10 Eyelid Appearance Changes Associated With Autoimmune and Thyroid Conditions
The eyes have long been considered windows to the soul, but for medical professionals, they serve as crucial diagnostic portals that can reveal underlying systemic conditions affecting the entire body. The delicate structures surrounding the eyes, particularly the eyelids, are remarkably sensitive to hormonal fluctuations, immune system dysfunction, and metabolic changes that characterize autoimmune and thyroid disorders. These conditions, which affect millions of people worldwide, often manifest their earliest and most visible signs through subtle yet distinctive changes in eyelid appearance, texture, positioning, and function. From the inflammatory cascades triggered by autoimmune responses to the metabolic disruptions caused by thyroid hormone imbalances, these systemic conditions create a complex interplay of symptoms that frequently converge on the periorbital region. Understanding these eyelid manifestations is not merely an academic exercise—it represents a critical component of early diagnosis and comprehensive patient care. The following exploration delves into ten specific eyelid appearance changes that serve as important clinical indicators, each representing a unique intersection between systemic disease processes and their ocular manifestations, providing healthcare providers and patients alike with valuable insights into the intricate connections between eye health and overall systemic wellness.
1. Eyelid Retraction - The Hallmark of Thyroid Eye Disease

Eyelid retraction stands as one of the most characteristic and immediately recognizable signs of thyroid-related eye disease, particularly in cases of hyperthyroidism and Graves' disease. This condition manifests as an abnormal elevation of the upper eyelid, creating an appearance where more of the white sclera is visible above the iris than would typically be seen in healthy individuals. The underlying mechanism involves the overstimulation of Müller's muscle, a smooth muscle component of the upper eyelid that responds to sympathetic nervous system activation, which becomes hyperactive due to excessive thyroid hormone levels. Additionally, the inferior rectus muscle may become fibrotic and restricted, mechanically pulling the lower eyelid downward and contributing to the overall retracted appearance. Patients often describe a startled or surprised facial expression that they cannot control, and this change can be particularly distressing as it significantly alters their natural appearance. The severity of eyelid retraction can vary considerably, from subtle changes that are only noticeable to trained observers to dramatic presentations where the retraction is immediately apparent to anyone. This condition not only affects cosmetic appearance but can also lead to functional problems, including difficulty with complete eyelid closure, increased tear evaporation, and subsequent dry eye symptoms that can compromise corneal health and visual comfort.
2. Periorbital Edema - Inflammatory Swelling Around the Eyes
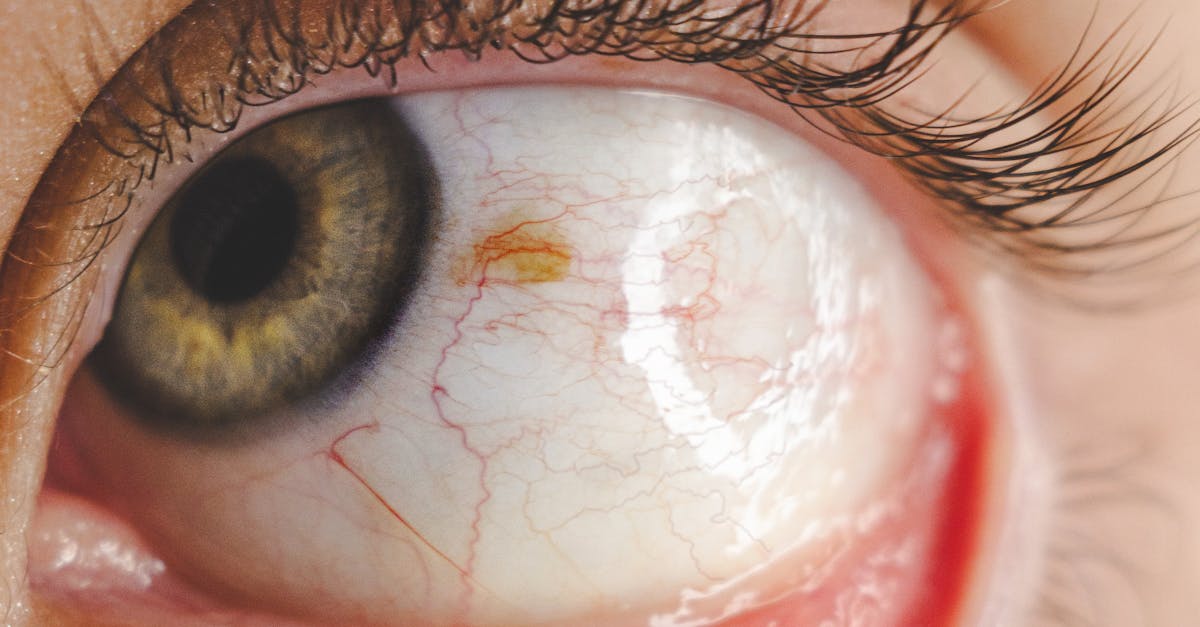
Periorbital edema represents a common and often early manifestation of both autoimmune conditions and thyroid disorders, characterized by fluid accumulation in the loose connective tissues surrounding the eyes. This swelling typically appears most prominently in the morning hours due to the effects of gravity and fluid redistribution during sleep, creating a puffy, swollen appearance that can range from mild to severe. In thyroid eye disease, the edema results from increased hyaluronic acid deposition and inflammatory infiltration within the orbital tissues, leading to increased tissue volume and subsequent fluid retention. Autoimmune conditions such as systemic lupus erythematosus, dermatomyositis, and various vasculitic disorders can also trigger periorbital edema through different mechanisms, including immune complex deposition, complement activation, and increased vascular permeability. The edema may be asymmetric, affecting one eye more than the other, or bilateral, involving both eyes equally. Patients often report that the swelling interferes with their ability to apply makeup, wear contact lenses, or even fully open their eyes in severe cases. The texture of the swollen tissue can provide diagnostic clues—thyroid-related edema often feels firm and non-pitting, while edema associated with certain autoimmune conditions may be softer and more compressible. Recognition of periorbital edema patterns can be crucial for early diagnosis and appropriate treatment initiation.
