10 Facial Skin Texture Patterns Linked to Hormonal and Autoimmune Conditions
The human face serves as a remarkable diagnostic window into our internal health, with skin texture patterns often revealing underlying hormonal imbalances and autoimmune conditions long before other symptoms manifest. Modern dermatological research has identified specific facial skin texture changes that correlate strongly with endocrine disruptions and immune system dysfunction, transforming how healthcare professionals approach early detection and treatment strategies. These textural variations—ranging from subtle changes in pore size and distribution to more pronounced alterations in skin thickness, elasticity, and surface irregularities—represent the complex interplay between hormonal fluctuations, inflammatory processes, and genetic predispositions. Understanding these patterns requires a multidisciplinary approach that combines dermatology, endocrinology, and immunology, as the skin's response to internal conditions involves intricate cellular mechanisms including collagen synthesis, sebaceous gland activity, and vascular changes. By recognizing these distinctive facial skin texture patterns, both medical professionals and individuals can gain valuable insights into potential underlying health conditions, enabling earlier intervention and more targeted treatment approaches that address root causes rather than merely surface symptoms.
1. Melasma and Hyperpigmentation Patterns in Hormonal Fluctuations
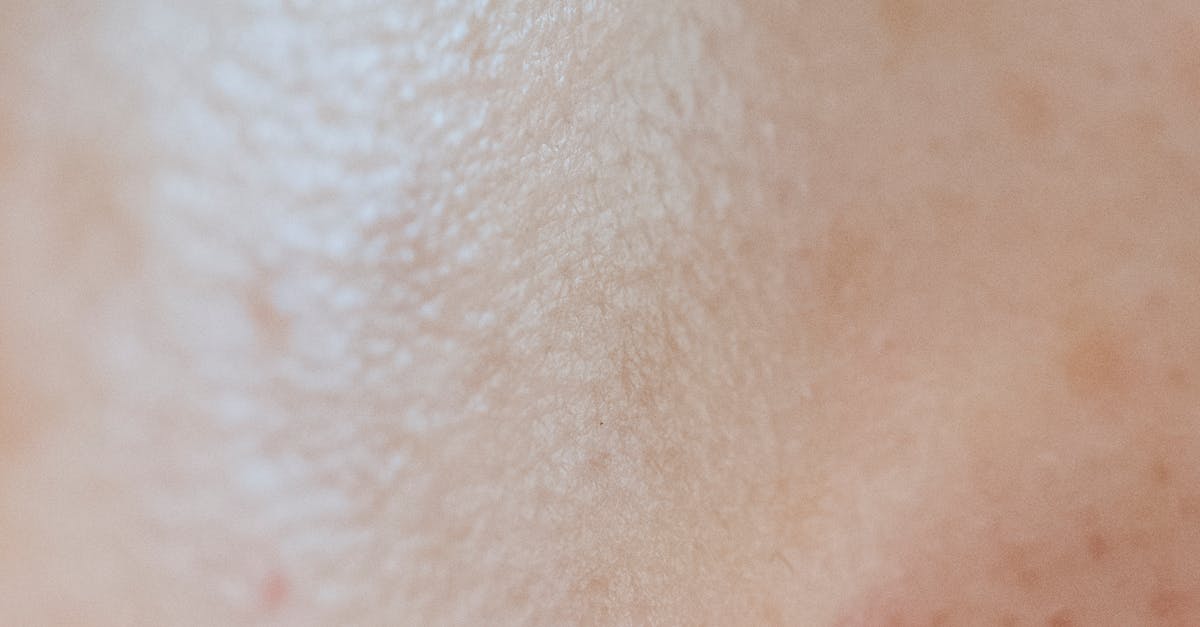
Melasma represents one of the most recognizable facial skin texture patterns associated with hormonal changes, particularly elevated estrogen and progesterone levels during pregnancy, oral contraceptive use, or hormone replacement therapy. This condition manifests as bilateral, symmetrical patches of hyperpigmentation typically appearing on the forehead, cheeks, bridge of the nose, and upper lip, creating a distinctive "mask of pregnancy" pattern that affects up to 90% of pregnant women. The underlying mechanism involves hormonal stimulation of melanocytes, the pigment-producing cells in the skin, leading to increased melanin production and deposition in both the epidermis and dermis. Research has shown that melasma patches often exhibit altered skin texture characteristics, including increased skin thickness, changes in dermal papillae structure, and modified collagen organization that can be detected through advanced imaging techniques such as reflectance confocal microscopy. The texture changes extend beyond visible pigmentation, with affected areas showing increased transepidermal water loss, altered pH levels, and modified sebaceous gland activity. These hormonal-induced textural modifications often persist even after pigmentation fades, suggesting permanent structural changes to the skin architecture. Understanding melasma's textural components is crucial for developing comprehensive treatment strategies that address both pigmentary and structural aspects of this hormonally-driven condition.
