12 Scalp Appearance Changes Beyond Hair Loss Worth Discussing With a Doctor
## Section 1: Introduction - Beyond the Surface: Understanding Scalp Health as a Window to Overall Wellness
While hair loss often dominates conversations about scalp health, the skin beneath our hair serves as a critical diagnostic window that can reveal underlying systemic conditions, nutritional deficiencies, autoimmune disorders, and infectious processes. The scalp's unique environment—rich in sebaceous glands, hair follicles, and blood vessels—makes it particularly susceptible to various pathological changes that extend far beyond simple pattern baldness or temporary shedding. Medical professionals increasingly recognize that scalp appearance alterations can serve as early warning signs for conditions ranging from hormonal imbalances to serious dermatological diseases. These changes may manifest as color variations, texture modifications, inflammatory responses, or unusual growths that warrant professional evaluation. Understanding these diverse manifestations empowers individuals to seek appropriate medical attention before conditions progress or become more challenging to treat. This comprehensive exploration examines twelve significant scalp appearance changes that merit discussion with healthcare providers, offering insight into their potential causes, associated symptoms, and the importance of professional assessment in maintaining both scalp and overall health.
1. Persistent Redness and Inflammation - When Your Scalp Signals Distress
Chronic scalp redness and inflammation represent one of the most common yet potentially serious changes that individuals should discuss with their healthcare providers. Unlike temporary irritation from harsh shampoos or styling products, persistent erythema often indicates underlying inflammatory conditions such as seborrheic dermatitis, psoriasis, or contact dermatitis that require targeted medical intervention. The scalp's rich vascular supply makes inflammatory changes particularly visible, with redness ranging from subtle pink discoloration to angry, deep red patches that may feel warm to the touch. These inflammatory responses can stem from autoimmune conditions