10 Scalp Sensation Symptoms Associated With Neurological and Autoimmune Conditions
The human scalp, richly innervated by multiple cranial and cervical nerves, serves as a remarkable diagnostic window into the complex interplay between neurological and autoimmune conditions. While many individuals experience occasional scalp discomfort or sensitivity, persistent or unusual scalp sensations can signal underlying systemic disorders that extend far beyond superficial skin conditions. The trigeminal nerve, occipital nerves, and extensive vascular network beneath the scalp create a sophisticated sensory apparatus that can manifest symptoms ranging from burning and tingling to profound numbness or hypersensitivity. Recent advances in neurological research have illuminated how autoimmune processes, inflammatory cascades, and neurological dysfunction can converge to produce distinctive scalp symptom patterns. These manifestations often precede or accompany more recognizable symptoms of conditions such as multiple sclerosis, lupus, fibromyalgia, and various neuropathies. Understanding these scalp-based warning signs represents a crucial frontier in early diagnosis and intervention, potentially improving outcomes for millions of patients worldwide. This comprehensive exploration examines ten specific scalp sensation symptoms that serve as important clinical indicators, providing healthcare professionals and patients with essential knowledge for recognizing when scalp discomfort transcends common causes and signals the need for deeper neurological or immunological investigation.
1. Burning Scalp Syndrome - When Fire Lives Beneath the Surface
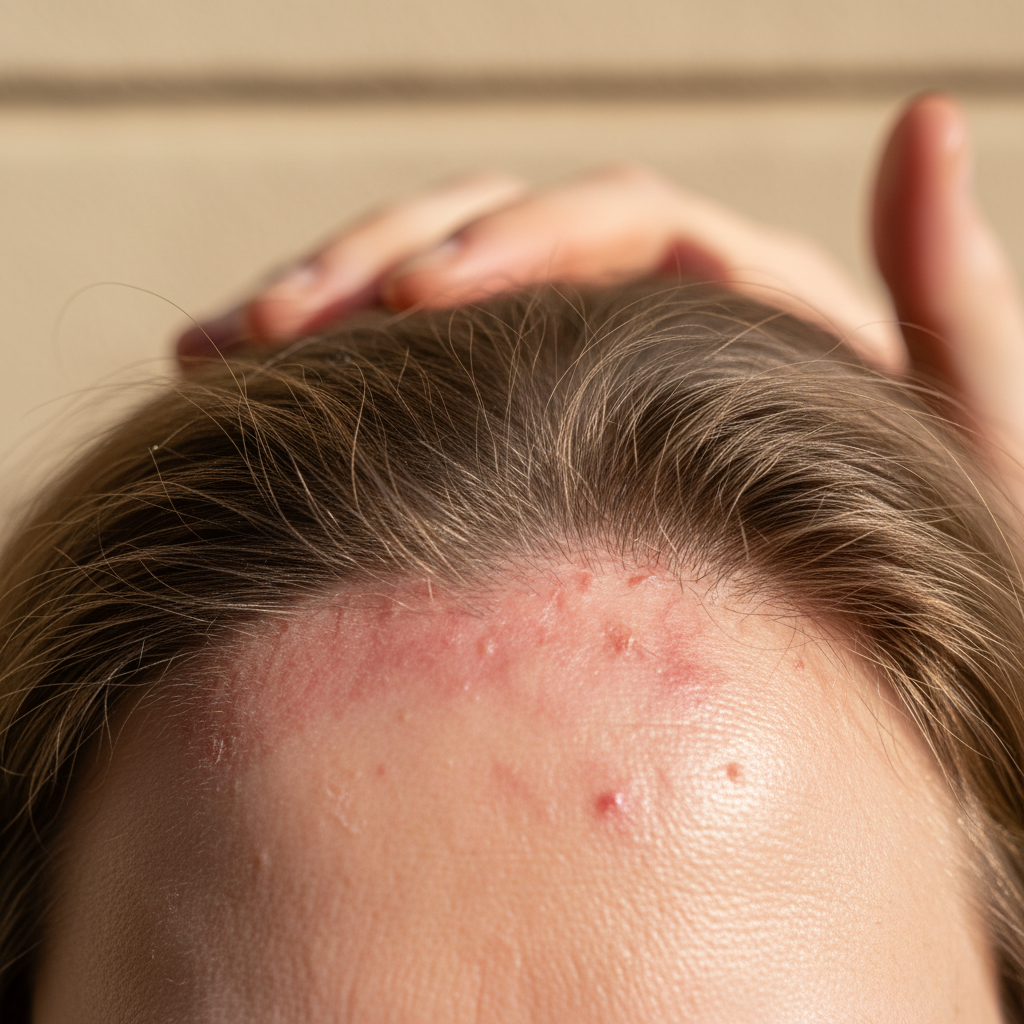
Burning scalp syndrome, medically termed trichodynia, represents one of the most distressing neurological manifestations affecting the cranial region, characterized by persistent burning, stinging, or scalding sensations across various areas of the scalp. This phenomenon frequently emerges as an early indicator of small fiber neuropathy, a condition where the smallest nerve fibers responsible for pain and temperature sensation become damaged or dysfunctional. Patients describe the sensation as feeling like their scalp is perpetually sunburned or as if hot oil has been poured across their head, with symptoms often intensifying during periods of stress, hormonal fluctuation, or exposure to certain environmental triggers. The burning sensation typically affects the crown, temples, or occipital regions and may migrate across different scalp areas throughout the day. Research has established strong correlations between burning