8 Breathing Pattern Irregularities and Their Medical Significance
Breathing, one of the most fundamental physiological processes sustaining human life, serves as a remarkable diagnostic window into our overall health status. While most people take approximately 12-20 breaths per minute without conscious thought, the subtle variations in respiratory patterns can reveal profound insights about underlying medical conditions, neurological function, and metabolic states. Healthcare professionals have long recognized that abnormal breathing patterns, collectively known as dyspnea or respiratory irregularities, often serve as early warning signs of serious medical conditions ranging from heart failure and pneumonia to neurological disorders and metabolic imbalances. These breathing irregularities manifest in various forms, each carrying distinct clinical significance and requiring specific diagnostic approaches. Understanding the eight primary categories of breathing pattern abnormalities—including their physiological mechanisms, associated conditions, and therapeutic implications—is crucial for both medical professionals and patients seeking to recognize potentially serious health concerns. This comprehensive exploration will examine each breathing irregularity through the lens of evidence-based medicine, providing essential knowledge for early detection and appropriate medical intervention.
1. Tachypnea - When Breathing Accelerates Beyond Normal Limits

Tachypnea, characterized by an abnormally rapid respiratory rate exceeding 20 breaths per minute in adults, represents one of the most commonly encountered breathing irregularities in clinical practice. This condition occurs when the body's metabolic demands increase or when respiratory efficiency becomes compromised, forcing the respiratory system to compensate through increased frequency. The underlying mechanisms triggering tachypnea include hypoxemia (low blood oxygen), hypercapnia (elevated carbon dioxide), metabolic acidosis, fever, pain, anxiety, and various pulmonary or cardiac conditions. Medical research has consistently demonstrated that tachypnea often serves as an early indicator of respiratory distress, sepsis, pneumonia, pulmonary embolism, or congestive heart failure. In pediatric patients, tachypnea thresholds differ significantly, with rates exceeding 60 breaths per minute in newborns and 40 breaths per minute in children aged 1-5 years considered abnormal. The clinical significance of tachypnea extends beyond mere symptom recognition, as studies have shown that persistent tachypnea in hospitalized patients correlates with increased mortality risk and longer hospital stays. Healthcare providers must carefully evaluate accompanying symptoms, oxygen saturation levels, and patient history to determine the underlying cause and implement appropriate therapeutic interventions, which may range from supplemental oxygen therapy to treatment of underlying infections or cardiac conditions.
2. Bradypnea - The Concerning Slowdown of Respiratory Function

Bradypnea, defined as an abnormally slow respiratory rate below 12 breaths per minute in adults, presents a potentially serious medical concern that demands immediate attention and thorough evaluation. This respiratory pattern irregularity typically indicates central nervous system depression, respiratory muscle fatigue, or severe metabolic disturbances that compromise the brain's respiratory control centers. Common causes of bradypnea include opioid overdose, severe hypothermia, increased intracranial pressure, brainstem lesions, severe hypothyroidism, and end-stage respiratory failure. Research has established that bradypnea often represents a more ominous clinical sign compared to tachypnea, as it may indicate impending respiratory arrest or profound physiological decompensation. The condition is particularly concerning in post-operative patients receiving narcotic pain medications, where respiratory depression can develop rapidly and progress to life-threatening hypoventilation. Clinical studies have demonstrated that patients with bradypnea frequently require immediate intervention, including naloxone administration for opioid-induced respiratory depression, mechanical ventilation support, or treatment of underlying neurological conditions. Healthcare providers must maintain heightened vigilance when monitoring patients at risk for bradypnea, implementing continuous respiratory monitoring and establishing protocols for rapid response when respiratory rates fall below critical thresholds. The prognosis for patients with bradypnea largely depends on the underlying cause and the timeliness of appropriate medical intervention.
3. Cheyne-Stokes Respiration - The Rhythmic Crescendo of Breathing Irregularity
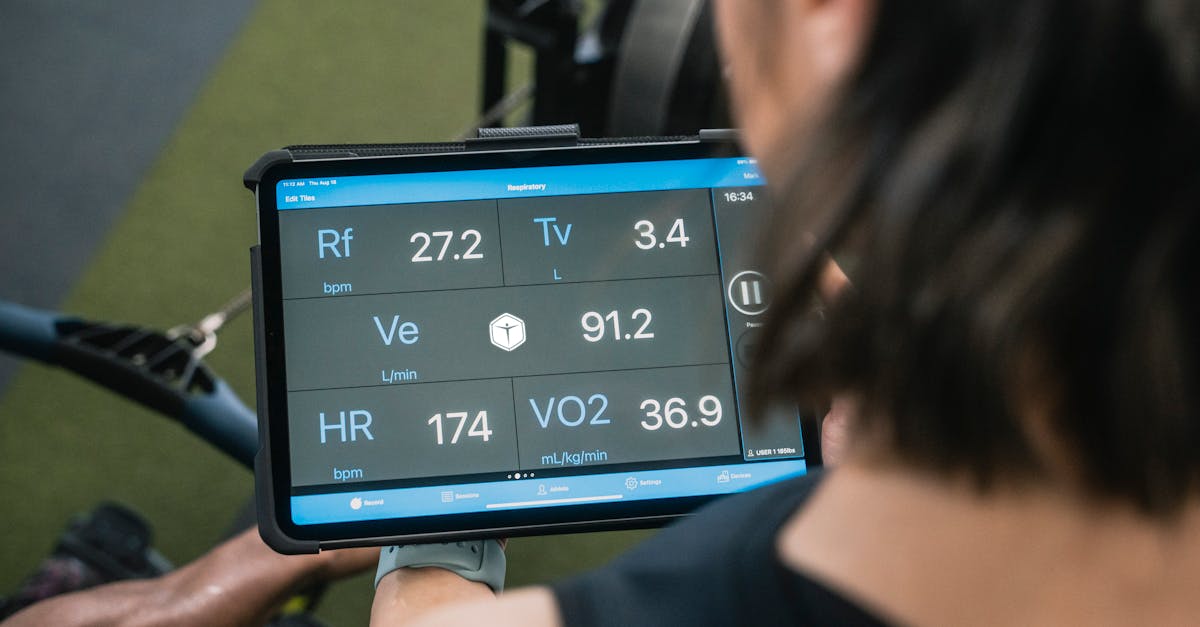

