15 Nose and Nasal Skin Changes Associated With Rosacea and Autoimmune Conditions
The nose, being the most prominent facial feature, serves as a critical diagnostic window for dermatologists and rheumatologists alike when evaluating patients for rosacea and autoimmune conditions. This central facial structure, with its rich vascular network and sebaceous glands, often becomes the first site to manifest visible changes that signal underlying inflammatory processes. The nasal skin's unique anatomy, characterized by thicker dermis, larger pores, and increased sebum production, makes it particularly susceptible to the inflammatory cascades associated with both rosacea and various autoimmune disorders. Understanding the specific manifestations that occur in this region is crucial for early detection, proper diagnosis, and effective treatment planning. From the subtle erythema of early rosacea to the dramatic nasal deformities seen in advanced cases, and from the butterfly rash of lupus to the saddle nose deformity of granulomatosis with polyangiitis, the nose presents a complex array of changes that require careful evaluation. This comprehensive exploration will examine fifteen distinct nasal and nasal skin changes, providing healthcare professionals and patients with essential knowledge for recognizing these important clinical signs and understanding their broader implications for systemic health.
1. Persistent Erythema and Telangiectasia
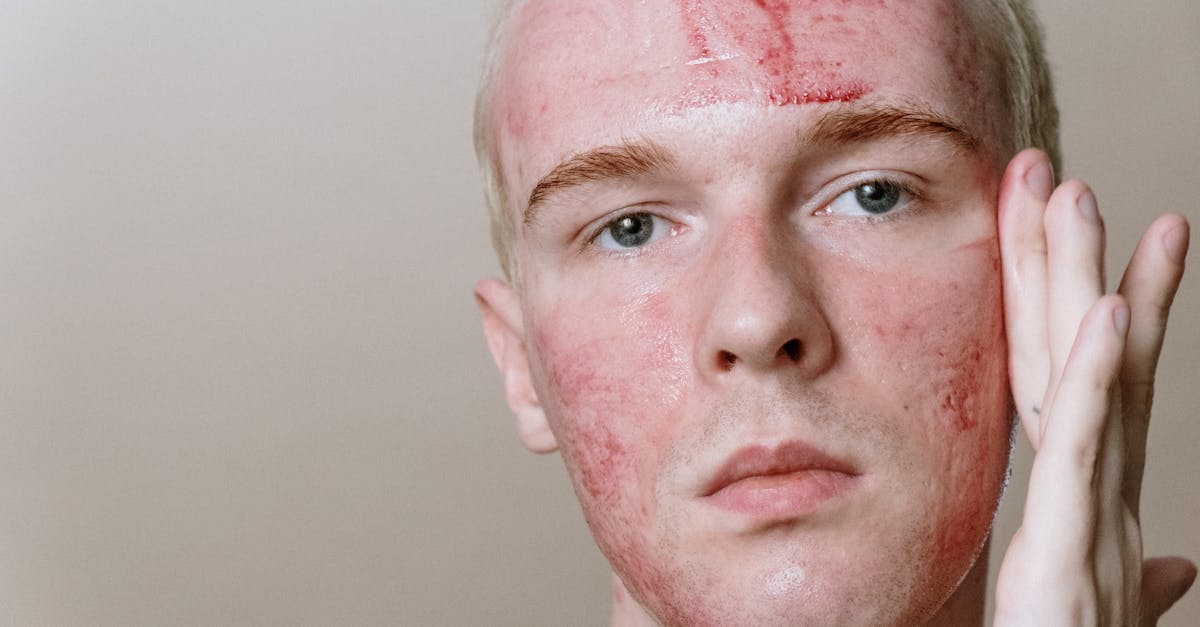
Persistent erythema represents one of the earliest and most common nasal manifestations of rosacea, characterized by a fixed redness that fails to resolve between flare-ups. This persistent vascular dilation occurs due to chronic inflammation of the superficial blood vessels, leading to structural changes in the vessel walls that prevent normal vasoconstriction. The erythema typically begins at the nasal alae and tip, areas with the highest concentration of sebaceous glands and blood vessels, before potentially spreading to involve the entire nasal surface. Accompanying this persistent redness, telangiectasia—visible dilated capillaries appearing as fine red or purple lines—often develops as the condition progresses. These spider-like vessels become permanently dilated due to chronic inflammation and loss of vascular elasticity, creating a characteristic web-like pattern across the nasal skin. The combination of persistent erythema and telangiectasia creates a distinctive appearance that distinguishes rosacea from other inflammatory conditions. Environmental triggers such as sun exposure, temperature extremes, and certain foods can exacerbate these vascular changes, leading to increased visibility and potential progression. Early recognition and treatment of these vascular manifestations are crucial for preventing permanent changes and maintaining optimal cosmetic outcomes.
