12 Wrist and Ankle Appearance Changes Linked to Systemic Inflammation
Systemic inflammation serves as a silent orchestrator of numerous physiological changes throughout the human body, with the wrists and ankles functioning as particularly revealing windows into this complex process. These peripheral joints, rich in synovial tissue and surrounded by delicate soft tissue structures, often manifest the earliest and most visible signs of inflammatory cascades that may be occurring systemically. Recent advances in rheumatological and immunological research have illuminated how inflammatory mediators such as tumor necrosis factor-alpha, interleukin-1 beta, and C-reactive protein can trigger a constellation of observable changes in these anatomical regions. From subtle alterations in skin texture and coloration to more pronounced structural modifications involving joint architecture and surrounding tissues, the wrists and ankles serve as diagnostic harbingers of underlying inflammatory conditions. Understanding these manifestations is crucial for healthcare providers and patients alike, as early recognition can lead to timely intervention and improved outcomes. The following exploration delves into twelve distinct appearance changes that may signal systemic inflammation, each representing a unique facet of the body's inflammatory response and offering valuable insights into overall health status.
1. Synovial Joint Swelling and Effusion
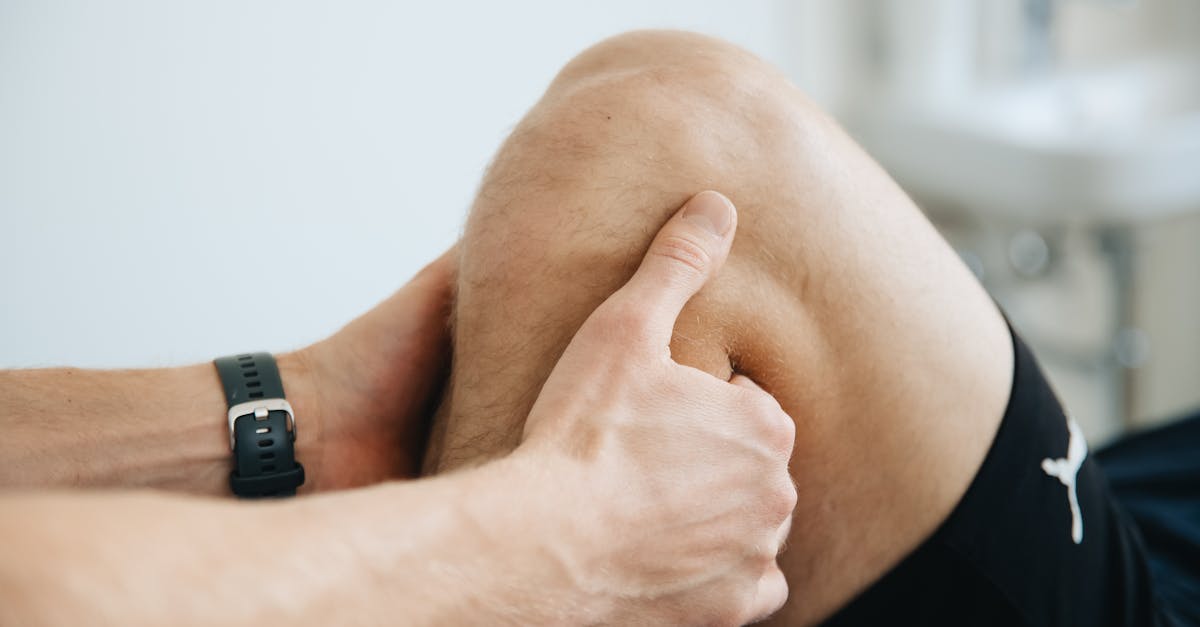
One of the most prominent and clinically significant appearance changes associated with systemic inflammation is the development of synovial joint swelling and effusion in the wrists and ankles. This phenomenon occurs when inflammatory mediators trigger increased vascular permeability within the synovial membrane, leading to fluid accumulation in the joint space and surrounding tissues. The inflammatory cascade begins with the release of cytokines such as interleukin-1 and tumor necrosis factor-alpha, which stimulate the synovial lining cells to produce excess synovial fluid while simultaneously compromising the normal drainage mechanisms. Visually, this manifests as a characteristic puffiness around the affected joints, with the normal anatomical contours becoming obscured by the accumulated fluid. In the wrist, this swelling typically appears as a loss of the normal depression between the tendons on the dorsal surface, while in the ankle, it presents as fullness around the malleoli and loss of the normal hollows anterior and posterior to these bony landmarks. The degree of swelling often correlates with the severity of the underlying inflammatory process, making it a valuable clinical indicator. Additionally, the affected joints may feel warm to the touch due to increased blood flow, and the skin may appear taut and shiny as it stretches to accommodate the increased volume beneath.