Cheyne-Stokes respiration represents a distinctive and clinically significant breathing pattern characterized by cyclical periods of gradually increasing and decreasing tidal volume, followed by periods of apnea lasting 10-30 seconds. This abnormal respiratory pattern, first described by physicians John Cheyne and William Stokes in the 19th century, results from instability in the respiratory control system, typically involving delayed feedback between peripheral chemoreceptors and the respiratory centers in the medulla. The condition most commonly occurs in patients with congestive heart failure, stroke, traumatic brain injury, or those at high altitudes, where circulatory delays and altered carbon dioxide sensitivity disrupt normal respiratory regulation. Medical research has revealed that Cheyne-Stokes respiration affects approximately 30-50% of patients with heart failure and serves as an independent predictor of increased mortality risk. The physiological mechanism involves a complex interplay between cardiac output, circulation time, and chemoreceptor sensitivity, creating a feedback loop that perpetuates the cyclical breathing pattern. Sleep studies have shown that Cheyne-Stokes respiration frequently occurs during non-REM sleep stages and can significantly impact sleep quality, leading to daytime fatigue and reduced quality of life. Treatment approaches include optimizing heart failure management, continuous positive airway pressure (CPAP) therapy, supplemental oxygen, and in some cases, adaptive servo-ventilation. Early recognition and appropriate management of Cheyne-Stokes respiration can improve patient outcomes and potentially reduce cardiovascular mortality risk.
4. Kussmaul Breathing - The Deep, Labored Response to Metabolic Crisis

