8 Circulatory Conditions With Visible Symptoms on the Skin
The human circulatory system serves as the body's intricate highway, delivering oxygen, nutrients, and vital substances to every cell while removing metabolic waste products. When this complex network of blood vessels, comprising arteries, veins, and capillaries, experiences dysfunction or disease, the effects often manifest visibly on the skin's surface. The skin, being the body's largest organ and containing an extensive network of blood vessels, acts as a remarkable diagnostic window into circulatory health. From subtle color changes and unusual patterns to dramatic swelling and distinctive lesions, the skin provides healthcare professionals and individuals with crucial visual clues about underlying vascular conditions. Understanding these visible manifestations is essential for early detection, proper diagnosis, and timely intervention of circulatory disorders. The eight conditions explored in this comprehensive examination represent some of the most significant circulatory ailments that present with characteristic skin symptoms, ranging from common venous insufficiency to life-threatening conditions like systemic lupus erythematosus. By recognizing these telltale signs, individuals can seek appropriate medical attention, potentially preventing serious complications and improving their overall cardiovascular health outcomes.
1. Chronic Venous Insufficiency - When Veins Fail to Return Blood Efficiently
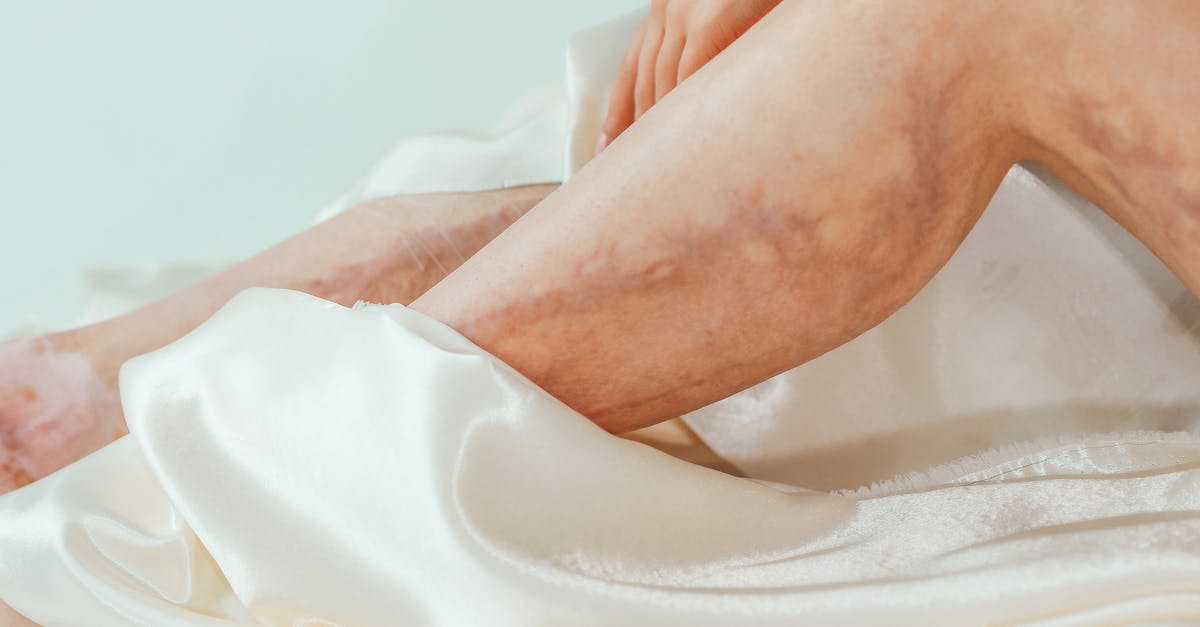
Chronic venous insufficiency represents one of the most prevalent circulatory conditions affecting millions worldwide, characterized by the inability of leg veins to efficiently return blood to the heart. This condition develops when the one-way valves within the veins become damaged or weakened, allowing blood to pool in the lower extremities rather than flowing upward against gravity. The visible skin manifestations of chronic venous insufficiency are both distinctive and progressive, beginning with the appearance of spider veins and varicose veins that create a web-like or rope-like pattern on the legs. As the condition advances, patients may notice skin discoloration, particularly around the ankles and lower legs, where the skin takes on a brownish or reddish hue due to the breakdown of red blood cells and the deposition of hemosiderin. The affected skin often becomes thickened, dry, and scaly, a condition known as lipodermatosclerosis, which gives the skin a leather-like appearance. In severe cases, venous stasis ulcers may develop, typically appearing as shallow, irregularly shaped wounds with surrounding inflammation and discoloration. These ulcers are notoriously difficult to heal and can become chronic without proper treatment. The skin changes associated with chronic venous insufficiency serve as important indicators of disease progression and help healthcare providers determine the most appropriate treatment strategies, which may include compression therapy, lifestyle modifications, or surgical interventions.
