12 Ear Symptom Types Beyond Hearing Loss and Their Associated Conditions
While hearing loss often dominates discussions about ear health, the complex anatomy of the auditory system can manifest a remarkable array of symptoms that extend far beyond diminished hearing capacity. The ear, comprising the outer, middle, and inner ear structures, serves not only as our gateway to sound but also plays crucial roles in balance, spatial orientation, and even immune function. From the external auditory canal to the intricate labyrinthine structures of the inner ear, each component can develop conditions that produce distinctive symptoms, many of which patients and even healthcare providers may not immediately associate with ear pathology. These symptoms can range from the obvious, such as pain and discharge, to the more subtle manifestations like cognitive changes, facial weakness, or systemic dizziness that significantly impact quality of life. Understanding these diverse presentations is essential for early recognition, proper diagnosis, and effective treatment of underlying conditions that could otherwise progress to more serious complications. This comprehensive exploration will illuminate twelve distinct ear symptom categories beyond hearing loss, examining their underlying mechanisms, associated conditions, and clinical significance in modern otolaryngology practice.
1. Otalgia - The Spectrum of Ear Pain

Otalgia, or ear pain, represents one of the most common and distressing ear symptoms, affecting millions of individuals annually and serving as a primary reason for emergency department visits and urgent care consultations. This symptom can manifest as sharp, stabbing sensations, dull aching, or throbbing pain that may be constant or intermittent, localized to one ear or bilateral, and can radiate to surrounding structures including the jaw, neck, and temporal region. Primary otalgia originates directly from ear pathology, including acute otitis media, otitis externa, temporomandibular joint disorders, or trauma to the ear canal, while secondary otalgia results from referred pain from distant structures sharing common nerve pathways, such as dental infections, pharyngeal inflammation, or cervical spine disorders. The intensity and character of ear pain can provide valuable diagnostic clues: sudden, severe pain often suggests acute infection or barotrauma, while chronic, burning pain might indicate neuropathic conditions or chronic inflammatory processes. Associated symptoms frequently accompany otalgia, including fever, hearing changes, discharge, or systemic malaise, which help clinicians differentiate between various underlying conditions and guide appropriate treatment strategies that may range from topical medications and oral antibiotics to surgical intervention in severe cases.
2. Otorrhea - Understanding Ear Discharge
Otorrhea, the medical term for ear discharge, encompasses any fluid emanating from the ear canal and represents a significant clinical finding that can indicate various underlying pathological processes requiring immediate medical attention. The characteristics of ear discharge provide crucial diagnostic information: clear, watery discharge may suggest cerebrospinal fluid leakage from temporal bone fractures or chronic otitis media with complications, while purulent, yellow-green discharge typically indicates bacterial infection such as acute otitis externa or chronic suppurative otitis media. Bloody discharge can result from trauma, foreign body insertion, or more concerning conditions like malignancy or severe infection with tissue necrosis, while thick, cheesy discharge often characterizes cholesteatoma, a serious condition requiring surgical management. The volume, odor, and consistency of otorrhea also provide diagnostic clues: foul-smelling discharge suggests anaerobic bacterial infection or cholesteatoma, while copious, thin discharge might indicate external auditory canal dermatitis or allergic reactions. Chronic otorrhea can lead to secondary complications including hearing loss, canal stenosis, and spread of infection to surrounding structures, making prompt evaluation and treatment essential. Management approaches vary significantly based on the underlying cause, ranging from topical antibiotic drops and thorough cleaning for simple infections to complex surgical procedures for structural abnormalities or chronic inflammatory conditions.
