12 Inflammatory Conditions That Show Up on the Skin First
The skin, our body's largest organ, serves as far more than a protective barrier—it functions as an intricate early warning system that can reveal internal inflammatory processes long before other symptoms manifest. When systemic inflammation begins to develop within the body, the skin often becomes the first canvas upon which these conditions paint their telltale signs. This phenomenon occurs because the skin's extensive vascular network, immune cell populations, and rapid cellular turnover make it exceptionally responsive to inflammatory mediators circulating throughout the body. From autoimmune disorders to metabolic dysfunction, numerous conditions announce their presence through distinctive cutaneous manifestations that trained eyes can recognize and interpret. Understanding these dermatological harbingers is crucial for both healthcare providers and patients, as early recognition can lead to prompt diagnosis and treatment, potentially preventing more serious complications. The following exploration delves into twelve significant inflammatory conditions that characteristically present with skin symptoms as their initial or most prominent feature, examining the underlying pathophysiology, clinical presentations, and the critical importance of recognizing these cutaneous clues in the broader context of systemic health.
1. Psoriasis - The Autoimmune Skin Accelerator
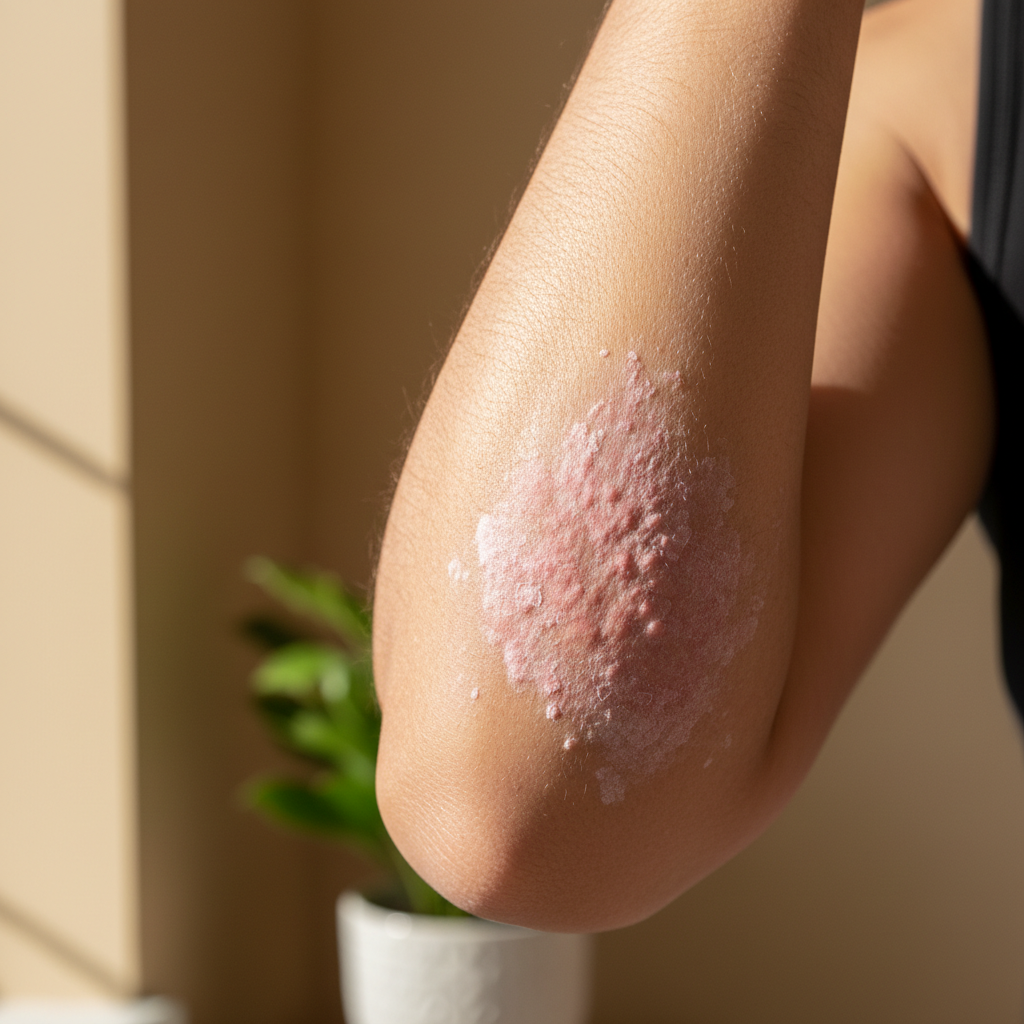
Psoriasis represents one of the most recognizable inflammatory skin conditions, characterized by the rapid overproduction of skin cells that creates thick, silvery scales and inflamed red patches. This chronic autoimmune disorder affects approximately 2-3% of the global population and results from a complex interplay between genetic predisposition and environmental triggers. The condition occurs when the immune system mistakenly attacks healthy skin cells, causing them to multiply at an accelerated rate—up to ten times faster than normal. While healthy skin typically regenerates every 28-30 days, psoriatic skin completes this cycle in just 3-4 days, leading to the characteristic buildup