12 Heart Rate Variation Symptoms and What Each Pattern Suggests to Doctors
Heart rate variability (HRV) represents one of the most sophisticated and revealing diagnostic tools in modern cardiology, offering physicians unprecedented insights into the autonomic nervous system's function and overall cardiovascular health. Unlike the simple measurement of beats per minute, HRV analyzes the subtle variations in time intervals between consecutive heartbeats, revealing patterns that can indicate everything from stress levels and fitness status to serious underlying cardiac conditions. This intricate dance of rhythm variations serves as a window into the body's ability to adapt to internal and external stressors, with each pattern telling a unique story about physiological function. When doctors observe specific HRV patterns, they're essentially reading the heart's own language—a complex communication system that reflects the delicate balance between the sympathetic and parasympathetic nervous systems. The twelve distinct symptoms and patterns we'll explore represent critical diagnostic markers that can help identify conditions ranging from anxiety disorders and sleep apnea to more serious concerns like heart failure, arrhythmias, and autonomic dysfunction. Understanding these patterns empowers both medical professionals and patients to recognize early warning signs, optimize treatment strategies, and make informed decisions about cardiovascular health management.
1. Consistently Low Heart Rate Variability - The Rigid Heart
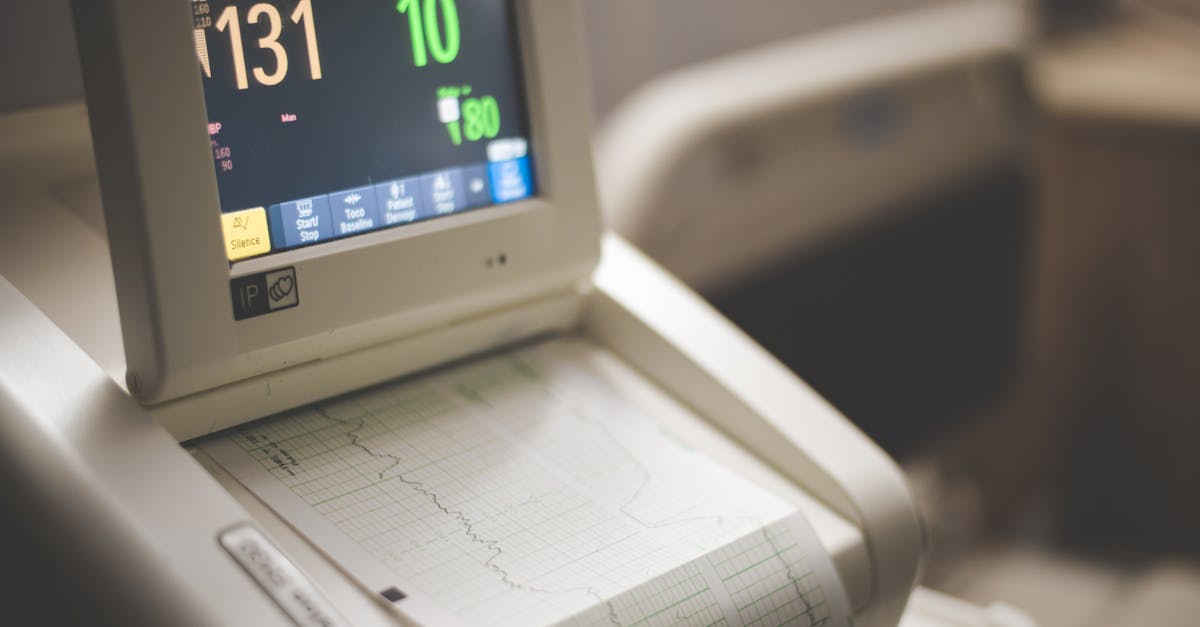
When heart rate variability consistently remains below normal ranges, typically showing minimal variation between heartbeats, it signals a concerning rigidity in the cardiovascular system that immediately captures a physician's attention. This pattern, characterized by a monotonous, almost mechanical rhythm, often indicates compromised autonomic nervous system function, where the heart loses its natural ability to respond dynamically to changing physiological demands. Doctors recognize this symptom as particularly significant because healthy hearts should demonstrate considerable variability, with the parasympathetic nervous system naturally creating fluctuations during breathing cycles and other activities. Low HRV can manifest in patients experiencing chronic stress, diabetes, heart disease, or aging-related cardiovascular decline, and it's frequently associated with increased mortality risk and reduced quality of life. The clinical implications are profound, as this pattern suggests the heart's regulatory mechanisms have become inflexible, potentially indicating inflammation, oxidative stress, or structural cardiac changes. Physicians often observe this pattern in patients with conditions such as diabetic neuropathy, where prolonged high blood sugar levels damage the nerves controlling heart rate, or in individuals with chronic fatigue syndrome, where the autonomic nervous system becomes dysregulated. Treatment approaches typically focus on lifestyle modifications, stress reduction techniques, regular exercise, and addressing underlying conditions that may be contributing to the reduced variability.