3. Tinnitus - The Phantom Sounds of the Auditory System
Tinnitus, characterized by the perception of sound in the absence of external acoustic stimuli, affects approximately 15-20% of the global population and represents one of the most challenging and poorly understood ear symptoms in modern medicine. This phantom auditory perception can manifest as ringing, buzzing, hissing, clicking, roaring, or musical sounds that may be constant or intermittent, unilateral or bilateral, and can vary significantly in pitch, volume, and character throughout the day or in response to environmental factors. Subjective tinnitus, experienced only by the patient, accounts for the vast majority of cases and can result from damage to any part of the auditory pathway, from outer ear wax impaction to complex central nervous system processing disorders, while objective tinnitus, audible to external observers, typically indicates vascular abnormalities, muscle spasms, or structural anomalies near the ear. The underlying mechanisms of tinnitus involve complex neuroplastic changes in the auditory system, including altered neural firing patterns, increased spontaneous activity in auditory neurons, and maladaptive central processing that can be triggered by hearing loss, ototoxic medications, noise exposure, or various medical conditions. Associated conditions frequently include anxiety, depression, sleep disturbances, and concentration difficulties, creating a cycle where tinnitus impacts quality of life while stress and emotional distress can exacerbate the perceived intensity of phantom sounds, requiring comprehensive management approaches that address both the auditory symptoms and psychosocial consequences.
4. Vertigo and Dizziness - When the World Spins

Vertigo and dizziness represent complex vestibular symptoms that arise from dysfunction in the inner ear's balance organs, the semicircular canals and otolith organs, which work in concert with visual and proprioceptive systems to maintain spatial orientation and postural stability. True vertigo involves a distinct sensation of rotational movement, either of the patient or their environment, and typically indicates peripheral vestibular pathology such as benign paroxysmal positional vertigo (BPPV), vestibular neuritis, or Ménière's disease, while non-vertiginous dizziness encompasses sensations of unsteadiness, lightheadedness, or disequilibrium that may suggest central nervous system involvement or systemic conditions. The duration, triggers, and associated symptoms of vestibular episodes provide crucial diagnostic information: brief episodes triggered by head position changes suggest BPPV, while prolonged vertigo with hearing loss and tinnitus may indicate Ménière's disease or vestibular schwannoma. Peripheral vestibular disorders often present with nausea, vomiting, and compensatory head movements, while central causes may involve additional neurological symptoms such as diplopia, dysarthria, or ataxia that require immediate medical evaluation. The impact of vestibular symptoms extends beyond the acute episodes, often leading to chronic imbalance, fall risk, activity limitations, and psychological consequences including anxiety and depression, particularly in elderly patients where vestibular dysfunction significantly increases morbidity and mortality risks through fall-related injuries and social isolation.
5. Aural Fullness - The Sensation of Blocked Ears
Aural fullness, described by patients as a sensation of pressure, blockage, or "cotton in the ears," represents a common but often overlooked ear symptom that can significantly impact quality of life and may indicate various underlying conditions ranging from benign to serious pathology. This subjective sensation can result from actual physical obstruction of the ear canal or eustachian tube, such as cerumen impaction, foreign bodies, or eustachian tube dysfunction, or may reflect changes in middle ear pressure, inner ear fluid dynamics, or even central auditory processing alterations. Eustachian tube dysfunction, one of the most frequent causes of aural fullness, occurs when the tube connecting the middle ear to the nasopharynx fails to open properly, leading to negative pressure in the middle ear space and subsequent sensations of fullness, muffled hearing, and sometimes pain or popping sounds. The sensation can be unilateral or bilateral, constant or intermittent, and may fluctuate with activities such as swallowing, yawning, or changes in altitude, providing important diagnostic clues about the underlying mechanism. Associated conditions include allergic rhinitis, upper respiratory infections, gastroesophageal reflux disease, and anatomical abnormalities, while more serious causes such as acoustic neuromas, temporal bone tumors, or autoimmune inner ear disease must be considered in cases with progressive or persistent symptoms. Management strategies vary widely based on the underlying cause, ranging from simple cerumen removal and nasal decongestants to complex surgical procedures for structural abnormalities or pressure equalization tube placement for chronic eustachian tube dysfunction.
