10 Types of Dizziness and How Doctors Distinguish Between Them
Dizziness represents one of the most challenging diagnostic puzzles in modern medicine, affecting millions of people worldwide and serving as a primary reason for medical consultations across all age groups. This seemingly simple symptom encompasses a vast spectrum of underlying conditions, ranging from benign inner ear disturbances to serious neurological disorders, cardiovascular issues, and metabolic imbalances. The complexity lies not only in the diverse array of potential causes but also in the subjective nature of how patients experience and describe their symptoms. What one person describes as "dizziness" might be vertigo to another, lightheadedness to a third, or disequilibrium to yet another. Medical professionals have developed sophisticated diagnostic frameworks and assessment tools to navigate this intricate landscape, utilizing detailed patient histories, physical examinations, specialized tests, and advanced imaging techniques. Understanding the distinct types of dizziness and the methodical approaches doctors use to differentiate between them is crucial for both healthcare providers and patients, as accurate diagnosis directly impacts treatment effectiveness and patient outcomes. This comprehensive exploration will illuminate the ten primary categories of dizziness, the diagnostic strategies employed by medical professionals, and the critical importance of precise classification in achieving optimal therapeutic results.
1. Peripheral Vertigo - When the Inner Ear Sends Mixed Signals
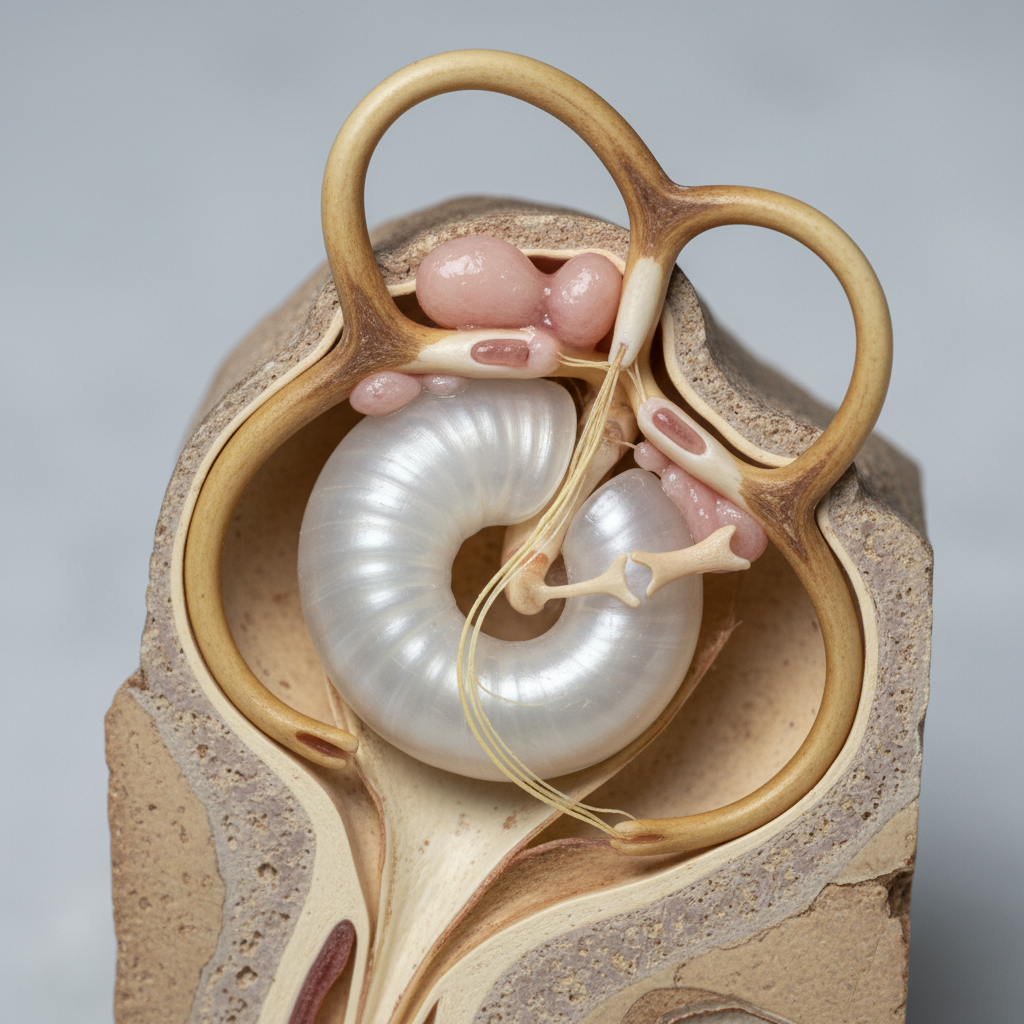
Peripheral vertigo, originating from disorders within the inner ear's vestibular system, represents the most common form of dizziness encountered in clinical practice, accounting for approximately 80% of all vertigo cases. This type of dizziness manifests as a distinct spinning sensation, often described by patients as feeling like they or their environment is rotating, tumbling, or moving when they are actually stationary. The inner ear houses the vestibular organs, including the semicircular canals and otolith organs, which detect head movements and spatial orientation. When these delicate structures become damaged, inflamed, or disrupted, they send conflicting signals to the brain about the body's position and movement, resulting in the characteristic spinning sensation. Doctors distinguish