2. Extremely High Heart Rate Variability - The Chaotic Heart
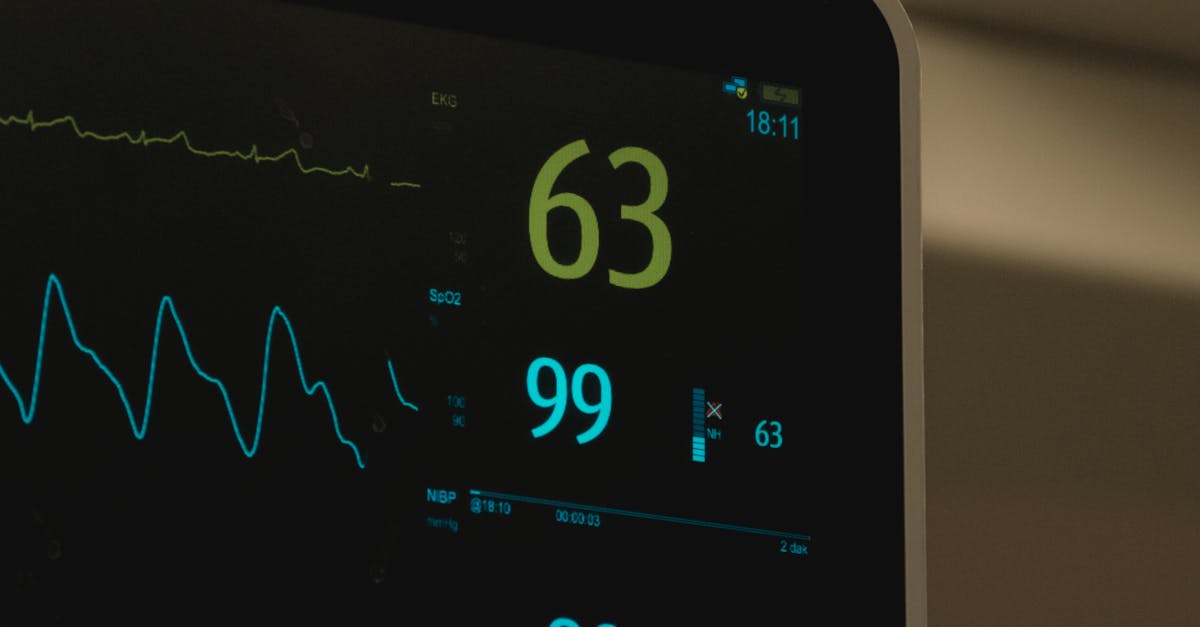
Paradoxically, excessively high heart rate variability can be equally concerning to physicians, as it may indicate an unstable or chaotic cardiovascular system struggling to maintain proper rhythm control. This pattern presents as dramatic, unpredictable swings in the intervals between heartbeats, creating an erratic rhythm that suggests the heart's regulatory mechanisms are overactive or poorly coordinated. While moderate HRV is healthy and desirable, extreme variability often points to underlying pathological conditions such as atrial fibrillation, where the heart's upper chambers beat irregularly and rapidly, or other arrhythmias that disrupt normal electrical conduction. Doctors are particularly alert to this pattern because it can indicate serious conditions requiring immediate intervention, including heart failure, where the compromised heart struggles to maintain consistent pumping efficiency, or acute stress responses that overwhelm the cardiovascular system. The excessive variability may also manifest in patients with hyperthyroidism, where elevated thyroid hormones create metabolic chaos that affects heart rhythm regulation, or in individuals experiencing severe anxiety or panic disorders that trigger extreme autonomic nervous system responses. Clinical evaluation of this pattern typically involves comprehensive cardiac monitoring, electrolyte assessment, thyroid function testing, and evaluation for structural heart disease. Treatment strategies focus on identifying and addressing the underlying cause while potentially using medications to stabilize heart rhythm and prevent dangerous complications such as stroke or sudden cardiac arrest.