6. Hyperacusis - When Normal Sounds Become Unbearable

Hyperacusis, characterized by an abnormal sensitivity to everyday sounds that are perceived as uncomfortably loud or painful, affects approximately 2% of the population and can severely impact social functioning, occupational performance, and overall quality of life. This condition involves dysfunction in the auditory system's natural protective mechanisms and sound processing pathways, leading to an abnormally low threshold for sound tolerance that can make normal environmental sounds such as running water, paper rustling, or conversation feel overwhelming or physically painful. The underlying mechanisms of hyperacusis are complex and not fully understood, but research suggests involvement of both peripheral and central auditory system dysfunction, including altered outer hair cell function, abnormal stapedius reflex responses, and maladaptive central gain mechanisms that amplify incoming auditory signals beyond normal levels. Primary hyperacusis can develop following acoustic trauma, ototoxic medication exposure, or viral infections affecting the auditory system, while secondary hyperacusis often accompanies conditions such as migraine, fibromyalgia, post-traumatic stress disorder, autism spectrum disorders, or Williams syndrome, suggesting shared neurological pathways between auditory processing and other sensory or emotional systems. The condition frequently coexists with tinnitus, creating a particularly challenging clinical scenario where patients experience both phantom sounds and hypersensitivity to real environmental noise, often leading to sound avoidance behaviors, social isolation, and secondary psychological complications including anxiety, depression, and phonophobia that require comprehensive, multidisciplinary treatment approaches combining audiological rehabilitation, cognitive behavioral therapy, and sometimes pharmacological intervention.
7. Facial Nerve Symptoms - When Ears Affect Facial Function
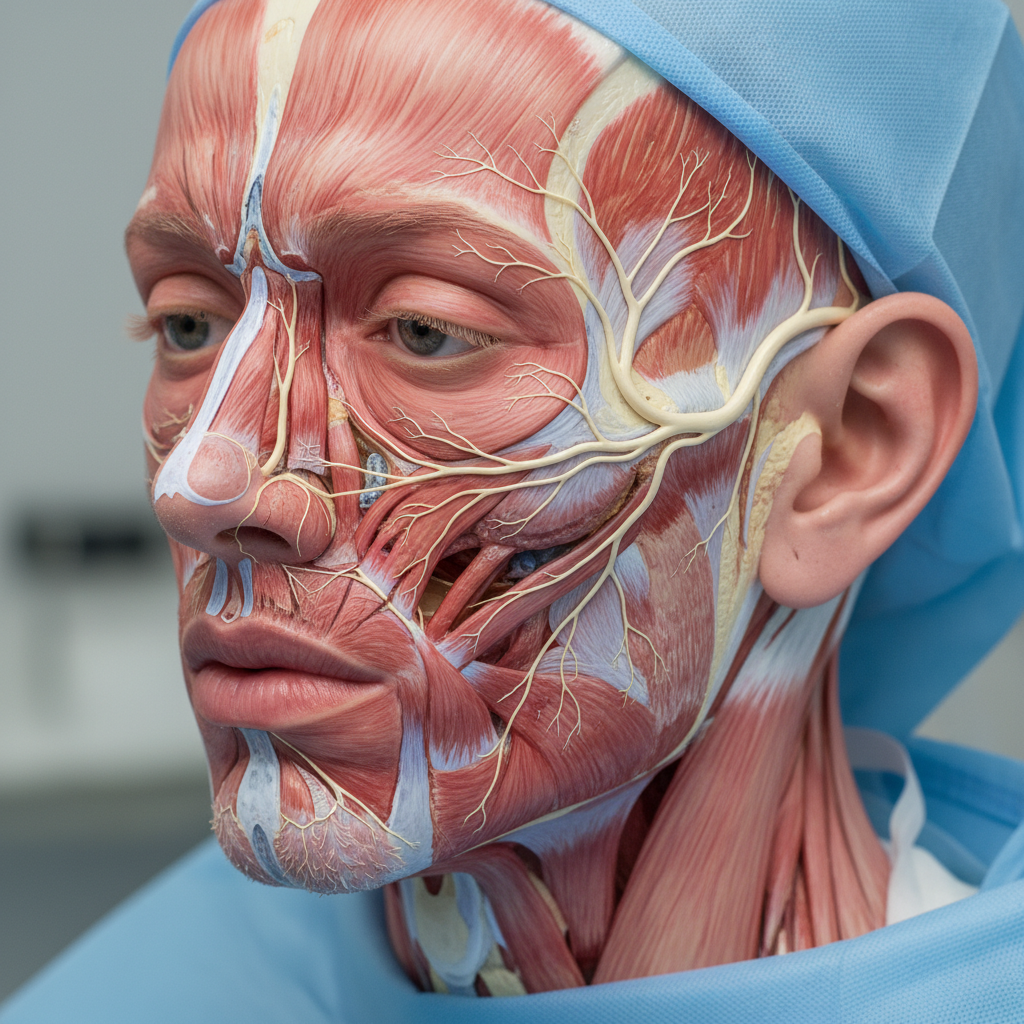
Facial nerve symptoms related to ear pathology represent a serious clinical concern that can indicate significant underlying conditions requiring immediate medical attention, as the facial nerve (cranial nerve VII) travels through the temporal bone in close proximity to middle and inner ear structures, making it vulnerable to various ear-related pathological processes. The facial nerve controls muscles of facial expression, provides taste sensation to the anterior two-thirds of the tongue, and innervates the stapedius muscle in the middle ear, so dysfunction can manifest as facial weakness or paralysis, altered taste perception, hyperacusis due to stapedius muscle paralysis, or decreased tear and saliva production. Acute facial paralysis in the setting of ear symptoms may indicate serious conditions such as acute otitis media with complications, cholesteatoma with erosion into the facial nerve canal, temporal bone fractures, malignant otitis externa, or acoustic neuromas compressing the nerve, all