where the body's immune system mistakenly attacks healthy scalp tissue, fungal infections that trigger inflammatory cascades, or allergic reactions to hair care products, medications, or environmental allergens. Accompanying symptoms often include itching, burning sensations, flaking, and in severe cases, oozing or crusting that can lead to secondary bacterial infections. The persistence of these symptoms—lasting more than a few weeks despite gentle care and over-the-counter treatments—signals the need for professional evaluation to identify the underlying cause and implement appropriate therapeutic strategies that may include prescription topical treatments, systemic medications, or lifestyle modifications.
2. Unusual Scaling and Flaking Patterns - Decoding Your Scalp's Distress Signals
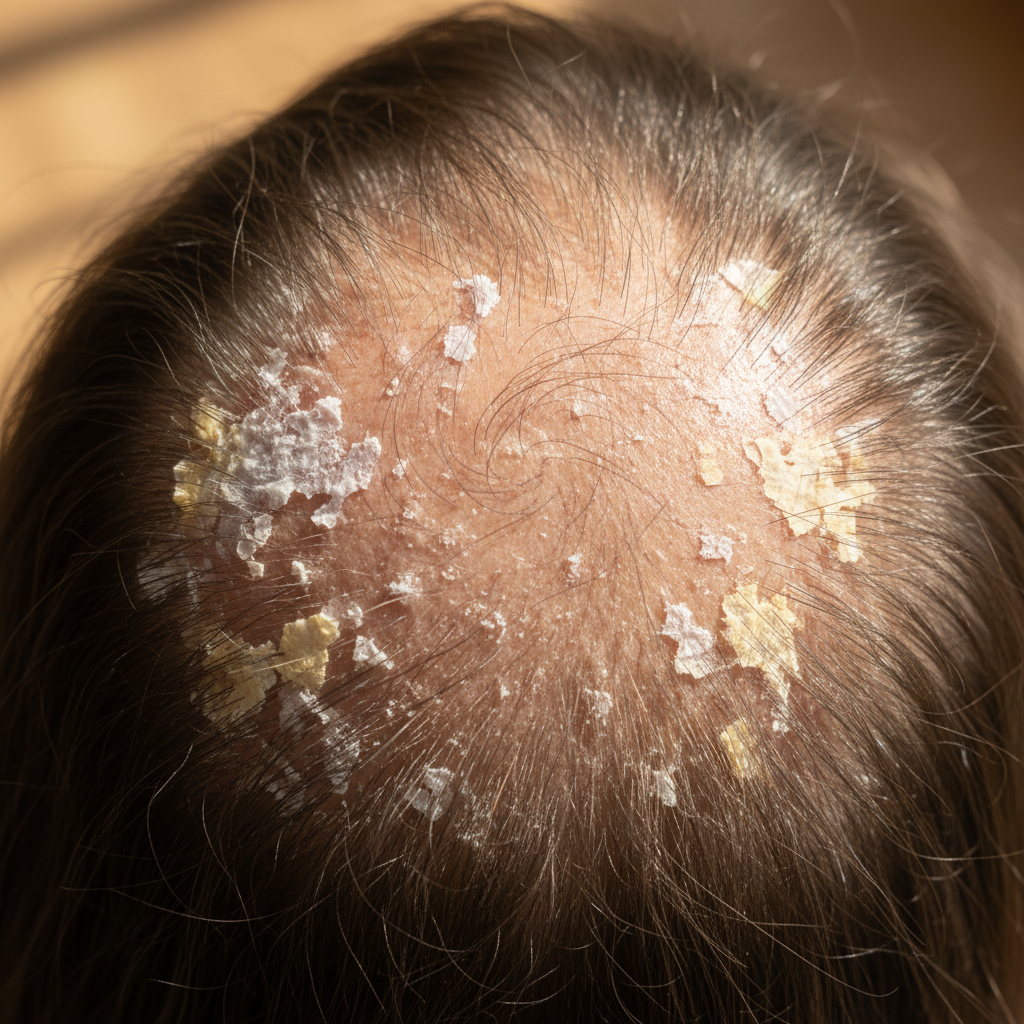
While mild flaking is common and often manageable with over-the-counter dandruff shampoos, unusual scaling patterns or excessive flaking can indicate more serious underlying conditions that require medical attention. Normal scalp shedding involves microscopic skin cells that are barely visible, but pathological scaling presents as thick, adherent flakes, silvery-white plaques, or greasy, yellowish scales that resist removal with regular shampooing. Psoriasis typically produces thick, silvery scales with well-defined borders, often extending beyond the hairline onto the forehead, neck, or behind the ears. Seborrheic dermatitis creates greasy, yellowish scales concentrated in areas rich in oil glands, while fungal infections may produce a combination of scaling and hair breakage with a distinctive musty odor. The distribution pattern of scaling provides crucial diagnostic clues—localized patches may suggest contact dermatitis or fungal infections, while widespread scaling could indicate systemic conditions, nutritional deficiencies, or autoimmune disorders. Additionally, scaling accompanied by hair loss, bleeding, or significant discomfort requires immediate medical evaluation, as these symptoms may indicate more serious conditions such as scarring alopecia, skin cancer, or severe inflammatory disorders that can cause permanent damage if left untreated.
