12 Skin Color Changes Doctors Use as Diagnostic Clues
4. Erythema - The Red Flag of Inflammation
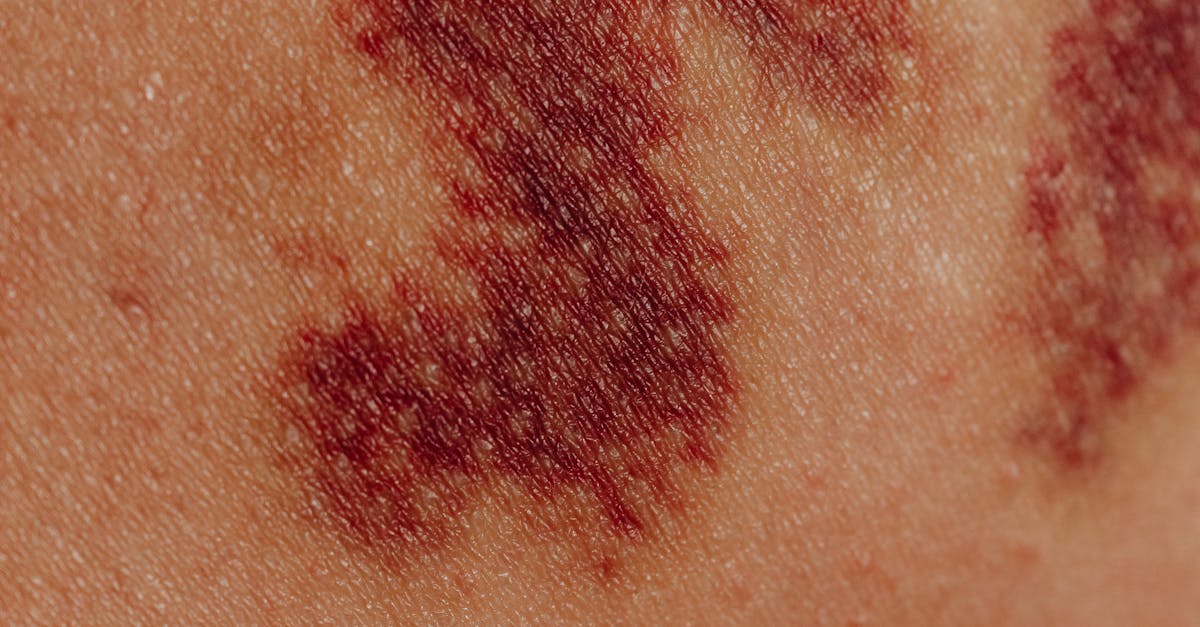
Erythema presents as abnormal redness of the skin caused by increased blood flow to the superficial capillaries, serving as a fundamental indicator of inflammation, infection, or vascular changes within affected tissues. This distinctive red discoloration occurs when arterioles and capillaries dilate in response to various stimuli, including inflammatory mediators, heat, mechanical irritation, or immune system activation. The clinical assessment of erythema involves evaluating its distribution, intensity, associated symptoms, and response to pressure, with blanching erythema (which temporarily disappears with pressure) indicating vasodilation, while non-blanching erythema may suggest more serious conditions involving bleeding into the skin. Localized erythema commonly accompanies skin infections such as cellulitis, where bacterial invasion triggers an intense inflammatory response characterized by warmth, swelling, and tenderness in addition to the characteristic redness. Systemic conditions can also manifest with widespread erythema, including autoimmune disorders like systemic lupus erythematosus, which may present with the classic butterfly rash across the cheeks and nose bridge. Drug reactions frequently cause erythematous eruptions ranging from mild skin redness to severe, life-threatening conditions like Stevens-Johnson syndrome or toxic epidermal necrolysis. Healthcare providers must carefully evaluate the pattern and progression of erythema, as certain distributions can provide specific diagnostic clues, such as the photosensitive distribution seen in lupus or the characteristic pattern of erythema migrans associated with Lyme disease. The temporal relationship between erythema onset and potential triggers, including medications, infections, or environmental exposures, provides crucial information for accurate diagnosis and appropriate treatment planning.