2. Rhinophyma - Progressive Nasal Tissue Hyperplasia
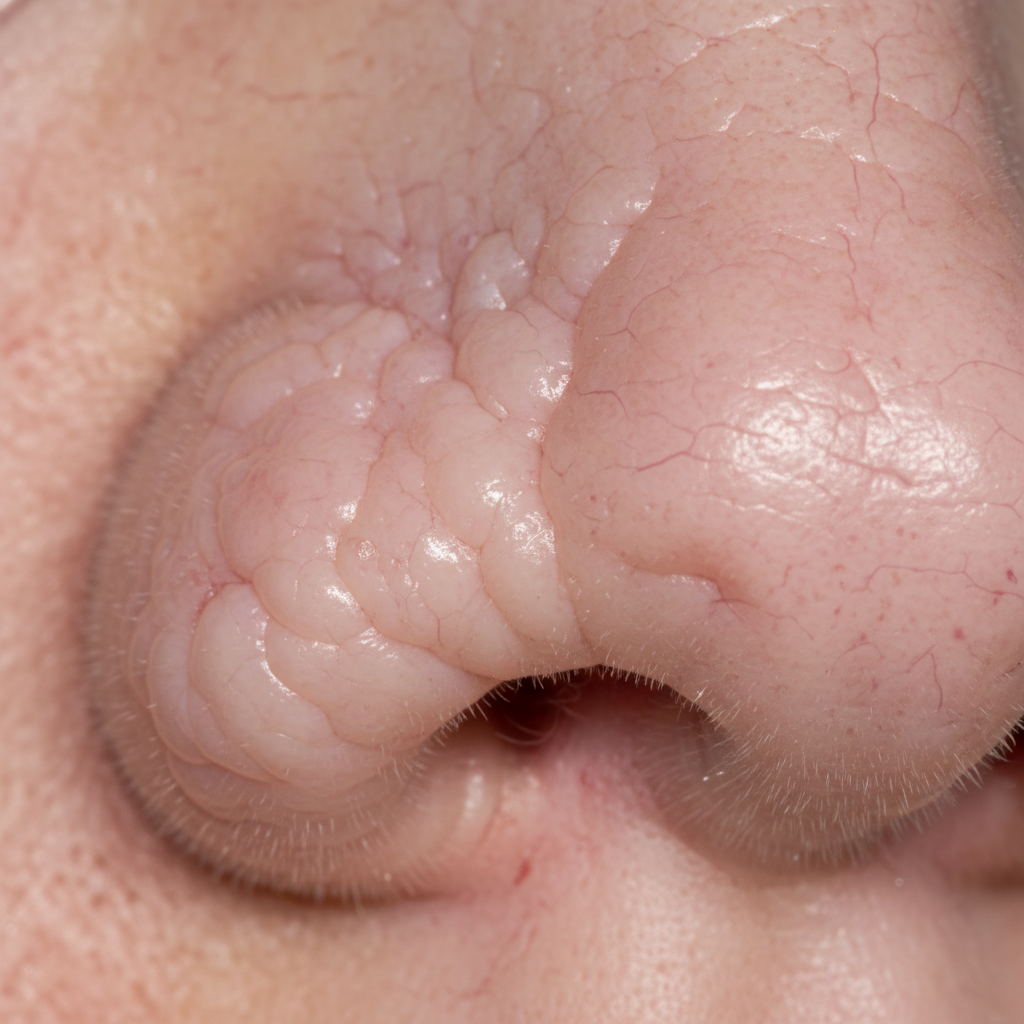
Rhinophyma represents the most severe and disfiguring manifestation of nasal rosacea, characterized by progressive hyperplasia of sebaceous glands, connective tissue, and blood vessels that results in significant nasal enlargement and deformity. This condition, historically and incorrectly associated with alcohol abuse, actually represents the end-stage of untreated or inadequately managed rosacea, occurring predominantly in middle-aged to elderly men. The pathophysiology involves chronic inflammation leading to fibroblast proliferation, increased collagen deposition, and sebaceous gland hyperplasia, creating the characteristic bulbous, irregular nasal appearance. The surface of the affected nose becomes nodular and pitted, with enlarged pores that may become infected or produce excessive sebum. The progressive nature of rhinophyma means that early intervention is crucial, as advanced cases may require surgical intervention including dermabrasion, laser therapy, or surgical excision to restore normal nasal contours. The psychological impact of rhinophyma cannot be understated, as patients often experience significant social embarrassment and reduced quality of life. Modern treatment approaches focus on early aggressive management of rosacea symptoms to prevent progression to this advanced stage, emphasizing the importance of patient education and compliance with long-term therapy regimens.
