10 Posture Patterns Linked to Musculoskeletal Conditions
In our increasingly sedentary world, the human body has become a victim of modern lifestyle demands, with postural deviations emerging as silent architects of widespread musculoskeletal dysfunction. Recent biomechanical research reveals that approximately 80% of adults will experience significant back pain during their lifetime, with postural abnormalities serving as primary contributing factors to this epidemic. The intricate relationship between posture and musculoskeletal health extends far beyond simple alignment issues, encompassing complex neurological, biomechanical, and physiological processes that influence everything from joint loading patterns to muscle activation sequences. Contemporary studies utilizing advanced motion analysis technology and electromyography have identified specific postural patterns that consistently correlate with distinct musculoskeletal conditions, creating predictable pathways from poor alignment to chronic pain and dysfunction. Understanding these connections provides healthcare professionals and individuals with powerful tools for prevention, early intervention, and targeted treatment strategies. This comprehensive analysis examines ten critical postural patterns that research has definitively linked to musculoskeletal conditions, exploring the underlying mechanisms, clinical presentations, and evidence-based interventions that can break the cycle of postural dysfunction and restore optimal movement patterns for long-term musculoskeletal health.
1. Forward Head Posture - The Digital Age Epidemic

Forward head posture (FHP) has emerged as one of the most prevalent postural deviations in modern society, characterized by the anterior translation of the head relative to the cervical spine's optimal alignment. Research indicates that for every inch the head moves forward from its ideal position, the effective weight bearing down on the cervical spine increases by approximately 10-15 pounds, creating exponential stress on the delicate structures of the neck and upper thoracic region. This postural pattern, often called "text neck" or "computer neck," results from prolonged periods of looking down at electronic devices or maintaining forward head positioning during desk work. The biomechanical consequences are far-reaching, as FHP creates compensatory muscle imbalances where the deep cervical flexors become inhibited and lengthened, while the upper cervical extensors, suboccipitals, and upper trapezius muscles become hyperactive and shortened. Clinical studies have consistently linked FHP to cervicogenic headaches, temporomandibular joint dysfunction, cervical disc degeneration, and thoracic outlet syndrome. The altered cervical lordosis associated with FHP also affects the entire kinetic chain, potentially contributing to shoulder impingement, upper crossed syndrome, and even lower back pain through compensatory mechanisms. Intervention strategies focusing on deep cervical flexor strengthening, posterior cervical muscle stretching, and ergonomic modifications have shown significant success in reversing FHP and reducing associated symptoms.
2. Rounded Shoulder Syndrome - The Collapse of Upper Body Architecture

Rounded shoulder syndrome represents a complex postural deviation where the shoulders assume a protracted and internally rotated position, fundamentally altering the biomechanics of the entire upper extremity and thoracic region. This condition, increasingly common in populations engaged in prolonged computer work, driving, or activities requiring sustained forward reaching, creates a cascade of muscular imbalances that extend throughout the kinetic chain. The primary characteristics include shortening and tightening of the pectoralis major and minor, anterior deltoid, and internal rotators, while the middle and lower trapezius, rhomboids, and posterior deltoid become lengthened and weakened. Research utilizing three-dimensional motion analysis has demonstrated that rounded shoulders significantly reduce glenohumeral joint space, increase the risk of subacromial impingement, and alter scapulothoracic rhythm during overhead movements. The condition is strongly associated with rotator cuff pathology, adhesive capsulitis, and chronic neck pain due to compensatory cervical extension. Furthermore, the thoracic kyphosis that often accompanies rounded shoulders can compromise respiratory function by reducing chest expansion capacity and altering diaphragmatic mechanics. Clinical studies have shown that individuals with rounded shoulder posture demonstrate decreased shoulder external rotation strength by up to 25% compared to those with normal alignment. Comprehensive treatment approaches incorporating posterior chain strengthening, anterior structure mobilization, and postural re-education have proven effective in restoring optimal shoulder positioning and preventing associated pathologies.