2. Peripheral Arterial Disease - Compromised Blood Flow to Extremities
Peripheral arterial disease (PAD) affects approximately 8.5 million adults in the United States alone, representing a significant circulatory condition where narrowed or blocked arteries reduce blood flow to the extremities, particularly the legs and feet. This atherosclerotic process results in inadequate oxygen and nutrient delivery to tissues, creating a cascade of visible skin changes that serve as important diagnostic markers. The skin of individuals with PAD often appears pale, cool to the touch, and may have a distinctive shiny, hairless appearance due to poor circulation. Hair loss on the legs and feet is particularly notable, as hair follicles require adequate blood supply to maintain normal growth cycles. The skin may also develop a characteristic pallor when the affected limb is elevated, followed by a dusky red or purple discoloration when the limb is lowered, a phenomenon known as dependent rubor. Patients frequently experience delayed wound healing, with even minor cuts or abrasions taking significantly longer to heal than normal, and wounds may appear pale or have poor granulation tissue formation. In advanced cases, tissue death or gangrene may occur, presenting as blackened, necrotic areas typically beginning at the toes or fingertips. The skin may also develop a mottled appearance, with irregular patches of discoloration that reflect the uneven distribution of blood flow. These visible manifestations of PAD not only aid in diagnosis but also help healthcare providers assess disease severity and monitor treatment effectiveness, emphasizing the critical importance of early recognition and intervention.
3. Deep Vein Thrombosis - Blood Clots and Their Cutaneous Consequences

Deep vein thrombosis (DVT) represents a serious circulatory emergency where blood clots form within the deep veins, most commonly in the legs, creating both immediate health risks and distinctive skin manifestations that can aid in rapid diagnosis. The formation of these clots typically occurs due to a combination of factors including prolonged immobility, injury to blood vessel walls, or increased blood clotting tendency, and the resulting skin changes reflect the underlying vascular obstruction and inflammatory response. The affected limb often exhibits noticeable swelling, with the skin appearing stretched and taut due to fluid accumulation caused by impaired venous drainage. This swelling is typically asymmetric, affecting only the limb with the clot, and may be accompanied by a sensation of heaviness or fullness. The skin over the affected area frequently displays a characteristic reddish or bluish discoloration, reflecting the compromised circulation and venous congestion. Patients may notice that the skin feels warm to the touch, indicating the inflammatory response triggered by the clot formation. In some cases, a network of superficial veins may become more prominent and visible on the skin surface as the body attempts to establish collateral circulation around the blocked deep vein. The skin may also develop a glossy or shiny appearance due to the stretching caused by underlying swelling. Pain and tenderness are common accompanying symptoms, often described as a cramping or aching sensation that worsens with movement or pressure. Recognition of these skin manifestations is crucial for prompt medical intervention, as untreated DVT can lead to life-threatening complications such as pulmonary embolism or long-term complications like post-thrombotic syndrome.
4. Raynaud's Phenomenon - Vascular Spasms and Color-Changing Episodes
Raynaud's phenomenon presents as one of the most visually dramatic circulatory conditions, characterized by episodic vascular spasms that cause distinctive color changes in the fingers, toes, and sometimes other extremities in response to cold temperatures or emotional stress. This condition affects approximately 5-10% of the population and manifests through a characteristic triphasic color response that serves as a hallmark diagnostic feature. During an episode, the affected digits initially turn white or pale as blood vessels constrict severely, cutting off circulation to the area and creating a stark, blanched appearance that may affect one or multiple fingers or toes. This pallor phase is followed by a blue or purple discoloration as oxygen levels in the tissues decrease, giving the skin a cyanotic appearance that can be quite alarming to observers. Finally, as the blood vessels begin to dilate and circulation returns, the affected areas turn bright red, often accompanied by throbbing, tingling, or burning sensations as blood flow is restored. These color changes typically occur in a symmetric pattern and may be accompanied by numbness, stiffness, or difficulty using the affected digits. The skin may also feel cold to the touch during episodes and may appear slightly swollen as circulation normalizes. In severe or chronic cases, repeated episodes can lead to skin changes including thinning, scarring, or the development of small ulcers at the fingertips. Some individuals may also notice that their skin becomes more sensitive to temperature changes over time, and the episodes may become more frequent or severe. Understanding these distinctive visual manifestations is essential for proper diagnosis and management, as Raynaud's phenomenon can be either primary (occurring on its own) or secondary to underlying autoimmune or connective tissue disorders.