3. Color Changes and Pigmentation Abnormalities - When Your Scalp Changes Hue
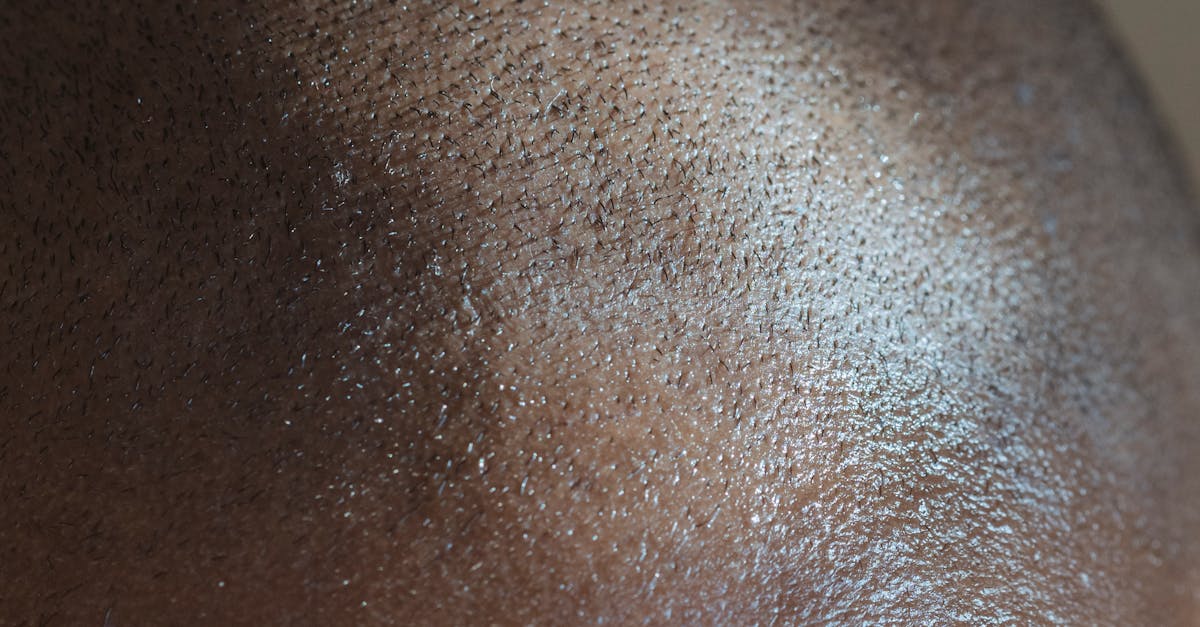
Scalp color changes represent significant alterations that can indicate various underlying health conditions, ranging from benign pigmentary disorders to serious systemic diseases requiring immediate medical attention. Normal scalp coloration varies among individuals based on ethnicity and sun exposure, but sudden or progressive color changes warrant professional evaluation. Hyperpigmentation may manifest as dark patches or spots that could indicate post-inflammatory changes from previous scalp conditions, melasma triggered by hormonal fluctuations, or more concerning possibilities such as melanoma or other skin cancers. Conversely, hypopigmentation or white patches might suggest vitiligo, an autoimmune condition affecting melanocyte function, or scarring from previous trauma or inflammatory conditions. Yellowish discoloration could indicate jaundice related to liver dysfunction, while grayish or ashen tones might suggest circulatory problems or certain medication side effects. Red or purple discoloration beyond typical inflammation patterns could indicate vascular abnormalities, bleeding disorders, or systemic conditions affecting blood vessels. The key distinguishing factor is the persistence and progression of these color changes—temporary discoloration from hair dyes or styling products typically fades within days to weeks, while pathological color changes persist or worsen over time, often accompanied by other symptoms such as texture changes, pain, or systemic symptoms that require comprehensive medical evaluation.
4. Texture Alterations and Surface Irregularities - Feeling the Difference

Changes in scalp texture represent subtle yet significant indicators of underlying pathological processes that can affect both cosmetic appearance and overall scalp health. A healthy scalp typically feels smooth and supple with minimal visible texture variations, but various conditions can create noticeable alterations in surface characteristics. Roughness or sandpaper-like texture may indicate chronic inflammatory conditions, excessive sun damage, or certain autoimmune disorders that affect skin cell turnover and organization. Thickening or induration of scalp tissue could suggest scleroderma, chronic inflammatory conditions, or in rare cases, infiltrative processes that require immediate medical attention. Conversely, unusual thinning or atrophy of scalp skin might indicate aging-related changes, chronic steroid use, or certain genetic conditions affecting connective tissue integrity. Bumpy or nodular textures could represent folliculitis, sebaceous cysts, lipomas, or more concerning growths that require professional evaluation and possible biopsy. The development of hard, immobile areas or sudden texture changes accompanied by pain, rapid growth, or associated systemic symptoms particularly warrant urgent medical consultation. Healthcare providers can perform detailed physical examinations, dermoscopy, and when necessary, tissue sampling to differentiate between benign texture variations and pathological changes requiring specific treatment interventions.
