15 Skin Pigmentation Changes That Doctors Use to Narrow Down a Diagnosis
The human skin serves as a remarkable diagnostic canvas, displaying subtle and dramatic pigmentation changes that can provide crucial clues about underlying health conditions. Medical professionals have long recognized that alterations in skin color, texture, and pigment distribution often represent the first visible manifestations of systemic diseases, genetic disorders, and localized pathological processes. From the deepening bronze hue that may signal hemochromatosis to the distinctive café-au-lait spots associated with neurofibromatosis, these pigmentary modifications serve as invaluable diagnostic markers that can significantly narrow differential diagnoses and expedite appropriate treatment interventions. The intricate relationship between melanin production, vascular changes, and cellular metabolism creates a complex spectrum of pigmentation patterns that experienced clinicians can interpret with remarkable precision. Understanding these visual cues requires not only knowledge of dermatological conditions but also appreciation for how systemic diseases manifest through cutaneous changes. This comprehensive exploration examines fifteen critical pigmentation changes that physicians routinely encounter in clinical practice, each representing a unique diagnostic pathway that can lead to life-changing medical discoveries and therapeutic breakthroughs.
1. Melasma - The Mask of Pregnancy and Hormonal Influence

Melasma presents as symmetrical, well-demarcated patches of hyperpigmentation that typically appear on the face, particularly affecting the cheeks, forehead, bridge of the nose, and upper lip in a characteristic butterfly pattern. This condition predominantly affects women of reproductive age, with pregnancy being a significant trigger due to elevated estrogen and progesterone levels that stimulate melanocyte activity. The pigmentation changes associated with melasma can range from light brown to dark brown or even grayish-black, depending on the depth of melanin deposition within the skin layers. Dermatologists utilize Wood's lamp examination to assess the extent and depth of pigmentation, as epidermal melasma typically enhances under ultraviolet light while dermal involvement may not show significant contrast. The condition serves as an important diagnostic indicator for hormonal imbalances, thyroid dysfunction, and can sometimes herald the onset of autoimmune conditions. Treatment approaches vary based on the severity and depth of pigmentation, with topical depigmenting agents, chemical peels, and laser therapies showing varying degrees of success. The persistence of melasma despite treatment cessation often indicates ongoing hormonal influences or genetic predisposition, requiring comprehensive endocrinological evaluation to address underlying causative factors.
2. Vitiligo - The Autoimmune Depigmentation Phenomenon
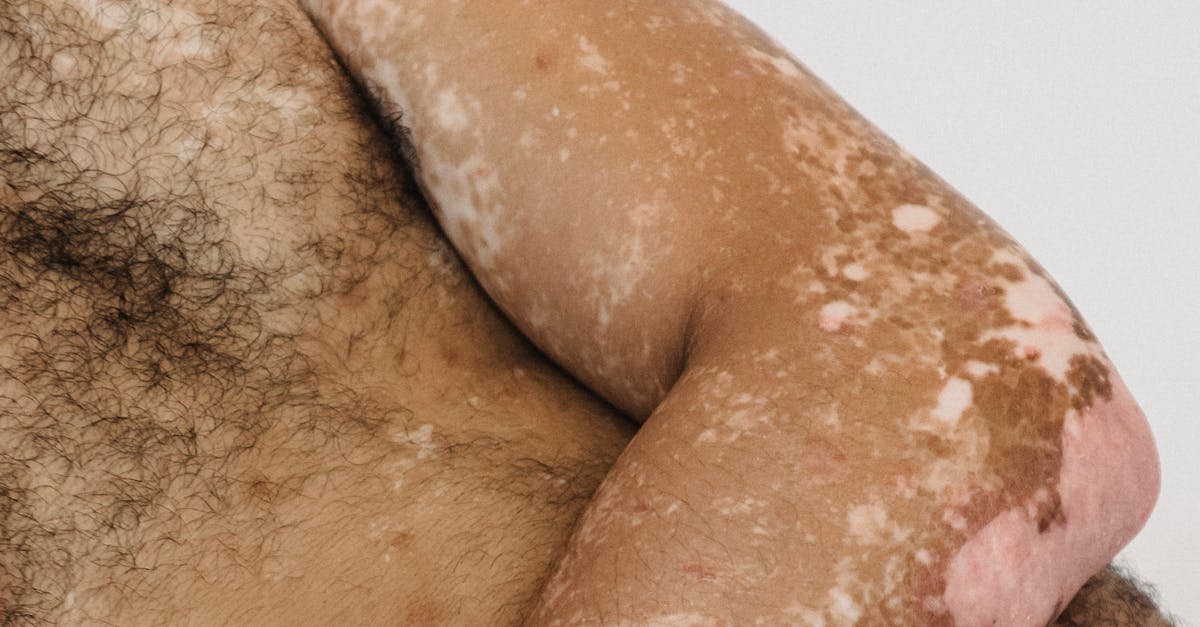
