12 Lower Leg Skin Changes That Reflect Vascular and Circulatory Health
The lower extremities serve as remarkable indicators of our cardiovascular and circulatory well-being, with the skin acting as a visible canvas that displays the intricate relationship between blood flow, tissue perfusion, and overall vascular health. The lower legs, positioned furthest from the heart and subject to gravitational challenges, are particularly vulnerable to circulatory compromises that manifest through distinctive skin changes. These dermatological alterations often represent the earliest visible signs of underlying vascular conditions, ranging from venous insufficiency and arterial disease to systemic circulation disorders. Healthcare professionals have long recognized that careful observation of lower leg skin characteristics can provide invaluable insights into a patient's cardiovascular status, often revealing conditions before they progress to more serious complications. The skin's appearance, texture, color, temperature, and healing capacity all reflect the adequacy of blood supply and the efficiency of venous return. Understanding these visual cues enables early intervention and appropriate management of vascular conditions that might otherwise go undetected until advanced stages. This comprehensive exploration examines twelve specific skin changes that serve as critical indicators of vascular and circulatory health, providing both medical professionals and individuals with essential knowledge for recognizing and addressing potential circulation issues before they become life-threatening complications.
1. Chronic Venous Stasis Dermatitis - The Foundation of Venous Disease
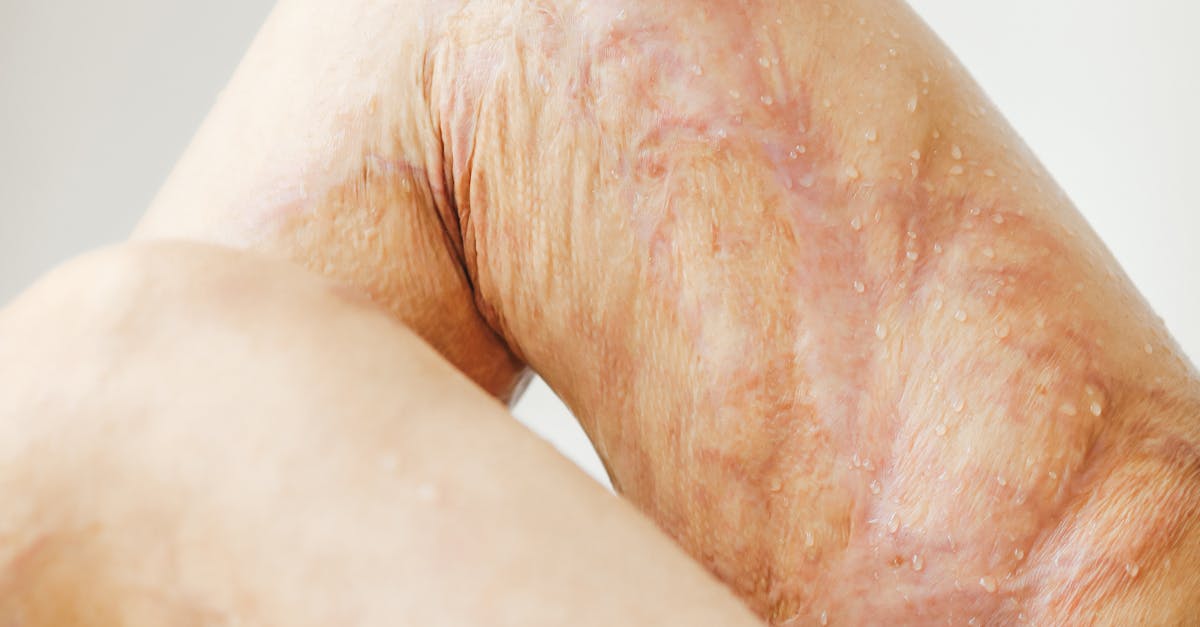
Chronic venous stasis dermatitis represents one of the most common and recognizable manifestations of venous insufficiency, characterized by inflammatory skin changes that develop as a direct result of prolonged venous hypertension and impaired venous return. This condition typically begins with subtle erythema and scaling around the ankles and gradually progresses to involve larger areas of the lower leg, creating a distinctive pattern of inflammation that reflects the underlying hemodynamic dysfunction. The pathophysiology involves increased venous pressure leading to capillary leakage, tissue edema, and subsequent inflammatory cascade that damages the skin's protective barrier. Patients often experience intense pruritus, which can lead to secondary bacterial infections and further skin deterioration through scratching and trauma. The affected skin becomes increasingly sensitive and reactive, developing a characteristic eczematous appearance with scaling, weeping, and crusting. Over time, the inflammatory process can lead to permanent skin changes including hyperpigmentation, fibrosis, and ultimately venous leg ulceration. Early recognition and treatment of venous stasis dermatitis are crucial for preventing progression to more severe complications, with management focusing on improving venous return through compression therapy, elevation, and addressing underlying venous pathology. The presence of stasis dermatitis should prompt comprehensive evaluation of the venous system to identify and treat any correctable causes of venous insufficiency.