12 Inflammatory Conditions That Show Up on the Skin First
8. Thyroid Disorders - Hormonal Inflammation's Dermatological Display
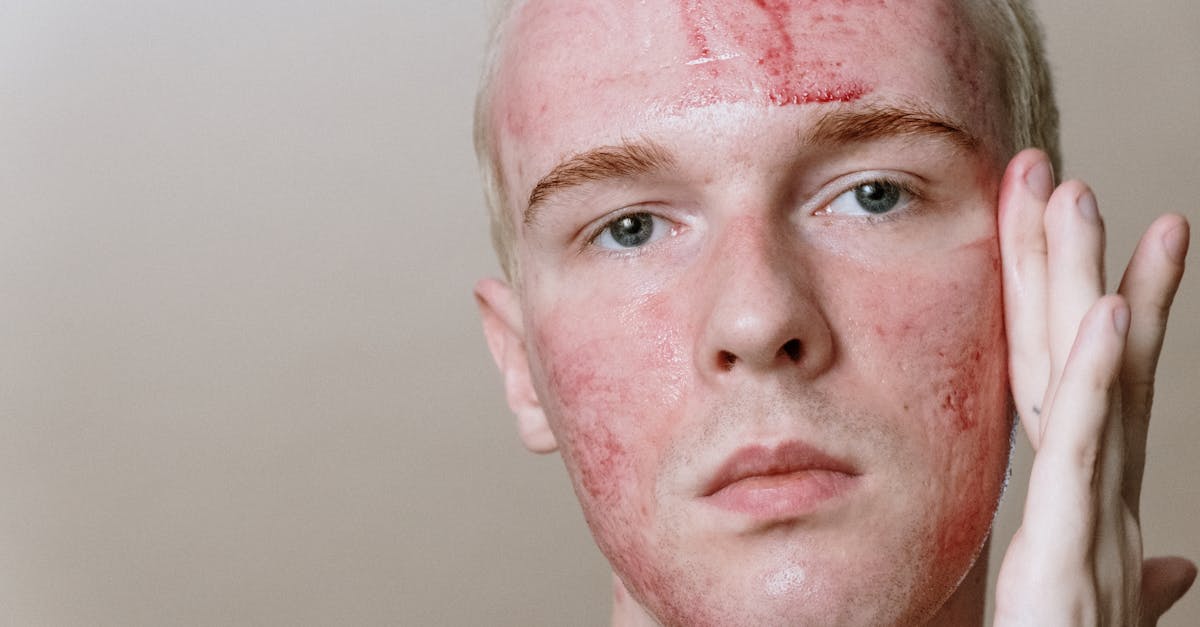
Thyroid dysfunction, whether hyperthyroid or hypothyroid, creates systemic inflammatory states that frequently manifest through distinctive cutaneous changes, often serving as early indicators of underlying endocrine pathology. In hyperthyroidism, particularly Graves' disease, the skin may develop pretibial myxedema (despite the name, this occurs in hyperthyroidism), characterized by thickened, waxy, orange-peel textured skin over the shins, resulting from glycosaminoglycan deposition triggered by thyroid-stimulating immunoglobulins. The inflammatory process in Graves' disease involves molecular mimicry, where antibodies directed against the thyroid-stimulating hormone receptor cross-react with similar receptors in skin and orbital tissues, creating localized inflammatory responses. Hyperthyroid patients also commonly develop warm, moist, smooth skin with increased vascularity and may show onycholysis (nail separation) and hair thinning. Conversely, hypothyroidism creates a different inflammatory milieu characterized by decreased metabolism and altered protein synthesis, leading to dry, coarse, cool skin with a yellowish tint from carotene accumulation, along with brittle hair and nails. The inflammatory component in hypothyroidism often relates to autoimmune thyroiditis (Hashimoto's disease), where chronic inflammation gradually destroys thyroid tissue. Both conditions can cause diffuse hair loss, changes in wound healing, and alterations in skin texture and appearance that may precede obvious systemic symptoms by months. Recognition of these dermatological changes is particularly important because thyroid disorders can significantly impact cardiovascular health, metabolism, and overall quality of life, making early detection and treatment crucial for optimal patient outcomes.