2. Erythematous Skin Discoloration
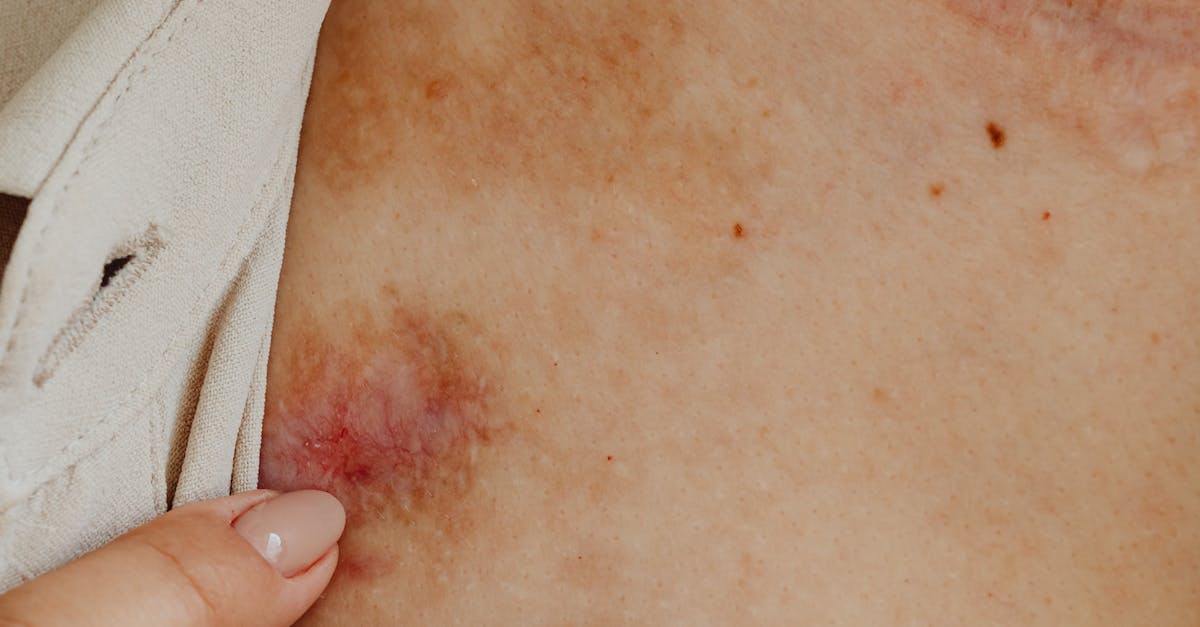
Erythematous skin discoloration represents another hallmark manifestation of systemic inflammation affecting the wrists and ankles, characterized by varying degrees of redness that reflect the underlying vascular changes associated with inflammatory processes. This discoloration occurs as a direct result of vasodilation and increased blood flow to the affected areas, mediated by inflammatory mediators such as histamine, prostaglandins, and nitric oxide. The redness may range from a subtle pink hue to a deep, angry red coloration, depending on the intensity and duration of the inflammatory response. In acute inflammatory conditions, the erythema tends to be more pronounced and may be accompanied by warmth and tenderness, while chronic inflammatory states may present with a more persistent, duller red appearance. The distribution of erythema can provide valuable diagnostic clues, as it may follow specific patterns related to the underlying condition. For instance, in rheumatoid arthritis, the redness often appears symmetrically over the affected joints, while in infectious processes, it may be more localized and intense. The erythema may also extend beyond the immediate joint area to involve surrounding soft tissues, creating a characteristic inflammatory field that can help clinicians assess the extent of the inflammatory process. Importantly, the presence of erythema in conjunction with other inflammatory signs should prompt further evaluation to determine the underlying cause and appropriate treatment approach.