2. Acne Scarring Patterns and Androgen Sensitivity
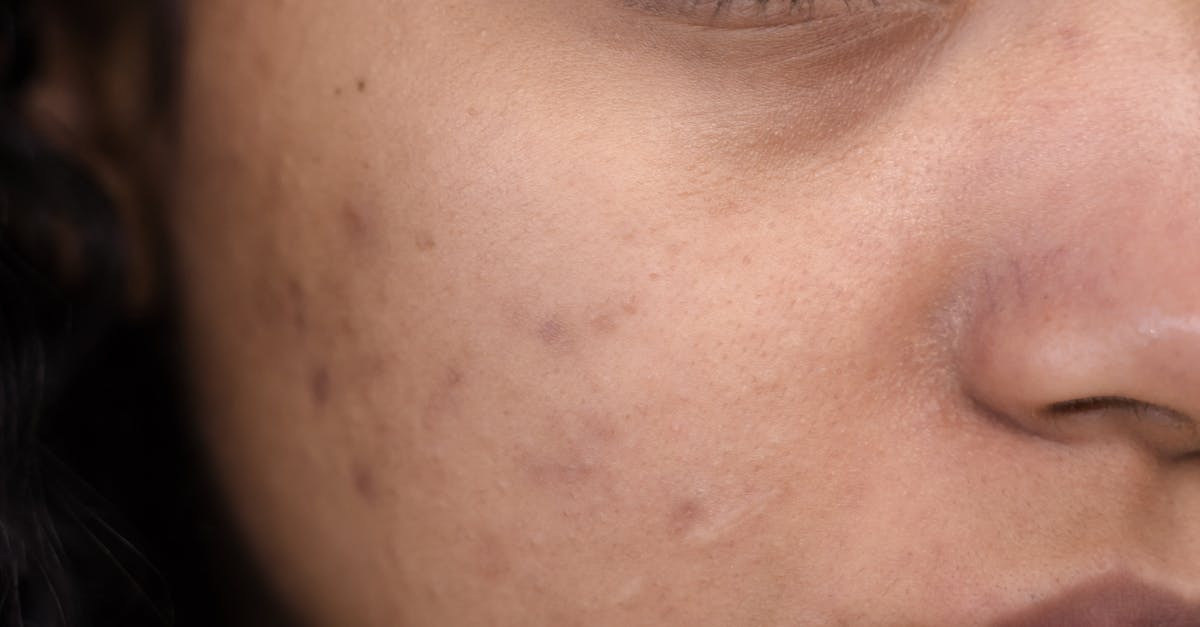
Androgenic hormones, particularly dihydrotestosterone (DHT) and testosterone, create distinctive facial skin texture patterns through their profound effects on sebaceous gland activity and follicular keratinization processes. Individuals with heightened androgen sensitivity often develop characteristic acne scarring patterns that reflect the underlying hormonal influence on skin structure and healing processes. These patterns typically manifest as ice-pick scars, boxcar scars, and rolling scars distributed primarily in the T-zone area, where sebaceous gland density is highest, creating a distinctive topographical landscape that correlates directly with androgen receptor distribution in facial skin. The textural changes extend beyond visible scarring to include enlarged pores, increased skin thickness in certain areas, and altered collagen remodeling patterns that can be quantified through dermatoscopic analysis and skin surface profilometry. Research has demonstrated that individuals with conditions such as polycystic ovary syndrome (PCOS) or congenital adrenal hyperplasia exhibit more severe and persistent acne scarring patterns due to chronically elevated androgen levels, which impair normal wound healing processes and promote excessive collagen degradation. The relationship between androgens and skin texture is further complicated by genetic variations in androgen receptor sensitivity, 5-alpha reductase activity, and aromatase expression, which influence individual susceptibility to hormonal skin changes. These androgen-related textural patterns serve as important clinical markers for underlying endocrine disorders and can guide both dermatological treatment and hormonal evaluation strategies.
