12 Bleeding Pattern Variations That Signal Clotting and Platelet Disorders
The human body's hemostatic system represents one of nature's most sophisticated biological mechanisms, orchestrating a delicate balance between bleeding and clotting that maintains vascular integrity while preventing life-threatening hemorrhage. When this intricate system malfunctions, it communicates through a complex vocabulary of bleeding patterns that serve as diagnostic windows into underlying platelet and coagulation disorders. These bleeding manifestations are not merely symptoms but rather precise indicators that reflect specific defects in platelet function, coagulation cascade abnormalities, or vascular integrity compromises. Understanding these bleeding pattern variations is crucial for healthcare professionals, as early recognition can mean the difference between timely intervention and potentially catastrophic outcomes. From the subtle appearance of petechiae suggesting thrombocytopenia to the dramatic presentation of deep tissue hematomas indicating severe coagulation factor deficiencies, each bleeding pattern tells a unique story about the underlying pathophysiology. This comprehensive exploration will examine twelve distinct bleeding pattern variations that serve as critical diagnostic markers, providing healthcare providers and patients with essential knowledge to recognize, interpret, and respond appropriately to these important clinical signs that may herald serious hematological disorders requiring immediate medical attention.
1. Petechial Bleeding - The Pinpoint Indicators of Platelet Dysfunction
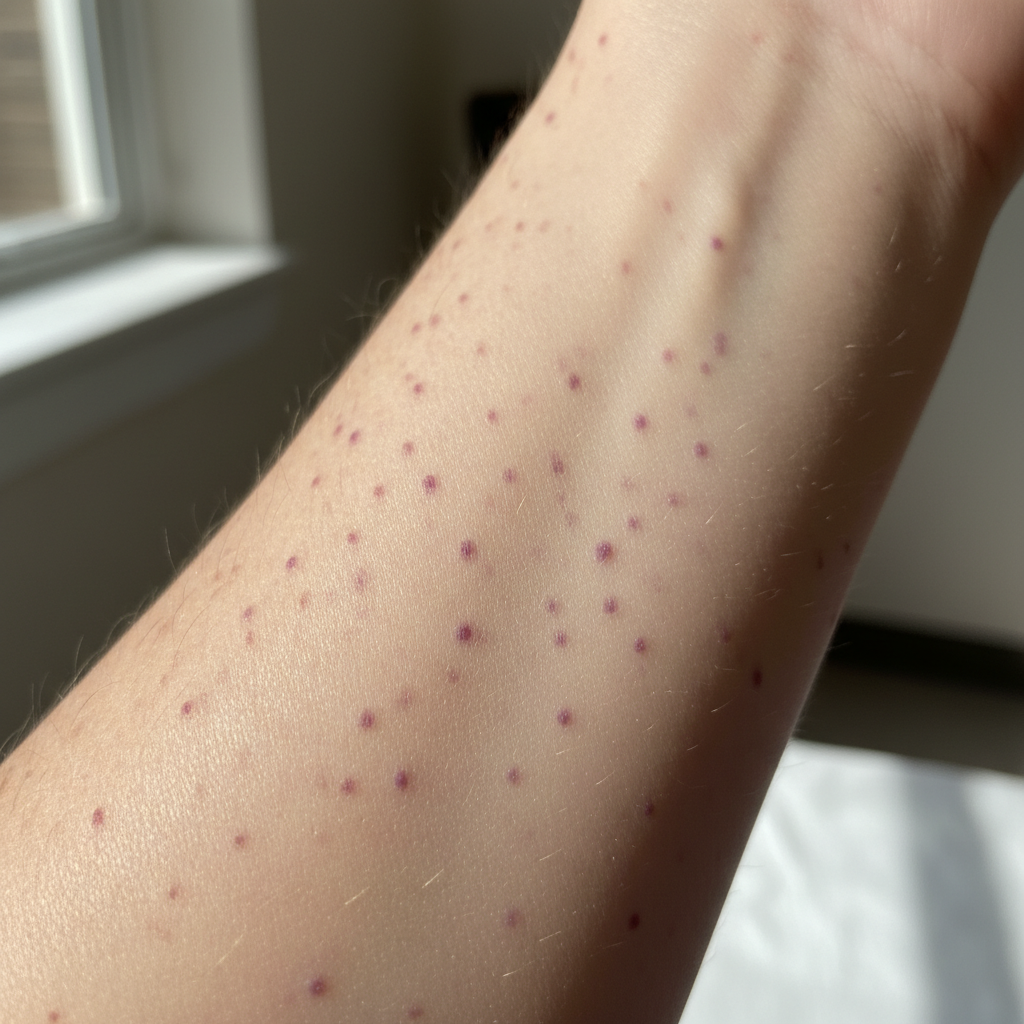
Petechial bleeding represents one of the most characteristic and diagnostically significant bleeding patterns associated with platelet disorders, manifesting as tiny, pinpoint-sized hemorrhages that appear as red or purple spots measuring less than 2 millimeters in diameter on the skin and mucous membranes. These minute bleeding points occur when capillaries rupture due to inadequate platelet plug formation, typically indicating thrombocytopenia (low platelet count) or qualitative platelet dysfunction. The distribution pattern of petechiae provides valuable diagnostic clues, with gravity-dependent areas such as the lower extremities, ankles, and feet commonly affected first, followed by areas of increased pressure or trauma. Unlike larger purpuric lesions, petechiae do not blanch with pressure and represent actual extravasation of red blood cells into the surrounding tissue. The density and progression of petechial bleeding often correlates with the severity of the underlying platelet disorder, with platelet counts below 50,000 per microliter typically associated with spontaneous petechial formation. Common causes include immune thrombocytopenic purpura (ITP), drug-induced thrombocytopenia, bone marrow disorders, and inherited platelet function defects. The presence of petechiae, particularly when accompanied by other bleeding manifestations, warrants immediate hematological evaluation including complete blood count with platelet assessment, peripheral blood smear examination, and potentially bone marrow biopsy to determine the underlying etiology and guide appropriate therapeutic intervention.