3. Sudden Drops in Heart Rate Variability - The Warning Signal
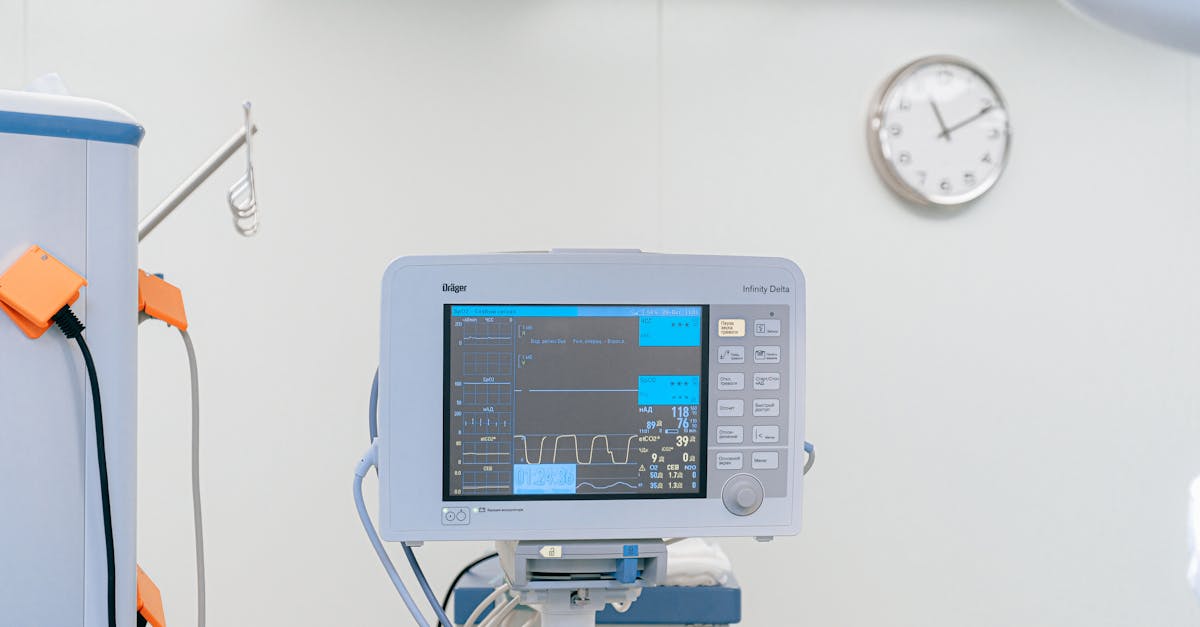
Acute decreases in heart rate variability represent one of the most clinically significant patterns physicians encounter, as they often herald the onset of serious medical conditions or indicate acute physiological stress that requires immediate attention. This pattern typically manifests as a previously normal or elevated HRV suddenly plummeting to abnormally low levels over hours, days, or weeks, creating a dramatic shift that suggests the body's adaptive mechanisms are becoming overwhelmed or compromised. Doctors recognize this symptom as particularly ominous because it frequently precedes major cardiac events, infections, or other medical emergencies, making it a valuable early warning system for proactive intervention. The sudden drop often indicates that the parasympathetic nervous system, which normally provides the calming, restorative influence on heart rhythm, is becoming suppressed while the sympathetic nervous system dominates, creating a state of chronic physiological alarm. This pattern is commonly observed in patients developing heart failure, where the heart's pumping efficiency deteriorates rapidly, or in individuals experiencing severe infections where systemic inflammation disrupts normal autonomic function. Additionally, physicians may notice this pattern in patients with sleep disorders, particularly sleep apnea, where repeated episodes of oxygen deprivation stress the cardiovascular system, or in individuals experiencing severe psychological trauma or chronic stress that overwhelms the body's coping mechanisms. Clinical response typically involves comprehensive evaluation to identify the underlying cause, intensive monitoring, and aggressive treatment of any identified conditions to prevent progression to more serious complications.