3. Papulopustular Eruptions on Nasal Skin
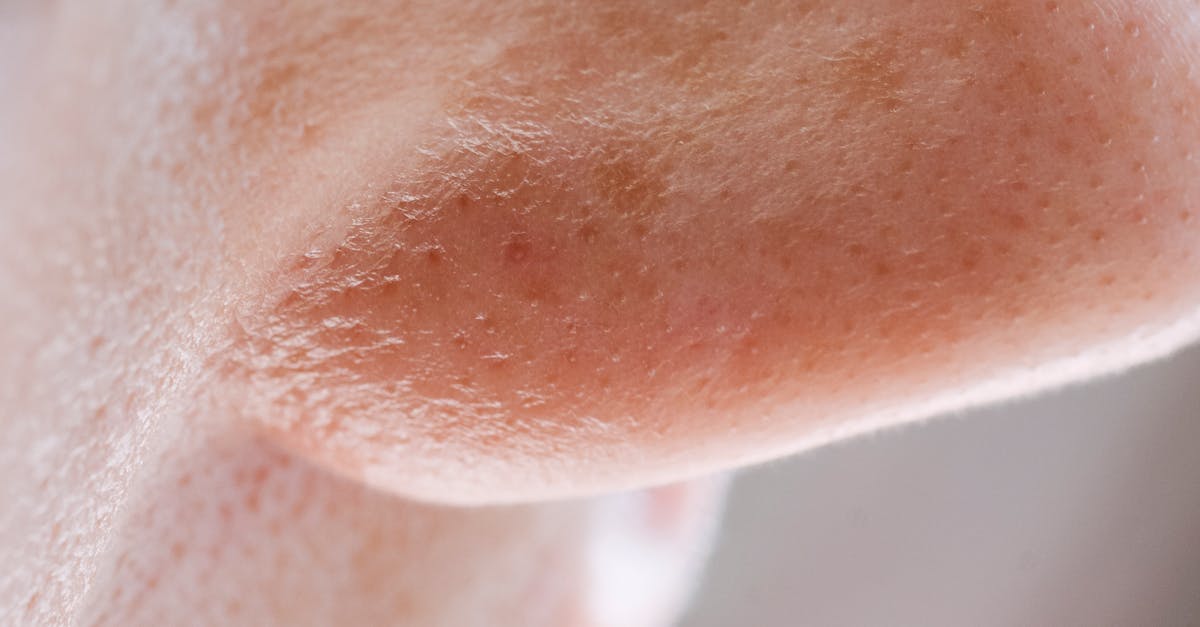
Papulopustular rosacea affecting the nasal region presents with inflammatory lesions that can be easily mistaken for acne vulgaris, though several distinguishing features help differentiate these conditions. The papules and pustules of rosacea typically occur on a background of persistent erythema and are often accompanied by burning or stinging sensations rather than the typical tenderness associated with acne. These inflammatory lesions tend to be more superficial than acne comedones and lack the characteristic blackheads and whiteheads seen in acne vulgaris. The distribution pattern also differs, with rosacea lesions typically affecting the central facial areas including the nose, while acne more commonly involves the entire face, chest, and back. The inflammatory response in rosacea-related papulopustular eruptions involves activation of innate immune pathways, including toll-like receptors and antimicrobial peptides, leading to the characteristic inflammatory infiltrate. Treatment requires careful selection of topical and systemic therapies that address the underlying inflammatory process without exacerbating the condition, as many traditional acne treatments can worsen rosacea symptoms. The chronic nature of these eruptions necessitates long-term management strategies that focus on trigger avoidance, gentle skincare routines, and appropriate anti-inflammatory medications to maintain remission and prevent scarring.