3. Thyroid-Related Skin Texture Manifestations
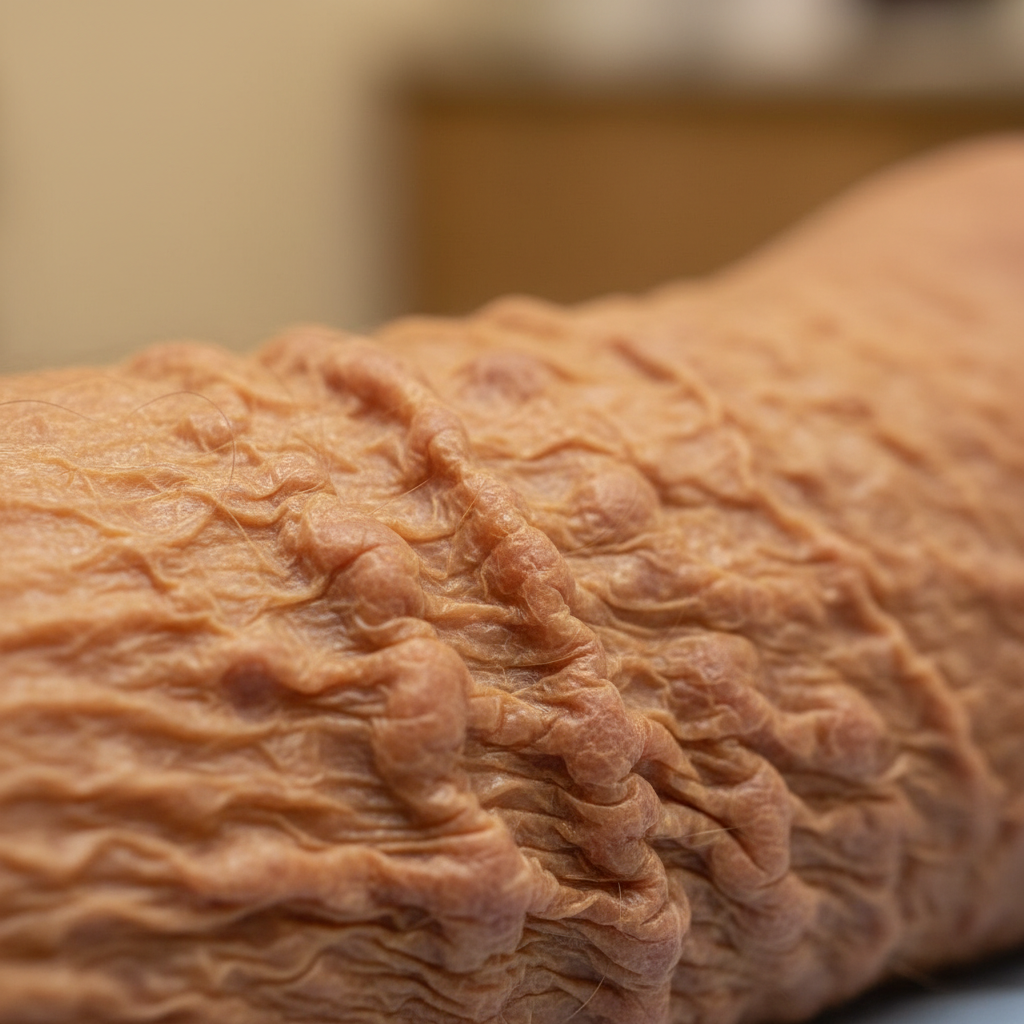
Thyroid dysfunction produces some of the most dramatic and recognizable changes in facial skin texture, with both hyperthyroidism and hypothyroidism creating distinct patterns that reflect the hormone's crucial role in cellular metabolism and skin barrier function. Hypothyroidism typically manifests as dry, coarse, and thickened facial skin with a characteristic waxy or doughy texture, particularly noticeable around the eyelids, cheeks, and jawline, where myxedematous changes can create a puffy, swollen appearance that obscures normal facial contours. The underlying pathophysiology involves decreased cellular turnover, reduced sebaceous gland activity, and accumulation of glycosaminoglycans in the dermis, leading to increased skin thickness and altered water-binding capacity. Conversely, hyperthyroidism produces fine, smooth, warm, and moist skin with increased vascularity that creates a characteristic flushed appearance and enhanced skin elasticity. Advanced imaging studies have revealed that thyroid-related skin texture changes involve modifications at multiple levels of skin architecture, including altered epidermal thickness, changes in dermal collagen organization, and modified vascular patterns that can be detected through techniques such as high-frequency ultrasound and optical coherence tomography. The temporal relationship between thyroid hormone levels and skin texture changes makes facial skin assessment a valuable tool for monitoring thyroid function and treatment response. These thyroid-induced textural modifications often precede other clinical symptoms by months, making dermatological examination an important component of endocrine screening protocols.