3. Subcutaneous Nodule Formation
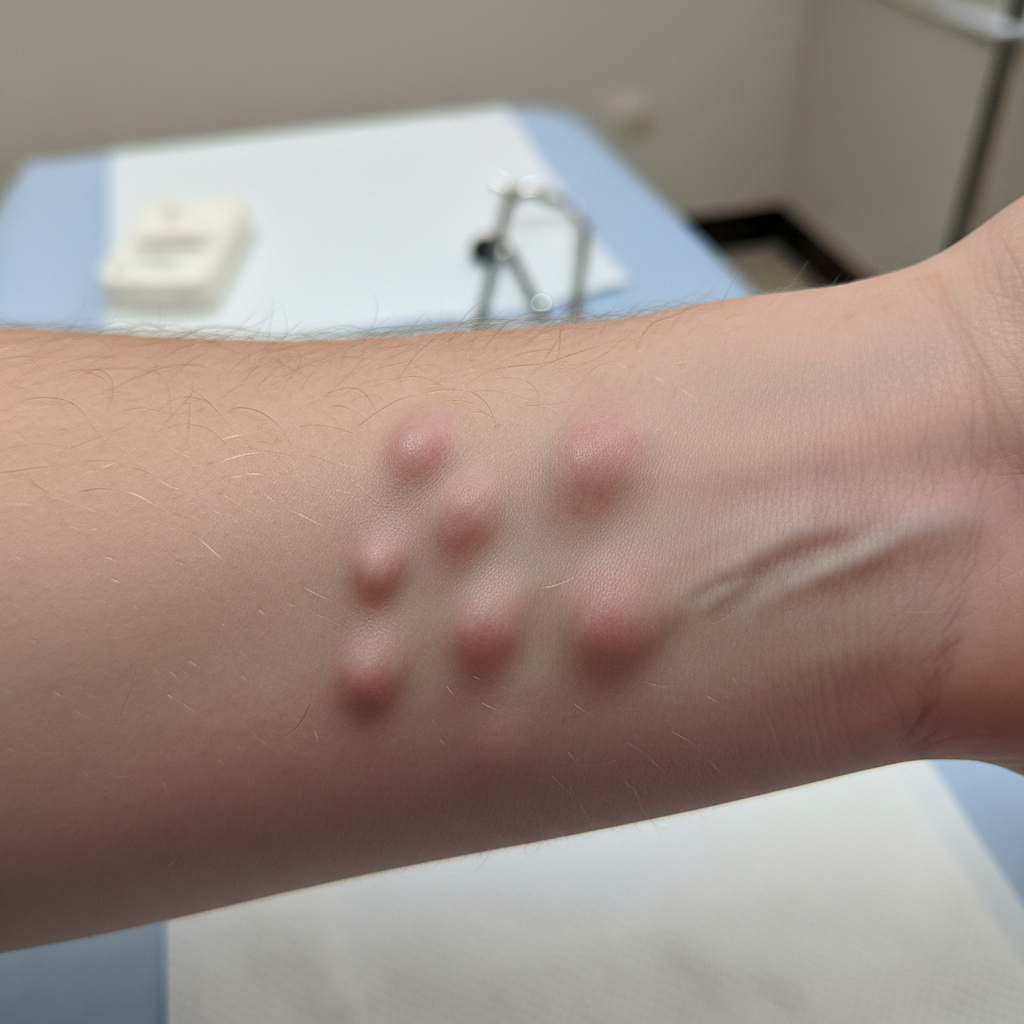
The development of subcutaneous nodules around the wrists and ankles represents a distinctive manifestation of chronic systemic inflammation, particularly associated with autoimmune conditions such as rheumatoid arthritis. These nodules, also known as rheumatoid nodules when occurring in the context of rheumatoid arthritis, are firm, non-tender masses that develop in the subcutaneous tissue overlying bony prominences and pressure points. The pathogenesis involves the formation of granulomatous inflammatory tissue in response to persistent inflammatory stimuli, with the nodules consisting of a central area of fibrinoid necrosis surrounded by epithelioid cells and lymphocytes. Around the wrists, these nodules commonly appear over the extensor surfaces and the ulnar border, while in the ankle region, they may develop over the Achilles tendon insertion or around the malleoli. The size of these nodules can vary considerably, ranging from small, barely palpable masses to large, prominent formations that significantly alter the contour of the affected area. While typically painless, these nodules can become problematic if they interfere with function or become ulcerated due to pressure or trauma. The presence of subcutaneous nodules often indicates a more aggressive form of inflammatory disease and may be associated with other systemic manifestations. Their appearance can fluctuate with disease activity, sometimes enlarging during inflammatory flares and potentially regressing with effective treatment of the underlying condition.
4. Tenosynovitis and Tendon Sheath Inflammation
Tenosynovitis, or inflammation of the tendon sheaths, represents a significant appearance change that commonly affects the wrists and ankles in the context of systemic inflammation. This condition involves inflammation of the synovial-lined sheaths that surround tendons, leading to visible swelling along the course of affected tendons and creating characteristic linear or tubular swellings. The inflammatory process begins when systemic inflammatory mediators infiltrate the tenosynovial tissue, causing increased vascular permeability, cellular infiltration, and subsequent fluid accumulation within the tendon sheath. In the wrist, this commonly affects the flexor tendons on the palmar side and the extensor tendons on the dorsal surface, creating visible swelling that may extend from the forearm into the hand. At the ankle, tenosynovitis frequently involves the posterior tibial, peroneal, or anterior tibial tendons, manifesting as swelling along their respective courses. The affected areas may appear as sausage-like swellings that move with tendon motion, helping to distinguish tenosynovitis from other forms of soft tissue swelling. Patients may experience pain, stiffness, and reduced range of motion, with the inflammation sometimes progressing to involve multiple tendon sheaths simultaneously. In severe cases, the inflammatory process can lead to adhesion formation between the tendon and its sheath, resulting in permanent functional impairment. The presence of tenosynovitis often indicates active systemic inflammation and may precede or accompany joint involvement in various inflammatory arthritides.