of cells on the surface. The inflammatory cascade involves multiple immune pathways, particularly the IL-17 and IL-23 axes, which drive the persistent inflammation and cellular proliferation. Beyond its obvious dermatological impact, psoriasis serves as a window into systemic inflammation, with patients showing increased risks for cardiovascular disease, diabetes, and inflammatory bowel disease. The skin lesions often appear first on the elbows, knees, scalp, and lower back, but can affect any area of the body, making early recognition and treatment essential for preventing both physical and psychological complications.
2. Lupus Erythematosus - The Great Mimicker's Skin Signature
Systemic lupus erythematosus (SLE) frequently announces its presence through distinctive cutaneous manifestations, earning its reputation as a condition where skin symptoms often precede systemic involvement by months or even years. The classic "butterfly rash" or malar rash across the cheeks and bridge of the nose affects approximately 30-60% of lupus patients and represents one of the most recognizable dermatological signs in medicine. This inflammatory autoimmune condition results from the body's immune system attacking its own tissues, creating widespread inflammation that can affect virtually every organ system. The skin manifestations in lupus are diverse and can include discoid lesions, photosensitive rashes, oral ulcers, and livedo reticularis, each providing important diagnostic clues about disease activity and prognosis. The underlying pathophysiology involves the formation of immune complexes and the production of autoantibodies that deposit in various tissues, triggering inflammatory responses. Cutaneous lupus can exist independently of systemic disease, but careful monitoring is essential as approximately 5-15% of patients with isolated skin involvement eventually develop systemic manifestations. The photosensitive nature of many lupus skin lesions highlights the importance of sun protection and serves as a daily reminder of the condition's inflammatory nature, making dermatological awareness crucial for early intervention and improved long-term outcomes.