of which require urgent evaluation and treatment to prevent permanent facial nerve damage. The degree and pattern of facial weakness provide important diagnostic information: complete facial paralysis suggests more severe pathology than partial weakness, while the presence of associated symptoms such as hearing loss, vertigo, or ear discharge helps localize the site of pathology and guide appropriate imaging and treatment decisions. Recovery from facial nerve dysfunction varies significantly depending on the underlying cause and degree of nerve damage, with some patients experiencing complete recovery within weeks to months, while others may have permanent deficits requiring reconstructive surgery, physical therapy, or other rehabilitative interventions to restore function and prevent complications such as corneal exposure, oral incompetence, or psychological distress from facial disfigurement.
8. Cognitive and Concentration Issues - The Hidden Neurological Impact

Cognitive and concentration difficulties associated with ear disorders represent an underrecognized but significant aspect of auditory pathology that can profoundly impact academic performance, occupational functioning, and overall quality of life, particularly as the auditory system plays crucial roles in attention, memory processing, and cognitive load management. Research has demonstrated that even mild hearing difficulties can increase cognitive load as the brain works harder to process degraded auditory signals, leaving fewer cognitive resources available for other mental tasks such as memory formation, problem-solving, and executive functioning. Chronic ear conditions such as persistent tinnitus, fluctuating hearing loss, or vestibular dysfunction can lead to attention deficits, memory problems, mental fatigue, and difficulty concentrating in noisy environments, symptoms that may be mistakenly attributed to aging, stress, or other medical conditions rather than recognized as consequences of auditory system dysfunction. The mechanisms underlying these cognitive effects involve complex interactions between auditory processing centers and higher-order brain regions responsible for attention and memory, with neuroimaging studies revealing altered brain activity patterns and structural changes in individuals with chronic ear disorders. Children with chronic ear infections or hearing difficulties are particularly vulnerable to cognitive and academic impacts, including delayed language development, reading difficulties, and behavioral problems that can have long-lasting educational and social consequences if not properly identified and addressed. Treatment approaches must address both the underlying ear pathology and its cognitive consequences, often requiring multidisciplinary care involving audiologists, otolaryngologists, neuropsychologists, and educational specialists to optimize both auditory function and cognitive performance through hearing aids, assistive listening devices, cognitive rehabilitation, and environmental modifications.