5. Skin Texture and Temperature Alterations
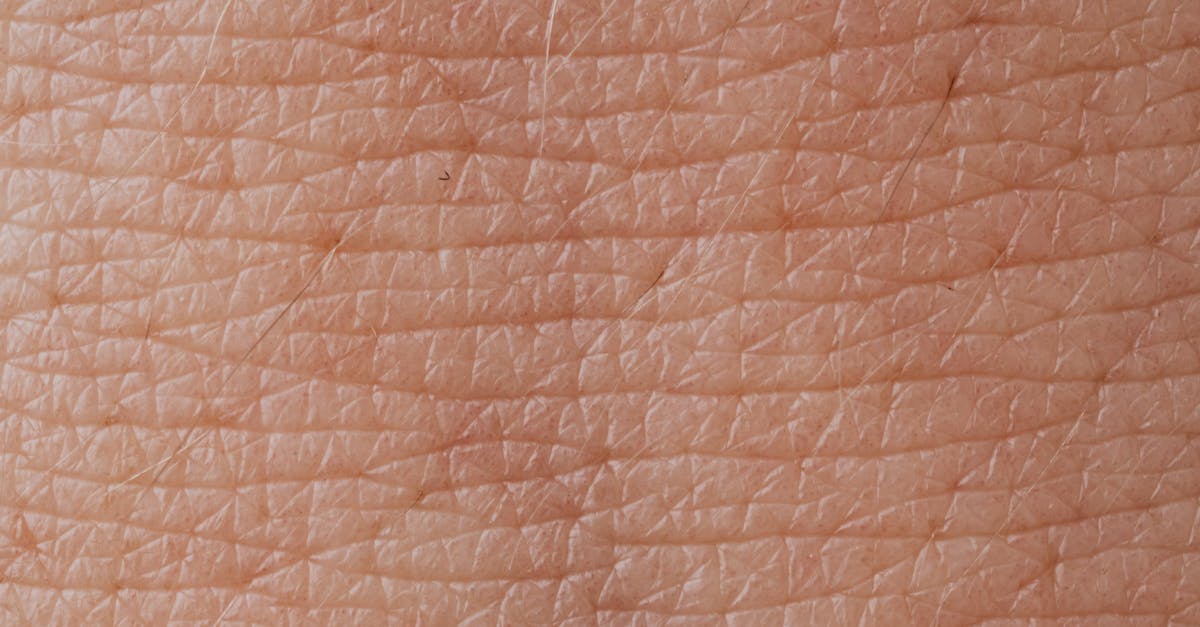
Systemic inflammation produces notable changes in skin texture and temperature around the wrists and ankles, reflecting the complex interplay between inflammatory mediators and cutaneous physiology. The inflammatory process triggers alterations in dermal blood flow, lymphatic drainage, and cellular metabolism, resulting in characteristic changes that can be both visually apparent and palpable. Affected skin often develops a smooth, taut appearance as underlying edema stretches the dermal layers, causing the normal skin creases and wrinkles to become less prominent or disappear entirely. The texture may shift from the normal slightly rough, flexible quality to a more rigid, shiny surface that reflects light differently than healthy skin. Temperature changes are equally significant, with inflamed areas typically feeling warmer than surrounding tissue due to increased blood flow and metabolic activity. This warmth can be detected through palpation and may be accompanied by a throbbing sensation that patients can feel subjectively. In chronic inflammatory conditions, the skin may eventually develop a thickened, leathery quality as repeated inflammatory episodes lead to fibrosis and collagen deposition. Conversely, some patients may experience areas of skin thinning and increased fragility, particularly if they have been treated with corticosteroids. The combination of these textural and temperature changes creates a distinctive clinical picture that experienced healthcare providers can recognize as indicative of underlying inflammatory processes, making careful examination of these characteristics an important component of clinical assessment.
