10 Autoimmune Conditions That First Appear as Skin or Eye Changes
The human body possesses an remarkable ability to communicate distress through its most visible organs—the skin and eyes. These external manifestations often serve as the first harbingers of complex autoimmune conditions brewing beneath the surface, acting as early warning systems that can provide crucial diagnostic clues years before systemic symptoms emerge. Autoimmune diseases, characterized by the immune system's misguided attack on healthy tissues, frequently announce their presence through distinctive dermatological and ophthalmological changes that trained healthcare providers recognize as red flags. From the characteristic butterfly rash of lupus to the dry, gritty sensation of Sjögren's syndrome, these surface-level symptoms represent the tip of an immunological iceberg that requires immediate attention and comprehensive evaluation. Understanding these early visual cues can mean the difference between prompt intervention and irreversible organ damage, making awareness of these conditions essential for both patients and healthcare providers. This comprehensive exploration will examine ten significant autoimmune conditions that commonly present with skin or eye manifestations, providing insight into their recognition, progression, and the critical importance of early detection in preserving long-term health outcomes.
1. Systemic Lupus Erythematosus - The Great Imitator's Telltale Mask
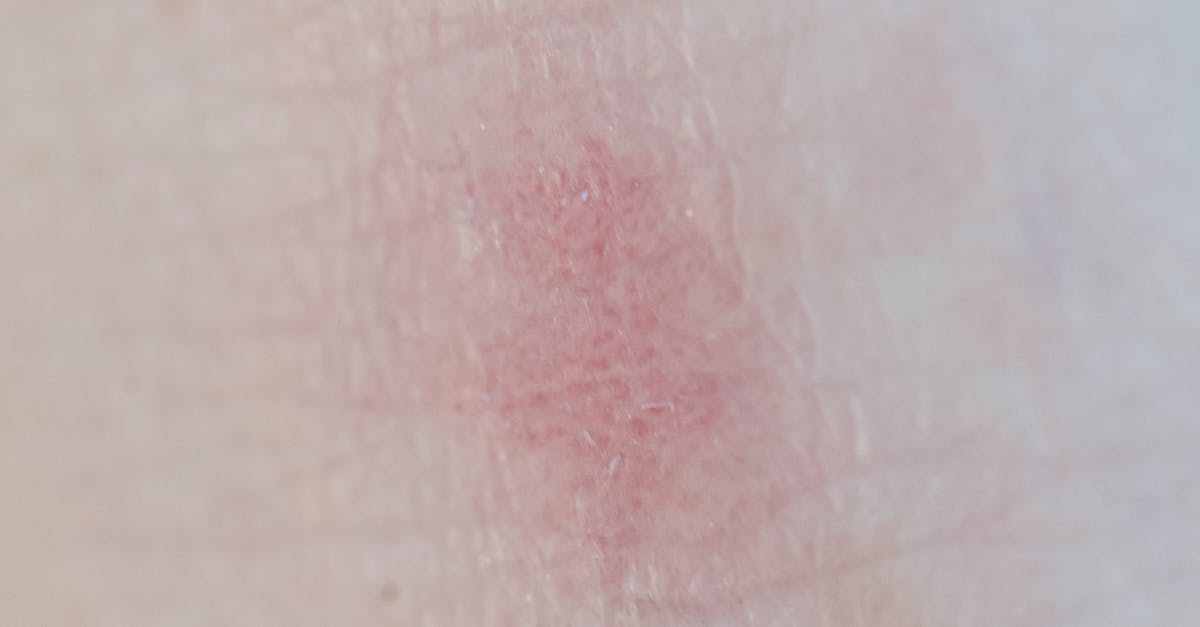
Systemic lupus erythematosus (SLE) stands as perhaps the most recognizable autoimmune condition presenting with distinctive skin manifestations, earning its reputation as "the great imitator" due to its ability to mimic numerous other diseases. The hallmark malar rash, commonly known as the "butterfly rash," appears as a distinctive red, flat or raised rash spreading across both cheeks and the bridge of the nose, resembling the wings of a butterfly. This characteristic presentation occurs in approximately 30-60% of lupus patients and often worsens with sun exposure due to photosensitivity, another common feature of the disease. Beyond the classic butterfly pattern, lupus can manifest through discoid lesions—coin-shaped, scaly patches that can cause permanent scarring and hair loss when they occur on the scalp. The condition also frequently affects the eyes, causing dry eye syndrome, retinal vasculitis, and in severe cases, vision-threatening complications such as optic neuritis. These ocular manifestations can occur in up to 30% of lupus patients and may precede other systemic symptoms by months or even years. The skin and eye changes in lupus often fluctuate with disease activity, serving as valuable indicators for monitoring treatment response and predicting flares. Early recognition of these dermatological and ophthalmological signs is crucial, as prompt treatment with immunosuppressive medications can prevent irreversible organ damage to the kidneys, heart, and central nervous system.