4. Circadian Rhythm Disruptions in Heart Rate Variability - The Confused Clock

Disruptions in the natural circadian patterns of heart rate variability provide physicians with crucial insights into sleep disorders, shift work complications, and various metabolic disturbances that affect the body's internal timing mechanisms. Normally, HRV follows a predictable daily rhythm, with higher variability during nighttime rest periods when parasympathetic activity dominates, and lower variability during daytime activities when sympathetic nervous system activation is more prominent. When doctors observe disrupted or absent circadian HRV patterns, they immediately suspect conditions that interfere with normal sleep-wake cycles or underlying disorders that affect the body's master biological clock located in the brain's suprachiasmatic nucleus. This pattern is particularly common in patients with sleep apnea, where repeated breathing interruptions prevent normal sleep architecture and disrupt the natural ebb and flow of autonomic nervous system activity throughout the night. Shift workers frequently display this pattern due to forced misalignment between their work schedules and natural biological rhythms, leading to chronic circadian disruption that affects cardiovascular health and increases disease risk. Physicians also observe disrupted circadian HRV patterns in patients with depression, bipolar disorder, or seasonal affective disorder, where mood disorders interfere with normal sleep patterns and autonomic regulation. Additionally, this pattern may indicate metabolic disorders such as diabetes, where blood sugar fluctuations disrupt normal physiological rhythms, or in elderly patients where age-related changes in the circadian system create less robust daily rhythm patterns. Treatment approaches typically focus on sleep hygiene optimization, light therapy, melatonin supplementation, and addressing underlying sleep disorders or medical conditions contributing to the circadian disruption.
5. Exercise-Related Heart Rate Variability Abnormalities - The Athletic Paradox
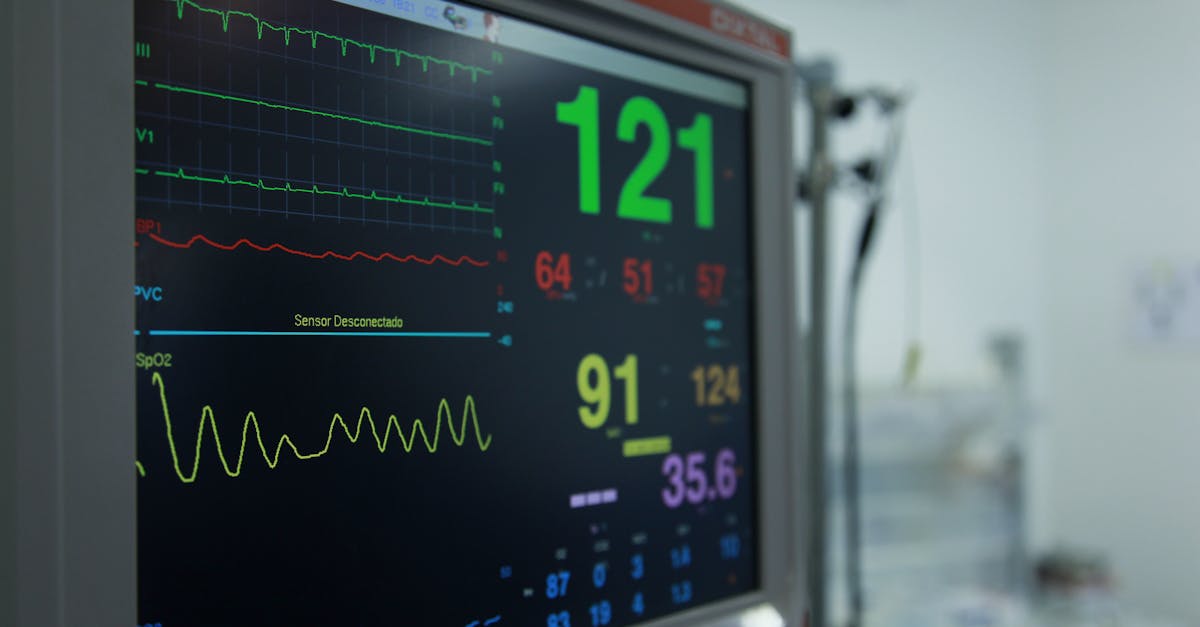
Exercise-induced changes in heart rate variability patterns provide physicians with valuable diagnostic information about cardiovascular fitness, overtraining syndrome, and the heart's ability to adapt to physical stress, revealing insights that extend far beyond simple fitness assessment. In healthy individuals, regular exercise typically enhances HRV by strengthening parasympathetic nervous system function and improving overall autonomic balance, but abnormal exercise-related patterns can indicate serious underlying problems or inappropriate training regimens. Doctors pay close attention to patients who show persistently low HRV following exercise, as this may indicate overtraining syndrome, where excessive physical stress overwhelms the body's recovery mechanisms and leads to chronic fatigue, decreased performance, and increased injury risk. Conversely, some patients may demonstrate paradoxically high HRV during exercise, which can suggest underlying