5. Systemic Lupus Erythematosus - Autoimmune Inflammation and Distinctive Rashes
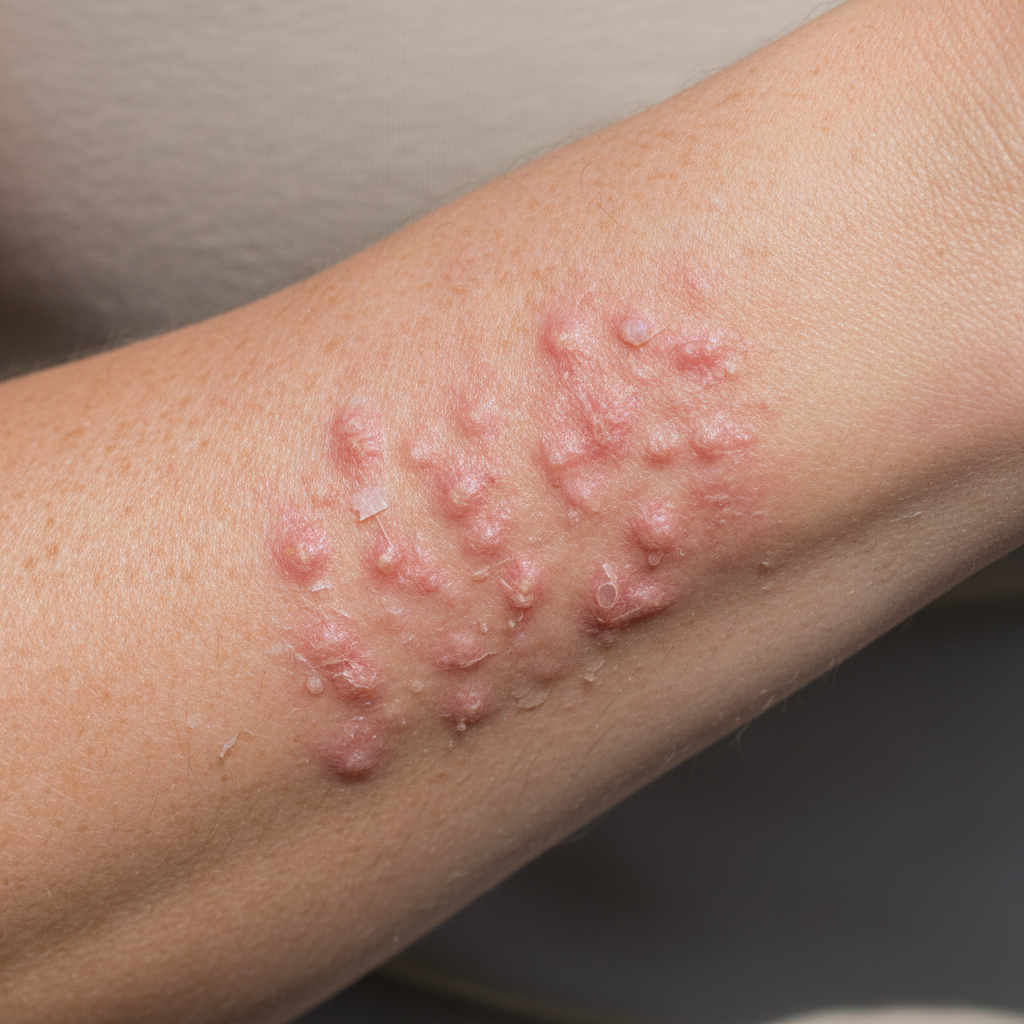
Systemic lupus erythematosus (SLE) represents a complex autoimmune disorder that significantly impacts the circulatory system while producing some of the most recognizable skin manifestations in medicine. This chronic inflammatory condition affects multiple organ systems, including blood vessels throughout the body, leading to vasculitis and distinctive cutaneous symptoms that often serve as early diagnostic clues. The most characteristic skin feature of lupus is the malar rash, commonly known as the "butterfly rash," which appears as a red, flat or raised rash across the cheeks and bridge of the nose, resembling the shape of a butterfly's wings. This rash typically spares the nasolabial folds and may worsen with sun exposure due to photosensitivity, another hallmark feature of the condition. Patients with lupus often develop discoid lesions, which are round, disk-shaped areas of inflammation that can occur anywhere on the body but are most common on the face, scalp, and ears. These lesions begin as red, scaly patches that may progress to scarring and permanent hair loss if they occur on the scalp. The skin may also exhibit livedo reticularis, a lace-like pattern of purple discoloration caused by inflammation of small blood vessels, creating a net-like appearance that is particularly visible on the arms and legs. Raynaud's phenomenon is common in lupus patients, affecting up to 95% of individuals with the condition, and may present before other symptoms become apparent. Additional skin manifestations include oral and nasal ulcers, which appear as painful sores in the mouth or nose, and various types of vasculitic lesions including purpura, which are small purple spots caused by bleeding under the skin. The skin may also become more fragile and prone to bruising, and some patients develop a distinctive rash on sun-exposed areas that may be the first sign of the disease.