2. Sjögren's Syndrome - When Dryness Signals Deeper Trouble

Sjögren's syndrome primarily targets the body's moisture-producing glands, creating a cascade of symptoms that begin with seemingly simple dryness but can evolve into serious systemic complications. The condition most commonly presents with keratoconjunctivitis sicca, or severe dry eyes, which patients often describe as feeling like sand or grit in their eyes, accompanied by burning, itching, and a sensation of heaviness in the eyelids. This ocular dryness occurs due to lymphocytic infiltration and destruction of the lacrimal glands, leading to decreased tear production and altered tear composition. The eyes may appear red and inflamed, with patients experiencing difficulty wearing contact lenses, increased sensitivity to light, and blurred vision that improves with blinking. Concurrently, the skin often becomes noticeably dry, rough, and prone to irritation, as the condition affects sebaceous glands and reduces natural oil production. Some patients develop a distinctive purplish rash on the lower legs called hypergammaglobulinemic purpura, which appears as small, raised spots and indicates vascular involvement. The combination of dry eyes and dry mouth (xerostomia) forms the classic presentation, but skin manifestations can include increased photosensitivity, easy bruising, and delayed wound healing. These seemingly minor symptoms can significantly impact quality of life and may precede more serious complications such as lymphoma, kidney disease, and neurological problems. Early recognition and treatment with artificial tears, immunosuppressive medications, and lifestyle modifications can help preserve glandular function and prevent progression to more severe systemic involvement.
3. Dermatomyositis - The Muscle Disease That Shows Its Face First
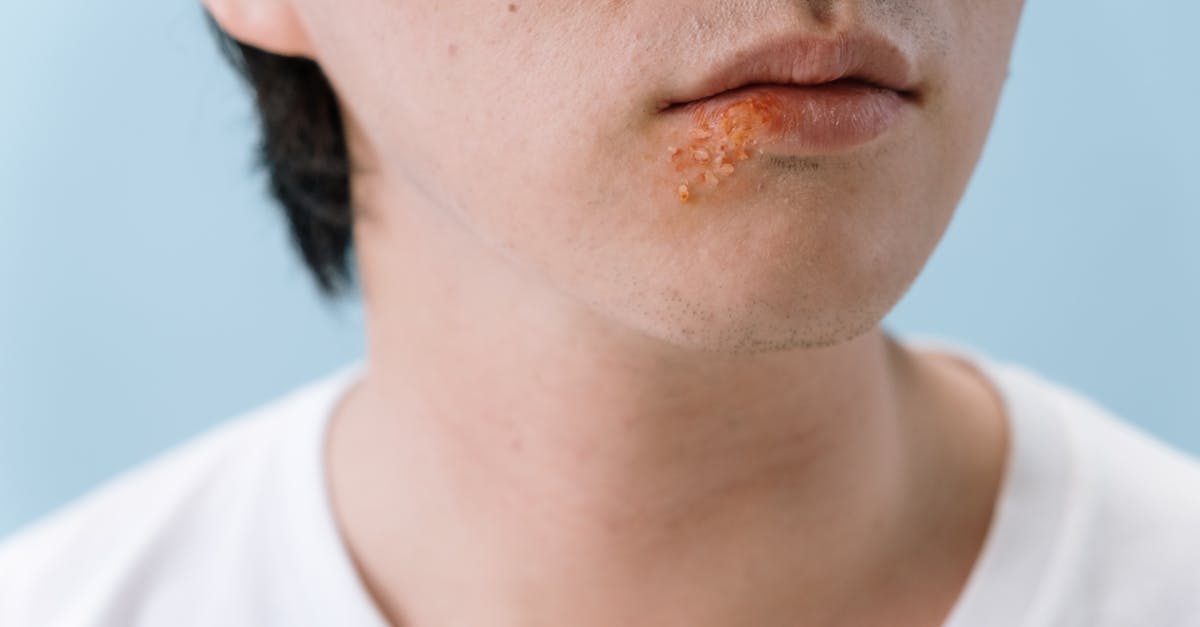
Dermatomyositis presents a unique paradox in autoimmune medicine, as its characteristic skin manifestations often appear months or even years before the muscle weakness that defines the condition becomes apparent. The pathognomonic Gottron's papules appear as violet-colored, scaly bumps over the knuckles, elbows, and knees, creating a distinctive pattern that experienced dermatologists can recognize immediately. Equally characteristic is the heliotrope rash, a purplish-red discoloration affecting the upper eyelids, often accompanied by periorbital edema that gives patients a distinctive "sleepy" appearance. This facial involvement frequently extends to include a photosensitive rash across the cheeks, forehead, and neck, creating a shawl-like distribution that worsens with sun exposure. The condition also produces distinctive changes around the nail beds, including