3. Dermatomyositis - When Muscle Disease Speaks Through Skin
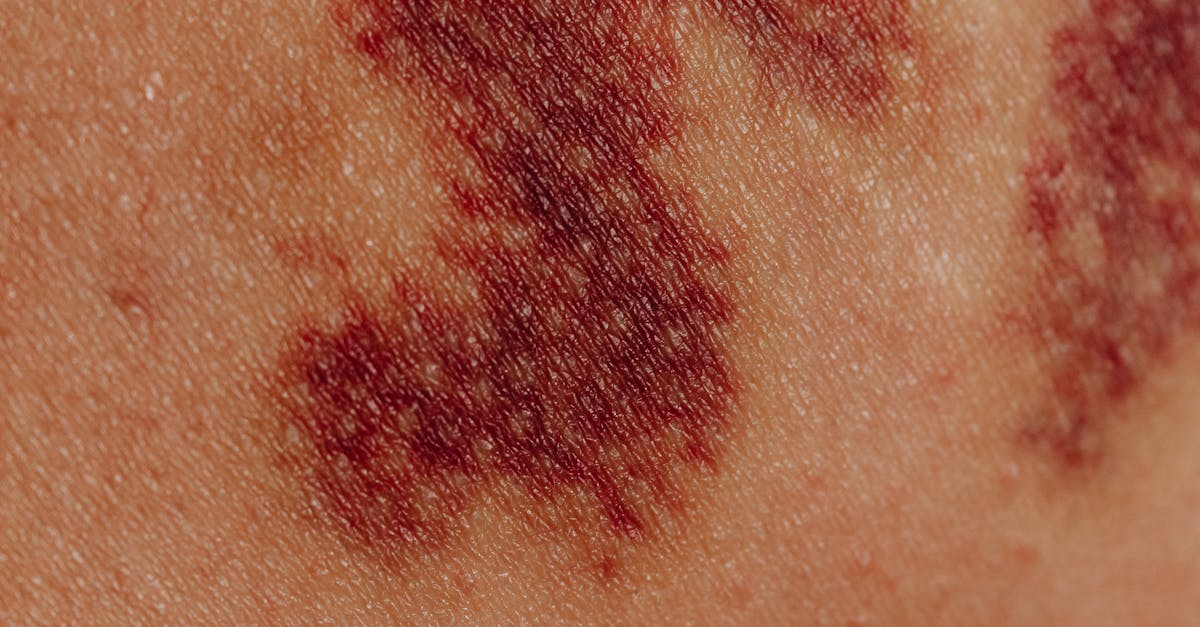
Dermatomyositis presents a unique inflammatory condition where characteristic skin changes often precede or accompany muscle weakness, making dermatological recognition crucial for early diagnosis and treatment. This rare autoimmune disorder affects both the skin and muscles, with distinctive cutaneous manifestations that are pathognomonic for the condition. The hallmark skin findings include the heliotrope rash—a purple-red discoloration around the eyelids—and Gottron's papules, which are raised, scaly lesions over the knuckles, elbows, and knees. These skin changes result from complement-mediated damage to small blood vessels in the skin and muscle, leading to characteristic inflammatory patterns that experienced clinicians can readily identify. The condition affects approximately 1 in 100,000 people annually, with a bimodal age distribution showing peaks in childhood and middle age. Beyond the classic skin findings, patients may develop a shawl sign (rash over the shoulders and upper back), mechanic's hands (rough, cracked skin on the palms and fingers), and periungual telangiectasias. The inflammatory process involves both cellular and humoral immune responses, with various myositis-specific antibodies correlating with different clinical phenotypes and prognoses. Early recognition of the dermatological features is particularly important because dermatomyositis can be associated with underlying malignancies in adult patients, making prompt evaluation and treatment essential for optimal outcomes.
4. Inflammatory Bowel Disease - Gut Inflammation's Cutaneous Echo
Inflammatory bowel disease (IBD), encompassing both Crohn's disease and ulcerative colitis, frequently manifests extraintestinal symptoms that can appear before, during, or after gastrointestinal symptoms develop, with skin manifestations being among the most common and recognizable. Approximately 15-20% of IBD patients develop cutaneous complications, which can be broadly categorized into specific manifestations directly related to IBD pathophysiology and reactive conditions triggered by the underlying inflammatory state. Erythema nodosum, characterized by tender, red nodules typically appearing on the shins, represents one of the most common skin manifestations and often correlates with active intestinal inflammation. Pyoderma gangrenosum, though less common, presents as painful ulcerative lesions that can be devastating if not recognized and treated promptly. The pathophysiology underlying these skin manifestations involves shared inflammatory pathways between the gut and skin, including dysregulated immune responses, increased intestinal permeability, and systemic circulation of inflammatory mediators. Other cutaneous manifestations include aphthous stomatitis, Sweet's syndrome, and various forms of vasculitis, each providing important clues about disease activity and treatment response. The timing of skin symptoms in relation to bowel symptoms varies considerably, with some patients developing cutaneous manifestations years before gastrointestinal symptoms become apparent, highlighting the importance of recognizing these dermatological harbingers in the context of potential IBD diagnosis and management.