4. Autoimmune-Induced Inflammatory Skin Patterns
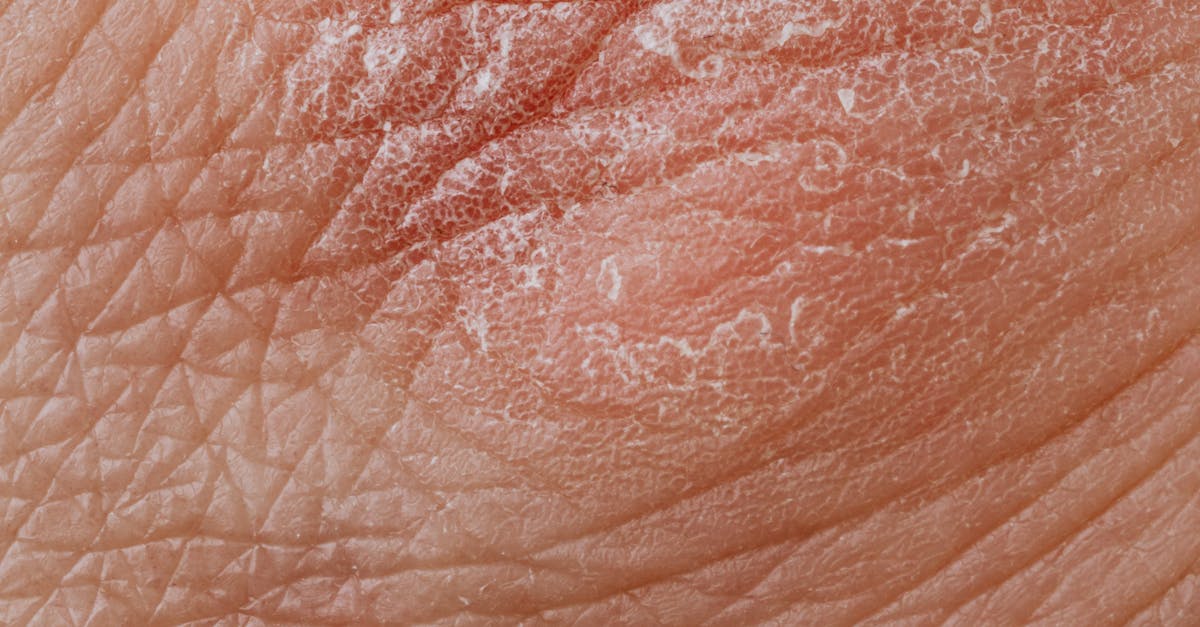
Autoimmune conditions create distinctive facial skin texture patterns characterized by chronic inflammation, altered barrier function, and immune-mediated tissue damage that manifests as specific textural signatures recognizable to trained clinicians. Systemic lupus erythematosus (SLE) produces the classic malar rash with associated skin texture changes including erythema, scaling, and in chronic cases, scarring and atrophy that creates a distinctive butterfly-shaped pattern across the cheeks and nasal bridge. The inflammatory process in autoimmune conditions involves complex interactions between activated immune cells, inflammatory mediators, and structural skin components, leading to disrupted collagen synthesis, increased matrix metalloproteinase activity, and compromised skin barrier function. Dermatomyositis presents with characteristic heliotrope rash around the eyelids accompanied by skin texture changes including edema, scaling, and eventual atrophy, while Gottron's papules create distinctive raised, scaly patches over the knuckles that extend to facial involvement in some cases. Research utilizing advanced histopathological techniques has revealed that autoimmune-related skin texture changes involve specific patterns of inflammatory cell infiltration, complement deposition, and basement membrane alterations that can be quantified through immunofluorescence studies and electron microscopy. The chronicity of autoimmune inflammation leads to progressive textural changes including skin thinning, telangiectasia formation, and altered pigmentation patterns that serve as important markers of disease activity and treatment response. Understanding these autoimmune-induced textural patterns is crucial for early diagnosis, disease monitoring, and development of targeted therapeutic interventions that address both inflammatory and structural components of skin involvement.
