12 Tingling Patterns in the Face and Scalp and Their Neurological Significance
The human face and scalp represent one of the most densely innervated regions of the body, containing an intricate network of sensory nerves that provide crucial information about our environment and internal physiological state. When tingling sensations, medically termed paresthesias, occur in these areas, they often signal underlying neurological processes that demand careful attention and understanding. These abnormal sensations can range from benign temporary phenomena to indicators of serious neurological conditions, making their proper interpretation essential for both healthcare providers and patients. The trigeminal nerve system, along with cervical spinal nerves and autonomic pathways, creates a complex sensory map that, when disrupted, produces distinct patterns of tingling that can be diagnostically significant. Understanding these patterns requires knowledge of neuroanatomy, pathophysiology, and the various conditions that can affect facial and scalp sensation. This comprehensive exploration will examine twelve specific tingling patterns, their neurological underpinnings, and their clinical significance, providing readers with essential insights into when these sensations warrant medical attention and what they might reveal about underlying health conditions.
1. Trigeminal Neuralgia - The Lightning Strike Pattern

Trigeminal neuralgia presents as one of the most distinctive and excruciating tingling patterns affecting the face, characterized by sudden, electric shock-like sensations that follow the distribution of the trigeminal nerve branches. This condition typically manifests as brief but intense episodes of tingling and pain that can be triggered by light touch, chewing, speaking, or even a gentle breeze across the face. The neurological significance lies in the dysfunction of the trigeminal nerve (cranial nerve V), often caused by vascular compression at the nerve root entry zone in the brainstem. Research has shown that demyelination of trigeminal nerve fibers leads to abnormal electrical activity and cross-excitation between pain and touch fibers, explaining why normally innocuous stimuli can trigger severe symptoms. The pattern typically follows one or more divisions of the trigeminal nerve: the ophthalmic division affecting the forehead and upper eyelid, the maxillary division involving the cheek and upper lip, or the mandibular division affecting the lower jaw and lip. Neuroimaging studies using high-resolution MRI have revealed that vascular compression, particularly by the superior cerebellar artery, occurs in approximately 80-90% of classical trigeminal neuralgia cases. The tingling often precedes or accompanies the characteristic stabbing pain, serving as an important diagnostic clue that distinguishes this condition from other facial pain syndromes.
2. Migraine Aura - The Spreading Wave Phenomenon

Migraine aura represents a fascinating neurological phenomenon that often begins with tingling sensations in the face and scalp, following a characteristic spreading pattern that reflects the underlying cortical spreading depression mechanism. This neurological event typically starts as a subtle tingling or numbness in one area of the face, often around the lips or cheek, and then progressively spreads in a predictable pattern over 15-30 minutes. The neurological significance of this pattern lies in its origin from the visual cortex, where a wave of neuronal depolarization followed by suppression spreads across the brain at a rate of 2-3 millimeters per minute. Research using functional neuroimaging has demonstrated that this cortical spreading depression activates trigeminovascular pathways, leading to the characteristic sensory symptoms that many migraine sufferers experience. The tingling often follows a "marching" pattern, moving from the face to the hand and arm, reflecting the somatotopic organization of the sensory cortex. Studies have shown that approximately 25-30% of migraine patients experience sensory aura symptoms, with facial tingling being reported in about 60% of these cases. The pattern's predictability and duration make it a valuable diagnostic tool, as it typically lasts longer than other causes of facial tingling and is often followed by the characteristic throbbing headache. Understanding this pattern is crucial because it represents one of the few neurological conditions where patients can actually feel the progression of a specific brain wave phenomenon.