cardiac conditions such as heart block or other conduction abnormalities that prevent normal heart rate acceleration during physical activity. Athletes and highly trained individuals sometimes present with unique HRV patterns that reflect their adapted cardiovascular systems, but physicians must distinguish between beneficial adaptations and pathological changes that could indicate conditions like athlete's heart syndrome or exercise-induced arrhythmias. The pattern of HRV recovery following exercise is particularly informative, as delayed normalization may suggest compromised cardiovascular health, poor fitness levels, or underlying conditions such as heart failure or coronary artery disease that impair the heart's ability to return to baseline function. Clinical evaluation typically involves exercise stress testing, comprehensive cardiac assessment, and careful analysis of training history to determine whether observed patterns represent healthy adaptations or concerning abnormalities requiring intervention.
6. Stress-Induced Heart Rate Variability Changes - The Body's Alarm System

Stress-related alterations in heart rate variability serve as one of the most sensitive and immediate indicators of psychological and physiological stress responses, providing physicians with real-time insights into how patients' cardiovascular systems react to various stressors and cope with challenging situations. When individuals experience acute stress, whether physical, emotional, or psychological, the sympathetic nervous system typically activates rapidly, leading to decreased HRV as the heart rate becomes more rigid and less variable in preparation for "fight or flight" responses. Doctors recognize that chronic stress exposure can lead to persistently reduced HRV, indicating that the autonomic nervous system has become stuck in a state of hypervigilance that increases cardiovascular disease risk and compromises overall health outcomes. This pattern is particularly evident in patients with anxiety disorders, post-traumatic stress disorder, or chronic work-related stress, where repeated activation of stress responses creates lasting changes in autonomic nervous system function and cardiovascular regulation. Physicians also observe stress-related HRV changes in patients experiencing major life events such as divorce, job loss, or bereavement, where emotional stress translates into measurable physiological changes that can persist for weeks or months. The relationship between stress and HRV is bidirectional, as individuals with naturally low HRV may be more susceptible to stress-related health problems and less resilient in the face of challenging circumstances. Clinical assessment often involves stress questionnaires, psychological evaluation, and monitoring HRV responses to controlled stressors to determine appropriate intervention strategies. Treatment approaches typically include stress management techniques, mindfulness meditation, cognitive-behavioral therapy, and lifestyle modifications designed to enhance stress resilience and restore healthy autonomic balance.