6. Vascular Pattern Changes and Prominence
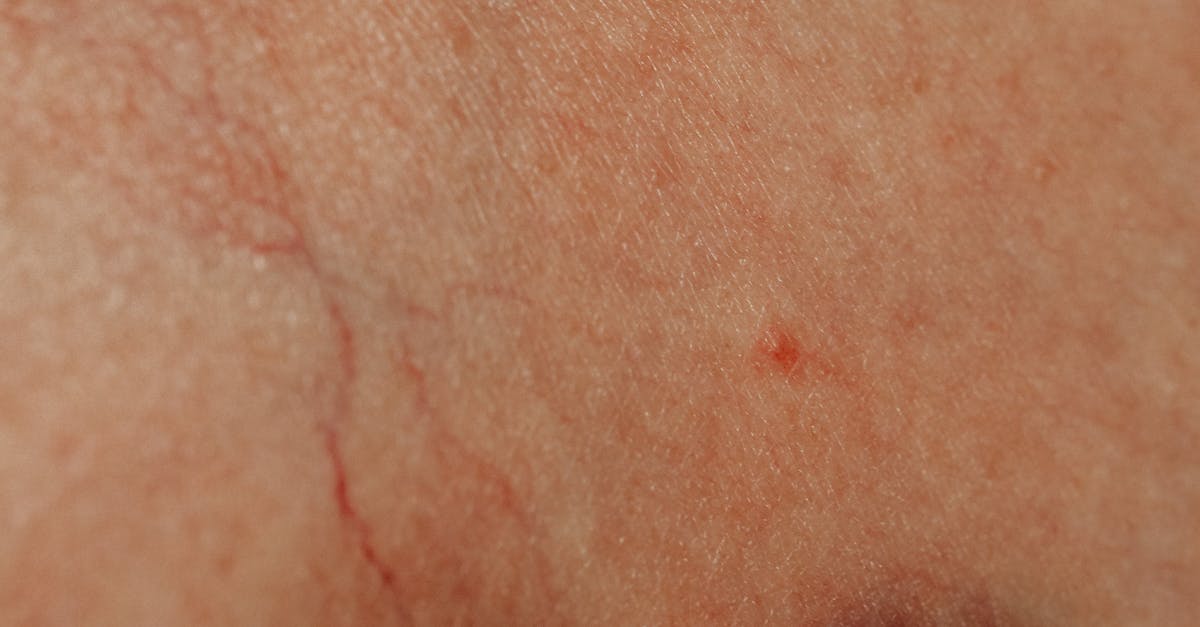
The inflammatory process significantly alters the vascular architecture and appearance around the wrists and ankles, creating distinctive patterns of vessel prominence and distribution that serve as important clinical indicators of systemic inflammation. Inflammatory mediators such as vascular endothelial growth factor (VEGF) and various cytokines promote angiogenesis and vasodilation, leading to the development of new blood vessels and the enlargement of existing ones. This results in increased visibility of superficial veins and capillaries, creating a network of prominent vessels that may appear as blue or purple lines beneath the skin surface. The dorsal aspects of the hands and feet are particularly prone to these changes, where the normally subtle venous pattern becomes markedly more apparent and may take on a tortuous, engorged appearance. In some cases, the inflammatory process can lead to the development of arteriovenous malformations or abnormal vascular connections that further alter the normal vascular architecture. The increased vascular prominence is often accompanied by enhanced perfusion, which contributes to the warmth and erythema associated with inflammatory conditions. Additionally, the inflammatory process can affect capillary integrity, leading to increased permeability and the potential for petechial hemorrhages or purpura in severe cases. These vascular changes may fluctuate with disease activity, becoming more prominent during inflammatory flares and potentially improving with effective anti-inflammatory treatment. Recognition of these vascular pattern changes can provide valuable insights into the severity and activity of the underlying inflammatory process.
7. Joint Deformity and Structural Changes
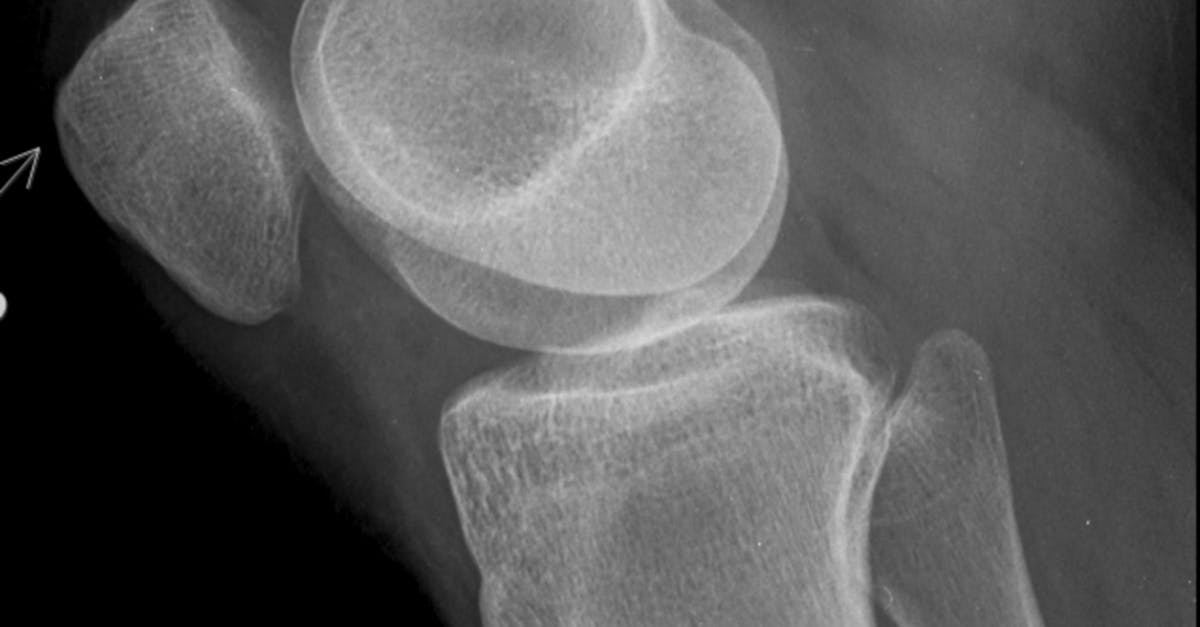
Progressive joint deformity and structural changes represent some of the most visually striking and functionally significant consequences of chronic systemic inflammation affecting the wrists and ankles. The inflammatory process, when persistent and inadequately controlled, leads to destruction of articular cartilage, erosion of subchondral bone, and damage to supporting ligamentous structures, ultimately resulting in permanent alterations to joint architecture. In the wrist, common deformities include ulnar deviation of the fingers, radial deviation of the wrist itself, and the development of a characteristic "zigzag" deformity as the normal alignment relationships become disrupted. The inflammatory process can also lead to carpal collapse, where the normal height and architecture of the wrist are lost due to cartilage destruction and bone erosion. At the ankle, chronic inflammation may result in valgus or varus deformities, where the foot tilts inward or outward relative to the leg, and the development of prominent bony prominences as the normal joint surfaces become irregular. These structural changes occur gradually over time, often beginning with subtle alterations in joint alignment that may be barely noticeable in the early stages but progressively worsening as the inflammatory process continues. The deformities not only create cosmetic concerns but also significantly impact function, leading to reduced range of motion, altered biomechanics, and compensatory changes in adjacent joints. Early recognition and aggressive treatment of systemic inflammation are crucial for preventing or minimizing these irreversible structural changes.