9. Sleep Disturbances - When Ear Problems Disrupt Rest

Sleep disturbances represent a frequently overlooked consequence of various ear disorders that can create a vicious cycle of worsening symptoms and decreased quality of life, as adequate sleep is essential for immune function, tissue repair, and overall health maintenance. Tinnitus represents one of the most common ear-related causes of sleep disruption, with phantom sounds becoming more noticeable in quiet nighttime environments and interfering with sleep initiation and maintenance, leading to chronic sleep deprivation that can exacerbate tinnitus perception and associated psychological distress. Ear pain from conditions such as acute otitis media or temporomandibular joint disorders can cause significant sleep fragmentation, while positional vertigo may force patients to sleep in uncomfortable positions or wake frequently due to dizziness when changing positions during normal sleep movements. Sleep-disordered breathing conditions such as obstructive sleep apnea can also impact ear health through eustachian tube dysfunction caused by negative pressure changes during apneic episodes, creating a bidirectional relationship between sleep disorders and ear pathology. The consequences of ear-related sleep disturbances extend far beyond simple fatigue, including impaired immune function that may predispose to recurrent ear infections, decreased pain tolerance that can worsen ear-related discomfort, cognitive dysfunction that compounds attention problems associated with hearing difficulties, and mood disturbances that can develop into clinical depression or anxiety disorders. Management strategies must address both the underlying ear pathology and sleep hygiene, often involving sound masking devices for tinnitus, pain management protocols for inflammatory conditions, positional therapy for vestibular disorders, and sometimes sleep studies to identify concurrent sleep disorders that may be contributing to the overall symptom complex.
10. Balance and Coordination Problems - Beyond Simple Dizziness

Balance and coordination problems related to ear disorders encompass a broad spectrum of symptoms that extend beyond simple dizziness to include postural instability, gait abnormalities, and fine motor coordination difficulties that can significantly impact daily activities and increase fall risk, particularly in elderly populations. The vestibular system in the inner ear works in complex coordination with visual and proprioceptive inputs to maintain balance and spatial orientation, so dysfunction in any component of this system can lead to compensatory mechanisms that may be inadequate for maintaining normal balance function. Chronic vestibular disorders such as bilateral vestibular hypofunction, vestibular migraine, or post-vestibular neuritis syndrome can result in persistent imbalance, oscillopsia (visual blurring with head movement), and difficulty walking in dark or uneven terrain, symptoms that may persist long after acute vestibular episodes have resolved. The impact of balance problems extends beyond physical symptoms to include psychological consequences such as anxiety about falling, activity avoidance, and social isolation that can lead to physical deconditioning and further worsening of balance function. Age-related changes in vestibular function, combined with other sensory deficits and medical conditions common in elderly patients, create particular challenges in this population where balance disorders significantly increase morbidity and mortality through fall-related injuries, hip fractures, and subsequent complications. Comprehensive evaluation of balance problems requires specialized testing including videonystagmography, rotary chair testing, and computerized dynamic posturography to identify specific vestibular deficits and guide targeted rehabilitation programs that may include vestibular rehabilitation therapy, balance training exercises, assistive devices, and environmental modifications to reduce fall risk and improve functional independence.
11. Pressure Sensations and Barotrauma - When Pressure Changes Cause Problems

Pressure sensations and barotrauma-related symptoms represent important ear manifestations that can occur when the normal pressure equalization mechanisms of the middle ear fail to accommodate rapid environmental pressure changes, commonly experienced during air travel, scuba diving, or even elevator rides in tall buildings. The eustachian tube normally opens during swallowing or yawning to equalize pressure between the middle ear and atmospheric pressure, but dysfunction of this mechanism can lead to pressure buildup, pain, hearing loss, and in severe cases, tympanic membrane rupture or middle ear hemorrhage. Barotrauma can manifest as acute, severe ear pain during pressure changes, persistent aural fullness after pressure exposure, temporary or permanent hearing loss, tinnitus, and sometimes vertigo if the pressure changes affect inner ear structures or cause perilymphatic fistulas. Individuals with pre-existing eustachian tube dysfunction, upper respiratory infections, allergies, or anatomical abnormalities are at increased risk for pressure-related ear problems, while certain occupations such as airline personnel, divers, or military personnel face repeated exposure to pressure changes that can lead to chronic ear problems. The severity of barotrauma can range from mild discomfort and temporary hearing changes to severe complications including permanent hearing loss, chronic ear infections, or cholesteatoma formation in cases of repeated trauma with poor healing. Prevention strategies include avoiding pressure changes during upper respiratory infections, using decongestants or nasal sprays before air travel, performing pressure equalization maneuvers during ascent and