5. Unusual Odors and Discharge - When Your Scalp Sends Chemical Signals

Abnormal scalp odors and discharge represent often-overlooked symptoms that can provide crucial diagnostic information about underlying infectious, inflammatory, or metabolic conditions affecting scalp health. A healthy scalp typically has minimal odor beyond natural sebaceous secretions, but pathological processes can create distinctive smells that warrant medical investigation. Foul, musty, or fishy odors often indicate bacterial or fungal infections that may not be visible to the naked eye but require targeted antimicrobial therapy. Sweet or fruity odors could suggest metabolic disorders such as diabetes, where altered glucose metabolism affects skin chemistry and susceptibility to infections. Discharge from the scalp, whether clear, purulent, bloody, or otherwise discolored, always requires professional evaluation as it may indicate active infection, inflammatory conditions, or in rare cases, more serious underlying pathologies. The consistency, color, and associated symptoms of discharge provide important diagnostic clues—thick, yellow discharge typically suggests bacterial infection, while clear or slightly cloudy discharge might indicate inflammatory conditions or allergic reactions. Bloody discharge, particularly when spontaneous or associated with pain, requires immediate medical attention to rule out serious conditions such as skin cancer, severe inflammatory disorders, or trauma-related complications. Healthcare providers can perform appropriate cultures, microscopic examinations, and other diagnostic tests to identify causative organisms and implement targeted treatment strategies.
6. Temperature Variations and Sensitivity Changes - Thermal Indicators of Scalp Health
Unusual temperature variations and sensitivity changes in the scalp can indicate underlying vascular, neurological, or inflammatory conditions that require medical evaluation and management. Normal scalp temperature should be consistent with overall body temperature and relatively uniform across different areas, but pathological processes can create noticeable thermal variations that patients may detect through touch or subjective sensations. Localized areas of increased warmth often indicate active inflammation, infection, or increased blood flow associated with various dermatological conditions, while cold spots might suggest vascular compromise, nerve dysfunction, or certain autoimmune conditions affecting circulation. Hypersensitivity to temperature changes, where normal environmental temperatures cause discomfort or pain, could indicate nerve damage, inflammatory conditions, or certain medications' side effects that affect sensory perception. Some patients develop allodynia, where normally non-painful stimuli such as gentle touch or mild temperature changes cause significant discomfort, suggesting underlying neurological involvement that requires specialized evaluation. Conversely, decreased temperature sensitivity or numbness might indicate nerve damage from trauma, certain medical conditions, or medication side effects that could affect scalp health and the ability to detect other warning signs. These thermal and sensitivity changes often accompany other symptoms such as pain, tingling, or visible alterations, and their presence should prompt comprehensive medical evaluation to identify underlying causes and implement appropriate treatment strategies.
7. Swelling and Edema - When Your Scalp Retains Fluid

Scalp swelling and edema represent concerning changes that can indicate various underlying medical conditions ranging from localized inflammatory processes to systemic disorders affecting fluid balance and circulation. Unlike temporary swelling from minor trauma or allergic reactions that resolve within hours to days, persistent or progressive scalp edema requires medical evaluation to identify and address underlying causes. Localized swelling may result from infections, cysts, tumors, or inflammatory conditions such as cellulitis that require prompt antibiotic therapy to prevent spread to deeper tissues or systemic circulation. Generalized scalp swelling could indicate systemic conditions such as heart failure, kidney disease, or liver dysfunction that affect the body's ability to regulate fluid balance, requiring comprehensive medical management beyond topical treatments. The character of swelling provides important diagnostic information—soft, pitting edema that leaves indentations when pressed suggests fluid accumulation, while firm, non-pitting swelling might indicate inflammatory infiltration, fibrosis, or mass lesions requiring different therapeutic approaches. Associated symptoms such as pain, warmth, redness, or systemic signs like fever, fatigue, or changes in urination patterns help healthcare providers determine the urgency and scope of necessary investigations. Rapid onset swelling, particularly when accompanied by difficulty breathing, facial swelling, or other signs of allergic reactions, constitutes a medical emergency requiring immediate intervention to prevent potentially life-threatening complications.