5. Insulin Resistance and Acanthosis Nigricans Texture Changes
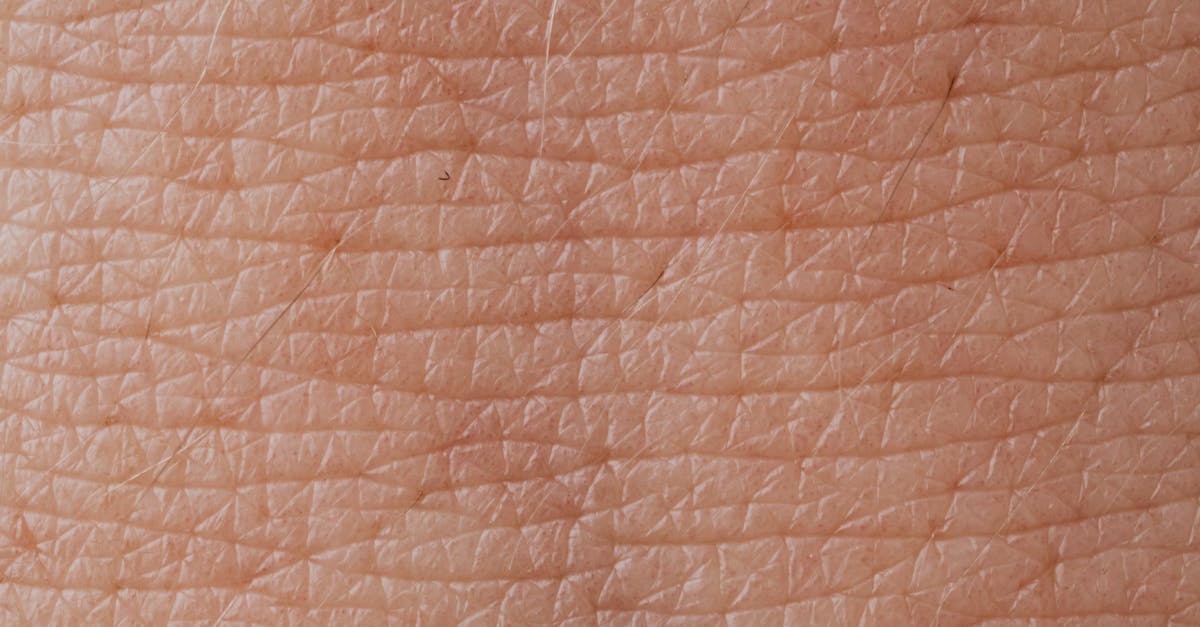
Insulin resistance creates distinctive facial skin texture patterns most notably exemplified by acanthosis nigricans, a condition characterized by hyperpigmented, velvety, papillomatous plaques that typically appear in flexural areas but can extend to facial regions, particularly around the neck, axillae, and inframammary areas. The pathophysiology involves insulin's binding to insulin-like growth factor receptors in keratinocytes and fibroblasts, stimulating cellular proliferation and creating the characteristic thickened, rough texture that feels distinctly different from normal skin. Advanced dermatoscopic examination reveals that acanthosis nigricans exhibits specific textural features including increased skin fold thickness, papillary surface irregularities, and altered reflectance properties that can be quantified through non-invasive imaging techniques. The condition serves as an important cutaneous marker of metabolic syndrome, with studies showing strong correlations between the severity of skin texture changes and degree of insulin resistance, making dermatological assessment a valuable screening tool for diabetes risk. Research has demonstrated that the textural changes in insulin resistance extend beyond visible acanthosis nigricans to include subtle modifications in skin elasticity, hydration levels, and barrier function that can be detected through biophysical measurements such as corneometry and cutometry. The relationship between insulin resistance and skin texture is further complicated by associated hormonal changes including elevated androgens and altered growth hormone levels, which contribute to additional textural modifications including increased sebaceous gland activity and altered collagen metabolism. These insulin-related textural patterns often improve with metabolic interventions, making skin texture assessment a useful marker for monitoring treatment response in patients with metabolic disorders.
6. Cortisol-Related Skin Atrophy and Striae Formation
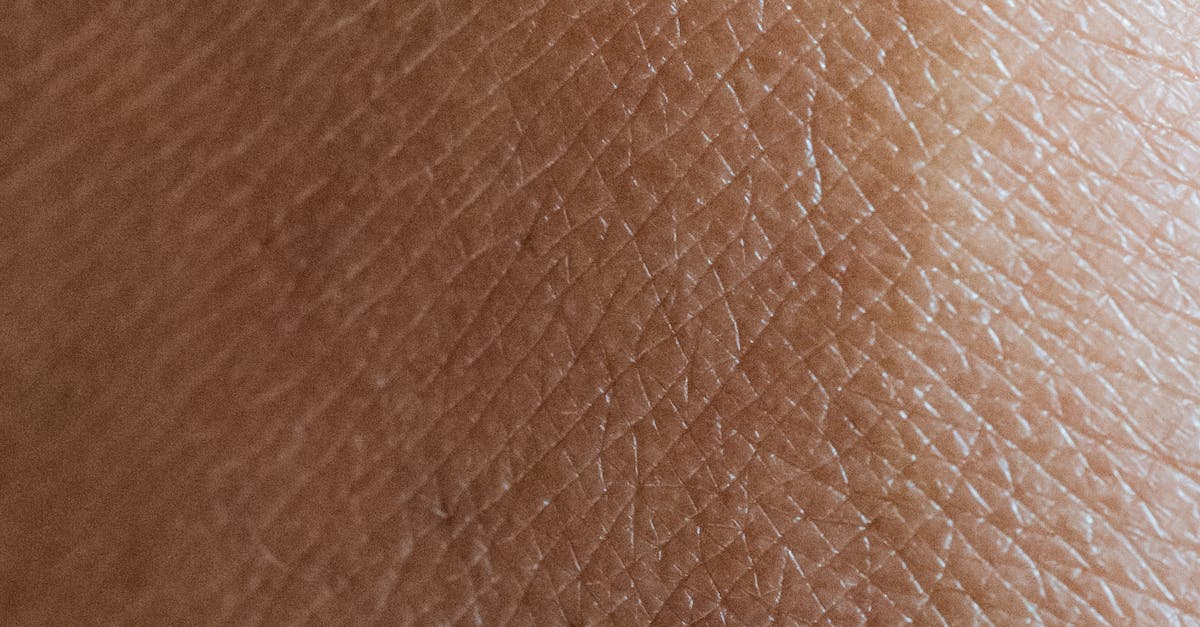
Chronic elevation of cortisol levels, whether from endogenous Cushing's syndrome or prolonged corticosteroid therapy, produces characteristic facial skin texture changes that reflect the hormone's profound effects on collagen synthesis, skin barrier function, and wound healing processes. The most recognizable pattern involves skin atrophy with associated thinning, increased fragility, and the development of striae that can appear on the face, particularly in areas of mechanical stress such as the lateral canthal regions and around the mouth. The underlying mechanism involves cortisol's inhibitory effects on fibroblast proliferation and collagen synthesis, leading to decreased dermal thickness, reduced tensile strength, and impaired skin barrier function that can be quantified through non-invasive techniques such as high-frequency ultrasound and transepidermal water loss measurements. Advanced histological studies have revealed that cortisol-induced skin changes involve specific alterations in