Vitiligo represents one of the most distinctive pigmentation disorders, characterized by the progressive loss of melanocytes resulting in well-defined, depigmented patches that appear as stark white areas against normal skin tone. This autoimmune condition affects approximately 1-2% of the global population and can manifest at any age, though onset typically occurs before age 30. The distribution pattern of vitiligo lesions provides crucial diagnostic information, with segmental vitiligo following dermatomal patterns suggesting neural involvement, while non-segmental vitiligo often presents bilaterally and symmetrically, indicating systemic autoimmune processes. Physicians recognize vitiligo as a potential marker for other autoimmune conditions, including thyroid disorders, diabetes mellitus, pernicious anemia, and Addison's disease, necessitating comprehensive screening for associated comorbidities. The psychological impact of vitiligo cannot be understated, as the stark contrast between affected and unaffected skin can significantly impact quality of life and social functioning. Advanced diagnostic techniques include dermoscopy to identify subtle depigmentation, confocal microscopy to assess melanocyte density, and serological testing for autoimmune markers. Treatment modalities range from topical corticosteroids and calcineurin inhibitors to phototherapy and surgical interventions, with newer JAK inhibitors showing promising results in halting disease progression and promoting repigmentation.
3. Post-Inflammatory Hyperpigmentation - The Skin's Memory of Trauma
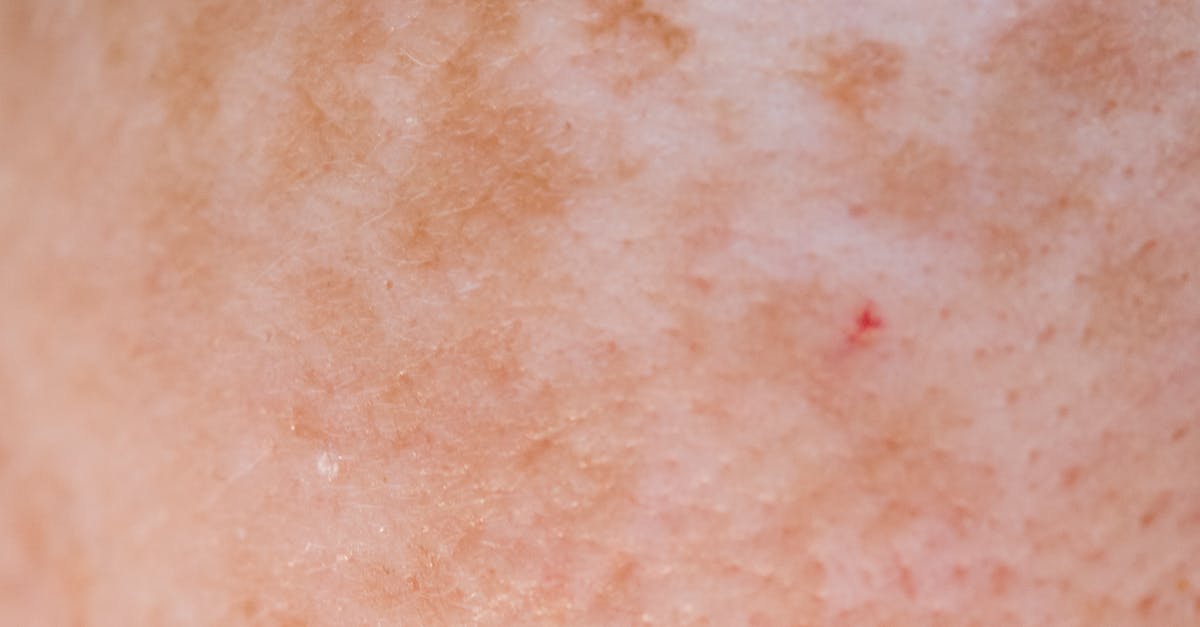
Post-inflammatory hyperpigmentation (PIH) represents the skin's response to injury, inflammation, or irritation, resulting in darkened patches that persist long after the initial insult has resolved. This condition is particularly prevalent in individuals with darker skin tones, where melanocytes respond more vigorously to inflammatory stimuli by producing excess melanin. The appearance of PIH can provide valuable diagnostic information about previous skin conditions, trauma, or ongoing inflammatory processes that may not be immediately apparent during clinical examination. Common triggers include acne, eczema, psoriasis, insect bites, burns, and various dermatological procedures, with the resulting hyperpigmentation serving as a historical record of skin trauma. The distribution and pattern of PIH often mirror the original inflammatory condition, allowing physicians to reconstruct the timeline and nature of previous skin disorders. Dermatologists utilize dermoscopy and reflectance confocal microscopy to differentiate PIH from other pigmentary disorders and assess the depth of melanin deposition. The persistence and intensity of PIH can indicate underlying inflammatory tendencies, immune system dysfunction, or genetic predisposition to hyperpigmentation responses. Treatment approaches include topical depigmenting agents, chemical peels, microneedling, and laser therapy, though prevention through proper management of underlying inflammatory conditions remains the most effective strategy for minimizing PIH development.