3. Hyperkyphosis - When the Spine Curves Beyond Normal Limits
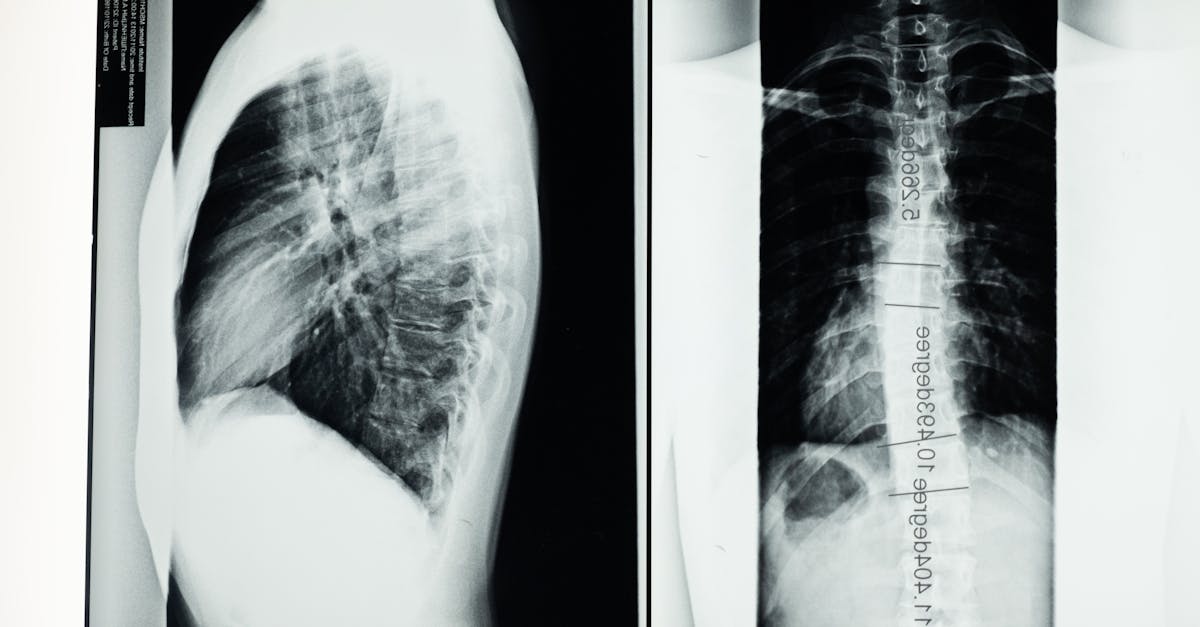
Thoracic hyperkyphosis, commonly referred to as excessive upper back curvature or "hunchback," represents a significant postural deviation that profoundly impacts both structural integrity and functional capacity of the spine. Normal thoracic kyphosis ranges between 20-40 degrees, but when this curvature exceeds 50 degrees, it creates substantial biomechanical dysfunction and increases the risk of multiple musculoskeletal conditions. Research has identified both structural and postural forms of hyperkyphosis, with the latter being more responsive to conservative intervention. The condition results from a combination of factors including prolonged flexed posturing, osteoporotic vertebral compression fractures, muscle imbalances, and genetic predisposition. Biomechanical studies reveal that excessive thoracic kyphosis significantly increases compressive forces on anterior vertebral bodies while creating excessive tension in posterior spinal structures, leading to accelerated disc degeneration and facet joint arthritis. The postural consequences extend beyond the thoracic region, as hyperkyphosis typically triggers compensatory cervical hyperextension and lumbar hyperlordosis to maintain horizontal gaze and overall balance. Clinical research has established strong correlations between thoracic hyperkyphosis and reduced pulmonary function, with severe cases showing up to 30% reduction in vital capacity due to chest wall restrictions. Additionally, individuals with hyperkyphosis demonstrate increased fall risk, reduced quality of life scores, and higher rates of vertebral fractures. Evidence-based interventions focusing on thoracic extension mobility, postural muscle strengthening, and spinal alignment awareness have shown remarkable success in reducing kyphotic angles and improving associated symptoms.