3. Bell's Palsy Prodrome - The Unilateral Warning Signal
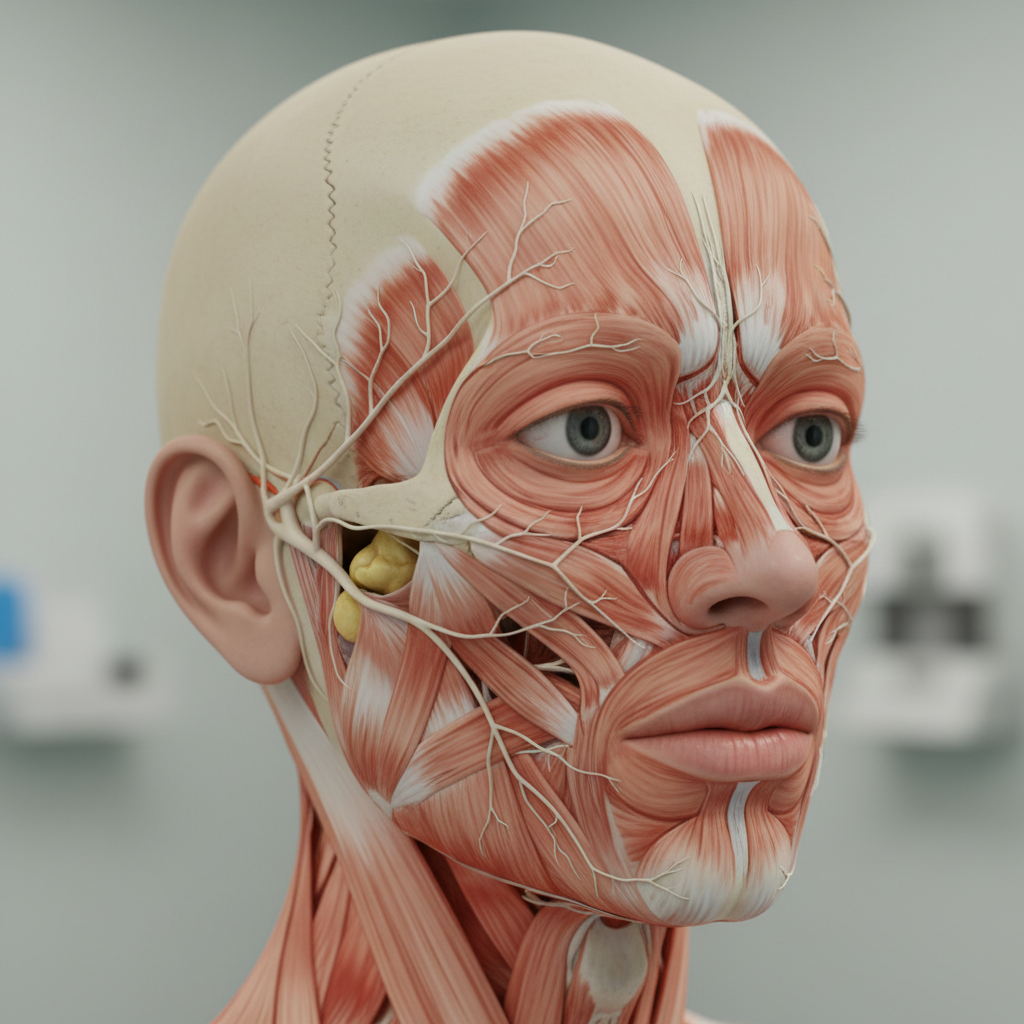
Bell's palsy, an acute peripheral facial nerve paralysis, often announces its onset through distinctive tingling patterns that serve as important early warning signs of impending facial weakness. The prodromal tingling typically occurs 24-48 hours before the onset of facial paralysis and follows the distribution of the facial nerve (cranial nerve VII), affecting the entire half of the face on the affected side. This pattern is neurologically significant because it reflects the inflammatory process affecting the facial nerve within the narrow confines of the facial canal (Fallopian canal) in the temporal bone. Research has demonstrated that viral infections, particularly herpes simplex virus reactivation, trigger an inflammatory cascade that leads to nerve swelling and compression within this bony canal. The tingling sensation results from the initial compression and ischemia of nerve fibers before complete conduction block occurs. Studies using electrophysiological testing have shown that these early sensory symptoms correlate with the degree of nerve inflammation and can predict the severity of subsequent facial weakness. The pattern is distinctly unilateral and often accompanied by subtle changes in taste sensation, as the facial nerve carries taste fibers from the anterior two-thirds of the tongue. Patients frequently describe the tingling as a "crawling" or "pins and needles" sensation that gradually intensifies before the dramatic onset of facial drooping. Recognition of this prodromal pattern is clinically crucial because early intervention with corticosteroids during this phase can significantly improve outcomes and reduce the risk of permanent facial weakness.