4. Café-au-Lait Macules - Genetic Markers in Disguise

Café-au-lait macules appear as uniformly pigmented, light to medium brown patches with smooth borders that can occur anywhere on the body and serve as important diagnostic markers for several genetic conditions. These benign hyperpigmented lesions derive their name from their resemblance to the color of coffee with milk and can range in size from a few millimeters to several centimeters in diameter. While isolated café-au-lait macules are relatively common in the general population, the presence of multiple lesions (typically six or more measuring greater than 5mm in prepubertal children or 15mm in postpubertal individuals) raises suspicion for neurofibromatosis type 1 (NF1), a genetic disorder affecting approximately 1 in 3,000 individuals. Physicians carefully document the number, size, and distribution of café-au-lait macules as part of comprehensive genetic screening protocols, as these lesions often represent the earliest and most consistent manifestation of NF1. The diagnostic significance extends beyond neurofibromatosis, as café-au-lait macules can also be associated with McCune-Albright syndrome, Legius syndrome, and other genetic conditions affecting melanin production and distribution. Advanced imaging techniques and genetic testing complement clinical examination in establishing definitive diagnoses when multiple café-au-lait macules are present. The psychological impact on patients and families requires careful consideration, as the identification of these seemingly innocuous pigmented lesions can lead to life-altering genetic diagnoses requiring ongoing medical surveillance and family counseling.
5. Acanthosis Nigricans - The Metabolic Warning Sign

Acanthosis nigricans manifests as velvety, hyperpigmented plaques that typically develop in flexural areas such as the neck, axillae, groin, and inframammary regions, serving as an important cutaneous marker for underlying metabolic dysfunction. This distinctive pigmentation change results from hyperkeratosis and papillomatosis rather than increased melanin production, creating a characteristic dark, thickened appearance that feels rough to the touch. The condition is strongly associated with insulin resistance, diabetes mellitus, and obesity, making it a valuable screening tool for metabolic syndrome and related cardiovascular risk factors. Physicians recognize acanthosis nigricans as an early warning sign that can precede the development of overt diabetes by several years, providing an opportunity for preventive interventions and lifestyle modifications. The severity and extent of acanthosis nigricans often correlate with the degree of insulin resistance, with more extensive involvement suggesting more advanced metabolic dysfunction. Malignant acanthosis nigricans, though rare, can indicate underlying adenocarcinoma, particularly gastric cancer, necessitating appropriate oncological screening when the condition appears suddenly in older adults without obvious metabolic risk factors. Treatment focuses primarily on addressing underlying insulin resistance through weight loss, dietary modifications, and antidiabetic medications, with topical retinoids and keratolytics providing symptomatic relief. The reversible nature of acanthosis nigricans makes it an excellent marker for monitoring treatment response and metabolic improvement over time.