4. Anterior Pelvic Tilt - The Foundation of Lower Body Dysfunction
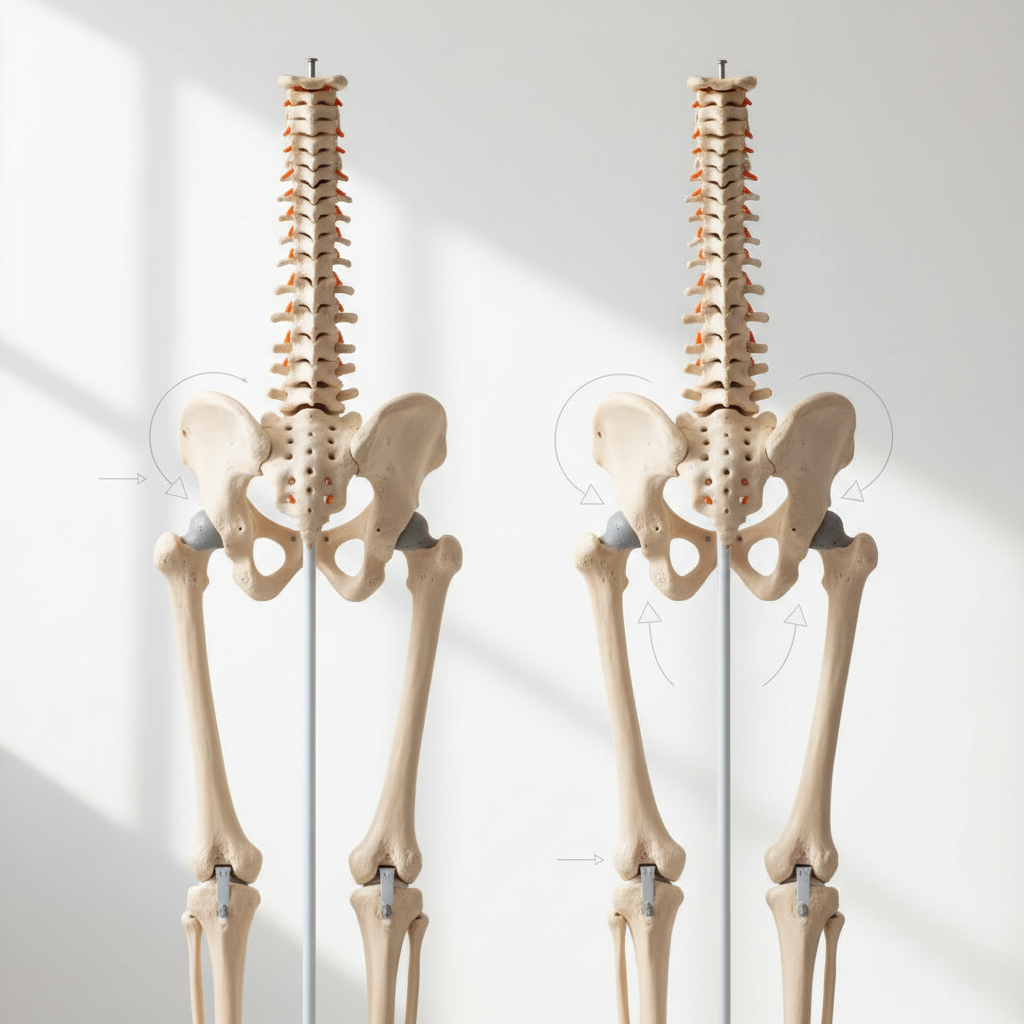
Anterior pelvic tilt (APT) represents a fundamental postural deviation where the pelvis rotates forward, creating excessive lumbar lordosis and establishing a foundation for numerous lower extremity and spinal pathologies. This condition, characterized by the anterior superior iliac spines positioning lower than the posterior superior iliac spines, affects an estimated 85% of males and 75% of females to varying degrees, making it one of the most common postural abnormalities observed in clinical practice. The biomechanical implications of APT are extensive, as it creates predictable muscle imbalances including tightness in the hip flexors (particularly the iliopsoas), rectus femoris, and lumbar erectors, while simultaneously weakening the gluteus maximus, hamstrings, and deep abdominal muscles. Research utilizing electromyographic analysis has demonstrated that APT significantly alters muscle activation patterns during functional movements, leading to compensatory strategies that increase injury risk and reduce movement efficiency. The condition is strongly associated with lumbar disc herniation, facet joint syndrome, sacroiliac joint dysfunction, and hip impingement due to the altered biomechanics it creates throughout the lumbopelvic region. Clinical studies have shown that individuals with significant APT demonstrate up to 40% reduction in gluteus maximus activation during hip extension activities, contributing to the development of gluteal amnesia and subsequent kinetic chain dysfunction. Furthermore, APT affects gait mechanics, creating increased lumbar extension moments during walking and running, which can accelerate degenerative changes in the lumbar spine. Comprehensive treatment protocols addressing hip flexor flexibility, core stabilization, and posterior chain strengthening have proven highly effective in correcting APT and preventing associated pathologies.
5. Lateral Pelvic Tilt - The Asymmetrical Foundation
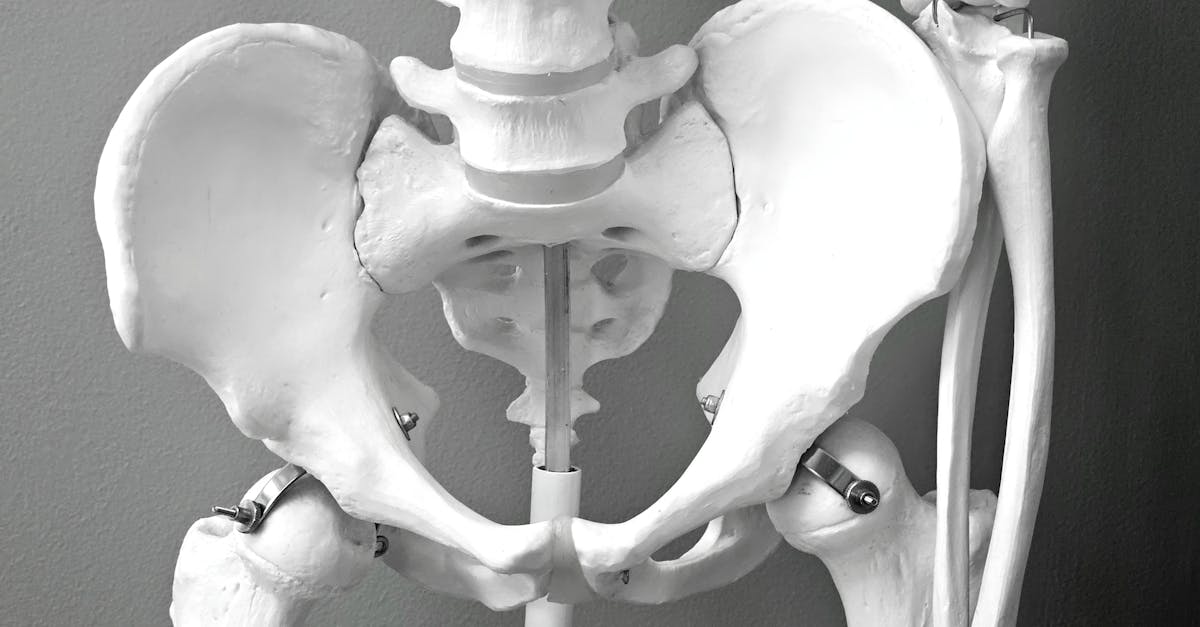
Lateral pelvic tilt, characterized by one side of the pelvis being higher than the other when viewed from behind, represents a common postural asymmetry that creates significant biomechanical dysfunction throughout the kinetic chain. This condition, also known as pelvic obliquity, can result from structural leg length discrepancies, functional imbalances, or habitual asymmetrical positioning patterns such as consistently carrying weight on one side or standing with weight shifted to one leg. Research indicates that even