8. Lymphatic Swelling and Edema Patterns
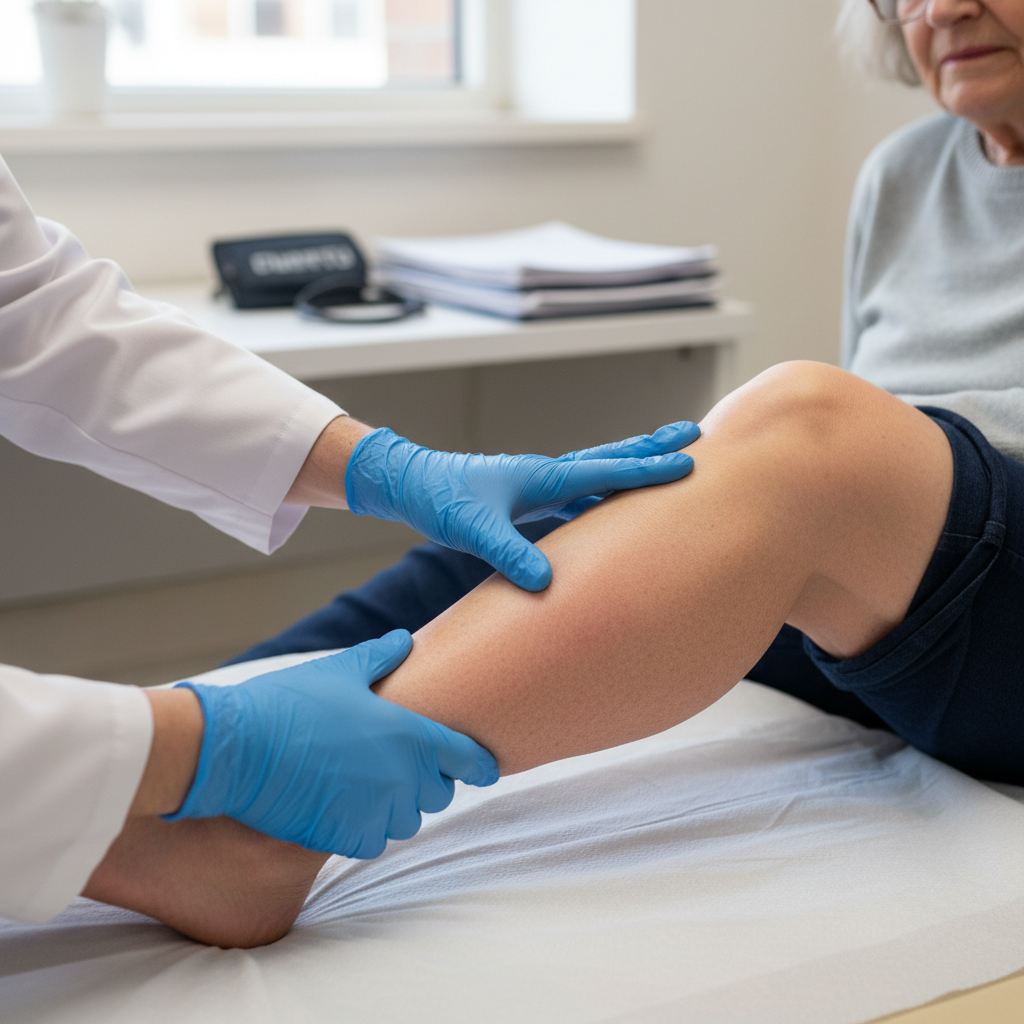
Systemic inflammation significantly impacts lymphatic function around the wrists and ankles, leading to characteristic patterns of swelling and edema that reflect the complex relationship between inflammatory processes and lymphatic drainage. The inflammatory cascade triggers increased vascular permeability and protein extravasation into the interstitial space, overwhelming the normal lymphatic drainage capacity and resulting in fluid accumulation. This lymphatic dysfunction manifests as a distinctive type of swelling that differs from simple fluid retention, characterized by a non-pitting quality that maintains its shape when pressure is applied and released. The edema typically follows anatomical patterns related to lymphatic drainage pathways, often appearing more prominent in dependent areas and showing asymmetric distribution that may not correspond directly to joint involvement. Around the wrists, lymphatic swelling may extend into the dorsum of the hand and fingers, creating a characteristic "sausage-like" appearance of the digits, while ankle involvement often includes the dorsum of the foot and may extend proximally into the lower leg. The inflammatory process can also lead to lymphangitis, or inflammation of the lymphatic vessels themselves, which may appear as red, tender streaks extending from the affected area toward regional lymph nodes. Chronic lymphatic dysfunction associated with persistent inflammation can eventually lead to fibrosis and permanent changes in tissue architecture, making early recognition and treatment essential. The presence of lymphatic swelling often indicates significant inflammatory activity and may be associated with systemic symptoms such as fatigue and malaise.