5. Sarcoidosis - The Multi-System Inflammatory Puzzle
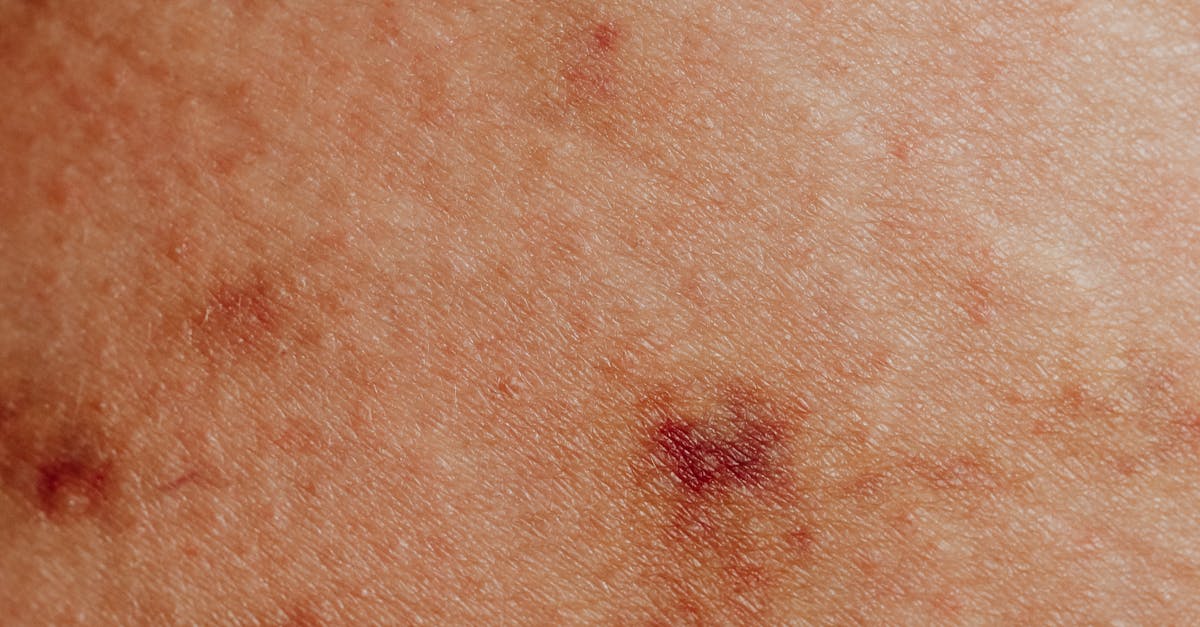
Sarcoidosis, a multi-system inflammatory disorder of unknown etiology, frequently presents with cutaneous manifestations that can be the first and sometimes only visible sign of this complex condition. Affecting approximately 10-20 per 100,000 people annually, sarcoidosis is characterized by the formation of non-caseating granulomas in various organs, with the skin being involved in 20-35% of cases. The dermatological presentations are remarkably diverse, ranging from erythema nodosum and lupus pernio to papular, nodular, and plaque-like lesions that can appear anywhere on the body. Lupus pernio, despite its name having no relation to lupus, represents a chronic form of cutaneous sarcoidosis that typically affects the nose, ears, and fingers, creating violaceous, indurated lesions that can be disfiguring if left untreated. The underlying inflammatory process involves an exaggerated immune response to unknown antigens, leading to the formation of epithelioid cell granulomas surrounded by lymphocytes and macrophages. These granulomas can resolve spontaneously or persist and cause tissue damage, making early recognition and appropriate treatment crucial. The skin lesions in sarcoidosis often provide accessible tissue for biopsy, making dermatological involvement particularly valuable for diagnosis. Additionally, the appearance and behavior of skin lesions can correlate with systemic disease activity, serving as a clinical barometer for monitoring treatment response and disease progression in this enigmatic inflammatory condition.