6. Solar Lentigines - Chronicles of Sun Exposure

Solar lentigines, commonly referred to as age spots or liver spots, represent discrete areas of hyperpigmentation that develop as a direct consequence of cumulative ultraviolet radiation exposure over time. These well-demarcated, uniformly brown macules typically appear on sun-exposed areas including the face, hands, shoulders, and arms, serving as visible markers of photodamage and providing valuable information about an individual's lifetime sun exposure history. The development of solar lentigines follows a predictable pattern, with lesions becoming more numerous and prominent with advancing age, particularly in individuals with fair skin types who have experienced significant sun exposure throughout their lives. Dermatologists utilize the presence and distribution of solar lentigines as indicators of overall photodamage risk and potential for developing skin malignancies, as these lesions often coexist with other signs of chronic sun damage including actinic keratoses and skin cancers. The diagnostic challenge lies in differentiating benign solar lentigines from early melanoma or other pigmented lesions, requiring careful dermoscopic examination and sometimes histopathological confirmation. Advanced imaging techniques such as reflectance confocal microscopy and optical coherence tomography can provide non-invasive assessment of lesion architecture and help guide management decisions. Treatment options include cryotherapy, laser therapy, chemical peels, and topical depigmenting agents, though prevention through sun protection remains the most effective approach for minimizing new lesion development and preventing progression of existing photodamage.
7. Drug-Induced Hyperpigmentation - Pharmaceutical Footprints
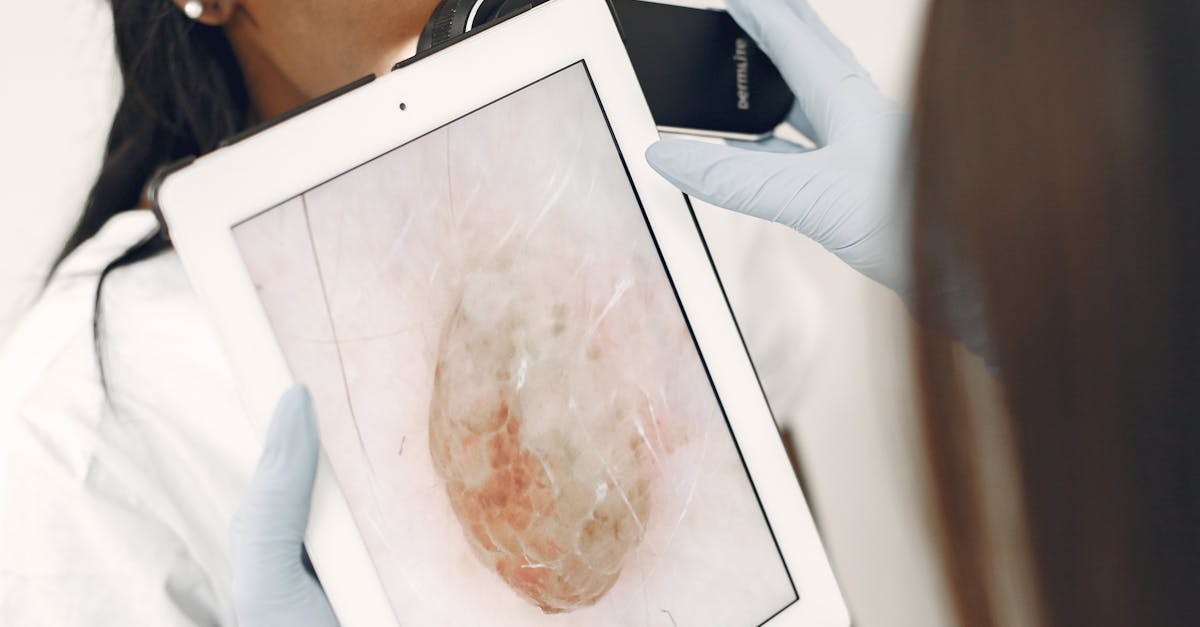
Drug-induced hyperpigmentation represents a diverse group of pigmentary changes that can occur as side effects of various medications, providing important diagnostic clues about medication exposure and potential adverse drug reactions. The mechanisms underlying drug-induced pigmentation vary widely, including direct melanin stimulation, drug-melanin complex formation, and inflammatory responses that trigger secondary hyperpigmentation. Common culprits include antimalarial drugs such as hydroxychloroquine and chloroquine, which can cause characteristic blue-gray pigmentation in sun-exposed areas, and amiodarone, which produces a distinctive slate-gray discoloration particularly affecting the face and hands. Chemotherapeutic agents frequently cause pigmentation changes, with bleomycin producing flagellate hyperpigmentation in linear patterns, and hydroxyurea causing distinctive nail and skin pigmentation that can serve as markers of treatment compliance and cumulative drug exposure. Psychotropic medications, particularly phenothiazines, can cause pigmentation changes that may persist long after drug discontinuation, requiring careful medication history review in patients presenting with unexplained hyperpigmentation. The temporal relationship between drug initiation and pigmentation onset provides crucial diagnostic information, though some drug-induced changes may not become apparent until months or years after treatment begins. Dermatologists must maintain high clinical suspicion for drug-induced pigmentation in patients with unusual or atypical pigmentation patterns, as early recognition and drug modification can prevent progression and potentially reverse existing changes. The reversibility of drug-induced pigmentation varies significantly depending on the causative agent and duration of exposure, with some changes resolving completely after drug discontinuation while others may persist indefinitely.