collagen fiber organization, elastic fiber fragmentation, and reduced glycosaminoglycan content that contribute to the characteristic atrophic appearance and altered mechanical properties. The facial distribution of cortisol-related texture changes often follows specific patterns, with the central face showing more pronounced atrophy due to higher glucocorticoid receptor density in these regions, while the peripheral face may exhibit compensatory changes including increased vascular prominence and altered pigmentation. Research has demonstrated that cortisol-related skin texture changes can serve as important clinical markers for hypercortisolism, with quantitative assessment of skin thickness and elasticity providing objective measures for diagnosis and monitoring of treatment response. The reversibility of these textural changes varies depending on the duration and severity of cortisol exposure, with some structural modifications persisting even after hormone levels normalize, emphasizing the importance of early recognition and intervention.
7. Growth Hormone Deficiency and Skin Aging Patterns
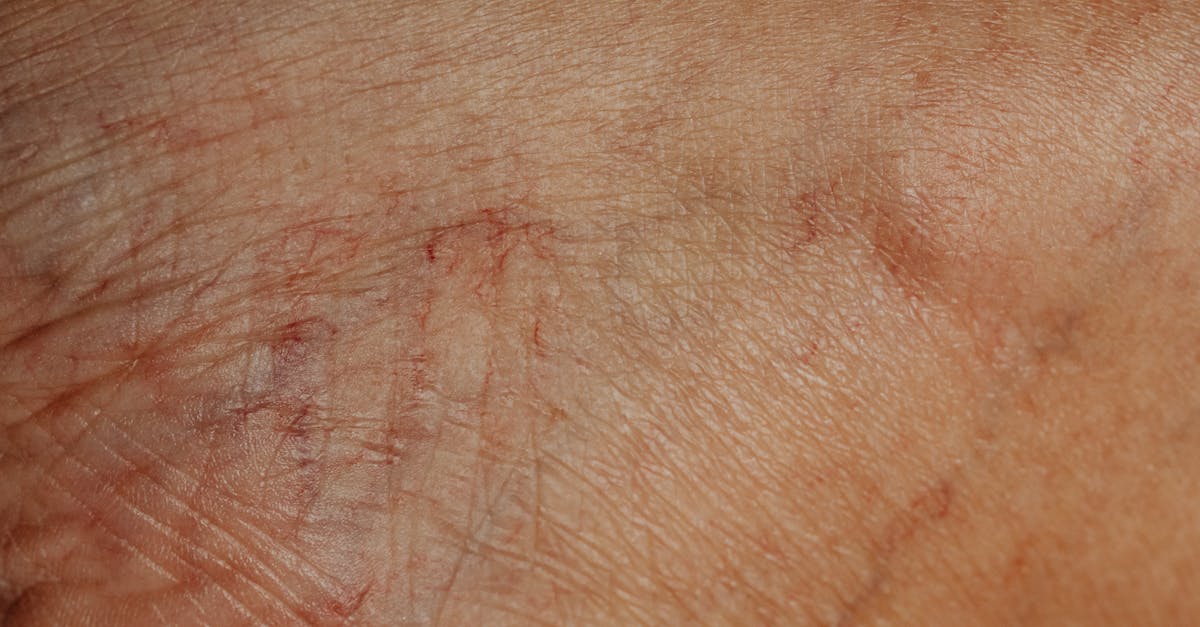
Growth hormone deficiency creates distinctive facial skin texture patterns that accelerate the appearance of aging and compromise skin structural integrity through complex effects on cellular metabolism, collagen synthesis, and skin barrier function. Individuals with growth hormone deficiency typically exhibit premature development of fine lines, decreased skin thickness, reduced elasticity, and altered hydration patterns that create a characteristic aged appearance disproportionate to chronological age. The pathophysiology involves growth hormone's crucial role in stimulating insulin-like growth factor-1 (IGF-1) production, which is essential for maintaining dermal thickness, promoting collagen synthesis, and supporting cellular regeneration processes throughout the skin. Advanced skin analysis techniques including optical coherence tomography and confocal microscopy have revealed that growth hormone deficiency leads to specific structural changes including reduced dermal thickness, altered collagen fiber organization, and decreased sebaceous gland activity that contribute to the characteristic dry, thin texture. The facial distribution of growth hormone-related texture changes often follows predictable patterns, with the periorbital and perioral regions showing the most pronounced effects due to the high metabolic demands of these areas and their sensitivity to growth factor deficiency. Research has demonstrated that growth hormone replacement therapy can partially reverse these textural changes, with improvements in skin thickness, hydration, and elasticity occurring within months of treatment initiation, making skin texture assessment a valuable marker for monitoring therapeutic response. The relationship between growth hormone and facial skin texture is further complicated by age-related decline in growth hormone secretion, which contributes to normal aging processes but can be distinguished from pathological deficiency through careful clinical assessment and biochemical testing.