4. Lupus-Associated Malar Rash Extension
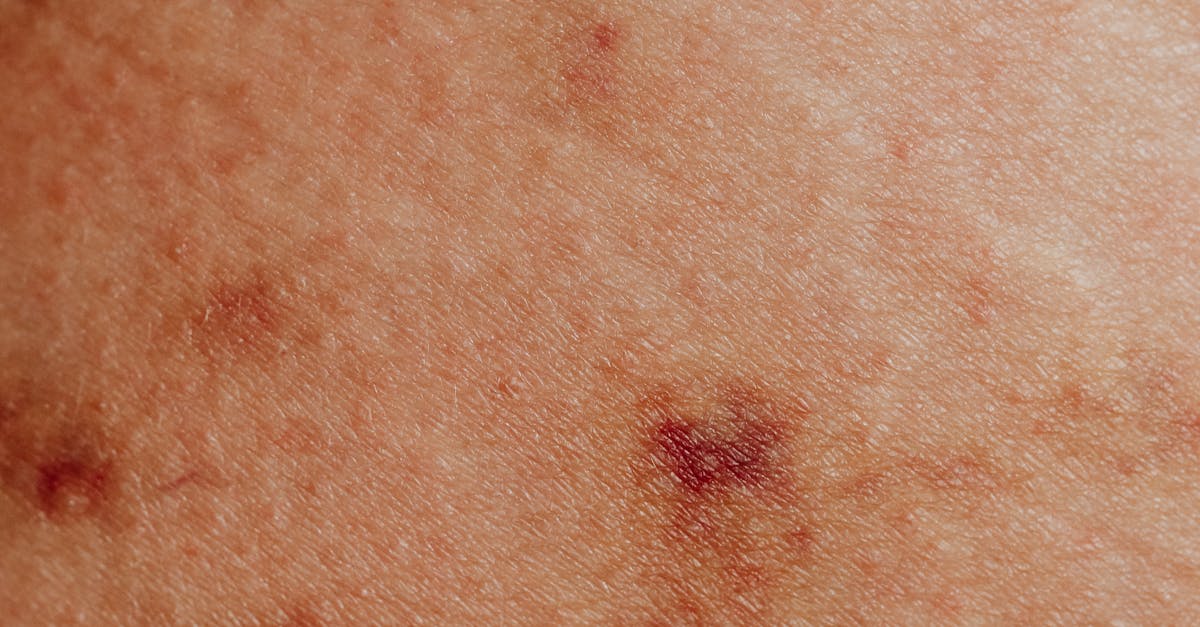
The classic malar rash of systemic lupus erythematosus often extends to involve the nasal bridge and dorsum, creating a distinctive butterfly pattern that serves as one of the most recognizable signs of this autoimmune condition. This photosensitive eruption typically spares the nasolabial folds, a key distinguishing feature that helps differentiate it from other facial rashes. The pathophysiology involves immune complex deposition in dermal blood vessels, leading to complement activation and subsequent inflammatory cascade that manifests as erythema, edema, and sometimes scaling. The nasal involvement in lupus can range from mild erythema to more severe manifestations including bullae, ulceration, or permanent scarring in cases of discoid lupus. The photosensitive nature of this rash means that sun exposure can trigger or worsen the condition, making sun protection a crucial component of management. Histopathological examination reveals interface dermatitis with basal cell vacuolization, dermal mucin deposition, and perivascular lymphocytic infiltration. The presence of nasal involvement in the malar rash often correlates with systemic disease activity and may serve as a marker for monitoring treatment response. Early recognition and appropriate treatment with sun protection, topical corticosteroids, and systemic immunosuppressive therapy when indicated can help prevent permanent scarring and disfigurement.
5. Granulomatosis with Polyangiitis - Saddle Nose Deformity
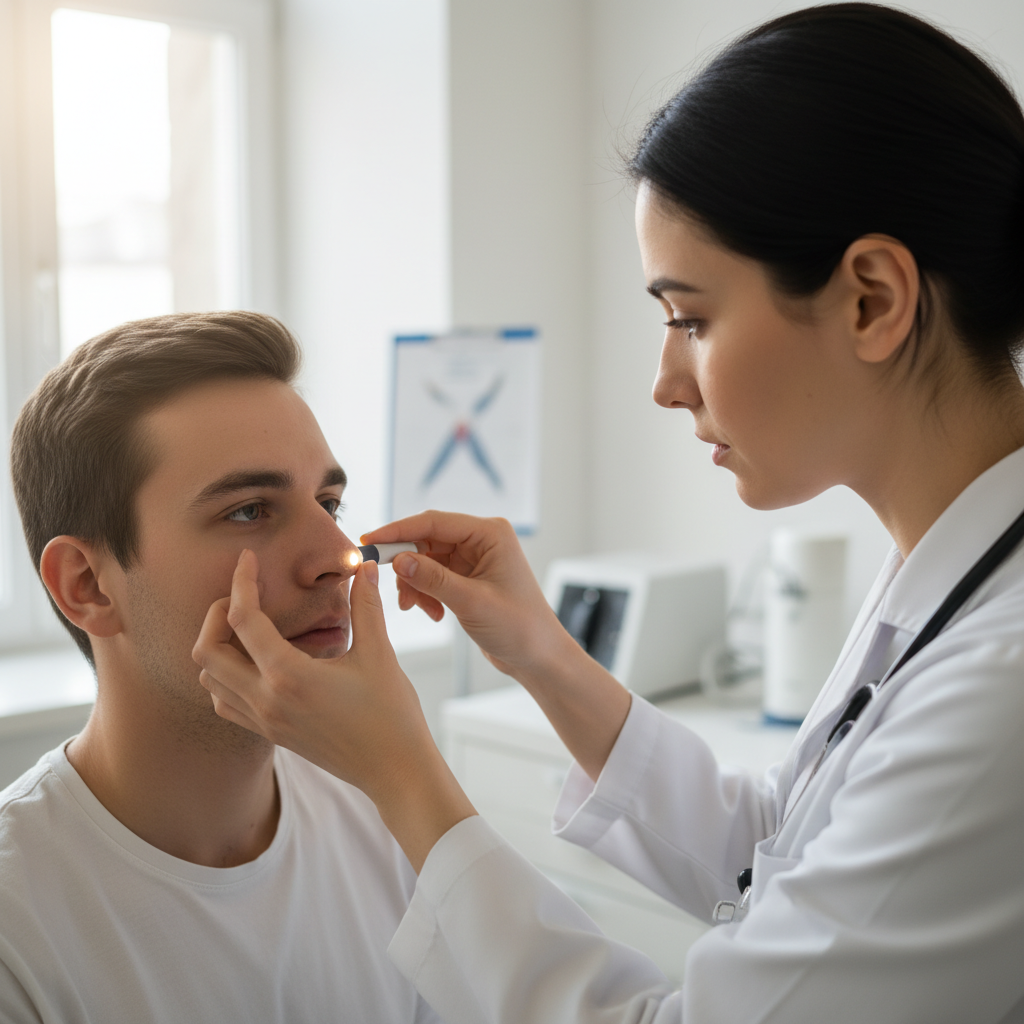
Granulomatosis with polyangiitis (GPA), formerly known as Wegener's granulomatosis, can cause devastating nasal and sinus manifestations, with saddle nose deformity representing one of the most characteristic and severe complications. This deformity results from chronic granulomatous inflammation affecting the nasal cartilage and bone, leading to destruction of the nasal septum and loss of structural support for the nasal bridge. The pathophysiology involves necrotizing granulomatous inflammation with giant cells, epithelioid cells, and areas of necrosis that progressively destroy normal tissue architecture. Early nasal symptoms may include persistent rhinorrhea, epistaxis, nasal crusting, and anosmia, which can