peripheral vertigo through specific clinical features: it typically has a sudden onset, is often triggered by head movements, and is frequently accompanied by nausea, vomiting, and hearing changes. The symptoms tend to be more severe initially but generally improve over time as the brain compensates for the vestibular dysfunction. Physical examination reveals characteristic nystagmus (involuntary eye movements) that is horizontal or rotatory, fatigable with repeated testing, and can be suppressed by visual fixation. Common causes include benign paroxysmal positional vertigo (BPPV), vestibular neuritis, labyrinthitis, and Meniere's disease, each requiring specific diagnostic approaches and treatment strategies.
2. Central Vertigo - When the Brain's Balance Center Malfunctions

Central vertigo arises from dysfunction within the central nervous system, specifically affecting the brainstem, cerebellum, or other brain regions responsible for processing vestibular information and maintaining balance. Unlike peripheral vertigo, central vertigo often presents with more subtle but persistent symptoms that may be accompanied by other neurological signs, making it a more concerning diagnosis that requires immediate medical attention. Patients with central vertigo typically describe a less intense spinning sensation compared to peripheral causes, but the symptoms tend to be more constant and less influenced by head position changes. The condition may develop gradually or have a sudden onset, depending on the underlying pathology, which can include stroke, multiple sclerosis, brain tumors, migraine-associated vertigo, or medication toxicity. Doctors identify central vertigo through careful neurological examination, looking for associated symptoms such as diplopia (double vision), dysarthria (speech difficulties), dysphagia (swallowing problems), weakness, numbness, or coordination problems. The nystagmus associated with central vertigo differs significantly from peripheral causes – it may be purely vertical, bidirectional, or change direction with gaze, and it typically doesn't fatigue with repeated testing nor can it be suppressed by visual fixation. Advanced imaging studies, particularly MRI of the brain, are often necessary to identify structural abnormalities, while additional tests may include blood work to assess for metabolic causes or toxicology screening for medication-related vertigo.