8. Hemochromatosis - The Bronze Diabetes Connection
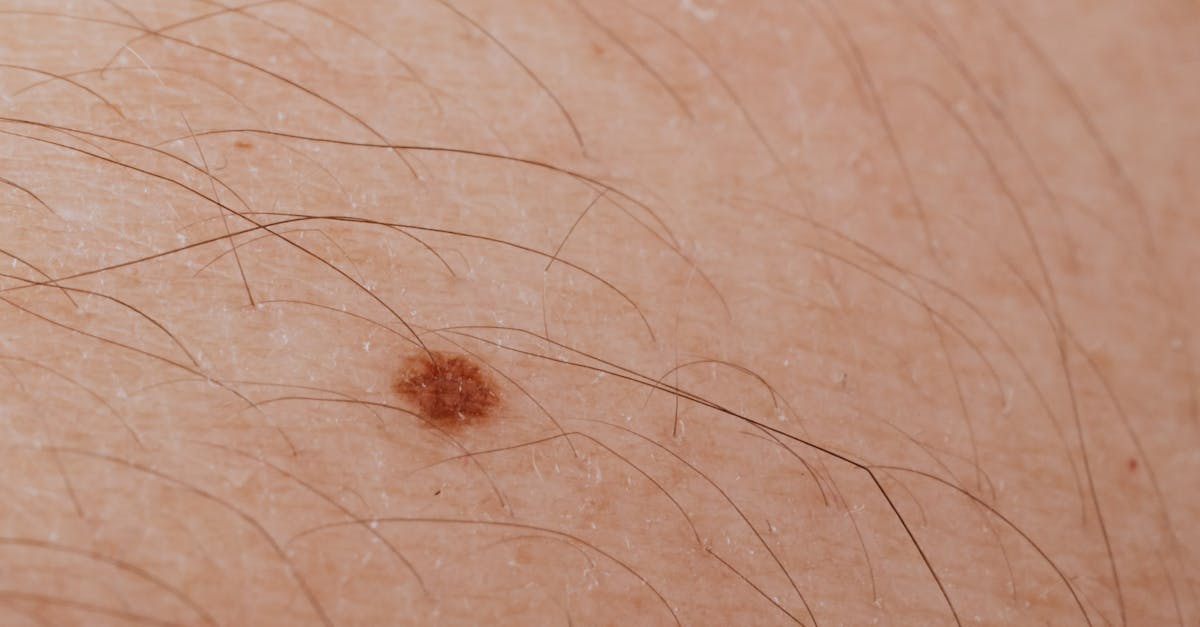
Hemochromatosis produces a characteristic bronze or grayish-brown hyperpigmentation that serves as one of the most recognizable cutaneous manifestations of iron overload disorders, earning the condition its historical moniker of "bronze diabetes." This distinctive pigmentation results from the deposition of iron and melanin in the skin, creating a metallic appearance that is most prominent in sun-exposed areas but can affect the entire integument in advanced cases. The pigmentation changes associated with hemochromatosis often represent a late manifestation of the disease, typically appearing after significant iron accumulation has occurred in vital organs including the liver, heart, and pancreas. Physicians recognize the diagnostic significance of this pigmentation pattern, particularly when accompanied by other clinical features such as diabetes mellitus, hepatomegaly, arthropathy, and cardiac dysfunction. The intensity of skin pigmentation generally correlates with the degree of iron overload, making it a useful clinical marker for disease severity and treatment monitoring. Genetic testing for HFE mutations has revolutionized the diagnosis of hereditary hemochromatosis, allowing for early detection before the development of irreversible organ damage and characteristic pigmentation changes. Secondary hemochromatosis due to repeated blood transfusions, chronic liver disease, or excessive iron supplementation can produce similar pigmentation patterns, requiring careful clinical correlation and laboratory assessment to determine the underlying cause. Treatment with phlebotomy or iron chelation therapy can lead to gradual improvement in skin pigmentation, though complete resolution may not occur if significant structural changes have developed in the skin architecture.