precede the development of obvious external deformity by months or years. The progressive nature of cartilage destruction means that early diagnosis and aggressive immunosuppressive treatment are crucial for preventing irreversible structural damage. Advanced cases may require complex reconstructive surgery to restore nasal function and appearance, though the underlying inflammatory process must be controlled before surgical intervention. The presence of nasal involvement in GPA often indicates more severe systemic disease and may be associated with pulmonary and renal manifestations. Regular monitoring with nasal endoscopy and imaging studies is essential for detecting early changes and adjusting treatment accordingly to prevent progression to saddle nose deformity.
6. Dermatomyositis-Related Periorbital and Nasal Changes

Dermatomyositis presents with distinctive cutaneous manifestations that often involve the nasal region as part of the characteristic heliotrope rash and Gottron's papules distribution. The nasal involvement typically manifests as erythematous to violaceous discoloration affecting the nasal bridge and extending toward the periorbital areas, creating a distinctive pattern that helps establish the diagnosis. This photodistributed eruption results from immune-mediated damage to dermal blood vessels and keratinocytes, leading to interface dermatitis and characteristic histopathological changes. The nasal skin may also develop the characteristic scaling and atrophy seen in other sun-exposed areas affected by dermatomyositis. In some cases, patients may develop nasal ulceration or perforation, particularly in the juvenile form of the disease or in cases associated with anti-MDA5 antibodies. The presence of nasal involvement often correlates with disease severity and may indicate increased risk for systemic complications including interstitial lung disease and malignancy in adult patients. Treatment typically involves systemic corticosteroids and immunosuppressive agents, along with aggressive sun protection to prevent exacerbation of photosensitive lesions. The chronic nature of dermatomyositis means that nasal changes may persist even with treatment, requiring long-term management strategies to minimize cosmetic impact and prevent complications such as secondary infection or scarring.