9. Nail and Periungual Changes

The nail apparatus and surrounding periungual tissues serve as sensitive indicators of systemic inflammation, with various changes in nail appearance and periungual structures providing valuable diagnostic clues about underlying inflammatory processes. Inflammatory mediators circulating in the bloodstream can affect nail matrix function, leading to alterations in nail growth, texture, and appearance that may be among the earliest visible signs of systemic inflammation. Common nail changes include the development of longitudinal ridging, where vertical lines appear along the length of the nail, and transverse ridging or Beau's lines, which represent periods of interrupted nail growth corresponding to inflammatory flares. The nail color may also change, with some patients developing a yellowish discoloration or the appearance of splinter hemorrhages, which are thin, dark lines running vertically under the nail that result from capillary damage. Periungual changes are equally significant and may include erythema and swelling of the nail folds, development of periungual telangiectasias (small dilated blood vessels), and the formation of cuticular overgrowth or ragged cuticles. In some inflammatory conditions, patients may develop nail fold capillary changes that can be visualized with magnification, showing dilated, tortuous capillaries and areas of capillary dropout. These changes may be accompanied by tenderness and increased sensitivity around the nail area. The nail changes associated with systemic inflammation often fluctuate with disease activity and may improve with effective anti-inflammatory treatment, making them useful markers for monitoring therapeutic response.
10. Muscle Atrophy and Soft Tissue Changes
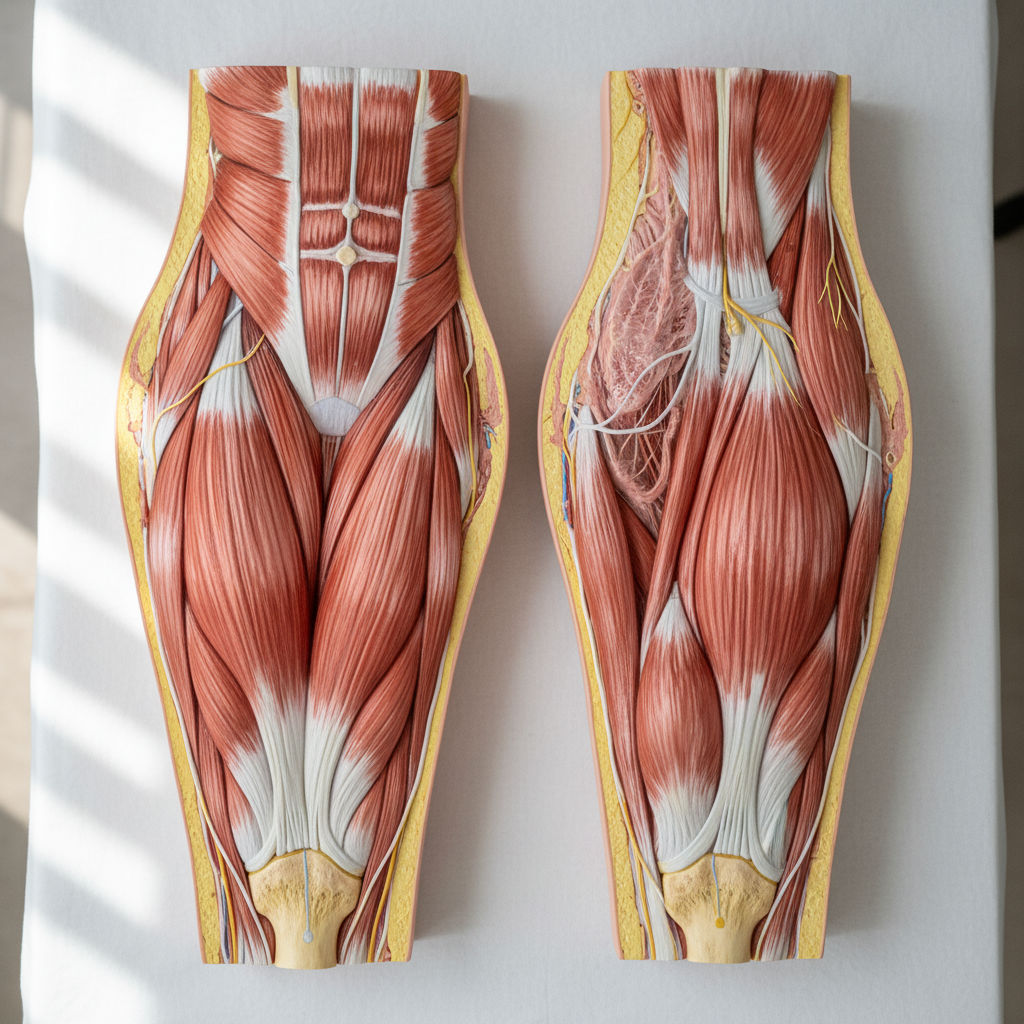
Chronic systemic inflammation exerts profound effects on muscle and soft tissue architecture around the wrists and ankles, leading to visible changes that reflect the catabolic processes associated with persistent inflammatory states. Inflammatory cytokines, particularly tumor necrosis factor-alpha and interleukin-1, promote protein degradation and inhibit protein synthesis, resulting in progressive muscle wasting and alterations in soft tissue composition. Around the wrists, this commonly manifests as atrophy of the intrinsic hand muscles, leading to hollowing of the spaces between the metacarpals and loss of the normal muscular contours of the thenar and hypothenar eminences. The interosseous muscles, which normally fill the spaces between the metacarpal bones, become wasted, creating visible depressions and giving the hand a skeletal appearance. Similarly, around the ankles, chronic inflammation can lead to atrophy of the small muscles of the foot and lower leg, resulting in loss of normal muscular definition and changes in foot contour. The inflammatory process also affects other soft tissue components, including subcutaneous fat and connective tissue, leading to alterations in tissue texture and consistency. Areas that were previously well-padded may become thin and bony prominences more apparent, while other regions may develop fibrotic thickening. These changes not only affect appearance but also have significant functional implications, as muscle atrophy leads to weakness, reduced grip strength, and impaired fine motor control. The progression of these changes can be slow and insidious, making regular monitoring important for detecting early signs of muscle wasting.