4. Temporal Arteritis - The Scalp Tenderness Pattern

Temporal arteritis, also known as giant cell arteritis, produces a distinctive pattern of scalp tingling and tenderness that carries profound neurological significance due to its potential for causing irreversible vision loss and stroke. This inflammatory condition affects medium and large arteries, particularly the temporal arteries, creating a characteristic pattern of tingling, burning, and exquisite tenderness over the temporal region of the scalp. The neurological importance stems from the systemic nature of this vasculitis, which can affect the ophthalmic arteries and posterior ciliary arteries, leading to anterior ischemic optic neuropathy and permanent blindness if left untreated. Research has shown that the tingling and tenderness result from inflammation of the arterial walls, which contain rich networks of sensory nerve fibers that become hyperexcitable during the inflammatory process. The pattern typically involves the temporal region bilaterally, though it may be more pronounced on one side, and patients often report that combing their hair or lying on a pillow becomes extremely uncomfortable. Histopathological studies have revealed that the inflammatory infiltrate consists primarily of T-lymphocytes and multinucleated giant cells, which release inflammatory mediators that sensitize surrounding nerve endings. The tingling is often accompanied by jaw claudication, where chewing becomes painful due to involvement of the maxillary artery branches. Temporal artery biopsy remains the gold standard for diagnosis, showing segmental inflammation that explains the patchy distribution of symptoms. Early recognition of this tingling pattern is critical because prompt treatment with high-dose corticosteroids can prevent devastating complications, making this one of the few neurological emergencies related to facial tingling.
5. Multiple Sclerosis Facial Symptoms - The Demyelinating Pattern
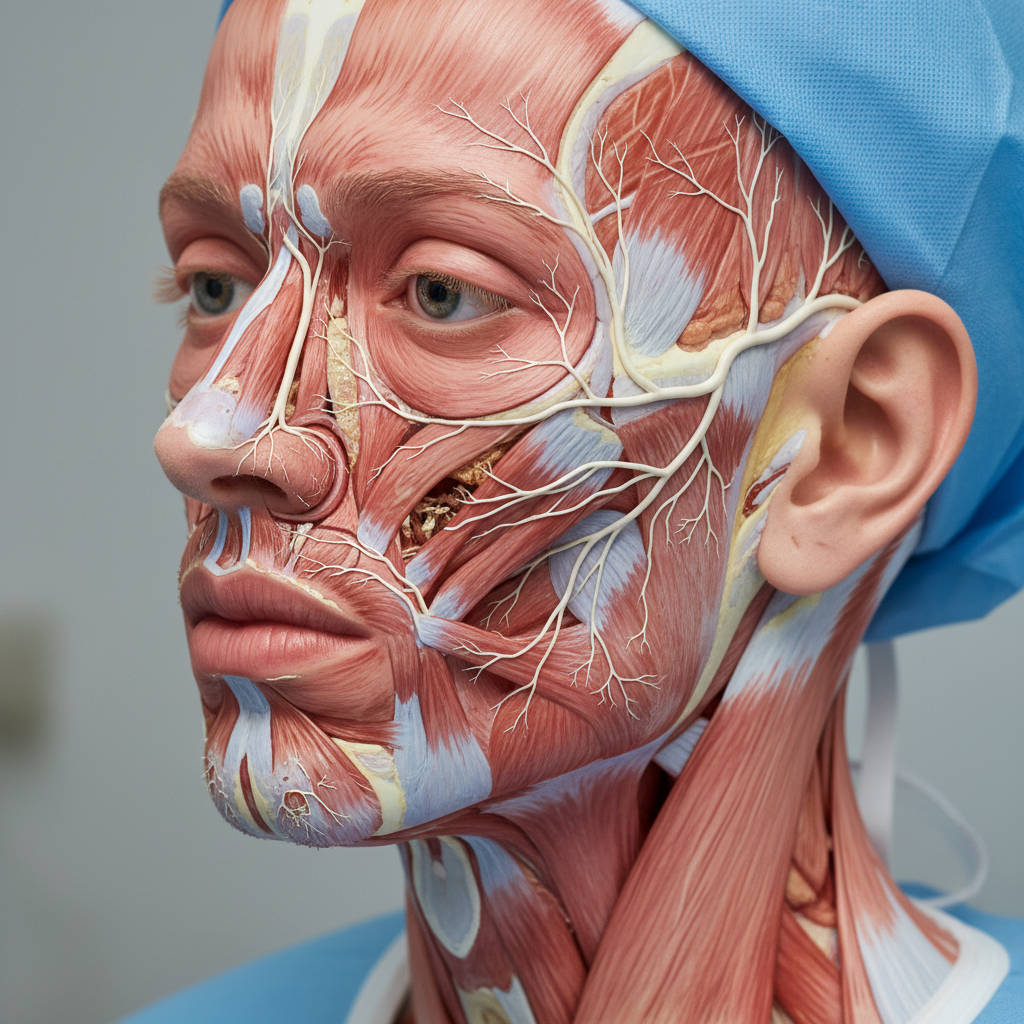
Multiple sclerosis (MS) frequently manifests with facial and scalp tingling patterns that reflect the characteristic demyelinating process affecting central nervous system white matter tracts. The tingling in MS typically presents as episodes of numbness, pins and needles sensations, or burning feelings that can affect various regions of the face and scalp in patterns that don't always follow peripheral nerve distributions. This occurs because MS lesions can affect the trigeminal sensory pathways at multiple levels, from the brainstem trigeminal nuclei to the thalamic relay stations and sensory cortex. Neuroimaging studies using high-resolution MRI have demonstrated that facial sensory symptoms in MS often correlate with lesions in the pons, particularly affecting the principal sensory nucleus of the trigeminal nerve or the trigeminal tract. The pattern is neurologically significant