scalp syndrome and autoimmune conditions such as systemic lupus erythematosus, Sjögren's syndrome, and autoimmune thyroiditis, where inflammatory processes target nerve endings and disrupt normal sensory processing. Neurological conditions including multiple sclerosis, diabetic neuropathy, and post-herpetic neuralgia also commonly present with scalp burning as inflammatory demyelination or nerve damage affects cranial sensory pathways. The intensity can range from mild warmth to excruciating burning that interferes with sleep, concentration, and daily activities, often accompanied by allodynia where normally non-painful stimuli like gentle touch or hair brushing become intensely uncomfortable.
2. Scalp Tingling and Paresthesias - Electric Signals of Neural Disruption

Scalp tingling, medically classified as paresthesia, manifests as abnormal sensations including pins-and-needles, electric shock-like feelings, or crawling sensations across the scalp surface, often serving as an early warning sign of neurological dysfunction or autoimmune activity. These sensations result from disrupted nerve signal transmission, where damaged or inflamed nerve fibers send erratic electrical impulses to the brain, creating the characteristic "electric" feeling that patients frequently describe as similar to static electricity or mild electrical shocks. The phenomenon commonly affects the vertex, parietal, and occipital regions of the scalp, though it can migrate or affect multiple areas simultaneously, often following specific dermatome patterns that correspond to particular nerve distributions. Multiple sclerosis patients frequently experience scalp paresthesias as one of their earliest symptoms, occurring when inflammatory demyelination affects the trigeminal nerve pathways or other cranial nerves responsible for scalp sensation. Autoimmune conditions such as antiphospholipid syndrome, vasculitis, and autoimmune encephalitis can trigger similar symptoms through inflammatory processes that compromise nerve function and blood flow to neural tissues. The tingling may be intermittent or constant, ranging from barely perceptible sensations to intense, distracting feelings that interfere with concentration and sleep. Vitamin B12 deficiency, often associated with autoimmune conditions like pernicious anemia, can also manifest with scalp paresthesias as the deficiency impairs nerve function and myelin synthesis. Understanding the pattern, duration, and associated symptoms of scalp tingling provides crucial diagnostic information for healthcare providers evaluating potential neurological or autoimmune conditions.