dilated capillary loops visible to the naked eye and painful, cracked skin along the sides and tips of the fingers known as "mechanic's hands." These cutaneous manifestations can be accompanied by subcutaneous calcifications, particularly in juvenile cases, creating firm nodules beneath the skin that may ulcerate and become infected. While muscle weakness typically develops gradually, affecting proximal muscles first, the skin changes often remain the most visible and distressing aspect of the disease for patients. The presence of these characteristic dermatological findings, particularly in combination with elevated muscle enzymes and specific autoantibodies, helps establish the diagnosis and guide treatment decisions. Early recognition is crucial because dermatomyositis carries an increased risk of malignancy, particularly in older adults, necessitating comprehensive cancer screening alongside immunosuppressive treatment.
4. Scleroderma - When Skin Becomes the Enemy
Scleroderma, or systemic sclerosis, transforms the body's largest organ into a rigid, thickened barrier that restricts movement and function while serving as a visible marker of internal organ involvement. The condition typically begins with Raynaud's phenomenon, where fingers and toes turn white, then blue, then red in response to cold or stress, indicating vascular dysfunction that will eventually affect internal organs. As the disease progresses, the skin becomes increasingly tight, shiny, and difficult to pinch, starting in the fingers and hands before potentially spreading to the arms, face, and trunk. This skin thickening, called sclerodactyly when it affects the fingers, can severely limit range of motion and make simple tasks like making a fist or opening the mouth challenging. Facial involvement creates a characteristic mask-like appearance with thinning of the lips, restriction of mouth opening, and the development of small blood vessel dilations called telangiectasias around the mouth and on the fingers. The condition also produces distinctive changes around the fingernails, including painful digital ulcers that heal slowly and may become infected, along with visible capillary abnormalities that can be observed with simple magnification. Calcinosis, the deposition of calcium deposits under the skin, can create painful nodules that may rupture and drain a chalky white substance. These dramatic skin changes often overshadow the equally serious internal manifestations affecting the lungs, heart, kidneys, and gastrointestinal tract. Early recognition of these cutaneous signs allows for prompt initiation of treatments that can slow disease progression and prevent life-threatening complications such as pulmonary hypertension and renal crisis.