because it often represents one of the earliest symptoms of MS, with studies showing that sensory symptoms occur as the presenting feature in approximately 20-25% of patients with relapsing-remitting MS. Research using evoked potential studies has revealed that the tingling reflects slowed or blocked nerve conduction due to demyelination, with some fibers showing complete conduction failure while others demonstrate delayed transmission. The symptoms in MS are characteristically episodic, lasting days to weeks, and may be triggered by heat (Uhthoff's phenomenon) or stress. Unlike peripheral nerve disorders, the tingling in MS may affect both sides of the face simultaneously or in unusual distributions that cross anatomical boundaries. Advanced neurophysiological studies have shown that remyelination can occur, explaining why many patients experience complete or partial recovery of sensation between relapses.
6. Anxiety-Induced Hyperventilation - The Bilateral Symmetrical Pattern

Anxiety-induced hyperventilation creates a distinctive bilateral and symmetrical pattern of facial and scalp tingling that has important neurological implications related to altered brain chemistry and cerebral blood flow. During episodes of acute anxiety or panic, rapid breathing leads to excessive elimination of carbon dioxide, resulting in respiratory alkalosis and subsequent changes in calcium ion availability and neuronal excitability. The tingling typically begins around the mouth and lips, then spreads symmetrically to involve the cheeks, forehead, and scalp in a characteristic perioral and facial distribution. Neurophysiologically, the reduced carbon dioxide levels cause cerebral vasoconstriction, decreasing blood flow to the brain by up to 40%, while simultaneously increasing the pH of blood and tissues. This alkalotic state reduces the availability of ionized calcium, which is essential for normal nerve function, leading to increased neuronal excitability and the characteristic tingling sensations. Research using transcranial Doppler studies has demonstrated significant reductions in cerebral blood flow velocity during hyperventilation episodes, correlating with the intensity of sensory symptoms. The pattern is neurologically significant because it represents a functional rather than structural disorder, yet the symptoms can be so severe that patients often fear they are experiencing a stroke or other serious neurological condition. Studies have shown that the tingling follows a predictable temporal pattern, typically beginning within 1-2 minutes of hyperventilation onset and resolving within 10-15 minutes of normal breathing restoration. Electrophysiological studies have revealed that the hyperventilation-induced changes primarily affect small-diameter sensory fibers, explaining why touch and vibration sensation remain intact while patients experience intense tingling and numbness.