7. Seborrheic Dermatitis Overlap Syndrome
Seborrheic dermatitis frequently coexists with rosacea in the nasal region, creating an overlap syndrome that can complicate both diagnosis and treatment. This condition, characterized by erythematous, scaly patches in areas rich in sebaceous glands, commonly affects the nasal alae, nasolabial folds, and eyebrows. The pathophysiology involves an inflammatory response to Malassezia yeasts that normally colonize sebaceous gland-rich areas, combined with individual susceptibility factors including genetic predisposition and environmental triggers. When seborrheic dermatitis occurs in patients with rosacea, the combination can create a more severe and persistent inflammatory condition that responds poorly to standard treatments for either condition alone. The scaling and flaking associated with seborrheic dermatitis can be particularly problematic in the nasal area, leading to social embarrassment and potential secondary bacterial infection from scratching or picking. Differential diagnosis requires careful evaluation of the clinical presentation, as the erythema and scaling can mimic other conditions including psoriasis, contact dermatitis, or lupus. Treatment strategies must address both the seborrheic component with antifungal agents and the rosacea component with appropriate anti-inflammatory therapies, while avoiding treatments that might exacerbate either condition. Long-term management often requires maintenance therapy and careful attention to trigger factors that might worsen either component of this overlap syndrome.
8. Photoaggravated Inflammatory Changes
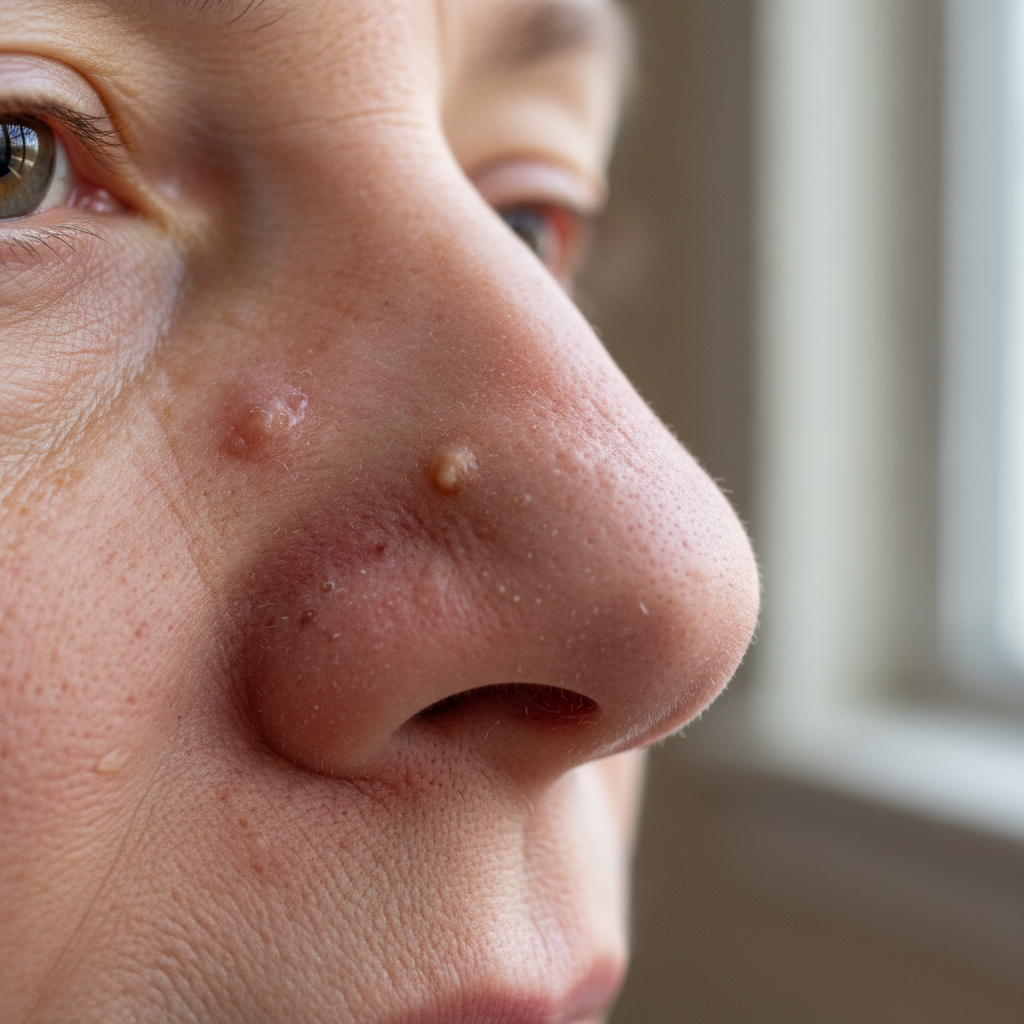
Photoaggravation represents a crucial factor in nasal skin changes associated with both rosacea and autoimmune conditions, as the nose's prominent position makes it particularly susceptible to ultraviolet radiation damage. The nasal tip and dorsum receive the highest UV exposure during normal daily activities, leading to cumulative photodamage that can trigger or worsen inflammatory conditions. In rosacea patients, UV exposure activates inflammatory pathways including matrix metalloproteinases and inflammatory cytokines, leading to increased erythema, papule formation, and vascular changes. The photosensitive nature of many autoimmune conditions, particularly lupus and dermatomyositis, means that nasal involvement is often among the first and most prominent manifestations of these diseases. Chronic photodamage can also lead to permanent changes including telangiectasia, hyperpigmentation, and increased skin fragility that persists even when the underlying inflammatory condition is controlled. The mechanism of photoaggravation involves both direct cellular damage from UV radiation and activation of innate immune pathways that amplify the inflammatory response. Prevention strategies focusing on broad-spectrum sunscreen use, protective clothing, and behavior modification are essential components of treatment for any nasal inflammatory condition. Understanding the role of photoaggravation helps explain why nasal symptoms often worsen during summer months and why sun protection is crucial for long-term management of these conditions.
9. Nasal Vestibulitis and Crusting