3. Eyelid Discoloration - Inflammatory and Metabolic Color Changes
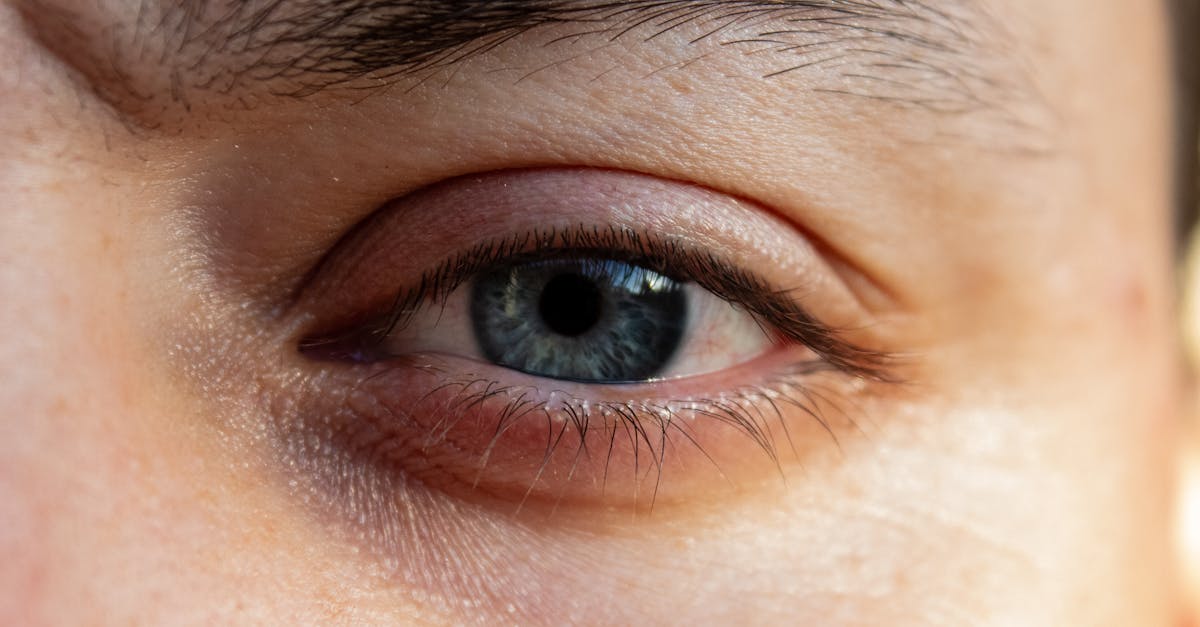
Distinctive color changes in the eyelids serve as important visual indicators of underlying autoimmune and thyroid conditions, reflecting the complex interplay between inflammation, vascular changes, and metabolic disruptions. In dermatomyositis, one of the most characteristic signs is the heliotrope rash, which presents as a distinctive purple or violet discoloration of the upper eyelids, often accompanied by periorbital edema. This pathognomonic sign results from inflammatory infiltration of the skin and underlying tissues, creating a color change that is virtually diagnostic of this autoimmune muscle disease. Thyroid disorders can also produce notable eyelid discoloration, though through different mechanisms. Hyperthyroidism may cause increased vascularity and a flushed appearance, while hypothyroidism can lead to a pale, yellowish tint due to carotenemia and reduced circulation. Some patients with autoimmune conditions develop hyperpigmentation around the eyes due to chronic inflammation and subsequent melanin deposition, creating darker patches that can be mistaken for cosmetic issues but actually represent systemic disease manifestations. The temporal pattern of these color changes can provide diagnostic clues—acute inflammatory conditions typically produce more vivid, rapidly developing discoloration, while chronic conditions may result in gradual, subtle changes that evolve over months or years. Understanding these color patterns helps differentiate between various conditions and guides appropriate diagnostic workup and treatment strategies.