small degrees of lateral pelvic tilt (as little as 5-10 degrees) can create substantial compensatory changes in spinal alignment, hip mechanics, and lower extremity function. The biomechanical consequences include altered weight distribution through the lumbar spine, creating increased compressive forces on the concave side and tensile stress on the convex side of the resulting lumbar scoliotic curve. Clinical studies have demonstrated strong correlations between lateral pelvic tilt and the development of lumbar disc pathology, sacroiliac joint dysfunction, and hip labral tears due to the altered joint loading patterns. The condition also affects the entire lower extremity kinetic chain, with the elevated side typically demonstrating hip adduction and internal rotation, while the lower side shows compensatory hip abduction and external rotation. Gait analysis reveals that individuals with lateral pelvic tilt exhibit asymmetrical ground reaction forces, altered step lengths, and compensatory trunk movements that can contribute to overuse injuries. Furthermore, the asymmetrical muscle activation patterns associated with lateral pelvic tilt can lead to unilateral muscle weakness and tightness, perpetuating the postural deviation and increasing the risk of injury during athletic activities or daily functional tasks.
6. Lumbar Hyperlordosis - The Exaggerated Lower Back Curve

Lumbar hyperlordosis, characterized by excessive inward curvature of the lower back, represents a significant postural deviation that fundamentally alters spinal biomechanics and contributes to numerous musculoskeletal pathologies. While normal lumbar lordosis ranges between 40-60 degrees, hyperlordosis occurs when this curvature exceeds normal limits, often as a compensatory mechanism for anterior pelvic tilt or thoracic hyperkyphosis. Research utilizing advanced imaging techniques has revealed that excessive lumbar lordosis significantly increases posterior element loading, particularly affecting the facet joints, ligamentum flavum, and posterior annular fibers of intervertebral discs. The condition creates predictable muscle imbalances, with the hip flexors, lumbar erectors, and quadratus lumborum becoming shortened and overactive, while the deep abdominal muscles, gluteus maximus, and hamstrings become lengthened and inhibited. Clinical studies have established strong correlations between lumbar hyperlordosis and the development of facet joint arthritis, spinal stenosis, spondylolysis, and spondylolisthesis, particularly in the L4-L5 and L5-S1 segments where lordotic stress is greatest. The biomechanical