9. Addison's Disease - The Hyperpigmentation of Adrenal Insufficiency
Addison's disease produces a characteristic pattern of hyperpigmentation that serves as one of the most important diagnostic clues for primary adrenal insufficiency, resulting from elevated adrenocorticotropic hormone (ACTH) levels that cross-react with melanocyte-stimulating hormone receptors. The pigmentation changes typically manifest as a generalized darkening of the skin with particular prominence in areas of friction, pressure, and sun exposure, including the knuckles, elbows, knees, and skin creases. Mucosal hyperpigmentation represents a pathognomonic feature of Addison's disease, affecting the oral cavity, particularly the buccal mucosa, gums, and tongue, creating dark patches that are rarely seen in other conditions. The development of hyperpigmentation in Addison's disease follows a gradual progression, often preceding other clinical manifestations such as fatigue, weight loss, and electrolyte abnormalities by months or years. Physicians must maintain high clinical suspicion for adrenal insufficiency in patients presenting with unexplained hyperpigmentation, particularly when accompanied by nonspecific symptoms such as weakness, anorexia, and salt craving. The diagnostic workup includes measurement of morning cortisol levels, ACTH stimulation testing, and assessment of electrolyte balance to confirm adrenal insufficiency and differentiate primary from secondary causes. Recent surgical scars may show particularly prominent hyperpigmentation in patients with Addison's disease, providing additional diagnostic clues during physical examination. Treatment with corticosteroid replacement therapy typically leads to gradual improvement in hyperpigmentation over months to years, though complete resolution may not occur, and the pigmentation changes can serve as markers of treatment adequacy and disease control.
10. Peutz-Jeghers Syndrome - Mucocutaneous Markers of Intestinal Polyposis
Peutz-Jeghers syndrome presents with characteristic mucocutaneous pigmentation consisting of small, dark brown to black macules affecting the lips, oral mucosa, and perioral skin, serving as pathognomonic markers for this autosomal dominant condition associated with gastrointestinal polyposis and increased cancer risk. The pigmented lesions typically appear in early childhood and are most prominent on the vermillion border of the lips, buccal mucosa, and around the mouth, though they can also affect the hands, feet, and genital areas. These distinctive pigmentation changes often represent the first recognizable manifestation of Peutz-Jeghers syndrome, appearing before gastrointestinal symptoms develop and providing an opportunity for early diagnosis and surveillance. The perioral pigmentation may fade with age, particularly on the external skin surfaces, while intraoral lesions tend to persist throughout life, making careful examination of the oral cavity essential for diagnosis. Physicians recognize the critical importance of identifying these pigmentation changes, as Peutz-Jeghers syndrome is associated with significantly increased risks of gastrointestinal and extraintestinal malignancies, including breast, ovarian, pancreatic, and lung cancers. Genetic testing for STK11 mutations can confirm the diagnosis and facilitate family screening, as the condition follows an autosomal dominant inheritance pattern with high penetrance. The management of patients with Peutz-Jeghers syndrome requires comprehensive surveillance protocols including regular endoscopic examination, imaging studies, and cancer screening beginning in adolescence or early adulthood. The distinctive mucocutaneous pigmentation serves not only as a diagnostic marker but also as a constant reminder of the need for ongoing medical surveillance and preventive care throughout the patient's lifetime.
11. Mongolian Spots - Benign Congenital Pigmentation Patterns
Mongolian spots represent benign congenital pigmented lesions that appear as blue-gray to blue-black patches typically located on the lumbosacral area, buttocks, and sometimes extending to the flanks and shoulders, serving as important markers of normal developmental variation rather than pathological processes. These distinctive pigmentation changes result from the delayed migration of melanocytes from the neural crest during embryonic development, leading to the persistence of dermal melanocytes that produce the characteristic blue-gray appearance. The prevalence of Mongolian spots varies significantly among different ethnic populations, occurring in over 90% of Asian, Native American, and African infants, while being relatively uncommon in Caucasian populations, making them important markers of genetic ancestry and population genetics. Pediatricians must be able to distinguish Mongolian spots from other pigmented lesions and, importantly, from signs of physical abuse, as the blue-gray coloration can sometimes be mistaken for bruising by inexperienced observers. The typical location, bilateral distribution, and presence from birth help differentiate Mongolian spots from traumatic injuries, which tend to be asymmetric, located in unusual areas, and show evidence of healing stages. Most Mongolian spots fade gradually during the first few years of life as the dermal melanocytes migrate deeper into the dermis or undergo apoptosis,