3. Scalp Numbness and Hypoesthesia - When Sensation Disappears

Scalp numbness, or hypoesthesia, represents a concerning neurological symptom characterized by reduced or absent sensation across portions of the scalp, often indicating significant nerve damage or dysfunction within the complex network of cranial and cervical nerves that innervate the head region. This loss of normal sensation can range from mild dulling of touch perception to complete anesthesia where patients cannot feel touch, temperature, or pain in affected areas, creating a distinctive "dead" feeling that many describe as wearing a tight cap or having areas of their scalp "go to sleep." The pattern of numbness often follows specific anatomical distributions corresponding to particular nerve territories, such as the trigeminal nerve branches, greater occipital nerve, or lesser occipital nerve pathways, providing valuable diagnostic clues about the underlying pathological process. Multiple sclerosis frequently presents with scalp numbness as inflammatory demyelination disrupts sensory nerve conduction, particularly affecting the trigeminal system and creating characteristic patches of reduced sensation that may expand or shift over time. Autoimmune vasculitis can cause scalp numbness through inflammatory damage to blood vessels supplying cranial nerves, leading to ischemic nerve injury and subsequent sensory loss. Systemic lupus erythematosus patients may develop scalp numbness as part of neuropsychiatric lupus, where autoimmune inflammation affects both peripheral and central nervous system components. The numbness may be accompanied by weakness in facial muscles, difficulty with jaw movement, or changes in taste sensation, indicating broader cranial nerve involvement that requires immediate medical attention and comprehensive neurological evaluation.
4. Scalp Hypersensitivity and Allodynia - When Gentle Touch Becomes Agony
Scalp hypersensitivity, particularly when accompanied by allodynia—a condition where normally non-painful stimuli become intensely painful—represents a complex neurological phenomenon that significantly impacts quality of life and often signals underlying autoimmune or neurological pathology. Patients experiencing this condition describe excruciating pain from activities as simple as brushing hair, wearing hats, or even gentle touches that would normally be comfortable or barely noticeable, transforming routine daily activities into sources of significant distress. This heightened sensitivity results from central sensitization processes where damaged or inflamed nerve pathways become hyperexcitable, amplifying normal sensory signals into painful experiences that far exceed the actual stimulus intensity. The phenomenon commonly affects individuals with fibromyalgia, where central nervous system dysfunction creates widespread hypersensitivity that frequently includes the scalp region, often accompanied by tender points at the occiput and suboccipital muscle attachments. Trigeminal neuralgia, while typically affecting facial regions, can extend to scalp areas innervated by trigeminal branches, creating zones of extreme hypersensitivity where even air movement or light touch triggers severe shooting pains. Autoimmune conditions such as systemic lupus erythematosus and antiphospholipid syndrome can cause scalp hypersensitivity through inflammatory processes that affect both peripheral nerves and central pain processing mechanisms. Post-herpetic neuralgia following shingles affecting cranial nerves can leave patients with persistent scalp hypersensitivity that may last months or years after the initial infection resolves. The condition often fluctuates in intensity, with stress, hormonal changes, weather patterns, and sleep disturbances serving as common triggers that can dramatically worsen symptoms and expand the affected areas.
5. Scalp Itching and Neuropathic Pruritus - Beyond Surface Irritation

Neuropathic scalp itching, distinct from common dermatological causes, represents a complex neurological symptom where damaged or dysfunctional nerve pathways create persistent, often unbearable itching sensations that cannot be relieved through conventional scratching or topical treatments. This type of itching, medically termed neuropathic pruritus, originates from disrupted nerve signaling rather than skin irritation, creating a maddening cycle where scratching provides no relief and may actually worsen the sensation through further nerve stimulation. Patients describe this itching as deep, burning, or electric in quality, often accompanied by sensations of crawling or movement beneath the scalp surface that can drive individuals to scratch until bleeding occurs, yet the itching persists unabated. Multiple sclerosis patients frequently experience neuropathic scalp itching as demyelinating lesions affect sensory processing pathways, particularly when lesions involve the brainstem or thalamic regions responsible for sensory integration and pain modulation. Autoimmune conditions such as primary biliary cholangitis and chronic kidney disease can trigger scalp pruritus through systemic inflammatory processes and metabolic disturbances that affect nerve function and neurotransmitter balance. Small fiber neuropathy, often associated with diabetes, autoimmune conditions, or vitamin deficiencies, commonly manifests with scalp itching as the smallest nerve fibers responsible for itch sensation become damaged or hyperactive. The itching may follow specific patterns corresponding to nerve distributions, such as the occipital or trigeminal territories, and often worsens at night or during periods of stress, significantly impacting sleep quality and psychological well-being. Understanding the neuropathic nature of this itching is crucial for appropriate treatment, as conventional antihistamines and topical preparations typically provide little relief, requiring neurologically-targeted interventions.
