10 Nail Changes That May Indicate an Underlying Health Issue
Your fingernails and toenails serve as remarkable windows into your overall health, functioning as diagnostic tools that can reveal underlying medical conditions long before other symptoms manifest. These seemingly simple keratin structures undergo continuous growth and renewal, making them sensitive barometers of your body's internal state. Changes in nail color, texture, shape, and growth patterns can signal everything from nutritional deficiencies and circulatory problems to serious systemic diseases and autoimmune disorders. Medical professionals have long recognized the diagnostic value of nail examination, with certain nail abnormalities being so characteristic of specific conditions that they bear the names of the physicians who first described them. Understanding these subtle yet significant changes can empower individuals to seek timely medical attention, potentially leading to earlier diagnosis and treatment of serious health issues. This comprehensive exploration will examine ten critical nail changes that warrant medical evaluation, providing you with the knowledge to recognize when your nails might be signaling that something deeper requires attention.
1. Clubbing - When Fingertips Bulge and Curve

Nail clubbing represents one of the most significant nail changes that can indicate serious underlying health conditions, particularly those affecting the cardiovascular and respiratory systems. This condition manifests as an enlargement and rounding of the fingertips, accompanied by nails that curve downward and appear to "float" on the nail bed. The angle between the nail and the cuticle, normally around 160 degrees, increases to 180 degrees or more in clubbing cases. This phenomenon occurs due to increased blood flow and tissue growth in the fingertips, often resulting from chronic low oxygen levels in the blood. Lung diseases such as lung cancer, chronic obstructive pulmonary disease (COPD), pulmonary fibrosis, and bronchiectasis are common causes of clubbing. Additionally, heart conditions including congenital heart disease, endocarditis, and certain congenital abnormalities can trigger this nail change. Liver disease, inflammatory bowel disease, and thyroid disorders may also manifest through nail clubbing. The development of clubbing is typically gradual, occurring over months or years, and while it can sometimes be hereditary and benign, new-onset clubbing in adults almost always warrants immediate medical investigation to rule out serious underlying pathology.
2. Spoon Nails (Koilonychia) - Concave Depressions Signal Iron Deficiency

Spoon nails, medically termed koilonychia, present as a distinctive nail deformity where the nails become thin, brittle, and develop a characteristic concave or spoon-like depression that can actually hold a drop of water. This condition most commonly affects the fingernails, though toenails can also be involved, and represents a classic sign of iron deficiency anemia. The nail plate becomes so thin and weak that it loses its normal convex curve and instead curves inward, creating the telltale spoon shape. Iron deficiency anemia occurs when the body lacks sufficient iron to produce healthy red blood cells, leading to decreased oxygen delivery to tissues throughout the body, including the nail matrix where nail growth occurs. This oxygen deprivation affects the normal keratinization process, resulting in the production of abnormally thin and weak nail plates. Beyond iron deficiency, spoon nails can also indicate other conditions such as hemochromatosis (iron overload), Raynaud's disease, lupus, and certain thyroid disorders. In some cases, spoon nails may result from repeated exposure to petroleum-based solvents or trauma. While mild spooning can occasionally be normal in infants and young children, persistent or progressive koilonychia in adults typically requires comprehensive evaluation including complete blood count, iron studies, and assessment for underlying causes of iron deficiency such as gastrointestinal bleeding or malabsorption disorders.
3. Beau's Lines - Horizontal Ridges Reveal Systemic Stress

Beau's lines appear as distinct horizontal ridges or grooves that run across the width of the nail, creating visible depressions that can be felt when running a finger over the nail surface. These lines represent temporary interruptions in nail growth caused by severe physiological stress or illness that affects the entire body. The nail matrix, responsible for producing new nail cells, becomes temporarily disrupted during periods of significant systemic stress, illness, or nutritional deficiency, resulting in the formation of these characteristic horizontal depressions. The timing of the underlying condition can often be estimated by measuring the distance of the Beau's line from the cuticle, as fingernails grow approximately 3 millimeters per month. Common causes include severe infections, high fever, major surgery, chemotherapy, severe malnutrition, uncontrolled diabetes, peripheral vascular disease, and zinc deficiency. Psychological stress, while significant, typically does not cause Beau's lines unless accompanied by physical manifestations such as poor nutrition or illness. Multiple Beau's lines may indicate repeated episodes of systemic stress or ongoing chronic conditions. In severe cases, the nail growth interruption can be so complete that the nail may actually separate from the nail bed, a condition called onychomadesis. The appearance of Beau's lines across multiple nails simultaneously strongly suggests a systemic rather than local cause, warranting medical evaluation to identify and address the underlying condition that triggered this nail growth disruption.
4. Yellow Nail Syndrome - Respiratory and Lymphatic Connections