7. Cervical Radiculopathy - The Referred Scalp Pattern

Cervical radiculopathy, particularly involving the upper cervical nerve roots (C2-C3), can produce distinctive tingling patterns in the posterior scalp and neck region that demonstrate the complex interconnections between spinal and cranial sensory systems. The greater occipital nerve, which arises from the C2 nerve root, provides sensation to a large portion of the posterior scalp, and when compressed or irritated, creates a characteristic pattern of tingling, burning, or shooting sensations that radiate from the suboccipital region to the vertex of the head. This neurological phenomenon is significant because it illustrates how cervical spine pathology can masquerade as primary headache disorders or scalp conditions. Research using high-resolution MRI and electromyography has shown that cervical disc herniation, facet joint arthropathy, or muscle spasm can compress nerve roots, leading to both local symptoms and referred sensations in the scalp distribution. The tingling pattern typically follows the anatomical distribution of the greater occipital nerve, starting at the occiput and radiating forward over the posterior and lateral aspects of the scalp, sometimes reaching as far as the frontal region. Neuroanatomical studies have revealed that the C2 nerve root has unique connections with the trigeminal system through the trigeminocervical complex in the upper cervical spinal cord, explaining why cervical pathology can produce symptoms that seem to originate from cranial nerve disorders. The pattern is often unilateral and may be triggered by neck movements, coughing, or Valsalva maneuvers, distinguishing it from primary headache disorders. Advanced imaging studies using diffusion tensor imaging have shown that chronic cervical radiculopathy can lead to microstructural changes in the affected nerve roots, potentially explaining why some patients develop persistent tingling even after the underlying mechanical compression is resolved.
8. Glossopharyngeal Neuralgia - The Deep Ear and Throat Connection
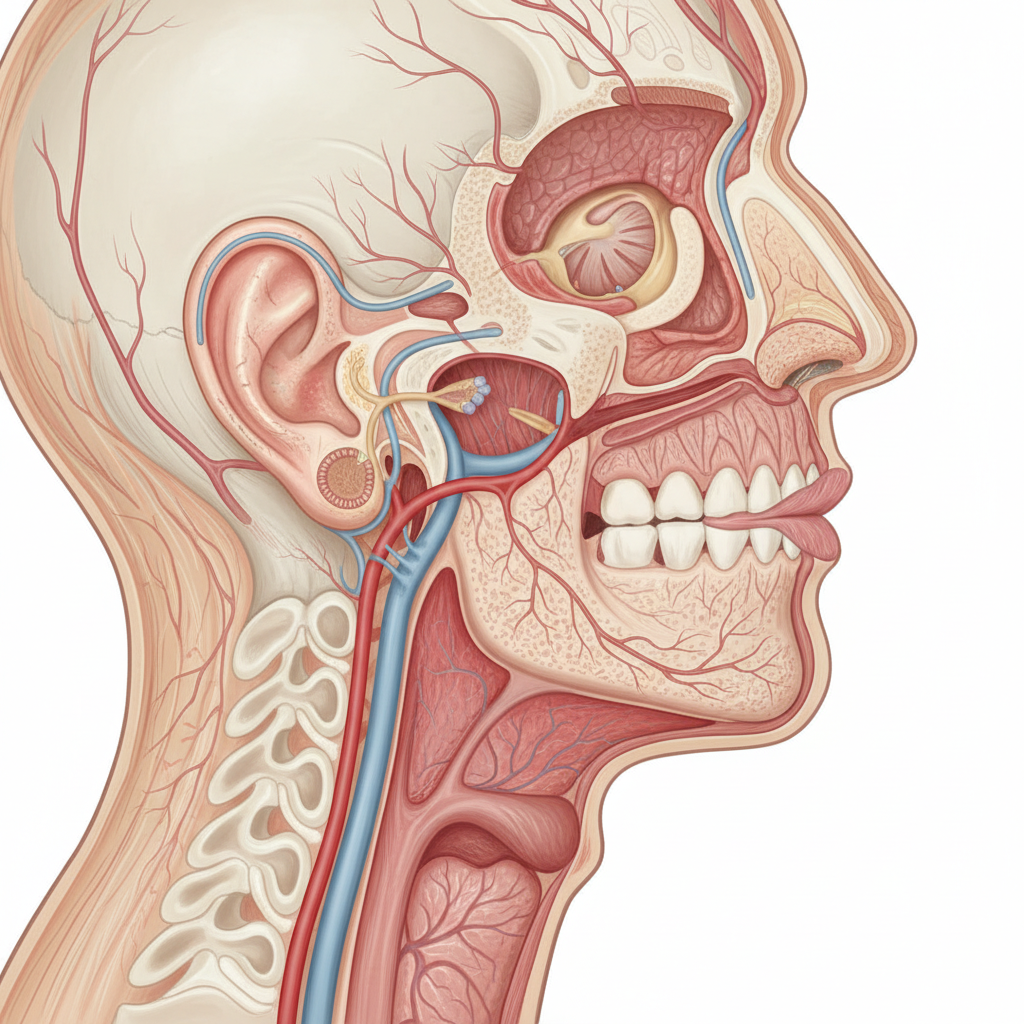
Glossopharyngeal neuralgia presents with a unique tingling pattern that affects the deep ear, throat, and posterior tongue regions, representing dysfunction of the ninth cranial nerve and demonstrating the complex sensory innervation of the head and neck. This rare but distinctive condition produces sharp, electric shock-like tingling sensations that radiate from the throat to the ear, often triggered by swallowing, talking, or touching specific areas of the throat or tongue. The neurological significance lies in the anatomical course of the