5. Behçet's Disease - The Silk Road's Inflammatory Legacy

Behçet's disease presents a complex constellation of symptoms that primarily affect the mucous membranes and skin, creating a pattern of recurrent inflammation that can be both painful and visually distinctive. The condition most commonly announces itself through recurrent oral ulcers that are typically larger, deeper, and more painful than common canker sores, often appearing in clusters and taking weeks to heal completely. These aphthous ulcers can occur anywhere in the mouth but frequently affect the tongue, lips, and soft palate, making eating, drinking, and speaking uncomfortable. Genital ulcers, though less common, are equally characteristic and often more painful, appearing on the vulva, vagina, penis, or scrotum and potentially leaving permanent scarring. The skin manifestations of Behçet's disease include erythema nodosum-like lesions, which appear as tender, red nodules typically on the lower legs, and papulopustular lesions that resemble acne but occur in unusual locations and patterns. A unique feature of Behçet's disease is pathergy, an abnormal skin reaction to minor trauma such as needle pricks, where small pustules develop at injury sites within 24-48 hours. Ocular involvement occurs in approximately half of patients and can be the most serious manifestation, presenting as recurrent uveitis with eye pain, redness, photophobia, and blurred vision that can lead to permanent vision loss if untreated. The combination of oral ulcers, genital ulcers, skin lesions, and eye inflammation forms the classic tetrad, though patients rarely present with all symptoms simultaneously. This chronic, relapsing condition requires careful monitoring and aggressive treatment to prevent serious complications, particularly vision-threatening eye disease and neurological involvement.
6. Antiphospholipid Syndrome - When Blood Clots Leave Their Mark

Antiphospholipid syndrome (APS) creates a unique pattern of skin manifestations that reflect the underlying hypercoagulable state and vascular dysfunction characteristic of this autoimmune condition. The most distinctive dermatological feature is livedo reticularis, a net-like, purplish mottling of the skin that becomes more pronounced in cold temperatures and typically affects the arms, legs, and trunk. This reticulated pattern results from impaired blood flow in the small vessels of the skin and serves as a visible marker of the systemic vascular abnormalities that predispose patients to thrombosis. Patients may also develop chronic leg ulcers, particularly around the ankles, that heal slowly and tend to recur due to poor circulation and the prothrombotic state. These ulcers can be painful, prone to infection, and may leave permanent scarring or pigmentation changes. Digital ischemia represents another serious manifestation, where reduced blood flow to the fingers or toes can cause pain, color changes, and in severe cases, tissue death requiring amputation. The condition can also cause splinter hemorrhages under the fingernails and small, painful infarcts in the fingertips. Ocular manifestations of APS include retinal vein or artery occlusions, which can present as sudden vision loss, visual field defects, or retinal hemorrhages visible on ophthalmologic examination. Some patients develop amaurosis fugax, or temporary vision loss, which serves as a warning sign for potential stroke. The skin and eye changes in APS often precede major thrombotic events such as stroke, heart attack, or pulmonary embolism, making recognition of these early signs crucial for preventing life-threatening complications through anticoagulation therapy.
7. Vogt-Koyanagi-Harada Disease - The Eyes as Windows to Systemic Inflammation

Vogt-Koyanagi-Harada (VKH) disease represents a fascinating example of how autoimmune inflammation targeting melanocytes can simultaneously affect multiple organ systems, with the eyes serving as the primary battleground for this complex condition. The disease typically begins with a prodromal phase characterized by flu-like symptoms, followed by the acute uveitic phase where patients develop severe bilateral panuveitis with eye pain, photophobia, blurred vision, and the pathognomonic "sunset glow" fundus appearance visible on ophthalmologic examination. This ocular inflammation can be so severe that it causes exudative retinal detachments, leading to significant vision impairment if not treated promptly and aggressively. The chronic phase brings distinctive integumentary changes that reflect the autoimmune attack on melanocytes throughout the body. Patients develop poliosis, a striking whitening of the eyelashes, eyebrows, and hair that can occur in patches or affect entire regions, creating a distinctive appearance that often causes significant psychological distress. Vitiligo-like depigmented patches appear on the skin, typically in a symmetrical distribution affecting the face, neck, and trunk, while alopecia can cause patchy or diffuse hair loss. The skin may also develop a distinctive "sugiura sign," where depigmented patches appear around the eyes, creating a characteristic mask-like appearance. Some patients experience auditory symptoms including tinnitus, hearing loss, and vertigo due to involvement of the inner ear's melanocytes. The combination of severe bilateral uveitis with these characteristic skin and hair changes creates a diagnostic picture that, while rare, is unmistakable when fully developed. Early recognition and treatment with high-dose corticosteroids and immunosuppressive agents are crucial for preserving vision and preventing the chronic complications that can significantly impact quality of life.