Yellow nail syndrome represents a rare but distinctive condition characterized by thick, yellow, slow-growing nails that often lack cuticles and may separate from the nail bed. This syndrome typically affects all twenty nails and is frequently associated with respiratory conditions and lymphatic system abnormalities. The nails in yellow nail syndrome grow at an abnormally slow rate, sometimes taking six months or longer to grow what would normally take two months, and they develop a characteristic golden-yellow to greenish-yellow coloration. The nail plate becomes significantly thickened and may develop a curved or "humped" appearance, while the cuticles often disappear entirely. This condition is most commonly associated with chronic respiratory conditions such as chronic sinusitis, bronchiectasis, pleural effusions, and chronic cough. Lymphatic abnormalities, including lymphedema and lymphatic drainage problems, are also frequently observed in patients with yellow nail syndrome. The exact mechanism linking these nail changes to respiratory and lymphatic conditions remains unclear, but theories suggest impaired lymphatic drainage may affect nail growth and appearance. Some cases have been associated with autoimmune conditions, thyroid disorders, and certain medications including penicillamine and bucillamine. While yellow nail syndrome can sometimes resolve spontaneously, treatment typically focuses on addressing the underlying respiratory or lymphatic conditions, with some patients benefiting from vitamin E supplementation, which may help improve nail growth and appearance.
5. Terry's Nails - Liver Disease and Aging Indicators