7. Age-Related Heart Rate Variability Decline - The Aging Heart's Story
The gradual decline in heart rate variability that occurs with advancing age represents a natural but significant physiological change that provides physicians with important insights into cardiovascular aging and helps distinguish between normal age-related changes and pathological conditions requiring intervention. As individuals age, the autonomic nervous system undergoes various changes, including reduced parasympathetic activity, altered neurotransmitter function, and decreased responsiveness to physiological stimuli, all of which contribute to the characteristic reduction in HRV observed in older adults. Doctors recognize that while some HRV decline is expected with aging, excessive or rapid deterioration may indicate accelerated cardiovascular aging, underlying disease processes, or increased risk for adverse cardiac events that warrant closer monitoring and potential intervention. The age-related HRV pattern typically shows a gradual, progressive decrease beginning in middle age and continuing throughout the later decades of life, but physicians must carefully evaluate whether the observed decline falls within expected ranges or suggests pathological acceleration. This pattern becomes particularly important when evaluating older patients for cardiovascular disease risk, as those with HRV values significantly below age-adjusted norms may have increased susceptibility to arrhythmias, heart failure, or sudden cardiac death. Additionally, age-related HRV changes can interact with other factors such as medications, comorbid conditions, and lifestyle factors to create complex patterns that require careful interpretation and individualized assessment. Physicians often use age-adjusted HRV reference values and consider factors such as physical fitness, medication use, and overall health status when evaluating whether observed patterns represent normal aging or concerning pathological changes. Treatment strategies for age-related HRV decline typically focus on lifestyle interventions such as regular exercise, stress reduction, adequate sleep, and management of cardiovascular risk factors to slow the rate of decline and maintain optimal autonomic function throughout the aging process.
8. Medication-Induced Heart Rate Variability Alterations - The Pharmaceutical Effect
Medication-induced changes in heart rate variability patterns represent a complex and clinically significant phenomenon that requires careful physician monitoring and interpretation, as various pharmaceutical agents can profoundly affect autonomic nervous system function and cardiovascular regulation in both beneficial and potentially harmful ways. Many commonly prescribed medications, including beta-blockers, antiarrhythmics, antidepressants, and blood pressure medications, directly influence the autonomic nervous system and can create characteristic HRV patterns that physicians must recognize and differentiate from underlying pathological conditions. Beta-blockers, for example, typically reduce heart rate and may initially decrease HRV by blocking sympathetic nervous system activity, but long-term use often leads to improved HRV as the cardiovascular system adapts and parasympathetic function becomes more prominent. Conversely, certain medications such as tricyclic antidepressants or anticholinergic drugs can significantly reduce HRV by suppressing parasympathetic activity, potentially increasing cardiovascular risk in susceptible patients. Physicians must carefully consider the timing of HRV changes in relation to medication initiation, dose adjustments, or discontinuation to determine whether observed patterns represent expected pharmacological effects or concerning adverse reactions requiring intervention. Some patients may experience paradoxical or unexpected HRV responses to medications due to individual variations in drug metabolism, underlying genetic factors, or interactions with other medications or medical conditions. The clinical challenge lies in distinguishing between therapeutic medication effects that may temporarily alter HRV patterns and potentially harmful changes that could indicate drug toxicity, inappropriate dosing, or adverse cardiovascular effects requiring immediate attention. Monitoring strategies typically involve baseline HRV assessment before medication initiation, regular follow-up measurements during dose titration periods, and careful correlation of HRV changes with clinical symptoms and other cardiovascular parameters to ensure optimal therapeutic outcomes while minimizing potential risks.