glossopharyngeal nerve, which provides sensory innervation to the posterior third of the tongue, the tonsillar region, the middle ear, and parts of the external auditory canal. Research has shown that, similar to trigeminal neuralgia, glossopharyngeal neuralgia often results from vascular compression of the nerve root entry zone, typically by the posterior inferior cerebellar artery or anterior inferior cerebellar artery. The tingling pattern is neurologically important because it can be associated with potentially life-threatening complications, including cardiac arrhythmias and syncope, due to the nerve's connections with the cardiac plexus through its parasympathetic fibers. Electrophysiological studies have demonstrated that the abnormal nerve activity can spread to adjacent neural structures, including the vagus nerve, explaining the cardiovascular symptoms that occur in some patients. The pattern typically involves deep, aching tingling sensations in the ear that may radiate to the angle of the jaw, the throat, or the base of the tongue. Advanced neuroimaging using high-resolution FIESTA (Fast Imaging Employing Steady-state Acquisition) sequences has improved the ability to visualize neurovascular compression in these patients, leading to better surgical outcomes when medical management fails.
9. Diabetic Neuropathy - The Stocking-Glove Facial Extension
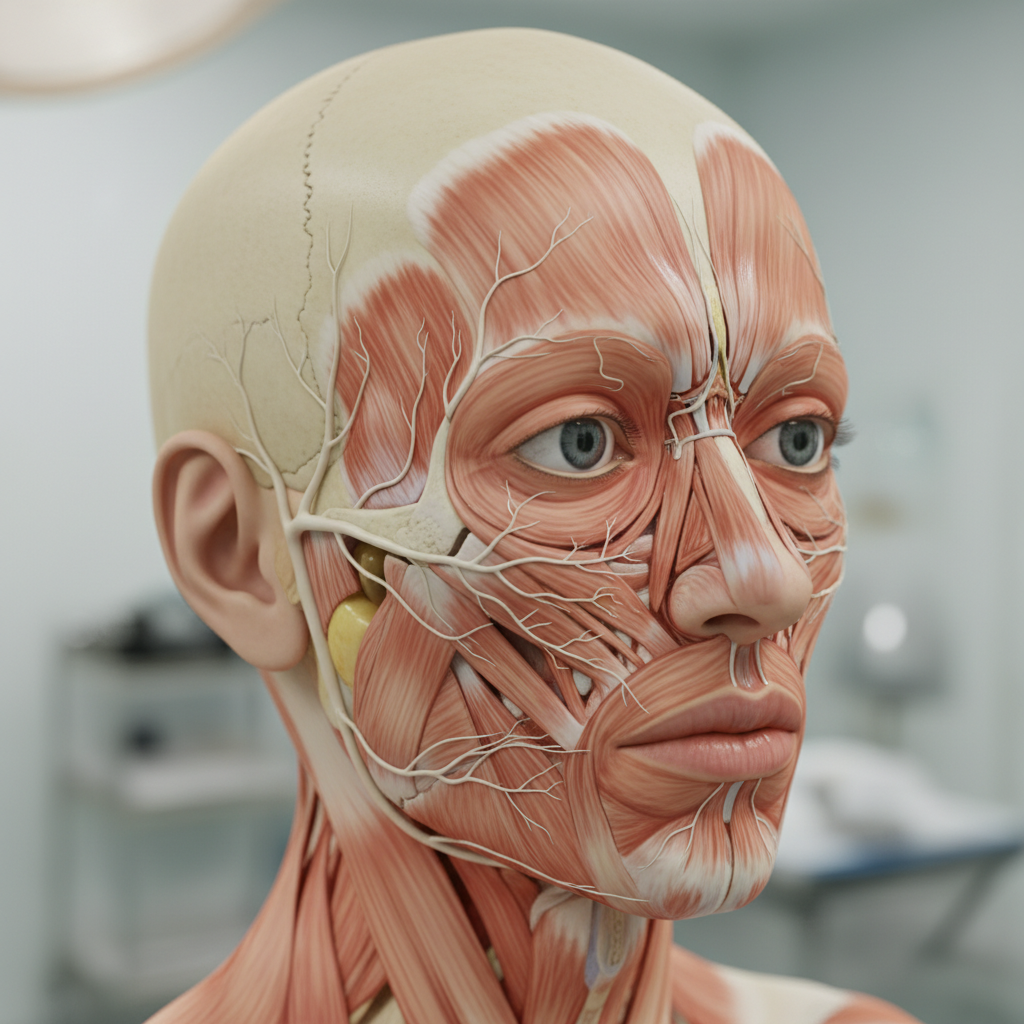
Diabetic neuropathy, while classically associated with distal extremity symptoms, can occasionally extend to involve facial and scalp regions, creating a distinctive pattern that reflects the metabolic and vascular effects of chronic hyperglycemia on peripheral nerves. The facial involvement in diabetic neuropathy typically manifests as bilateral tingling, burning, or numbness that may affect the perioral region, cheeks, and sometimes the scalp, representing an extension of the characteristic distal sensory loss pattern. This neurological phenomenon is significant because it usually indicates advanced diabetic neuropathy with involvement of both large and small nerve fibers, suggesting poor glycemic control and increased risk for other diabetic complications. Research has demonstrated that chronic hyperglycemia leads to multiple pathological processes affecting nerve function, including advanced glycation end-product formation, oxidative stress, and microvascular dysfunction that can affect cranial nerves. The tingling pattern in diabetic facial neuropathy often follows a bilateral and symmetrical distribution, distinguishing it from focal cranial neuropathies that diabetes can also cause, such as diabetic third nerve palsy or Bell's palsy. Nerve