6. Vasculitis - When Blood Vessels Under Siege Signal Through Skin
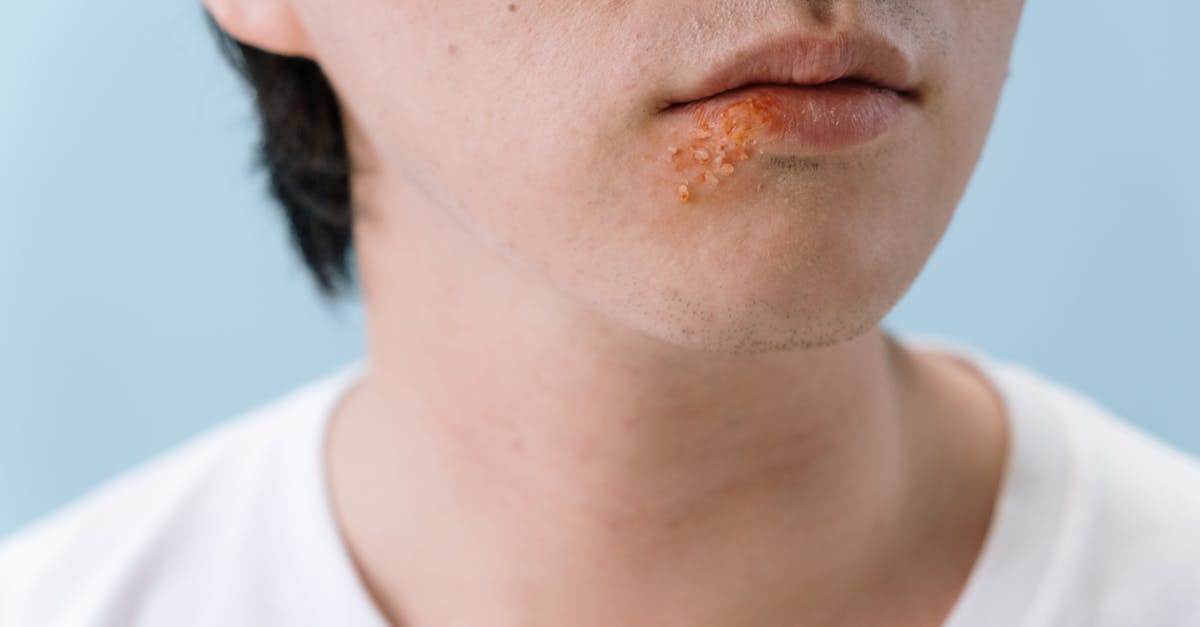
Vasculitis encompasses a group of inflammatory conditions affecting blood vessels of various sizes, and cutaneous manifestations often serve as the most visible and accessible indicators of this potentially serious systemic process. The skin's rich vascular network makes it particularly susceptible to vasculitic changes, with dermatological findings frequently being the presenting feature that leads to diagnosis. Small vessel vasculitis, such as hypersensitivity vasculitis or leukocytoclastic vasculitis, typically presents as palpable purpura—raised, purple lesions that do not blanch with pressure—most commonly appearing on the lower extremities due to gravitational effects on blood flow. Medium-sized vessel vasculitis, including polyarteritis nodosa, may present with livedo reticularis, subcutaneous nodules, or ulcerations, while large vessel involvement can cause claudication symptoms and asymmetric pulse findings. The pathophysiology involves immune complex deposition, direct antibody attack against vessel walls, or cell-mediated immune responses targeting vascular structures, leading to inflammation, necrosis, and potential organ dysfunction. Cutaneous vasculitis can be primary (isolated to the skin) or secondary to systemic conditions such as systemic lupus erythematosus, rheumatoid arthritis, or infections. The morphology, distribution, and associated symptoms of skin lesions provide crucial diagnostic clues about the underlying type of vasculitis, the size of vessels involved, and the urgency of systemic evaluation and treatment required to prevent serious complications.