8. Visible Blood Vessels and Vascular Changes - Circulatory Clues on Your Scalp
The appearance of prominent blood vessels or vascular changes on the scalp can indicate various underlying conditions affecting circulation, skin integrity, or systemic health that warrant professional medical evaluation. While some degree of visible vasculature is normal, particularly in individuals with fair skin or thin scalp tissue, sudden appearance or progressive prominence of blood vessels may signal underlying pathological processes. Telangiectasias, or small dilated blood vessels, can result from chronic sun exposure, rosacea, certain medications, or systemic conditions affecting vascular integrity and require evaluation to determine appropriate management strategies. Spider angiomas, characterized by a central red spot with radiating vessels, may indicate liver disease, hormonal changes, or other systemic conditions requiring comprehensive medical assessment. Varicose-like changes in scalp vessels, while rare, can occur in certain vascular malformations or conditions affecting venous return that may require specialized vascular evaluation. The sudden appearance of dark, twisted vessels or vascular lesions could indicate more serious conditions such as arteriovenous malformations or certain types of skin cancer that require immediate medical attention. Changes in vascular patterns, particularly when accompanied by pain, pulsation, bleeding, or rapid growth, should prompt urgent medical consultation. Healthcare providers can perform appropriate vascular assessments, imaging studies when necessary, and coordinate with specialists to ensure proper diagnosis and management of underlying vascular conditions affecting scalp health.
9. Growths, Bumps, and Nodules - Identifying Concerning Scalp Lesions
The development of new growths, bumps, or nodules on the scalp represents one of the most important changes requiring immediate medical evaluation, as these lesions can range from benign sebaceous cysts to serious malignancies requiring prompt treatment. The scalp's rich hair follicle density and sebaceous gland concentration make it susceptible to various types of growths that may initially appear innocuous but require professional assessment to determine their nature and appropriate management. Sebaceous cysts, while generally benign, can become infected, rupture, or in rare cases, undergo malignant transformation, necessitating proper evaluation and sometimes surgical removal. Lipomas, or fatty tumors, typically feel soft and mobile but require confirmation through physical examination and sometimes imaging to differentiate from other soft tissue masses. More concerning are firm, fixed, or rapidly growing lesions that could indicate skin cancers such as basal cell carcinoma, squamous cell carcinoma, or melanoma, which require immediate biopsy and treatment to prevent metastasis and preserve life. The ABCDE criteria—Asymmetry, Border irregularity, Color variation, Diameter greater than 6mm, and Evolution or change over time—help identify potentially malignant lesions requiring urgent medical attention. Additionally, lesions that bleed spontaneously, ulcerate, or cause significant pain warrant immediate evaluation regardless of their appearance, as these characteristics often indicate aggressive or malignant processes requiring prompt intervention.