8. Relapsing Polychondritis - When Cartilage Becomes the Target
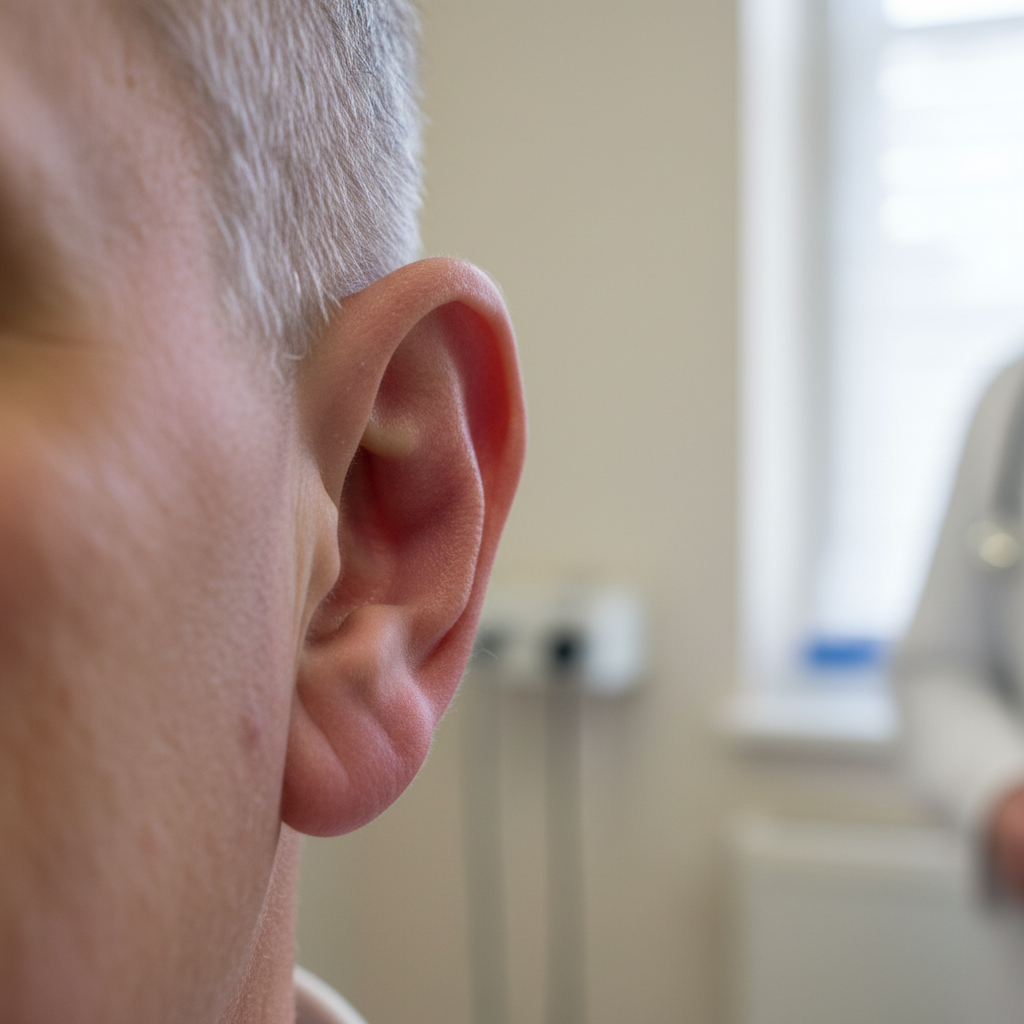
Relapsing polychondritis presents a unique clinical picture where inflammation targets cartilaginous structures throughout the body, creating distinctive visible changes that often serve as the first clue to this rare but serious autoimmune condition. The most characteristic and often initial manifestation is auricular chondritis, where one or both ears become red, swollen, and exquisitely tender, with the inflammation typically sparing the soft, non-cartilaginous earlobe, creating a distinctive pattern that experienced clinicians recognize immediately. This ear involvement can be episodic, with attacks lasting days to weeks before resolving, only to recur weeks or months later, often affecting the opposite ear or returning to the same location. Over time, repeated episodes can lead to permanent deformation of the ear's architecture, creating a characteristic "cauliflower ear" appearance as the cartilage becomes weakened and collapses. Nasal involvement is equally dramatic, with inflammation of the nasal cartilage causing pain, swelling, and eventual collapse of the nasal bridge, leading to a distinctive "saddle nose" deformity that can significantly impact both appearance and breathing function. Ocular manifestations occur in approximately 60% of patients and can include conjunctivitis, episcleritis, scleritis, and uveitis, with some patients developing vision-threatening complications such as corneal perforation or retinal vasculitis. The skin changes in relapsing polychondritis can include livedo reticularis, erythema nodosum-like lesions, and purpura, reflecting the systemic vascular inflammation that accompanies the cartilage destruction. Perhaps most concerning is the potential for laryngeal and tracheal involvement, which can cause hoarseness, stridor, and life-threatening airway obstruction. The episodic nature of the condition, combined with its rarity, often leads to delayed diagnosis, making awareness of these characteristic ear and nose changes crucial for early recognition and treatment.
9. Pemphigus Vulgaris - When Skin Loses Its Cohesion

Pemphigus vulgaris represents one of the most serious autoimmune blistering diseases, where antibodies target the proteins that hold skin cells together, creating a condition that can be both visually dramatic and life-threatening if left untreated. The disease typically begins insidiously with painful oral lesions that patients often mistake for severe canker sores or dental problems, but