8. Estrogen Deficiency and Collagen Degradation Patterns

Estrogen deficiency, particularly during menopause or in conditions causing premature ovarian failure, creates distinctive facial skin texture patterns characterized by accelerated collagen degradation, reduced skin thickness, and compromised barrier function that manifests as specific textural signatures. The decline in estrogen levels leads to decreased collagen synthesis, increased matrix metalloproteinase activity, and reduced hyaluronic acid production, resulting in skin that appears thinner, less elastic, and more prone to wrinkle formation, particularly in areas of repeated muscle movement such as around the eyes and mouth. Advanced research utilizing skin biopsy analysis and non-invasive imaging techniques has revealed that estrogen deficiency causes specific changes in collagen fiber architecture, with Type I collagen showing the most significant reduction and alterations in cross-linking patterns that compromise skin mechanical properties. The temporal relationship between estrogen decline and skin texture changes follows predictable patterns, with the most rapid changes occurring during the first five years after menopause when estrogen levels drop most dramatically, creating a characteristic acceleration in skin aging that can be quantified through objective measurements of skin thickness, elasticity, and hydration. Facial areas with higher estrogen receptor density, including the cheeks and forehead, often show more pronounced textural changes, while areas with lower receptor concentrations may exhibit more gradual modifications. The relationship between estrogen and skin texture is further complicated by individual variations in estrogen receptor sensitivity, aromatase activity, and genetic polymorphisms affecting hormone metabolism, which influence the severity and pattern of skin changes. Understanding these estrogen-related textural patterns is crucial for developing targeted interventions including hormone replacement therapy, topical estrogen applications, and alternative treatments that can help maintain skin structural integrity during hormonal transitions.
9. Vitamin D Deficiency and Skin Barrier Dysfunction

Vitamin D deficiency creates subtle but significant facial skin texture patterns that reflect the hormone's crucial role in skin barrier function, cellular differentiation, and immune regulation, with deficient individuals often exhibiting compromised skin integrity and altered textural characteristics. The active form of vitamin D, calcitriol, functions as a hormone that regulates keratinocyte proliferation and differentiation, influences sebaceous gland activity, and modulates inflammatory responses, making its deficiency a significant factor in various skin texture abnormalities. Research has demonstrated that vitamin D deficiency leads to impaired skin barrier function with increased transepidermal water loss, altered lipid composition in the stratum corneum, and modified desquamation patterns that create characteristic textural changes including dryness, roughness, and increased sensitivity to environmental factors. Advanced skin analysis techniques have revealed that vitamin D-deficient individuals exhibit specific changes in epidermal thickness, altered corneocyte morphology, and modified lipid bilayer organization that can be detected through techniques such as tape stripping analysis and confocal Raman spectroscopy. The facial distribution of vitamin D deficiency-related texture changes often affects sun-exposed areas paradoxically, as chronic sun avoidance behaviors that contribute to deficiency also prevent the normal adaptive responses that maintain skin health in these regions. Clinical studies have shown strong correlations between serum vitamin D levels and various skin texture parameters, including skin hydration, elasticity, and barrier function measurements, making dermatological assessment a potential screening tool for vitamin D status. The relationship between vitamin D and skin texture is further complicated by seasonal variations, geographic factors, and individual differences in vitamin D metabolism, which influence both deficiency risk and the severity of associated skin changes.