6. Congestive Heart Failure - Fluid Retention and Circulatory Compromise
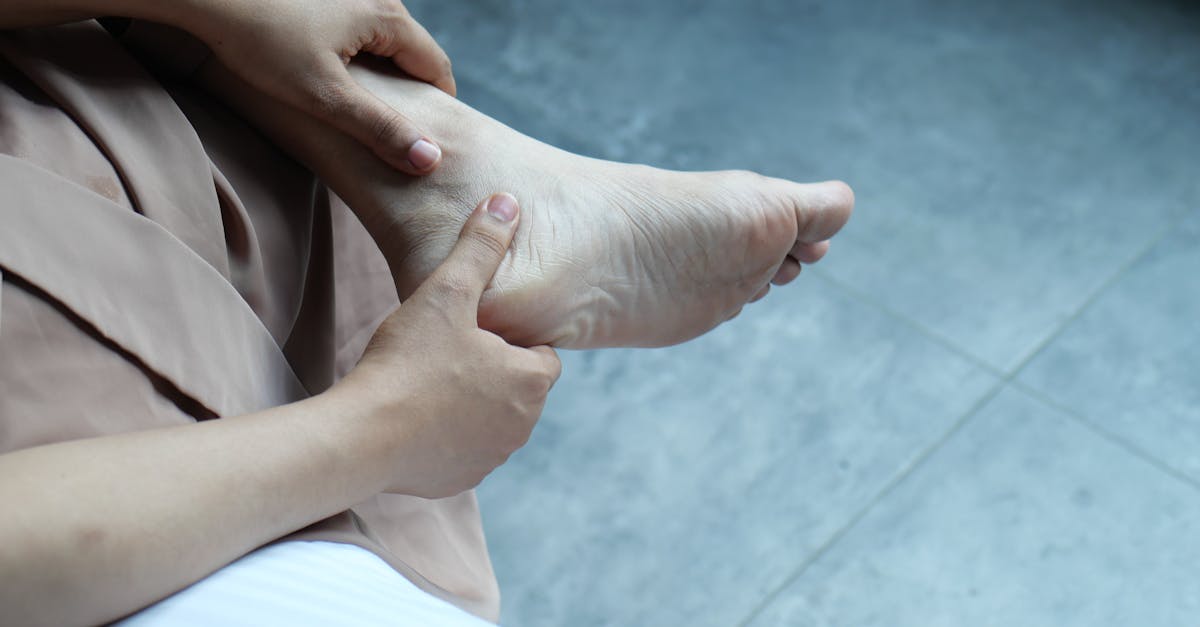
Congestive heart failure represents a progressive condition where the heart's pumping ability becomes compromised, leading to inadequate circulation and distinctive skin manifestations that reflect the body's struggle to maintain proper fluid balance and tissue perfusion. As the heart fails to pump blood efficiently, fluid begins to accumulate in various parts of the body, creating visible changes that can help healthcare providers assess disease severity and monitor treatment response. The most prominent skin manifestation of heart failure is peripheral edema, which typically begins in the feet and ankles and may progress up the legs as the condition worsens. This swelling creates a characteristic appearance where the skin appears stretched, shiny, and may retain indentations when pressed, a phenomenon known as pitting edema. The affected skin often takes on a pale or slightly bluish tint due to poor circulation and reduced oxygen delivery to the tissues. As fluid accumulation progresses, the skin may develop a tight, uncomfortable feeling, and patients may notice that their shoes no longer fit properly or that socks leave deep impressions on their legs. In advanced cases, the skin may become so stretched that it develops small cracks or fissures, particularly around the ankles and lower legs, which can become entry points for infection. The skin temperature may also be noticeably cooler in the affected areas due to reduced blood flow. Some patients develop a condition called cardiac cirrhosis, where prolonged heart failure leads to liver congestion and subsequent yellowing of the skin and eyes (jaundice). Additionally, chronic poor circulation may cause the skin to develop a mottled appearance with irregular patches of discoloration, and nail beds may appear blue or purple, indicating decreased oxygen levels in the blood. These visible manifestations serve as important indicators of heart failure progression and help guide treatment decisions.
