10 Facial Skin Texture Patterns Linked to Hormonal and Autoimmune Conditions
3. Thyroid-Related Skin Texture Manifestations
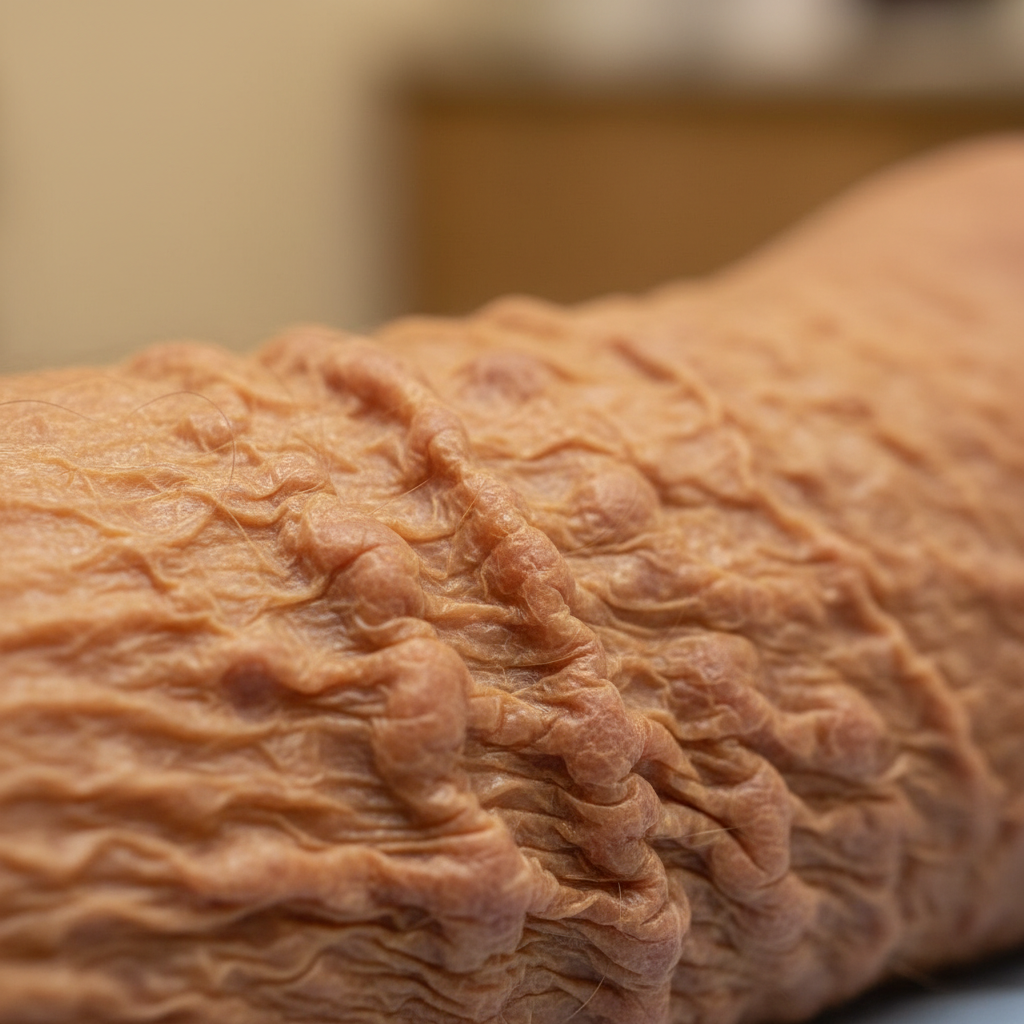
Thyroid dysfunction produces some of the most dramatic and recognizable changes in facial skin texture, with both hyperthyroidism and hypothyroidism creating distinct patterns that reflect the hormone's crucial role in cellular metabolism and skin barrier function. Hypothyroidism typically manifests as dry, coarse, and thickened facial skin with a characteristic waxy or doughy texture, particularly noticeable around the eyelids, cheeks, and jawline, where myxedematous changes can create a puffy, swollen appearance that obscures normal facial contours. The underlying pathophysiology involves decreased cellular turnover, reduced sebaceous gland activity, and accumulation of glycosaminoglycans in the dermis, leading to increased skin thickness and altered water-binding capacity. Conversely, hyperthyroidism produces fine, smooth, warm, and moist skin with increased vascularity that creates a characteristic flushed appearance and enhanced skin elasticity. Advanced imaging studies have revealed that thyroid-related skin texture changes involve modifications at multiple levels of skin architecture, including altered epidermal thickness, changes in dermal collagen organization, and modified vascular patterns that can be detected through techniques such as high-frequency ultrasound and optical coherence tomography. The temporal relationship between thyroid hormone levels and skin texture changes makes facial skin assessment a valuable tool for monitoring thyroid function and treatment response. These thyroid-induced textural modifications often precede other clinical symptoms by months, making dermatological examination an important component of endocrine screening protocols.