11. Pigmentation and Discoloration Patterns

Systemic inflammation can produce distinctive patterns of pigmentation and discoloration around the wrists and ankles that reflect the complex interplay between inflammatory processes, vascular changes, and melanocyte function. The inflammatory cascade affects melanin production and distribution through various mechanisms, including the release of inflammatory mediators that can stimulate or inhibit melanocyte activity, and vascular changes that alter the delivery of nutrients and oxygen to pigment-producing cells. Post-inflammatory hyperpigmentation is a common finding, where areas of previous inflammation develop increased melanin deposition, resulting in brown or darkened patches that may persist long after the acute inflammatory process has resolved. Conversely, some patients may develop hypopigmentation or depigmented areas where chronic inflammation has damaged melanocytes or interfered with normal pigment production. The pattern of discoloration often provides clues about the underlying inflammatory process, with some conditions producing characteristic distributions or configurations of pigmentary changes. Hemosiderin deposition, resulting from chronic inflammation and associated bleeding, can create a distinctive brownish or rust-colored discoloration that is particularly common around the ankles in patients with chronic venous insufficiency or inflammatory conditions affecting the lower extremities. Vascular changes associated with inflammation can also contribute to color alterations, with areas of increased blood flow appearing more red or purple, while regions of compromised circulation may develop a pale or cyanotic appearance. These pigmentary changes may be permanent or may gradually improve with successful treatment of the underlying inflammatory condition, depending on the extent of damage to the pigment-producing apparatus.
12. Range of Motion and Functional Appearance Changes

The impact of systemic inflammation on range of motion and functional appearance around the wrists and ankles represents a critical aspect of disease progression that significantly affects both cosmetic appearance and daily functioning. Inflammatory processes lead to structural changes within and around joints that progressively limit normal movement patterns, creating characteristic postural adaptations and compensatory mechanisms that become visually apparent over time. In the acute phase, inflammation causes pain and swelling that naturally limit movement as patients unconsciously avoid positions that exacerbate discomfort, leading to the adoption of protective postures that may become habitual over time. As inflammation persists, it promotes the formation of adhesions between normally mobile tissue planes, fibrosis of periarticular structures, and contracture of muscles and tendons, all of which contribute to permanent restrictions in joint mobility. Around the wrists, this commonly manifests as