7. Atherosclerosis - Arterial Hardening and Its Cutaneous Manifestations
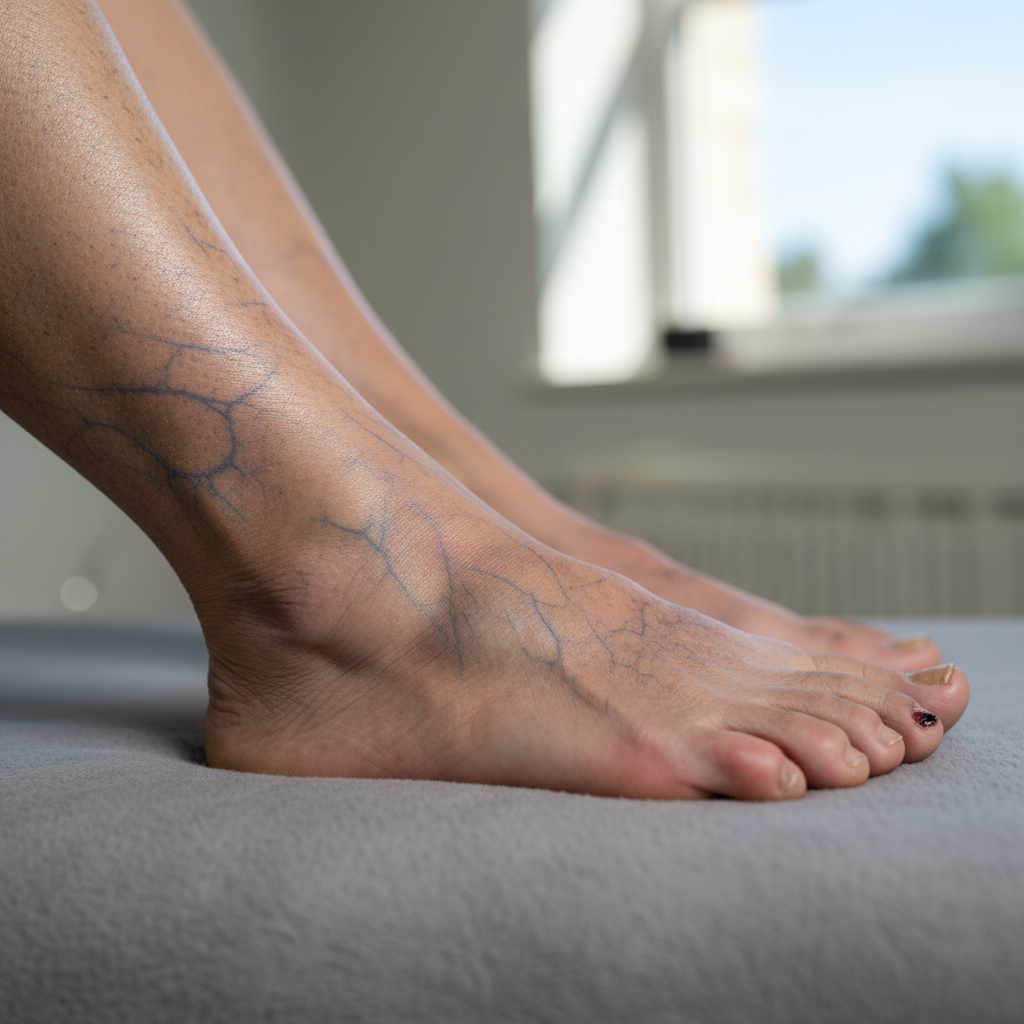
Atherosclerosis, the progressive hardening and narrowing of arteries due to plaque buildup, represents one of the most significant circulatory conditions affecting modern society, with skin manifestations that often provide early warning signs of this potentially life-threatening disease. As atherosclerotic plaques accumulate within arterial walls, they gradually reduce blood flow to various organs and tissues, creating a range of visible skin changes that reflect compromised circulation. The skin supplied by affected arteries often appears pale, cool, and may have a characteristic waxy or translucent quality due to reduced blood flow and decreased delivery of oxygen and nutrients. Hair loss is commonly observed in areas with poor circulation, particularly on the lower legs and feet, where hair follicles cannot maintain normal growth cycles without adequate blood supply. The skin may also develop a distinctive shiny, atrophic appearance, becoming thin and fragile with reduced subcutaneous fat and muscle mass. Nail changes are frequently present, with toenails and fingernails growing more slowly, becoming thick, brittle, or developing ridges due to poor circulation to the nail beds. Patients may notice that minor wounds heal very slowly or not at all, and even small cuts or abrasions may develop into chronic ulcers, particularly on the feet and lower legs where circulation is most compromised. The skin may also exhibit a phenomenon called claudication pallor, where the affected limb becomes noticeably pale during exercise or activity and may develop a dusky red color during rest as blood flow attempts to compensate. In severe cases, tissue death or gangrene may occur, beginning as small dark spots that gradually expand if blood flow is not restored. Some patients develop distinctive yellow deposits called xanthomas, which are cholesterol-rich lesions that may appear on the eyelids, hands, or other areas, indicating underlying lipid metabolism disorders that contribute to atherosclerosis.