6. Scalp Pressure and Tension Sensations - The Weight of Neurological Dysfunction

Scalp pressure sensations, often described as feeling like wearing an extremely tight hat, having a heavy weight pressing down on the head, or experiencing a vice-like grip around the skull, represent significant neurological symptoms that frequently accompany autoimmune and neurological conditions affecting cranial structures and nerve pathways. These sensations differ markedly from typical tension headaches, as patients report feeling external pressure or constriction specifically affecting the scalp surface rather than deep head pain, often accompanied by a sense of swelling or expansion that creates discomfort when lying down or wearing anything on the head. The pressure sensations commonly result from inflammation affecting the dura mater, the tough membrane surrounding the brain, or from increased intracranial pressure that transmits tension to scalp tissues through complex anatomical connections between internal and external cranial structures. Multiple sclerosis patients frequently experience scalp pressure as part of their symptom complex, particularly when inflammatory lesions affect areas of the brain responsible for sensory processing or when pseudotumor cerebri develops as a secondary complication. Autoimmune conditions such as systemic lupus erythematosus can cause scalp pressure through neuropsychiatric manifestations that include cerebral edema, vasculitis affecting cranial blood vessels, or direct autoimmune inflammation of meningeal structures. Idiopathic intracranial hypertension, often associated with autoimmune conditions or hormonal fluctuations, creates characteristic scalp pressure sensations that worsen with position changes, coughing, or straining, and may be accompanied by visual disturbances and pulsatile tinnitus. The pressure may fluctuate throughout the day, often correlating with stress levels, barometric pressure changes, or hormonal cycles, and can significantly impact concentration, sleep, and daily functioning when severe.
7. Scalp Throbbing and Pulsatile Sensations - Vascular and Neural Convergence
Scalp throbbing and pulsatile sensations represent complex neurological symptoms where patients experience rhythmic, beating, or pulsing feelings across various scalp regions, often synchronous with heartbeat or creating independent pulsation patterns that can be both distressing and diagnostically significant. These sensations differ from typical headaches by focusing specifically on scalp tissues rather than deep cranial structures, with patients describing feelings of blood vessels visibly pulsing beneath the skin, waves of pressure moving across the scalp surface, or rhythmic electrical sensations that create a drumming or beating pattern. The phenomenon often results from vascular inflammation, altered blood flow patterns, or nerve dysfunction affecting the rich network of arteries, veins, and nerve pathways that supply scalp tissues, creating abnormal sensory experiences that reflect underlying pathological processes. Giant cell arteritis, a serious autoimmune condition affecting large and medium-sized arteries, commonly presents with scalp throbbing and tenderness, particularly over the temporal arteries, where inflammation can cause visible vessel prominence, exquisite tenderness, and characteristic pulsatile pain that may herald vision-threatening complications. Systemic lupus erythematosus can cause scalp pulsations through vasculitis affecting cranial blood vessels or through neuropsychiatric manifestations that alter cerebral blood flow and create secondary scalp sensations. Migraine disorders, while primarily neurological, often include prominent scalp throbbing that extends beyond typical headache patterns, with patients experiencing persistent pulsatile sensations in scalp tissues that may continue between actual headache episodes. Hypertensive episodes can manifest with scalp throbbing as elevated blood pressure creates increased pulsatile flow through cranial vessels, often accompanied by neck stiffness, visual changes, or other signs of hypertensive emergency requiring immediate medical attention.
