12 Achilles Tendon and Heel Appearance Changes Linked to Metabolic Disorders
# 12 Achilles Tendon and Heel Appearance Changes Linked to Metabolic Disorders: A Comprehensive Medical Analysis
The human foot and ankle complex serves as a remarkable window into systemic health, with the Achilles tendon and heel region functioning as sensitive indicators of underlying metabolic dysfunction. Recent advances in medical research have illuminated a profound connection between various metabolic disorders and distinctive changes in the appearance, structure, and function of these critical lower extremity components. From the crystalline deposits of gout that create characteristic nodular deformities to the glycation-induced stiffening seen in diabetes mellitus, metabolic disturbances manifest in predictable and diagnostically significant ways throughout the heel and Achilles tendon complex. This comprehensive analysis explores twelve specific appearance changes that serve as clinical markers for metabolic disorders, ranging from the subtle early signs of insulin resistance to the dramatic structural alterations associated with advanced endocrine dysfunction. Understanding these connections empowers healthcare providers to recognize systemic disease through careful examination of the lower extremities, while simultaneously helping patients appreciate how their metabolic health directly impacts their mobility and quality of life. The following detailed exploration reveals how conditions such as diabetes, thyroid disorders, lipid abnormalities, and inflammatory metabolic syndromes leave their distinctive signatures on the heel and Achilles tendon, creating a roadmap for early detection, intervention, and comprehensive metabolic management.
1. Diabetic Achilles Tendon Thickening and Glycation-Induced Changes
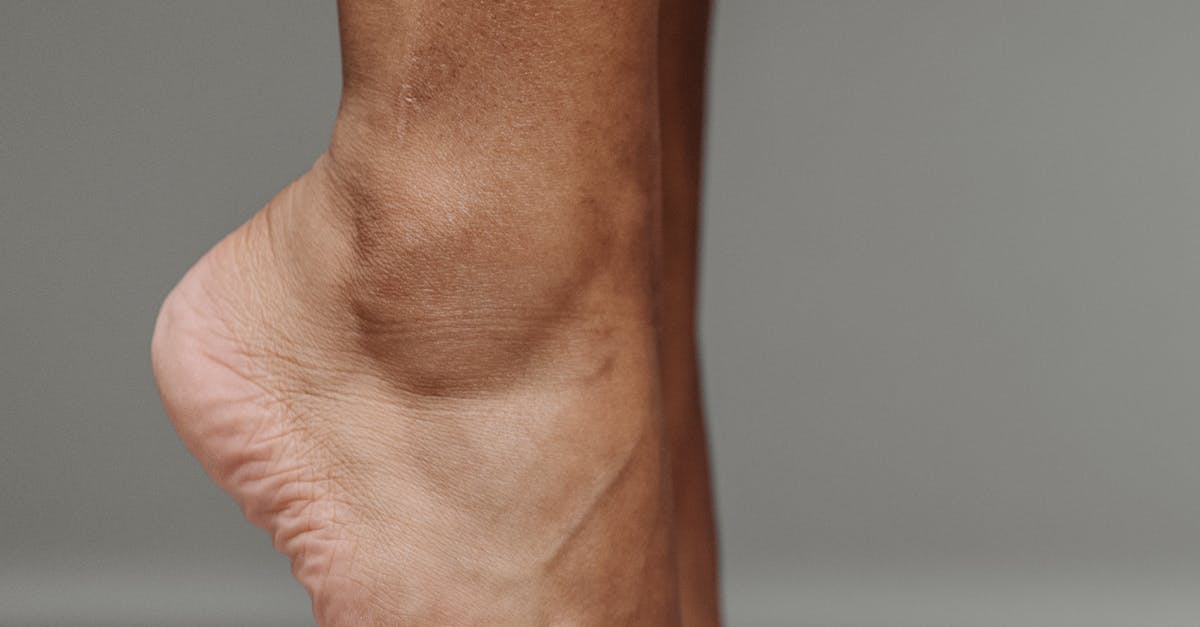
Diabetes mellitus produces some of the most recognizable and clinically significant changes in Achilles tendon morphology, primarily through the process of advanced glycation end product (AGE) formation. In diabetic patients, chronically elevated blood glucose levels lead to non-enzymatic glycation of collagen fibers within the tendon structure, resulting in cross-linking that fundamentally alters the mechanical properties and appearance of the tissue. This biochemical transformation manifests as progressive tendon thickening, with diabetic patients showing Achilles tendons that are typically 20-30% thicker than those of non-diabetic individuals. The affected tendons develop a characteristic rope-like appearance with loss of the normal subtle undulations visible on ultrasound imaging. Additionally, the tendon's echogenicity changes, appearing more heterogeneous and hyperechoic due to the accumulated glycation products and associated inflammatory responses. Clinically, patients may notice decreased ankle flexibility, morning stiffness that persists longer than typical age-related changes, and a gradual loss of the springy quality that normally characterizes healthy tendon function. The glycation process also compromises the tendon's ability to repair micro-injuries, leading to a higher susceptibility to rupture and slower healing times when injuries do occur. These changes often precede the development of more obvious diabetic complications, making Achilles tendon assessment a valuable tool for monitoring glycemic control and predicting future diabetic complications.