8. Vasculitis - Inflammatory Blood Vessel Disease and Skin Lesions

Vasculitis encompasses a group of inflammatory conditions that affect blood vessels of various sizes throughout the body, producing diverse and often dramatic skin manifestations that serve as important diagnostic markers for these potentially serious disorders. This inflammatory process can affect arteries, veins, or capillaries, leading to vessel wall damage, reduced blood flow, and characteristic skin lesions that vary depending on the type and severity of vasculitis involved. Palpable purpura represents one of the most common skin manifestations of vasculitis, appearing as raised, purple spots that do not blanch when pressure is applied, indicating bleeding from inflamed small blood vessels in the skin. These lesions typically appear on the lower legs and feet but can occur anywhere on the body and may be accompanied by pain, burning, or itching sensations. Livedo reticularis, a net-like pattern of purple discoloration, is another characteristic finding that results from inflammation of small arteries and arterioles, creating a lace-like appearance on the skin that is particularly visible on the arms and legs. Patients with vasculitis may also develop various types of ulcers, ranging from small, shallow lesions to large, deep wounds that are slow to heal due to compromised blood flow to the affected tissues. Nodular lesions may appear as firm, red bumps under the skin, particularly along the course of blood vessels, and these may be tender to the touch or painless depending on the specific type of vasculitis. Some forms of vasculitis produce distinctive rashes, such as the characteristic "saddle-nose" deformity seen in certain systemic vasculitides, or the digital ischemia that can lead to fingertip ulcers or gangrene in severe cases. The skin may also exhibit signs of chronic inflammation, including thickening, scarring, or changes in pigmentation where previous lesions have healed. Fever, fatigue, and joint pain often accompany the skin manifestations, reflecting the systemic nature of these inflammatory conditions.
9. Integrating Skin Signs for Comprehensive Circulatory Health Assessment
The eight circulatory conditions explored in this comprehensive examination demonstrate the profound interconnection between vascular health and skin manifestations, highlighting the critical importance of recognizing these visible signs for early detection, accurate diagnosis, and effective management of circulatory disorders. From the progressive skin changes of chronic venous insufficiency to the dramatic color transformations of Raynaud's phenomenon, each condition presents unique cutaneous features that serve as valuable diagnostic tools for healthcare providers and important warning signs for patients. The skin's role as a window into circulatory health cannot be overstated, as these visible manifestations often appear before more serious complications develop, providing crucial opportunities for early intervention and treatment. Understanding the relationship between circulatory dysfunction and skin changes empowers individuals to seek timely medical attention when concerning symptoms arise, potentially preventing serious complications such as tissue death, chronic ulcers, or life-threatening events like pulmonary embolism. Healthcare providers must maintain a high index of suspicion for underlying circulatory conditions when evaluating patients with unexplained skin changes, as prompt recognition and treatment can significantly improve patient outcomes and quality of life. The integration of clinical assessment, patient history, and recognition of characteristic skin manifestations forms the foundation of effective circulatory health management. As our understanding of these conditions continues to evolve, the importance of patient education and awareness becomes increasingly apparent, emphasizing the need for continued research and public health initiatives focused on circulatory disease prevention and early detection. By recognizing these eight key conditions and their associated skin manifestations, we can work together to improve circulatory health outcomes and reduce the burden of vascular disease in our communities.