alterations associated with hyperlordosis also affect hip joint mechanics, creating anterior femoral glide and predisposing individuals to hip impingement and labral pathology. Furthermore, the exaggerated lumbar curve can compromise core stability by placing the diaphragm and pelvic floor in suboptimal positions, reducing their ability to contribute to intra-abdominal pressure and spinal stabilization. Electromyographic research has shown that individuals with hyperlordosis demonstrate altered muscle activation patterns during functional movements, with delayed or reduced activation of key stabilizing muscles, increasing the risk of acute injury and chronic pain development.
7. Flat Back Syndrome - The Loss of Natural Spinal Curves

Flat back syndrome, characterized by the loss or reversal of normal lumbar lordosis, represents a complex postural condition that significantly impacts spinal biomechanics and functional capacity. This condition, which can be developmental, degenerative, or iatrogenic (resulting from surgical interventions), creates a rigid, straight appearance to the lumbar spine when viewed from the side, fundamentally altering the spine's natural shock-absorbing capacity and load distribution mechanisms. Research has identified multiple etiologies for flat back syndrome, including ankylosing spondylitis, degenerative disc disease, previous spinal fusion surgeries, and chronic hip flexor contractures that prevent normal pelvic positioning. The biomechanical consequences are profound, as the loss of lumbar lordosis shifts the body's center of gravity forward, requiring compensatory mechanisms throughout the kinetic chain to maintain upright posture and balance. Clinical studies have demonstrated that individuals with flat back syndrome experience significantly increased energy expenditure during walking and standing activities due to the muscular effort required to maintain erect posture against gravitational forces. The condition is associated with chronic low back pain, hip flexor contractures, knee hyperextension, and thoracic hyperkyphosis as the body attempts to compensate for the altered spinal alignment. Furthermore, flat back syndrome can lead to sagittal imbalance, where the individual cannot maintain an upright posture without significant muscular effort, resulting in forward stooping and progressive functional decline. Advanced imaging studies reveal that the loss of lumbar lordosis increases disc pressure by up to 300% compared to normal alignment, accelerating degenerative changes and increasing the risk of disc herniation and vertebral compression fractures.