Kussmaul breathing, named after German physician Adolph Kussmaul, manifests as deep, rapid, and labored respirations that represent the body's compensatory response to severe metabolic acidosis. This distinctive breathing pattern is characterized by increased tidal volume and respiratory rate, creating a hyperpnea that helps eliminate excess carbon dioxide and partially correct the underlying acid-base imbalance. The condition most commonly occurs in patients with diabetic ketoacidosis (DKA), where the accumulation of ketoacids leads to profound metabolic acidosis requiring immediate respiratory compensation. Research has demonstrated that Kussmaul breathing serves as a critical clinical sign indicating severe metabolic derangement, with arterial pH levels typically below 7.2 and serum bicarbonate concentrations less than 15 mEq/L. The physiological mechanism involves stimulation of peripheral and central chemoreceptors by increased hydrogen ion concentration, triggering the respiratory centers to increase ventilation and lower arterial carbon dioxide levels. Clinical studies have shown that patients exhibiting Kussmaul breathing require urgent medical intervention, including intravenous fluid resuscitation, insulin therapy, electrolyte correction, and careful monitoring for complications such as cerebral edema. The breathing pattern may also occur in other conditions causing severe metabolic acidosis, including uremia, salicylate poisoning, methanol ingestion, and lactic acidosis. Healthcare providers must recognize Kussmaul breathing as a medical emergency requiring immediate diagnostic evaluation and aggressive treatment to prevent potentially fatal complications. The resolution of this breathing pattern typically correlates with correction of the underlying metabolic acidosis and serves as an important marker of therapeutic response.
5. Biot's Breathing - The Unpredictable Pattern of Neurological Compromise
Biot's breathing, also known as ataxic breathing, presents as an irregular respiratory pattern characterized by unpredictable periods of apnea alternating with clusters of breaths of variable depth and frequency. This abnormal breathing pattern, first described by French physician Camille Biot, typically indicates severe damage to the respiratory control centers in the medulla oblongata or pons, often resulting from increased intracranial pressure, brainstem lesions, or severe central nervous system infections. Unlike the predictable cyclical nature of Cheyne-Stokes respiration, Biot's breathing exhibits complete irregularity in both timing and depth, making it a particularly concerning clinical finding that often portends poor neurological prognosis. Medical literature has consistently associated this breathing pattern with conditions such as meningitis, encephalitis, severe head trauma, brainstem strokes, and terminal stages of increased intracranial pressure. The underlying pathophysiology involves disruption of the normal neural networks responsible for respiratory rhythm generation, particularly affecting the pre-Bötzinger complex and other medullary respiratory centers. Research has shown that patients exhibiting Biot's breathing frequently require immediate neurological evaluation, including brain imaging and intracranial pressure monitoring, as this pattern often indicates impending respiratory failure or brain herniation. The clinical significance extends beyond respiratory concerns, as Biot's breathing typically represents advanced neurological compromise requiring intensive care management and potential neurosurgical intervention. Treatment focuses primarily on addressing the underlying neurological condition, providing respiratory support through mechanical ventilation when necessary, and managing intracranial pressure through various medical and surgical approaches. The prognosis for patients with Biot's breathing remains guarded, with outcomes largely dependent on the underlying cause and the rapidity of appropriate medical intervention.
6. Apneustic Breathing - The Prolonged Inspiratory Hold Pattern

Apneustic breathing represents a rare but clinically significant respiratory abnormality characterized by prolonged inspiratory pauses, creating a distinctive pattern where patients appear to "hold" their breath at the peak of inspiration before eventually exhaling. This unusual breathing pattern results from damage to the pneumotaxic center in the upper pons, which normally regulates the transition from inspiration to expiration and helps maintain smooth respiratory rhythm. The condition typically occurs following severe brainstem injury, pontine strokes, or lesions affecting the parabrachial nuclei, which serve as critical components of the respiratory control network. Medical research has identified apneustic breathing as a relatively uncommon but important neurological sign that often indicates significant brainstem pathology requiring immediate medical attention. The physiological mechanism involves disruption of the normal inhibitory signals that terminate inspiration, leading to abnormally prolonged inspiratory efforts that can compromise ventilation efficiency and gas exchange. Clinical studies have shown that patients with apneustic breathing frequently present with other neurological deficits, including altered consciousness, cranial nerve abnormalities, and motor dysfunction, reflecting the extensive nature of brainstem damage. The condition poses significant challenges for respiratory management, as the irregular pattern can lead to inadequate ventilation, respiratory fatigue, and potential respiratory failure. Treatment approaches focus on providing mechanical ventilatory support when necessary, addressing underlying neurological conditions, and implementing comprehensive neurological monitoring to assess for progression or improvement. The prognosis for patients with apneustic breathing varies considerably depending on the underlying cause, extent of brainstem damage, and timeliness of appropriate medical intervention, with some patients showing improvement as neurological function recovers while others may require long-term respiratory support.
7. Central Sleep Apnea - The Neurological Disruption of Sleep Breathing

Central sleep apnea represents a complex breathing disorder characterized by repeated episodes of breathing cessation during sleep, resulting from temporary failure of the central nervous system to send appropriate signals to the respiratory muscles. Unlike obstructive sleep apnea, which involves physical airway blockage, central sleep apnea stems from neurological dysfunction affecting the brainstem's respiratory control centers, leading to periods where respiratory effort completely ceases. This condition affects approximately 0.9% of adults over 40 years old but occurs much more frequently in patients with heart failure, stroke, or other neurological conditions, where prevalence can reach 30-50%. The pathophysiology involves instability in the respiratory control system, often related to altered carbon dioxide sensitivity, delayed circulatory feedback, or direct damage to respiratory control centers. Research has identified several distinct subtypes of central sleep apnea, including primary central sleep apnea, treatment-emergent central sleep apnea (occurring with CPAP therapy), and central sleep apnea associated with medical conditions such as congestive heart failure or opioid use. Clinical studies have demonstrated that central sleep apnea significantly impacts sleep quality, daytime functioning, and cardiovascular health, with untreated cases showing increased risk of arrhythmias, sudden cardiac death, and progression of heart failure. Diagnostic evaluation typically requires overnight polysomnography to document breathing patterns, oxygen saturation changes, and sleep architecture disruption. Treatment options include adaptive servo-ventilation, bilevel positive airway pressure therapy, supplemental oxygen, optimization of underlying medical conditions, and in some cases, medication adjustments or implantable devices that stimulate respiratory muscles. The management approach must be individualized based on the underlying cause, severity of symptoms, and patient-specific factors to achieve optimal therapeutic outcomes.
8. Paradoxical Breathing - The Inverted Pattern of Respiratory Mechanics

