuses on identifying and correcting underlying nutritional deficiencies through comprehensive dietary assessment and targeted supplementation, while stress reduction techniques and avoidance of trigger foods can help minimize symptom severity and frequency of flare-ups.
8. Dry Mouth and Reduced Saliva - Dehydration and Electrolyte Imbalance

Persistent dry mouth, medically known as xerostomia, represents a significant oral health concern that often signals underlying dehydration, electrolyte imbalances, or deficiencies in essential nutrients required for optimal salivary gland function. Saliva production depends on adequate hydration, proper electrolyte balance (particularly sodium, potassium, and chloride), and sufficient levels of various vitamins and minerals that support glandular metabolism and nerve function. When these nutritional requirements are not met, salivary glands may reduce their output, leading to the uncomfortable sensation of dry mouth along with associated complications including difficulty swallowing, altered taste perception, and increased risk of dental decay and oral infections. The condition affects up to 30% of elderly individuals and can result from various factors including inadequate fluid intake, excessive sodium consumption, diuretic medications, and deficiencies in B-vitamins that support nerve function controlling salivary glands. Chronic dry mouth creates a cascade of oral health problems, as saliva normally serves crucial protective functions including neutralizing acids produced by oral bacteria, washing away food particles and debris, and providing antimicrobial compounds that help prevent infections. Individuals with persistent xerostomia often experience difficulty eating dry foods, increased dental cavities, bad breath, and oral discomfort that significantly impacts quality of life. Assessment requires evaluation of hydration status, medication review, and nutritional analysis to identify correctable causes. Treatment involves optimizing fluid intake, addressing electrolyte imbalances, correcting identified nutritional deficiencies, and implementing strategies to stimulate natural saliva production while protecting oral tissues from the complications of reduced salivary flow.
9. Delayed Wound Healing in Mouth - Protein and Vitamin Deficiencies

Significantly delayed healing of oral wounds, including cuts, ulcers, or surgical sites within the mouth, serves as an important indicator of protein deficiency and inadequate levels of vitamins A, C, and E, nutrients essential for tissue repair and regeneration processes. The oral cavity normally demonstrates remarkable healing capacity due to its rich blood supply and rapid cellular turnover, with minor injuries typically resolving within 7-14 days under optimal nutritional conditions. However, when protein intake falls below requirements or when key vitamins supporting wound healing are deficient, this natural repair process becomes significantly impaired, leading to prolonged healing times, increased infection risk, and potential complications. Protein provides the essential amino acids required for collagen synthesis, cellular proliferation, and immune function, while vitamin A supports epithelial cell differentiation, vitamin C enables collagen cross-linking, and vitamin E provides antioxidant protection during the inflammatory healing phase. Individuals experiencing delayed oral wound healing often report that minor injuries such as accidental bites, dental work sites, or small ulcers persist for weeks rather than days, sometimes becoming secondarily infected or developing into chronic lesions. This condition particularly affects elderly individuals, those following restrictive diets, patients with malabsorption disorders, and individuals with chronic diseases that increase nutritional requirements. The assessment requires careful evaluation of protein intake, typically requiring 0.8-1.2 grams per kilogram of body weight daily for healthy adults, along with adequate consumption of vitamin-rich foods including colorful fruits and vegetables, lean proteins, and healthy fats. Treatment involves optimizing nutritional intake through dietary counseling, addressing any underlying absorption issues, and potentially providing targeted supplementation to restore adequate levels of healing-supporting nutrients.
10. Loss of Taste Sensation - Zinc and Vitamin Deficiencies

The gradual or sudden loss of taste sensation, known as hypogeusia or ageusia, represents a significant nutritional red flag often indicating zinc deficiency, along with potential inadequacies in vitamins A, B12, and other nutrients essential for proper taste bud function and nerve transmission. Taste perception depends on complex interactions between specialized taste cells, nerve pathways, and various nutrients that support cellular metabolism and regeneration within taste buds, which have a relatively short lifespan of 7-10 days and require constant renewal. Zinc plays a particularly crucial role in taste function, serving as a cofactor for numerous enzymes involved in taste cell metabolism and supporting the structural integrity of taste pore proteins that detect different flavor compounds. When zinc levels drop below optimal ranges, individuals may first notice that foods seem bland or require more seasoning than usual, progressing to more significant taste alterations or complete loss of certain taste sensations. This condition affects approximately 5% of the general population but shows much higher prevalence among elderly individuals, with some studies reporting taste disorders in up to 27% of those over 60 years of age. The impact extends beyond mere inconvenience, as taste loss often leads to decreased appetite, poor food choices, unintentional weight loss, and reduced quality of life that can significantly affect nutritional status and overall health. Associated symptoms may include altered smell perception, since taste and smell work synergistically, along with other signs of zinc deficiency such as delayed wound healing, hair loss, and increased susceptibility to infections. Diagnosis requires comprehensive assessment including detailed dietary history, physical examination of oral structures, and laboratory testing to evaluate zinc status along with other potentially involved nutrients, followed by targeted nutritional intervention to restore proper taste function.
11. Integrating Oral Health Monitoring into Nutritional Wellness
The intricate relationship between oral health and nutritional status demonstrates the mouth's remarkable capacity to serve as an early warning system for developing nutrient deficiencies, offering healthcare providers and individuals valuable opportunities for early intervention and prevention of more serious health complications. Throughout this comprehensive exploration, we have examined ten distinct oral and lip changes that reliably indicate specific nutritional inadequacies, from the angular cheilitis associated with B-vitamin deficiencies to the delayed wound healing that signals protein and vitamin insufficiencies. These manifestations represent just the visible tip of the nutritional iceberg, often appearing weeks or months before more serious systemic symptoms develop, making regular oral health monitoring an essential component of comprehensive nutritional assessment. The interconnected nature of these conditions highlights the importance of maintaining balanced nutrition rather than focusing on individual nutrients in isolation, as many oral health problems result from multiple overlapping deficiencies that require comprehensive dietary and supplementation strategies. Healthcare providers increasingly recognize the value of thorough oral examinations as part of routine nutritional screening, particularly for high-risk populations including elderly individuals, those with restrictive diets, patients with chronic diseases, and individuals with limited access to diverse, nutrient-rich foods. Moving forward, individuals can empower themselves by conducting regular self-assessments of their oral health, noting changes in lip color or texture, tongue appearance, gum health, and taste sensation as potential indicators of nutritional needs