7. Celiac Disease - Gluten's Inflammatory Signature on Skin
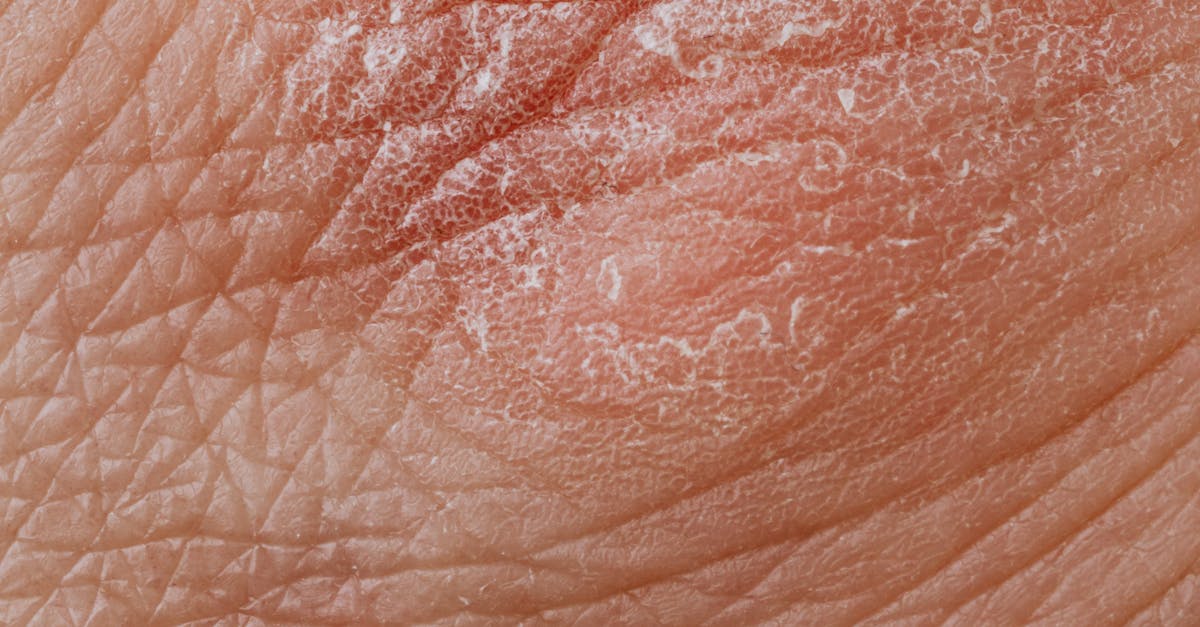
Celiac disease, an autoimmune disorder triggered by gluten consumption in genetically susceptible individuals, can manifest through a distinctive skin condition called dermatitis herpetiformis (DH), which often appears before gastrointestinal symptoms become apparent. This cutaneous manifestation affects approximately 15-25% of celiac patients and is characterized by intensely pruritic, vesicular lesions that typically appear symmetrically on the elbows, knees, buttocks, and scalp. The pathophysiology involves the deposition of IgA antibodies in the dermal papillae, triggered by the same autoimmune process that damages the small intestinal villi in response to gluten exposure. These antibodies cross-react with tissue transglutaminase in the skin, creating inflammatory lesions that can be exquisitely itchy and persistent. The inflammatory cascade begins in the gut, where gliadin peptides trigger an immune response in genetically predisposed individuals carrying HLA-DQ2 or HLA-DQ8 alleles, but the systemic nature of this autoimmune response means that skin manifestations can occur even in patients with minimal or absent gastrointestinal symptoms. Diagnosis is confirmed through skin biopsy showing characteristic IgA deposits and positive serology for anti-tissue transglutaminase or anti-endomysial antibodies. The skin lesions typically respond dramatically to a strict gluten-free diet, though improvement may take months to years, and temporary treatment with dapsone may be necessary for symptom control. Recognition of dermatitis herpetiformis is crucial because it indicates the presence of celiac disease and the need for lifelong dietary modification to prevent complications.