8. Scalp Electrical Sensations and Shock-Like Feelings - Neural Storm Warnings

Scalp electrical sensations, characterized by sudden shock-like feelings, lightning-bolt pains, or sustained electrical buzzing across scalp regions, represent dramatic neurological symptoms that often indicate significant nerve dysfunction or damage within the complex cranial nerve network. Patients describe these sensations as feeling like electrical wires firing beneath their scalp, sudden jolts of electricity shooting across their head, or continuous electrical humming that can be both painful and deeply unsettling, often accompanied by visible muscle twitching or involuntary head movements. These electrical phenomena typically result from nerve hyperexcitability, demyelination, or direct nerve irritation that causes abnormal electrical discharge patterns, creating the characteristic shock-like sensations that can occur spontaneously or be triggered by light touch, movement, or emotional stress. Trigeminal neuralgia, one of the most severe pain conditions known to medicine, can extend to scalp regions innervated by trigeminal branches, creating sudden, excruciating electrical shocks that can be triggered by minimal stimuli such as gentle touch, air movement, or even speaking. Multiple sclerosis frequently presents with electrical scalp sensations as inflammatory demyelination disrupts normal nerve conduction, creating areas of hyperexcitability that generate spontaneous electrical discharges or abnormal responses to normal stimuli. Occipital neuralgia, affecting the greater and lesser occipital nerves, produces characteristic electrical shooting pains that radiate from the neck to the back and top of the head, often described as lightning bolts or electrical shocks that can be triggered by neck movement or pressure on trigger points. Autoimmune conditions such as Guillain-Barré syndrome or chronic inflammatory demyelinating polyneuropathy can cause scalp electrical sensations when cranial nerves become involved in the inflammatory demyelinating process, creating widespread electrical disturbances that may progress or fluctuate over time.
9. Scalp Temperature Dysregulation - Hot and Cold Sensory Disruption
Scalp temperature dysregulation manifests as abnormal sensations of extreme heat or cold affecting scalp regions, where patients experience burning hot or freezing cold sensations that bear no relationship to actual environmental temperature, representing significant dysfunction in the small nerve fibers responsible for temperature sensation and autonomic regulation. These temperature disturbances can present as persistent feelings of scalp burning despite normal skin temperature, sensations of ice-cold patches that feel frozen to the touch, or dramatic temperature fluctuations where areas of the scalp alternate between feeling extremely hot and cold within minutes or hours. The phenomenon results from damage to unmyelinated C-fibers and thinly myelinated A-delta fibers that normally transmit temperature information, creating false signals that the brain interprets as extreme temperature sensations even when no actual temperature change has occurred. Small fiber neuropathy, commonly associated with diabetes, autoimmune conditions, and vitamin deficiencies, frequently presents with scalp temperature dysregulation as the smallest nerve fibers become damaged or dysfunctional, leading to abnormal temperature perception and autonomic dysfunction. Systemic lupus erythematosus can cause temperature dysregulation through autoimmune inflammation affecting peripheral nerves and central temperature regulation centers, creating complex patterns of hot and cold sensations that may correlate with disease activity or medication effects. Multiple sclerosis patients often experience scalp temperature abnormalities as demyelinating lesions affect temperature processing pathways in the brainstem or spinal cord, leading to characteristic patterns of temperature dysregulation that may worsen with heat exposure or physical exertion. Raynaud's phenomenon, while typically affecting fingers and toes, can extend to scalp blood vessels in some patients with autoimmune conditions, creating episodes of extreme cold sensation followed by reactive hyperemia and burning sensations as blood flow returns to affected areas.
10. Scalp Crawling Sensations and Formication - When Nerves Create Phantom Movement
Scalp crawling sensations, medically termed formication when specifically feeling like insects crawling on or under the skin, represent disturbing neurological symptoms where patients experience vivid sensations of movement, creeping, or crawling across their scalp surface despite the absence of any actual external cause. These phantom sensations can be so realistic and intense that patients frequently check mirrors, ask others to examine their scalp, or even seek dermatological evaluation for suspected parasitic infestations, only to find no physical evidence of the perceived movement. The crawling sensations result from