3. Presyncope - The Warning Before the Fall

Presyncope, commonly described as lightheadedness or feeling faint, represents a distinct category of dizziness characterized by the sensation of impending loss of consciousness without the spinning quality of vertigo. This condition occurs when there is inadequate blood flow or oxygen delivery to the brain, creating a feeling that patients often describe as "about to pass out," "woozy," or "floating." The underlying mechanisms typically involve cardiovascular issues, including orthostatic hypotension, dehydration, cardiac arrhythmias, or vasovagal responses. Doctors distinguish presyncope through careful attention to the patient's description of symptoms and the circumstances surrounding their occurrence. Unlike vertigo, presyncope is often triggered by specific situations such as standing up quickly, prolonged standing, emotional stress, pain, or hot environments. The symptoms typically improve when the patient sits or lies down, which helps restore adequate cerebral blood flow. Physical examination focuses on vital signs, including blood pressure measurements in different positions to assess for orthostatic changes, cardiac rhythm evaluation, and assessment of volume status. Patients may also experience associated symptoms such as pallor, sweating, nausea, weakness, or visual changes. The diagnostic workup often includes electrocardiography to evaluate for arrhythmias, echocardiography to assess cardiac function, blood tests to check for anemia or metabolic abnormalities, and sometimes more specialized cardiac monitoring or tilt table testing to evaluate autonomic function and reproduce symptoms in a controlled environment.
4. Disequilibrium - When Balance Becomes a Challenge

Disequilibrium represents a form of dizziness characterized by unsteadiness, imbalance, or the feeling of being off-kilter without the spinning sensation of vertigo or the faint feeling of presyncope. Patients with disequilibrium often describe feeling "wobbly," "unsteady on their feet," or having difficulty maintaining their balance, particularly when walking or standing. This condition typically results from problems with the multiple systems involved in maintaining balance, including the vestibular system, visual input, proprioception (position sense), and the musculoskeletal system. Age-related changes, peripheral neuropathy, medication side effects, visual impairments, and musculoskeletal disorders are common underlying causes. Doctors identify disequilibrium through comprehensive balance assessment, observing the patient's gait, stance, and ability to perform specific balance tasks. The Romberg test, tandem walking, and single-leg standing tests help evaluate different aspects of balance function. Unlike other forms of dizziness, disequilibrium is primarily noticed during movement or when maintaining upright posture, while symptoms typically resolve when sitting or lying down. The condition is particularly common in elderly patients, where multiple contributing factors often coexist, creating a complex clinical picture. Diagnostic evaluation may include neurological examination to assess for neuropathy, vision testing, medication review to identify potentially contributing drugs, and sometimes specialized balance testing such as posturography. Treatment approaches focus on addressing underlying causes, physical therapy for balance training, fall prevention strategies, and careful medication management to minimize contributing factors.
5. Psychogenic Dizziness - When Mind and Body Disconnect

Psychogenic dizziness, also known as psychiatric or functional dizziness, represents a significant category where psychological factors contribute to or entirely cause dizzy symptoms without identifiable organic pathology. This condition affects a substantial number of patients, particularly those with anxiety disorders, panic disorder, depression, or somatization disorders. Patients typically describe vague, non-specific symptoms such as feeling "spacey," "disconnected," "floating," or experiencing a sense of unreality or detachment from their surroundings. The symptoms often lack the clear characteristics of other dizziness types and may be accompanied by other somatic complaints such as fatigue, headaches, or gastrointestinal symptoms. Doctors distinguish psychogenic dizziness through careful psychiatric assessment, detailed history taking that explores the relationship between symptoms and stressors, and the exclusion of organic causes through appropriate testing. The temporal relationship between psychological stressors and symptom onset or exacerbation provides important diagnostic clues. Physical examination is typically normal, and specialized vestibular testing usually shows no abnormalities. However, the diagnosis should not be made hastily or by exclusion alone, as psychological symptoms can coexist with organic vestibular disorders. Anxiety can both cause dizziness and result from it, creating a complex cycle that requires careful evaluation. Treatment approaches include cognitive-behavioral therapy, stress management techniques, anxiolytic medications when appropriate, and patient education about the mind-body connection. Vestibular rehabilitation therapy may also be beneficial, as it can help break the cycle of anxiety and avoidance behaviors that often perpetuate psychogenic dizziness.