8. Thyroid Disorders - Hormonal Inflammation's Dermatological Display
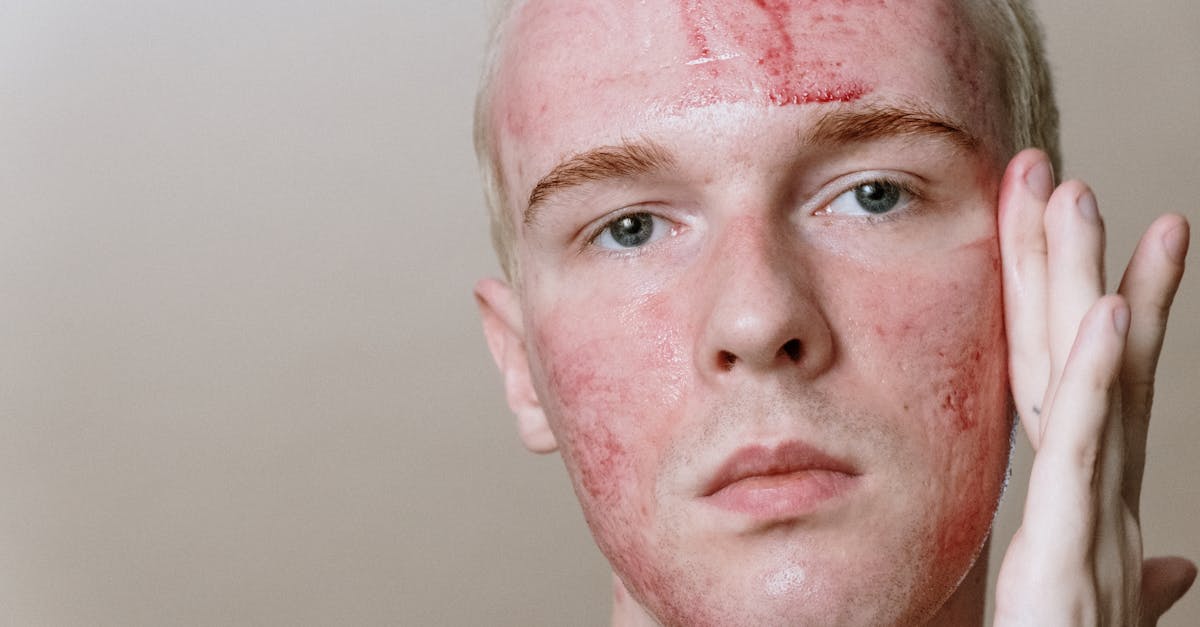
Thyroid dysfunction, whether hyperthyroid or hypothyroid, creates systemic inflammatory states that frequently manifest through distinctive cutaneous changes, often serving as early indicators of underlying endocrine pathology. In hyperthyroidism, particularly Graves' disease, the skin may develop pretibial myxedema (despite the name, this occurs in hyperthyroidism), characterized by thickened, waxy, orange-peel textured skin over the shins, resulting from glycosaminoglycan deposition triggered by thyroid-stimulating immunoglobulins. The inflammatory process in Graves' disease involves molecular mimicry, where antibodies directed against the thyroid-stimulating hormone receptor cross-react with similar receptors in skin and orbital tissues, creating localized inflammatory responses. Hyperthyroid patients also commonly develop warm, moist, smooth skin with increased vascularity and may show onycholysis (nail separation) and hair thinning. Conversely, hypothyroidism creates a different inflammatory milieu characterized by decreased metabolism and altered protein synthesis, leading to dry, coarse, cool skin with a yellowish tint from carotene accumulation, along with brittle hair and nails. The inflammatory component in hypothyroidism often relates to autoimmune thyroiditis (Hashimoto's disease), where chronic inflammation gradually destroys thyroid tissue. Both conditions can cause diffuse hair loss, changes in wound healing, and alterations in skin texture and appearance that may precede obvious systemic symptoms by months. Recognition of these dermatological changes is particularly important because thyroid disorders can significantly impact cardiovascular health, metabolism, and overall quality of life, making early detection and treatment crucial for optimal patient outcomes.