Terry's nails present as a distinctive nail abnormality where the majority of the nail plate appears white or pale pink, with only a narrow band of normal pink color remaining at the tip near the free edge. This condition, first described by Dr. Richard Terry in 1954, affects the nail bed rather than the nail plate itself, creating the characteristic "ground glass" appearance that obscures the normal pink color of the nail bed. The white or opaque appearance results from changes in the nail bed's blood supply and the underlying connective tissue structure. Terry's nails are most commonly associated with liver disease, particularly cirrhosis, where they may be present in up to 80% of patients with severe liver dysfunction. The mechanism is believed to involve decreased albumin production by the diseased liver, leading to fluid retention and changes in the nail bed's vascular architecture. However, Terry's nails are not exclusively associated with liver disease and can also occur in patients with congestive heart failure, diabetes mellitus, chronic kidney disease, and malnutrition. Additionally, this nail change becomes increasingly common with advanced age, affecting up to 25% of individuals over 40 years old, though the age-related occurrence is typically less pronounced than disease-related cases. The presence of Terry's nails, especially when they develop suddenly or are accompanied by other symptoms, warrants medical evaluation to assess liver function and screen for other potential underlying conditions.
6. Pitting and Nail Psoriasis - Autoimmune Manifestations
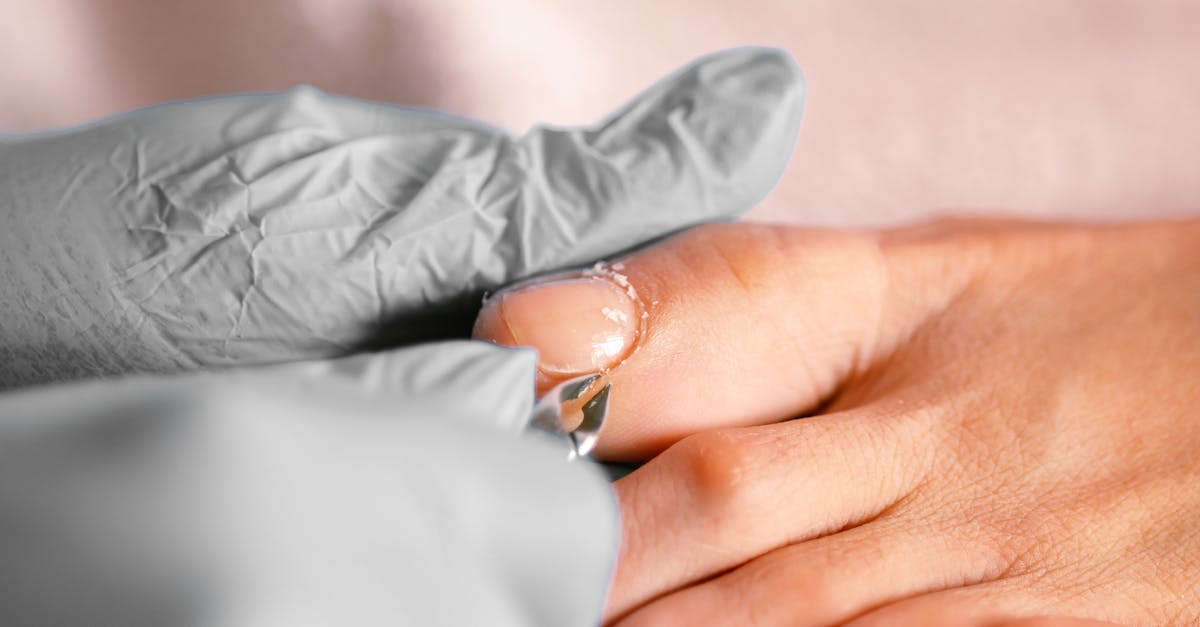
Nail pitting appears as small, punctate depressions scattered across the nail surface, resembling the surface of a thimble or the skin of an orange. These tiny holes or dents in the nail plate result from localized defects in nail formation within the nail matrix, where inflammatory processes disrupt the normal keratinization process. Nail pitting is most commonly associated with psoriasis, affecting approximately 50% of individuals with this autoimmune skin condition, and up to 80% of those with psoriatic arthritis. The pitting pattern in psoriasis can vary from fine, superficial depressions to deeper, more irregular holes, and may be accompanied by other nail changes such as onycholysis (nail separation), subungual hyperkeratosis (thickening under the nail), and oil drop discoloration. Beyond psoriasis, nail pitting can also occur in other autoimmune and inflammatory conditions including alopecia areata, where it may affect up to 46% of patients, eczema, lichen planus, and reactive arthritis. The severity and pattern of pitting can sometimes help differentiate between these conditions, with psoriatic pitting typically being more irregular and deeper compared to the fine, uniform pitting often seen in alopecia areata. In some cases, nail pitting may be the first or only manifestation of psoriasis, appearing years before skin lesions develop. The presence of nail pitting, especially when accompanied by joint pain, skin changes, or hair loss, should prompt evaluation for underlying autoimmune conditions, as early diagnosis and treatment can help prevent progression and complications.
7. Melanonychia - Dark Streaks and Cancer Concerns
Melanonychia refers to brown or black pigmentation of the nail, which can appear as diffuse discoloration or as distinct longitudinal bands running from the cuticle to the free edge of the nail. This pigmentation results from increased melanin production by melanocytes in the nail matrix or nail bed, and while it can be benign, it may also indicate serious conditions including melanoma. Longitudinal melanonychia, presenting as dark vertical bands, is more common in individuals with darker skin tones and can be a normal variant, particularly when it affects multiple nails symmetrically. However, new-onset melanonychia in fair-skinned individuals, or changes in existing pigmented bands, require careful evaluation to rule out subungual melanoma, a potentially deadly form of skin cancer that accounts for 1-3% of all melanomas. Warning signs include irregular borders, color variation within the band, width greater than 3 millimeters, extension of pigmentation onto the surrounding skin (Hutchinson's sign), and involvement of a single digit, particularly the thumb or great toe. Benign causes of melanonychia include trauma, certain medications (such as antimalarials, chemotherapy agents, and antimicrobials), endocrine disorders, nutritional deficiencies, and inflammatory conditions. Ethnic melanonychia, common in individuals of African, Asian, or Hispanic descent, typically presents as multiple uniform bands that remain stable over time. Any new or changing melanonychia, especially in light-skinned individuals or when accompanied by nail dystrophy, pain, or bleeding, requires prompt dermatological evaluation and possible biopsy to exclude malignancy.
8. Half-and-Half Nails - Kidney Disease Markers