6. Medication-Induced Dizziness - When Treatment Becomes the Problem

Medication-induced dizziness represents a common and often overlooked cause of balance problems, particularly in elderly patients who frequently take multiple medications. Numerous drug classes can cause dizziness through various mechanisms, including ototoxicity (damage to the inner ear), cardiovascular effects, central nervous system depression, or metabolic disturbances. Commonly implicated medications include aminoglycoside antibiotics, loop diuretics, aspirin in high doses, anticonvulsants, sedatives, antihypertensives, and chemotherapy agents. The onset of symptoms may be acute following initiation of a new medication or gradual with chronic use and accumulation. Doctors identify medication-induced dizziness through meticulous medication history review, including prescription drugs, over-the-counter medications, and supplements. The temporal relationship between medication initiation or dose changes and symptom onset provides crucial diagnostic information. Polypharmacy, particularly in elderly patients, increases the risk of drug interactions and cumulative effects that can contribute to dizziness. Some medications cause bilateral vestibular damage, resulting in oscillopsia (visual blurring with head movement) and imbalance, while others may affect cardiovascular function leading to orthostatic hypotension and presyncope. Diagnostic evaluation includes careful medication reconciliation, assessment of drug levels when appropriate, and sometimes trial discontinuation or dose reduction of suspected offending agents. The challenge lies in balancing the need to treat underlying medical conditions while minimizing medication-related side effects. Treatment strategies include medication substitution when possible, dose optimization, timing adjustments to minimize peak effects, and careful monitoring during medication changes. Patient education about potential side effects and the importance of reporting new symptoms is essential for early recognition and management.
7. Migraine-Associated Dizziness - When Headaches Affect Balance
Migraine-associated dizziness, including vestibular migraine, represents an increasingly recognized cause of episodic vertigo and balance problems that may occur with or without the classic headache component. This condition affects millions of people worldwide and can present significant diagnostic challenges, as the vestibular symptoms may precede, accompany, or follow headache episodes, or even occur independently. Patients typically experience episodes of vertigo, motion sensitivity, imbalance, or spatial disorientation that can last minutes to hours or even days. The symptoms may be triggered by typical migraine triggers such as stress, certain foods, hormonal changes, sleep deprivation, or sensory stimuli. Doctors diagnose migraine-associated dizziness based on specific criteria that include a history of migraine headaches, episodic vestibular symptoms, and temporal association between vestibular symptoms and migraine features such as headache, photophobia, phonophobia, or visual aura. The diagnosis can be challenging because not all episodes include headache, and the vestibular symptoms may be the predominant or only manifestation. Physical examination during acute episodes may reveal nystagmus, but between episodes, examination is typically normal. Specialized vestibular testing may show abnormalities during acute episodes but is often normal between attacks. The pathophysiology involves the trigeminovascular system and shared neural pathways between pain and vestibular processing centers in the brain. Treatment approaches include migraine prevention medications such as beta-blockers, calcium channel blockers, or anticonvulsants, acute episode management with triptans or anti-nausea medications, and lifestyle modifications including trigger identification and avoidance. Vestibular rehabilitation therapy may also be beneficial for patients with persistent balance problems between episodes.
8. Orthostatic Hypotension - When Gravity Wins the Battle
Orthostatic hypotension represents a specific form of presyncope characterized by a significant drop in blood pressure upon standing, leading to inadequate cerebral perfusion and resulting dizziness, lightheadedness, or even syncope. This condition is defined as a decrease in systolic blood pressure of at least 20 mmHg or diastolic blood pressure of at least 10 mmHg within three minutes of standing. The underlying mechanisms involve failure of normal cardiovascular reflexes that typically compensate for the gravitational effects on blood distribution when changing from supine to upright positions. Common causes include dehydration, medication effects (particularly antihypertensives, diuretics, and vasodilators), autonomic neuropathy (often associated with diabetes), age-related changes in cardiovascular reflexes, and various medical conditions affecting blood volume or vascular function. Doctors diagnose orthostatic hypotension through careful vital sign measurement, including blood pressure and heart rate in supine and standing positions at specific time intervals. The symptoms typically occur within seconds to minutes of standing and improve with sitting or lying down. Associated symptoms may include weakness, fatigue, neck pain, visual disturbances, or cognitive impairment. The condition is particularly common in elderly patients and those with multiple comorbidities. Diagnostic evaluation includes assessment for underlying causes such as dehydration, medication review, evaluation for autonomic dysfunction, and sometimes more specialized testing such as tilt table studies. Treatment strategies focus on addressing underlying causes, optimizing hydration, medication adjustment, graduated compression stockings, physical counter-maneuvers, and in some cases, medications to support blood pressure such as fludrocortisone or midodrine. Patient education about rising slowly and recognizing warning symptoms is crucial for preventing falls and injuries.
