8 Appetite Changes Linked to Hormonal and Mental Health Conditions
The intricate relationship between appetite, hormonal fluctuations, and mental health represents one of the most fascinating yet underexplored aspects of human physiology and psychology. Our eating patterns serve as a complex barometer of internal health, reflecting the delicate interplay between neurotransmitters, hormones, and emotional states that govern our daily lives. When hormonal imbalances occur—whether due to thyroid dysfunction, reproductive hormone fluctuations, or stress-related cortisol changes—they create cascading effects that fundamentally alter how our brains perceive hunger, satiety, and food reward. Similarly, mental health conditions such as depression, anxiety, and eating disorders can dramatically reshape appetite through their impact on brain chemistry and behavioral patterns. Understanding these eight key appetite changes linked to hormonal and mental health conditions is crucial for both healthcare providers and individuals seeking to decode their body's signals. This comprehensive exploration reveals how conditions ranging from hypothyroidism to seasonal affective disorder can manifest through distinct appetite patterns, offering valuable insights into the body's remarkable ability to communicate distress through our relationship with food.
1. Thyroid Dysfunction and Metabolic Appetite Disruption
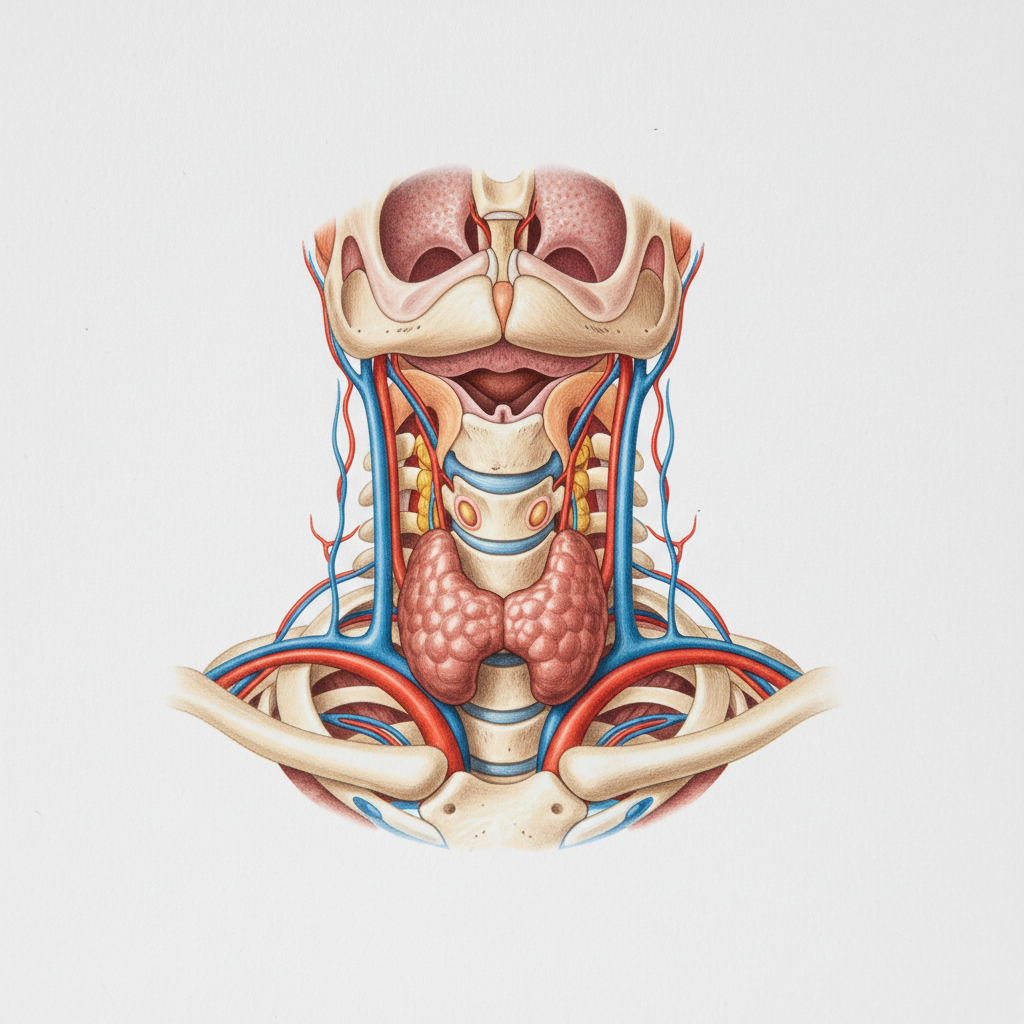
Thyroid disorders represent one of the most significant hormonal causes of appetite changes, with both hyperthyroidism and hypothyroidism creating distinct patterns of eating behavior that often serve as early warning signs of thyroid dysfunction. In hyperthyroidism, the overproduction of thyroid hormones accelerates metabolic processes throughout the body, leading to dramatically increased appetite despite concurrent weight loss—a paradoxical situation that can be both confusing and concerning for patients. The thyroid hormones T3 and T4 directly influence the hypothalamus, the brain's appetite control center, causing individuals to experience intense hunger and cravings, particularly for high-calorie foods that can provide quick energy to match their elevated metabolic demands. Conversely, hypothyroidism creates the opposite scenario, where decreased thyroid hormone production slows metabolism and often leads to reduced appetite, though weight gain typically occurs due to the body's decreased ability to burn calories efficiently. Research has shown that thyroid hormones interact with leptin and ghrelin, the primary hunger and satiety hormones, creating a complex feedback loop that can take months to normalize even after thyroid hormone levels are restored through medication. The appetite changes associated with thyroid dysfunction often persist beyond the initial treatment period, requiring careful monitoring and sometimes additional interventions to help patients reestablish healthy eating patterns and achieve optimal metabolic function.