Nasal vestibulitis and crusting represent common but often overlooked manifestations of both rosacea and autoimmune conditions, causing significant discomfort and potential complications if left untreated. This condition involves inflammation of the nasal vestibule—the area just inside the nostrils—leading to pain, crusting, bleeding, and sometimes secondary bacterial infection. In rosacea patients, nasal vestibulitis may result from the chronic inflammatory state affecting the entire nasal region, while in autoimmune conditions like granulomatosis with polyangiitis, it may represent early mucosal involvement that precedes more serious complications. The pathophysiology involves disruption of the normal mucosal barrier, leading to increased susceptibility to bacterial colonization, particularly with Staphylococcus aureus. Chronic crusting can create a cycle of trauma and re-inflammation as patients pick at or remove crusts, leading to further tissue damage and delayed healing. The presence of persistent nasal crusting, particularly when associated with epistaxis or anosmia, should prompt evaluation for underlying systemic conditions. Treatment typically involves gentle nasal hygiene with saline irrigation, topical antibiotics when bacterial infection is suspected, and addressing the underlying inflammatory condition. In severe cases, systemic antibiotics may be necessary to treat secondary bacterial infection. Patient education about proper nasal hygiene and the importance of avoiding trauma to the nasal vestibule is crucial for preventing recurrence and complications.
10. Vascular Malformations and Telangiectatic Changes
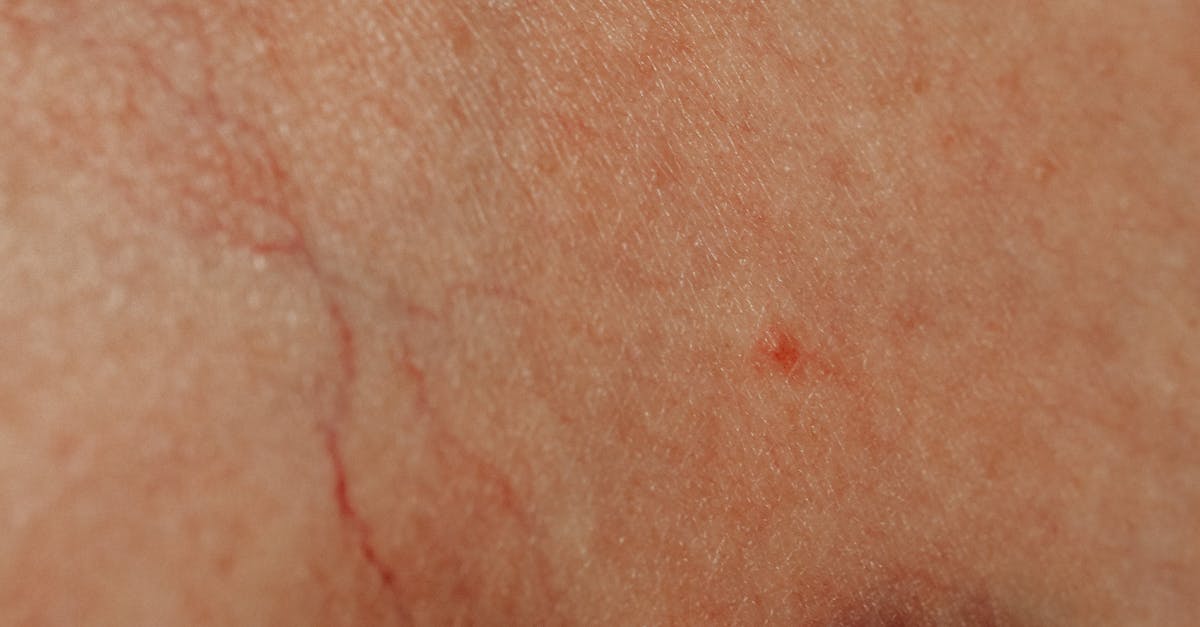
Progressive vascular changes in the nasal region represent a hallmark of chronic inflammatory conditions, with telangiectatic changes evolving from simple capillary dilation to complex vascular malformations over time. These changes begin with functional vasodilation in response to inflammatory mediators but progress to structural alterations in vessel walls that result in permanent dilation and tortuosity. The nasal tip and alae are particularly susceptible due to their rich vascular supply and exposure to environmental triggers. In advanced cases, these telangiectatic vessels can become quite prominent, creating a web-like pattern across the nasal surface that significantly impacts cosmetic appearance. The pathophysiology involves chronic inflammation leading to endothelial dysfunction, loss of smooth muscle tone in vessel walls, and eventual structural remodeling that prevents normal vasoconstriction. These vascular changes can also compromise normal skin barrier function, leading to increased sensitivity to topical products and environmental irritants. Treatment options include laser therapy, intense pulsed light, and sclerotherapy, though the underlying inflammatory condition must be controlled to prevent recurrence. The progressive nature of these vascular changes emphasizes the importance of early intervention in inflammatory conditions affecting the nasal region. Understanding the natural history of these vascular malformations helps guide treatment decisions and patient counseling regarding long-term prognosis and the need for ongoing management.