9. Diabetes Mellitus - Metabolic Inflammation's Cutaneous Consequences

Diabetes mellitus, characterized by chronic hyperglycemia and associated metabolic dysfunction, creates a pro-inflammatory state that frequently manifests through various cutaneous changes, many of which can appear before diabetes is formally diagnosed. The chronic elevation of blood glucose levels triggers advanced glycation end product (AGE) formation, oxidative stress, and inflammatory cascades that affect skin structure and function in multiple ways. Acanthosis nigricans, characterized by velvety, hyperpigmented plaques in flexural areas such as the neck, axillae, and groin, often represents an early sign of insulin resistance and can precede type 2 diabetes by years. This condition results from insulin-like growth factor stimulation of keratinocytes and dermal fibroblasts, creating the characteristic thickened, darkened skin appearance. Diabetic dermopathy, presenting as small, round, atrophic brown spots typically on the shins, affects up to 70% of diabetic patients and results from microangiopathy and reduced collagen synthesis. The inflammatory environment in diabetes also predisposes to various skin infections, delayed wound healing, and conditions such as necrobiosis lipoidica diabeticorum, which presents as yellowish, atrophic plaques with telangiectasias, typically on the shins. Digital sclerosis, causing thickened, waxy skin on the fingers and hands, can limit joint mobility and serves as a marker for potential diabetic complications. These cutaneous manifestations not only provide diagnostic clues but also serve as indicators of glycemic control and vascular health, making dermatological awareness crucial for diabetes prevention, early detection, and comprehensive management of this increasingly prevalent metabolic disorder.
10. Rheumatoid Arthritis - Joint Inflammation's Skin Manifestations

Rheumatoid arthritis (RA), a chronic autoimmune inflammatory disorder primarily affecting joints, frequently produces cutaneous manifestations that can provide important diagnostic and prognostic information about disease activity and severity. Approximately 20-30% of RA patients develop skin-related symptoms, with rheumatoid nodules being the most characteristic and common extraarticular manifestation. These firm, subcutaneous nodules typically appear over pressure points such as the elbows, knuckles, and Achilles tendons, and their presence often correlates with more severe, erosive disease and positive rheumatoid factor serology. The pathophysiology involves the formation of granulomatous inflammation with central necrosis, surrounded by epithelioid cells and lymphocytes, similar to the synovial inflammation seen in affected joints. Rheumatoid vasculitis, though less common in the modern era of effective disease-modifying treatments, can present with nail fold infarcts, digital gangrene, or leg ulcers, indicating severe systemic inflammation and poor prognosis. Palmar erythema and livedo reticularis may also occur, reflecting the systemic inflammatory state and vascular involvement characteristic of RA. The inflammatory cytokines central to RA pathogenesis, particularly tumor necrosis factor-alpha, interleukin-1, and interleukin-6, create systemic effects that extend beyond the joints to affect skin, blood vessels, and other organs. Cutaneous manifestations in RA often parallel joint disease activity, making skin examination an important component of disease monitoring. Additionally, some skin changes may result from medications used to treat RA, highlighting the importance of distinguishing between disease-related and treatment-related dermatological findings in comprehensive patient care.
11. Behçet's Disease - The Silk Road Inflammatory Syndrome

Behçet's disease, a chronic multisystem vasculitis most commonly found along the ancient Silk Road trade routes, presents with a constellation of inflammatory symptoms where mucocutaneous manifestations often serve as the earliest and most consistent features. This complex inflammatory disorder affects blood vessels of all sizes and can involve virtually any organ system, but oral and genital ulcerations, along with various skin lesions, form the cornerstone of diagnosis. Recurrent painful oral aphthous ulcers occur in nearly 100% of patients and are often the presenting symptom, appearing as deep, well-demarcated ulcers with yellow bases and erythematous borders that can significantly impact quality of life. Genital ulcerations, affecting 60-90% of patients, are typically deeper and more painful than oral lesions and may heal with scarring. The skin manifestations are diverse and include erythema nodosum-like lesions, pseudofolliculitis, papulopustular lesions, and acneiform eruptions, each reflecting different aspects of the underlying inflammatory process. A unique feature of Behçet's disease is pathergy, an exaggerated inflammatory response to minor trauma such as needle pricks, which