8. Sway Back Posture - The Posterior Displacement Pattern
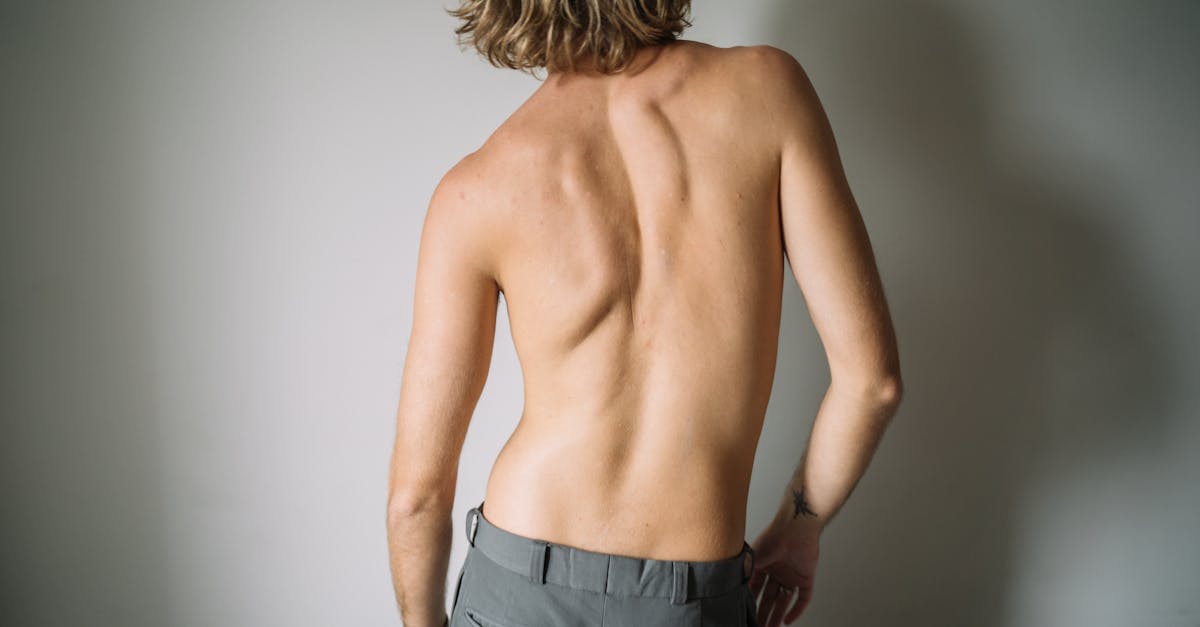
Sway back posture represents a unique postural deviation characterized by a posterior displacement of the thoracic spine relative to the pelvis, creating a distinctive "S" curve when viewed from the side. This condition, also known as posterior displacement syndrome, involves a combination of thoracic kyphosis, posterior pelvic tilt, and hip extension, resulting in the hips being positioned anterior to the ankles and the thoracic spine posterior to the hips. Research indicates that sway back posture often develops as a compensation for prolonged standing or as a result of muscle imbalances affecting the entire posterior chain. The biomechanical implications are complex, as this posture creates altered loading patterns throughout the spine and lower extremities, with increased stress on the thoracolumbar junction and altered hip joint mechanics. Clinical studies have identified specific muscle imbalances associated with sway back posture, including tightness in the hamstrings, upper abdominals, and neck extensors, combined with weakness in the hip flexors, lower abdominals, and neck flexors. The condition is frequently associated with thoracolumbar pain, hip flexor weakness, and cervical dysfunction due to the compensatory forward head posture that often accompanies the thoracic posterior displacement. Furthermore, individuals with sway back posture demonstrate altered movement patterns during functional activities, with reduced hip flexion range of motion and compensatory lumbar flexion during forward bending tasks. The postural deviation can also affect respiratory function by altering the position and function of the diaphragm and accessory breathing muscles, potentially contributing to reduced exercise tolerance and increased fatigue during physical activities.