11. Autoimmune Bullous Disease Manifestations
Autoimmune bullous diseases, including pemphigus vulgaris and bullous pemphigoid, can present with nasal involvement that ranges from subtle erosions to dramatic bullous lesions that significantly impact both function and appearance. These conditions result from autoantibodies directed against structural proteins in the skin and mucous membranes, leading to loss of cell-to-cell adhesion and subsequent blister formation. Nasal involvement in pemphigus vulgaris typically begins with mucosal lesions that may extend to involve the nasal vestibule and external nasal skin, while bullous pemphigoid more commonly affects the external nasal skin with tense bullae that may rupture to form erosions. The nasal location of these lesions can be particularly problematic due to the constant movement and manipulation associated with breathing, speaking, and facial expressions, leading to frequent rupture and slow healing. Secondary bacterial infection is a common complication, particularly when lesions involve the nasal vestibule where bacterial colonization is common. Diagnosis requires careful clinical evaluation combined with histopathological examination and direct immunofluorescence studies to identify characteristic autoantibody patterns. Treatment typically involves systemic immunosuppressive therapy with corticosteroids and steroid-sparing agents, along with local wound care to promote healing and prevent secondary infection. The chronic nature of these conditions requires long-term management strategies that balance disease control with minimization of treatment-related side effects.
12. Sarcoidosis-Related Nasal Infiltration

Sarcoidosis can manifest with distinctive nasal involvement characterized by granulomatous infiltration that creates a characteristic violaceous, infiltrated appearance often described as "lupus pernio." This manifestation typically affects the nasal alae, tip, and sometimes the entire external nose, creating a dusky, purple discoloration that may be accompanied by nodular thickening and surface changes. The pathophysiology involves the formation of non-caseating granulomas composed of epithelioid cells, giant cells, and lymphocytes that infiltrate the dermis and subcutaneous tissue. Unlike other forms of cutaneous sarcoidosis that may resolve spontaneously, nasal involvement often indicates chronic, progressive disease that may be associated with pulmonary fibrosis and other serious systemic complications. The granulomatous infiltration can lead to destruction of normal tissue architecture, resulting in permanent disfigurement if left untreated. Diagnosis requires histopathological confirmation showing characteristic non-caseating granulomas, along with appropriate clinical correlation and exclusion of other granulomatous conditions. Treatment typically involves systemic corticosteroids or other immunosuppressive agents, though response may be slow and incomplete. The presence of nasal sarcoidosis often indicates a more severe form of the disease that may require aggressive treatment and long-term monitoring for systemic complications. Understanding the implications of nasal involvement in sarcoidosis is crucial for appropriate patient counseling and