these erosions are characteristically more extensive, persistent, and painful than typical mouth ulcers. These oral lesions can affect any part of the mouth, including the gums, tongue, palate, and throat, making eating, drinking, and speaking extremely difficult and often leading to significant weight loss and dehydration. The transition from oral to cutaneous involvement marks a critical phase in the disease progression, with flaccid blisters appearing on normal-appearing skin, typically starting on the scalp, face, chest, or back. These blisters are characteristically fragile and rupture easily, leaving behind painful, raw erosions that heal slowly and are prone to secondary bacterial infection. The Nikolsky sign, where gentle pressure on apparently normal skin causes the epidermis to separate and slide away, becomes positive and serves as an important diagnostic clue. Unlike other blistering conditions, pemphigus blisters arise from within the epidermis rather than at the dermal-epidermal junction, creating the characteristic histologic pattern of acantholysis. The condition can also affect other mucous membranes, including the conjunctiva, nasal passages, esophagus, and genital areas, creating a widespread erosive process that significantly impacts quality of life. Without treatment, pemphigus vulgaris has a high mortality rate due to fluid loss, electrolyte imbalances, and secondary infections, but early recognition and treatment with high-dose corticosteroids and immunosuppressive agents can achieve remission in most patients. The key to successful management lies in recognizing the early oral manifestations and understanding that persistent, painful mouth sores in adults warrant immediate dermatologic evaluation.
10. Inflammatory Bowel Disease - When Gut Inflammation Shows on the Surface
Inflammatory bowel disease, encompassing both Crohn's disease and ulcerative colitis, frequently manifests through extraintestinal symptoms that can appear on the skin and eyes, sometimes preceding gastrointestinal symptoms by months or years. The most common dermatological manifestation is erythema nodosum, appearing as tender, red nodules typically on the shins and ankles, which often correlates with active intestinal inflammation and can serve as a marker for disease flares. These painful lesions can make walking difficult and may leave behind areas of hyperpigmentation as they resolve. Pyoderma gangrenosum represents a more serious skin manifestation, beginning as small pustules or nodules that rapidly progress to deep, painful ulcers with