conduction studies and quantitative sensory testing have shown that diabetic neuropathy preferentially affects small unmyelinated C-fibers and thinly myelinated A-delta fibers, which carry pain and temperature sensation, explaining why patients often experience burning tingling rather than simple numbness. The facial symptoms typically develop gradually over months to years, in contrast to the acute onset seen with other causes of facial tingling. Skin biopsy studies measuring intraepidermal nerve fiber density have provided objective evidence of small fiber neuropathy in diabetic patients with facial symptoms, correlating with the severity of tingling and burning sensations.
10. Herpes Zoster (Shingles) - The Dermatomal Tingling Pattern
Herpes zoster affecting the trigeminal nerve creates one of the most characteristic and clinically significant tingling patterns in the face and scalp, following precise dermatomal distributions that reflect the anatomical organization of sensory nerve pathways. The condition results from reactivation of varicella-zoster virus that has remained dormant in trigeminal ganglia since initial chickenpox infection, creating a distinctive prodromal phase characterized by tingling, burning, and hypersensitivity in the affected dermatome. The neurological significance is profound because trigeminal zoster, particularly when involving the ophthalmic division (zoster ophthalmicus), can lead to serious complications including corneal ulceration, glaucoma, and vision loss. Research has shown that the reactivated virus travels along sensory nerve fibers from the ganglion to the skin, causing inflammation and damage to nerve pathways that results in the characteristic tingling sensations that precede the visible rash by several days. The pattern strictly follows anatomical boundaries of trigeminal nerve divisions: V1 (ophthalmic) affecting the forehead, upper eyelid, and scalp; V2 (maxillary) involving the cheek, nose, and upper lip; or V3 (mandibular) affecting the lower jaw and lip area. Immunohistochemical studies have demonstrated that the virus causes direct cytopathic effects on neurons and satellite cells within the ganglion, leading to inflammation and altered nerve function. The tingling is often described as deep, aching, or burning, and may be accompanied by allodynia, where normally non-painful stimuli become painful. Neuroimaging studies using MRI have shown enhancement of the affected trigeminal nerve and ganglion during acute episodes, reflecting the inflammatory process. The risk of developing postherpetic neuralgia, a chronic pain condition that can persist for months or years after the acute infection