9. Knee Valgus - The Inward Collapse Pattern
Knee valgus, characterized by the inward angulation of the knees toward the midline, represents a significant postural and movement pattern dysfunction that affects both static alignment and dynamic movement quality. This condition, commonly observed during weight-bearing activities such as squatting, landing, and single-leg stance, creates substantial biomechanical stress throughout the lower extremity kinetic chain and is strongly associated with increased injury risk, particularly anterior cruciate ligament (ACL) tears and patellofemoral pain syndrome. Research utilizing three-dimensional motion analysis has identified multiple contributing factors to knee valgus, including hip abductor weakness, gluteus medius dysfunction, ankle mobility restrictions, and altered neuromuscular control patterns. The biomechanical consequences of knee valgus extend beyond the knee joint itself, creating altered loading patterns at the hip, patellofemoral joint, and ankle complex. Clinical studies have demonstrated that excessive knee valgus increases lateral patellofemoral contact pressure by up to 45%, contributing to cartilage degeneration and chronic pain. Furthermore, the condition affects the entire lower extremity alignment, often accompanied by femoral internal rotation, tibial external rotation, and foot pronation, creating a predictable pattern of dysfunction known as lower crossed syndrome. Electromyographic research has revealed that individuals with knee valgus demonstrate reduced gluteus medius and gluteus maximus activation during functional movements, combined with increased tensor fasciae latae and quadriceps dominance. The postural implications of knee valgus extend to standing alignment, where chronic valgus positioning can lead to adaptive shortening of the iliotibial band, lateral retinaculum, and hip adductors, while creating compensatory lengthening and weakness in the hip abductors and external rotators.
10. Foot Pronation and Supination Patterns - The Ground-Up Effect
Foot posture abnormalities, particularly excessive pronation and supination patterns, represent fundamental postural deviations that create far-reaching effects throughout the entire kinetic chain due to the foot's role as the primary interface between the body and ground. Excessive pronation, characterized by flattening of the medial longitudinal arch, calcaneal eversion, and forefoot abduction, affects approximately 20-25% of the population and creates significant biomechanical dysfunction during weight-bearing activities. Conversely, excessive supination, involving high arches, calcaneal inversion, and reduced shock absorption capacity, affects a smaller but significant portion of the population and creates its own unique set of compensatory patterns. Research utilizing pressure plate analysis and three-dimensional gait analysis has revealed that abnormal foot posture significantly alters ground reaction forces and joint loading patterns throughout the lower extremity. Excessive pronation creates internal rotation moments that travel proximally through the kinetic chain, contributing to tibial internal rotation, knee valgus, femoral internal rotation, and anterior pelvic tilt. Clinical studies have established strong correlations between excessive pronation and the development of plantar fasciitis, posterior tibial tendon dysfunction, medial knee pain, and hip internal rotation syndrome. Conversely, excessive supination reduces the foot's natural shock absorption capacity, increasing the transmission of impact forces to proximal structures and contributing to lateral ankle instability, iliotibial band syndrome, and stress fractures. The postural implications extend beyond the lower extremity, as altered foot mechanics can influence pelvic positioning, spinal alignment, and even upper extremity function through compensatory mechanisms. Furthermore, research has