Half-and-half nails, also known as Lindsay's nails, present a distinctive appearance where the proximal portion of the nail (closest to the cuticle) appears white or pale, while the distal portion (toward the tip) maintains a normal pink or reddish-brown coloration. This striking bicolor pattern typically affects all fingernails and creates a clear demarcation line roughly halfway across the nail plate. The condition was first described by Dr. P.G. Lindsay in 1967 in patients with chronic kidney disease, and it remains most strongly associated with chronic renal failure and uremia. The pathophysiology involves changes in the nail bed's vascular supply and possibly the accumulation of uremic toxins that affect nail bed coloration. Studies indicate that half-and-half nails occur in approximately 20-50% of patients with chronic kidney disease, with prevalence increasing as kidney function declines. The white proximal portion is thought to result from decreased blood flow and edema in the nail bed, while the preserved distal coloration reflects areas with better vascular perfusion. While chronic kidney disease remains the primary association, half-and-half nails can occasionally be seen in other conditions including liver disease, heart failure, HIV infection, Kawasaki disease, and zinc deficiency. The presence of half-and-half nails, particularly when they develop acutely or are accompanied by other symptoms such as swelling, fatigue, or changes in urination, should prompt evaluation of kidney function through blood tests including creatinine, blood urea nitrogen, and estimated glomerular filtration rate.
9. Leukonychia - White Spots and Systemic Conditions
Leukonychia refers to white discoloration of the nails, which can manifest in several distinct patterns, each potentially indicating different underlying conditions. True leukonychia involves white coloration of the nail plate itself, while apparent leukonychia results from changes in the nail bed that create a white appearance through the translucent nail plate. Punctate leukonychia, the most common form, appears as small white spots scattered across the nail surface and is typically caused by minor trauma to the nail matrix during nail growth. These traumatic white spots are generally benign and grow out with the nail over several months. However, more extensive forms of leukonychia can indicate serious systemic conditions. Total leukonychia, where the entire nail appears white, can be hereditary or acquired, with acquired cases potentially signaling liver disease, kidney disease, or protein deficiency. Transverse leukonychia presents as horizontal white bands across the nail and may indicate acute illness, chemotherapy, or arsenic poisoning. Mees' lines, a specific type of transverse leukonychia, appear as single or multiple white bands and are classically associated with arsenic poisoning, though they can also occur with other heavy metal toxicity, severe illness, or chemotherapy. Partial leukonychia may be associated with heart failure, liver disease, diabetes, or hyperthyroidism. The pattern, extent, and timing of leukonychia development can provide valuable diagnostic clues, with sudden onset or progressive white discoloration warranting medical evaluation to assess for underlying systemic disease, nutritional deficiencies, or toxic exposures.
10. Nail Texture Changes - Ridging and Surface Abnormalities

Nail texture abnormalities encompass a range of surface changes that can provide important clues about underlying health conditions, nutritional status, and systemic diseases. Longitudinal ridging, appearing as vertical lines running from cuticle to nail tip, becomes increasingly common with age and is often considered a normal part of aging, though pronounced ridging may indicate underlying conditions such as rheumatoid arthritis, peripheral vascular disease, or lichen planus. Transverse ridging, distinct from Beau's lines, presents as horizontal waves or corrugations across the nail surface and may result from repeated trauma, eczema, or systemic illness. Nail brittleness and splitting can indicate thyroid disorders, with both hyperthyroidism and hypothyroidism capable of causing nail fragility, though the mechanisms differ. Rough, sandpaper-like nail texture may suggest alopecia areata, psoriasis, or lichen planus, while smooth, shiny nails might indicate collagen vascular diseases or chronic malnutrition. Trachyonychia, or "twenty-nail dystrophy," presents as rough, opaque nails affecting all twenty nails and is associated with alopecia areata, psoriasis, lichen planus, and atopic dermatitis. Oil drop or salmon patch discoloration combined with texture changes strongly suggests psoriasis. Nail thickening (onychauxis) can result from trauma, fungal infections, psoriasis, or peripheral vascular disease, while nail thinning may indicate nutritional deficiencies, autoimmune conditions, or certain medications. The combination of texture changes with other nail abnormalities often provides more diagnostic information than isolated findings, emphasizing the importance of comprehensive nail examination in clinical assessment.
11. When to Seek Medical Attention - Red Flags and Professional Evaluation

Recognizing when nail changes warrant professional medical evaluation is crucial for early detection and treatment of potentially serious underlying conditions. Certain nail abnormalities should prompt immediate medical attention, including sudden onset of clubbing, new melanonychia in fair-skinned individuals, rapidly progressing nail changes, nail changes accompanied by pain or bleeding, and any nail abnormality associated with systemic symptoms such as fatigue, weight loss, or difficulty breathing. Progressive changes affecting multiple nails simultaneously often indicate systemic rather than local conditions and require comprehensive evaluation. Healthcare providers will typically conduct a thorough history focusing on the timeline of nail changes, associated symptoms, medications, occupational exposures, and family history of similar conditions. Physical examination extends beyond the nails to include assessment of skin, lymph nodes, heart, lungs, and other organ systems that might be related to the nail findings. Diagnostic testing may include complete blood count, comprehensive metabolic panel, liver function tests, thyroid studies, inflammatory markers, iron studies, and specific tests based on suspected conditions. In cases of suspected melanoma, dermoscopy and biopsy may be necessary. Fungal cultures might be obtained for suspected infections, while imaging studies could be indicated for suspected systemic diseases. The key is understanding that while many nail changes are benign and related to aging, trauma, or minor conditions, persistent, progressive, or concerning nail abnormalities often reflect the body's internal state and should not be ignored. Early medical evaluation allows for timely diagnosis and treatment of underlying conditions, potentially preventing complications and improving outcomes for serious diseases that might otherwise go undetected until more advanced stages.