9. Sleep Disorder-Related Heart Rate Variability Patterns - The Nighttime Disruption

Sleep disorders create distinctive heart rate variability patterns that provide physicians with valuable diagnostic clues about sleep quality, respiratory function, and overall cardiovascular health, as the intimate relationship between sleep and autonomic nervous system function makes HRV monitoring an essential tool for evaluating sleep-related medical conditions. During normal sleep, HRV typically increases as parasympathetic nervous system activity dominates, creating higher variability during deep sleep stages and lower variability during REM sleep periods, but various sleep disorders disrupt these natural patterns in characteristic ways that physicians can recognize and interpret. Sleep apnea, one of the most common and serious sleep disorders, creates a distinctive HRV pattern characterized by cyclical changes that correspond to apneic episodes, where breathing stops temporarily and oxygen levels drop, triggering sympathetic nervous system activation and dramatic changes in heart rate variability. Physicians observe that patients with obstructive sleep apnea often show reduced overall HRV with superimposed periodic fluctuations that mirror their breathing disruptions, creating a signature pattern that can aid in diagnosis and severity assessment. Insomnia and other sleep disorders that fragment normal sleep architecture typically result in persistently low HRV throughout the night, as the autonomic nervous system remains in a state of heightened activation rather than transitioning to the restorative parasympathetic dominance that characterizes healthy sleep. Restless leg syndrome, periodic limb movement disorder, and other conditions that cause frequent sleep interruptions create HRV patterns showing multiple brief arousals and autonomic activations that prevent the normal recovery and restoration that should occur during sleep. Clinical evaluation often involves overnight sleep studies combined with continuous HRV monitoring to correlate sleep stages, breathing patterns, and autonomic function, providing comprehensive insights into sleep quality and cardiovascular impact. Treatment approaches typically focus on addressing the underlying sleep disorder through continuous positive airway pressure therapy for sleep apnea, sleep hygiene optimization, or other targeted interventions designed to restore normal sleep architecture and improve autonomic balance.
## Section 11: Inflammatory Conditions and Heart Rate Variability Suppression - The Body's Defense Response
Inflammatory conditions and systemic inflammation create characteristic heart rate variability patterns that serve as important biomarkers for physicians monitoring disease activity, treatment response, and overall health status in patients with various inflammatory disorders ranging from autoimmune diseases to acute infections. When the body's immune system becomes activated in response to infection, tissue damage, or autoimmune processes, inflammatory mediators such as cytokines and chemokines directly affect the autonomic nervous system, typically leading to reduced HRV as sympathetic activity increases and parasympathetic function becomes suppressed. Physicians recognize that this inflammatory suppression of HRV represents an adaptive response designed to mobilize the body's resources for fighting infection or healing injured tissues, but chronic inflammation can lead to persistently low HRV that increases cardiovascular disease risk and compromises overall health outcomes. Acute infections such as pneumonia, sepsis, or viral illnesses often produce dramatic reductions in HRV that correlate with disease severity and can serve as early warning signs of clinical deterioration requiring aggressive intervention. Chronic inflammatory conditions including rheumatoid arthritis, inflammatory bowel disease, and systemic lupus erythematosus typically show persistently reduced HRV that may fluctuate with disease activity and respond to anti-inflammatory treatments. The relationship between inflammation and HRV is bidirectional, as individuals with chronically low HRV may be more susceptible to inflammatory conditions and may experience more severe symptoms or complications when inflammatory diseases develop. Physicians often use HRV monitoring as an objective measure of inflammatory burden and treatment response, particularly in conditions where traditional inflammatory markers may not fully capture the systemic impact of the disease process. Clinical management typically involves comprehensive anti-inflammatory strategies including appropriate medications, lifestyle modifications such as anti-inflammatory diets and regular exercise, stress reduction techniques, and careful monitoring of both inflammatory markers and HRV patterns to optimize treatment outcomes and prevent cardiovascular complications associated with chronic inflammation.
10. Mental Health Disorders and Heart Rate Variability Connections - The Mind-Heart Link
Mental health disorders demonstrate profound and characteristic effects on heart rate variability patterns that provide physicians with objective physiological markers for understanding the complex interplay between psychological well-being and cardiovascular health, revealing how emotional and psychiatric conditions directly impact autonomic nervous system