9. Benign Paroxysmal Positional Vertigo (BPPV) - When Crystals Go Astray
Benign Paroxysmal Positional Vertigo (BPPV) represents the most common cause of peripheral vertigo, characterized by brief episodes of intense spinning sensation triggered by specific head movements or position changes. This condition occurs when tiny calcium carbonate crystals (otoconia) become dislodged from their normal location in the utricle and migrate into one of the semicircular canals, most commonly the posterior canal. When the head moves, these displaced crystals move within the canal, creating abnormal fluid motion that sends false signals to the brain about head rotation. Patients typically describe sudden onset of severe vertigo lasting seconds to minutes, triggered by movements such as rolling over in bed, looking up, or bending forward. The episodes are often accompanied by nausea but rarely by hearing loss or neurological symptoms. Doctors diagnose BPPV through characteristic history and specific positional testing maneuvers, most commonly the Dix-Hallpike test for posterior canal BPPV. During testing, patients develop typical rotatory nystagmus with a brief delay (latency), limited duration, and fatigue with repeated testing. The diagnosis is confirmed when the maneuver reproduces the patient's symptoms along with the characteristic eye movements. Different types of BPPV affect different semicircular canals, each with specific testing maneuvers and treatment approaches. Posterior canal BPPV is most common, followed by horizontal canal and anterior canal variants. Treatment involves canalith repositioning procedures, such as the Epley maneuver for posterior canal BPPV, which use gravity and specific head movements to guide the displaced crystals back to their proper location. These procedures are highly effective, with success rates exceeding 80% after one or two treatments. Patient education about home exercises and activity modifications during recovery is important for optimal outcomes.
10. Meniere's Disease - The Unpredictable Inner Ear Disorder
Meniere's disease represents a chronic inner ear disorder characterized by episodic vertigo, fluctuating hearing loss, tinnitus (ear ringing), and aural fullness, creating a complex clinical syndrome that significantly impacts patients' quality of life. This condition results from abnormal fluid accumulation (endolymphatic hydrops) within the inner ear's membranous labyrinth, though the exact underlying mechanisms remain incompletely understood. The disease typically affects one ear initially but may eventually involve both ears in approximately 30% of patients over time. Episodes of vertigo can last from minutes to hours and are often severe enough to cause nausea, vomiting, and complete incapacitation. Between attacks, patients may experience varying degrees of hearing loss, tinnitus, and balance problems. Doctors diagnose Meniere's disease based on specific criteria established by international consensus, including definite episodes of vertigo lasting 20 minutes to 12 hours, audiometrically documented hearing loss, fluctuating aural symptoms, and exclusion of other causes. The diagnosis can be challenging in early stages when not all symptoms may be present or clearly defined. Audiometric testing reveals characteristic sensorineural hearing loss, often affecting low frequencies initially and potentially progressing to involve all frequencies over time. Additional testing may include electrocochleography to assess endolymphatic hydrops, vestibular function testing, and MRI to exclude retrocochlear pathology. The unpredictable nature of attacks creates significant anxiety and disability for patients, who often develop anticipatory anxiety and activity restrictions. Treatment approaches include dietary modifications (low-sodium diet), diuretics, vestibular suppressants for acute episodes, and in severe cases, more invasive procedures such as intratympanic steroid injections, endolymphatic sac surgery, or vestibular nerve section. Recent advances include intratympanic gentamicin therapy for intractable cases, though this carries risk of hearing loss.
11. Mastering the Art of Dizziness Diagnosis