10. Polycystic Ovary Syndrome (PCOS) and Sebaceous Hyperplasia

Polycystic Ovary Syndrome (PCOS) creates distinctive facial skin texture patterns primarily through elevated androgen levels that stimulate sebaceous gland hyperplasia, alter keratinization processes, and promote inflammatory responses that manifest as characteristic textural changes across the face. Women with PCOS typically exhibit enlarged pores, increased skin thickness in the T-zone, persistent acne with associated scarring, and areas of sebaceous hyperplasia that create a distinctive bumpy, uneven texture particularly noticeable on the forehead, nose, and chin regions. The pathophysiology involves complex interactions between elevated testosterone and dihydrotestosterone levels, insulin resistance, and chronic low-grade inflammation that collectively disrupt normal skin homeostasis and create the characteristic PCOS skin phenotype. Advanced dermatological assessment techniques including dermoscopy and sebum measurement have revealed that PCOS-related skin changes involve specific alterations in sebaceous gland size and activity, follicular hyperkeratinization patterns, and inflammatory cell infiltration that can be quantified through objective measurements. The facial distribution of PCOS-related texture changes follows predictable anatomical patterns corresponding to androgen receptor density and sebaceous gland concentration, with the central face showing the most pronounced effects while the peripheral face may exhibit secondary changes related to chronic inflammation and altered barrier function. Research has demonstrated strong correlations between biochemical markers of PCOS including free testosterone levels, insulin resistance indices, and inflammatory markers with specific skin texture parameters, making dermatological assessment a valuable component of PCOS diagnosis and monitoring. The multifaceted nature of PCOS-related skin changes requires comprehensive treatment approaches that address hormonal imbalances, insulin sensitivity, and inflammatory processes to achieve optimal improvement in skin texture and overall dermatological health.
11. Clinical Applications and Future Diagnostic Potential
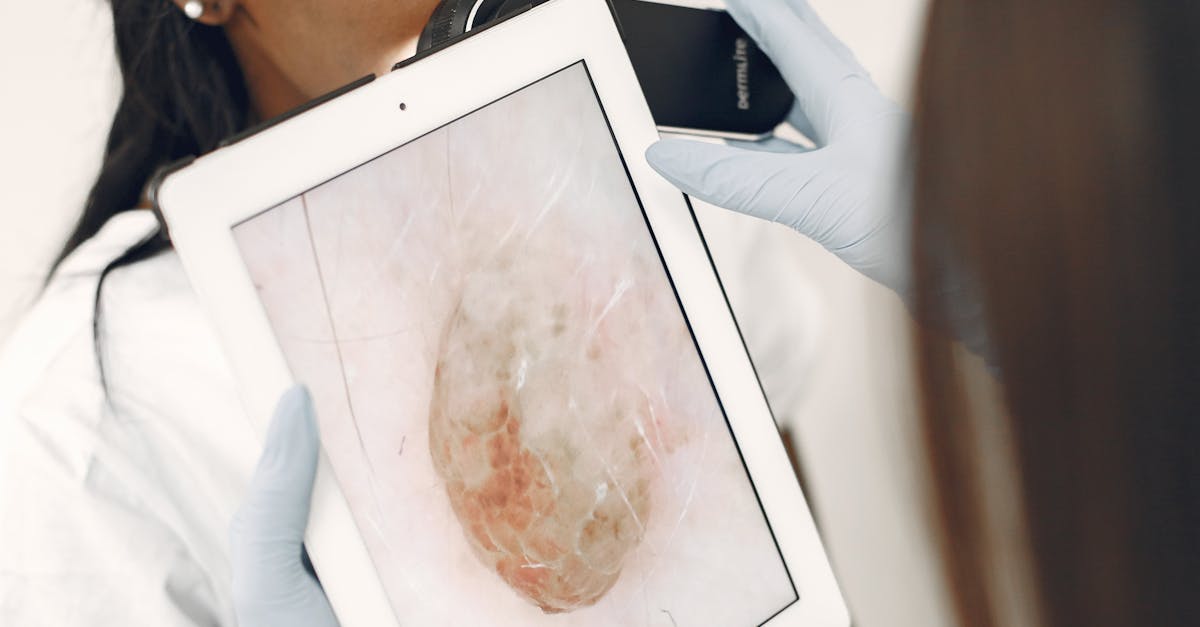
The recognition and systematic analysis of facial skin texture patterns linked to hormonal and autoimmune conditions represents a paradigm shift toward more holistic, non-invasive diagnostic approaches that leverage the skin's role as a window into systemic health. Modern dermatological practice increasingly incorporates advanced imaging technologies including optical coherence tomography, confocal microscopy, and artificial intelligence-powered skin analysis systems that can detect subtle textural changes before they become clinically apparent, enabling earlier intervention and improved patient outcomes. The development of standardized protocols for assessing facial skin texture patterns requires interdisciplinary collaboration between dermat