Paradoxical breathing, also known as reverse breathing or seesaw breathing, manifests as an abnormal respiratory pattern where the chest and abdomen move in opposite directions during breathing, contrary to the normal coordinated movement where both expand during inspiration and contract during expiration. This concerning breathing irregularity typically indicates respiratory muscle weakness, diaphragmatic paralysis, or severe respiratory distress, creating inefficient ventilation that can rapidly progress to respiratory failure. The condition most commonly occurs in patients with neuromuscular disorders such as amyotrophic lateral sclerosis (ALS), muscular dystrophy, or Guillain-Barré syndrome, where progressive weakness of respiratory muscles disrupts normal breathing mechanics. Medical research has established that paradoxical breathing often serves as an early indicator of diaphragmatic dysfunction, with studies showing that patients exhibiting this pattern frequently have significant reductions in vital capacity and inspiratory muscle strength. The physiological mechanism involves weakness or paralysis of the diaphragm, forcing accessory respiratory muscles to compensate, which creates the characteristic inward movement of the abdomen during inspiration as the weakened diaphragm is pulled upward by negative thoracic pressure. Clinical evaluation of paradoxical breathing requires comprehensive assessment including pulmonary function tests, diaphragmatic ultrasound, and arterial blood gas analysis to determine the severity of respiratory compromise. The condition can also occur acutely in cases of bilateral diaphragmatic paralysis following cardiac surgery, cervical spine injury, or phrenic nerve damage, requiring immediate recognition and potential mechanical ventilation support. Treatment strategies focus on addressing underlying neuromuscular conditions, providing non-invasive ventilatory support such as bilevel positive airway pressure, and in severe cases, implementing mechanical ventilation to prevent respiratory failure. Early recognition and appropriate management of paradoxical breathing can significantly improve patient outcomes and quality of life, particularly in progressive neuromuscular conditions where respiratory support may extend survival and maintain functional independence.
9. Clinical Assessment and Therapeutic Implications of Breathing Irregularities
The comprehensive evaluation and management of breathing pattern irregularities require a systematic approach that integrates clinical observation, diagnostic testing, and evidence-based therapeutic interventions tailored to each patient's specific condition and underlying pathophysiology. Healthcare providers must develop proficiency in recognizing these distinct respiratory patterns, understanding their clinical significance, and implementing appropriate diagnostic and treatment strategies to optimize patient outcomes. The assessment process begins with careful observation of respiratory rate, rhythm, depth, and effort, followed by evaluation of associated symptoms such as cyanosis, use of accessory muscles, and changes in mental status that may indicate respiratory compromise. Advanced diagnostic tools including arterial blood gas analysis, pulmonary function testing, chest imaging, and sleep studies provide crucial information about gas exchange efficiency, respiratory muscle function, and underlying pathological processes. Research has consistently demonstrated that early recognition and appropriate management of breathing irregularities can significantly impact patient prognosis, with timely interventions often preventing progression to respiratory failure and reducing mortality risk. Treatment approaches must address both the immediate respiratory concerns and underlying conditions, incorporating strategies such as supplemental oxygen therapy, non-invasive ventilation, mechanical ventilation when necessary, and specific therapies targeting root causes such as heart failure management, neurological interventions, or metabolic corrections. The integration of multidisciplinary care teams including pulmonologists, neurologists, cardiologists, and respiratory therapists ensures comprehensive management that addresses all aspects of complex breathing disorders. Ongoing monitoring and adjustment of therapeutic interventions based on patient response and disease progression remain essential components of successful management, with regular reassessment of respiratory status and modification of treatment plans as clinical conditions evolve. The ultimate goal of managing breathing pattern irregularities extends beyond mere symptom control to include improvement in quality of life, functional capacity, and long-term survival, emphasizing the critical importance of early recognition, accurate diagnosis, and appropriate therapeutic intervention in these potentially life-threatening conditions.