10. Hair Follicle Abnormalities - Beyond Simple Hair Loss

While hair loss itself is common and often benign, specific abnormalities in hair follicle appearance and function can indicate underlying dermatological or systemic conditions that require medical attention and targeted treatment approaches. Folliculitis, or inflammation of hair follicles, presents as small red bumps or pustules around individual hairs and can result from bacterial, fungal, or viral infections requiring specific antimicrobial therapy. Keratosis pilaris on the scalp, characterized by small, rough bumps around hair follicles, may indicate underlying genetic conditions or vitamin deficiencies requiring nutritional assessment and management. Trichostasis spinulosa, where multiple hair shafts emerge from single follicles, can indicate hormonal imbalances or certain genetic conditions affecting hair growth patterns. Follicular hyperkeratosis, presenting as thickened, rough areas around follicles, may suggest vitamin A deficiency, certain autoimmune conditions, or chronic inflammatory processes requiring comprehensive evaluation and treatment. Perifollicular erythema or inflammation extending beyond individual follicles could indicate autoimmune conditions such as lupus or dermatomyositis that require systemic treatment and monitoring. The presence of follicular scarring, where hair follicles appear permanently damaged or absent, may indicate scarring alopecia conditions that require immediate intervention to prevent progressive hair loss and scalp damage. These follicular abnormalities often provide early clues to systemic conditions, making their recognition and proper medical evaluation crucial for both scalp health and overall wellness.
11. Pain and Neurological Symptoms - When Your Scalp Hurts

Scalp pain and neurological symptoms represent concerning changes that can significantly impact quality of life while indicating various underlying conditions requiring medical evaluation and management. Unlike temporary discomfort from tight hairstyles or minor trauma, persistent or severe scalp pain may indicate inflammatory conditions, nerve dysfunction, vascular abnormalities, or systemic diseases requiring targeted treatment approaches. Trigeminal neuralgia affecting scalp branches can cause severe, shooting pains triggered by light touch or movement, requiring specialized neurological evaluation and often prescription medications for effective management. Temporal arteritis, particularly concerning in older adults, can cause severe scalp tenderness along with systemic symptoms and requires immediate medical attention to prevent serious complications including vision loss. Occipital neuralgia presents as sharp, shooting pains in the back of the head and upper neck, often requiring nerve blocks or other specialized treatments for relief. Burning scalp syndrome, characterized by persistent burning sensations without visible changes, may indicate nerve dysfunction, hormonal imbalances, or psychological stress requiring comprehensive evaluation and multidisciplinary management. Tingling, numbness, or altered sensation in scalp areas could indicate nerve compression, vitamin deficiencies, or systemic conditions affecting peripheral nerves. The presence of scalp pain accompanied by fever, visual changes, jaw pain, or other systemic symptoms requires immediate medical evaluation to rule out serious conditions such as temporal arteritis, meningitis, or other inflammatory conditions requiring urgent treatment.
12. Photosensitivity and Sun-Related Changes - When Light Becomes the Enemy

Increased scalp photosensitivity and unusual sun-related changes can indicate various underlying conditions, medication effects, or genetic disorders that require medical evaluation and protective management strategies. While some degree of sun sensitivity is normal, particularly in fair-skinned individuals, sudden onset or severe photosensitivity may indicate autoimmune conditions such as lupus, dermatomyositis, or certain genetic disorders affecting DNA repair mechanisms. Medication-induced photosensitivity from antibiotics, diuretics, or other common medications can cause severe scalp burning, blistering, or hyperpigmentation with minimal sun exposure, requiring medication review and sun protection counseling. Polymorphous light eruption affecting the scalp presents as itchy bumps or blisters following sun exposure and may require prescription treatments and strict photoprotection measures. Solar keratoses, or precancerous lesions resulting from chronic sun damage, appear as rough, scaly patches that require medical evaluation and often treatment to prevent progression to skin cancer. The development of unusual pigmentation patterns, persistent redness, or textural changes following sun exposure may indicate photodamage requiring dermatological assessment and possibly biopsy to rule out malignancy. Individuals with certain genetic conditions such as xeroderma pigmentosum require specialized management and extreme photoprotection to prevent severe complications. Healthcare providers can assess photosensitivity patterns, review medications, recommend appropriate photoprotection measures, and when necessary, perform patch testing or other evaluations to identify specific triggers and implement effective management strategies.
13. Integrating Scalp Health into Comprehensive Healthcare