4. Eyelid Thickening and Induration - Structural Changes from Chronic Inflammation
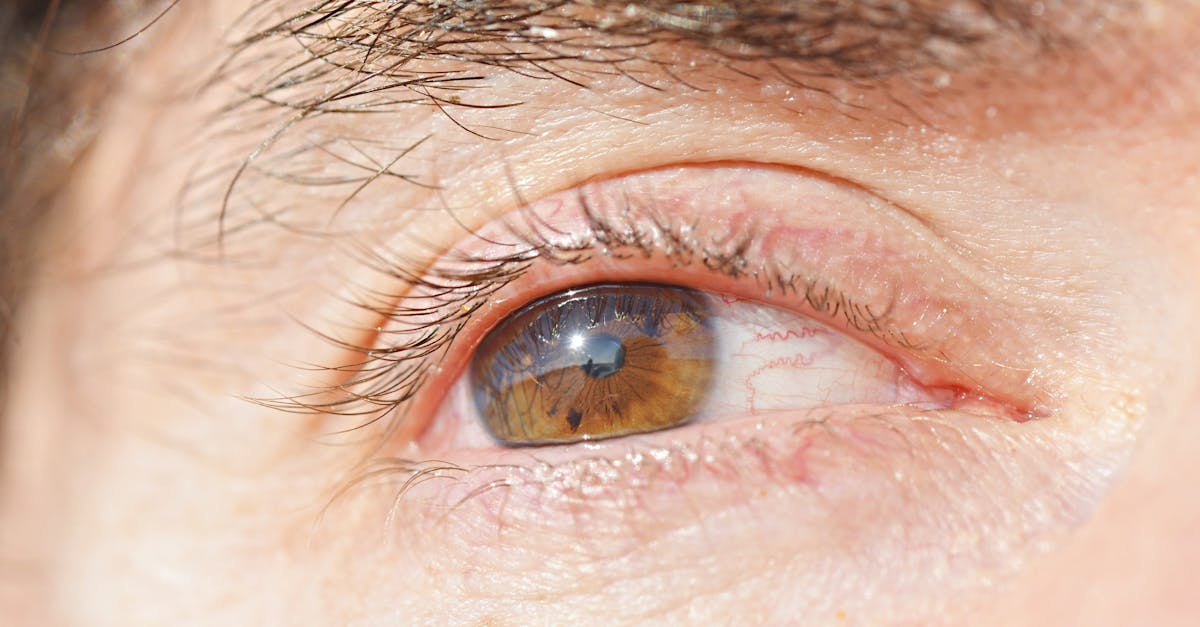
Chronic autoimmune and thyroid conditions frequently lead to significant structural changes in eyelid tissues, manifesting as thickening, induration, and altered texture that reflects ongoing inflammatory processes and tissue remodeling. In thyroid eye disease, the accumulation of glycosaminoglycans, particularly hyaluronic acid, within the eyelid tissues creates a characteristic thickening that gives the eyelids a heavy, swollen appearance that persists even when acute inflammation subsides. This process, known as tissue remodeling, involves the deposition of abnormal extracellular matrix components that alter the normal architecture of the eyelid structures. Autoimmune conditions such as scleroderma can cause progressive thickening and hardening of eyelid skin, leading to a tight, mask-like appearance that restricts normal eyelid mobility and expression. The thickening may be uniform across the entire eyelid or localized to specific areas, creating asymmetric appearances that can be both cosmetically and functionally significant. Patients often describe their eyelids as feeling heavy, tight, or uncomfortable, and may notice difficulty with normal blinking patterns or complete eyelid closure. The degree of thickening can serve as a marker of disease activity and progression, with more severe cases often correlating with greater systemic involvement. Palpation of the affected eyelids may reveal a firm, indurated texture that differs markedly from the normal soft, pliable feel of healthy eyelid tissue, providing important tactile diagnostic information for healthcare providers.
5. Ptosis - Drooping Eyelids from Muscle Weakness and Inflammation

Ptosis, characterized by abnormal drooping of one or both upper eyelids, represents a significant manifestation of various autoimmune conditions that affect neuromuscular function and eyelid support structures. Myasthenia gravis, an autoimmune disorder targeting acetylcholine receptors at the neuromuscular junction, commonly presents with ptosis as one of its earliest and most recognizable symptoms. The ptosis in myasthenia gravis typically demonstrates characteristic variability, worsening with sustained upward gaze or toward the end of the day when muscle fatigue is most pronounced, and improving with rest or the application of ice. This fluctuating nature helps distinguish myasthenic ptosis from other causes of eyelid drooping. Chronic progressive external ophthalmoplegia, another condition with autoimmune components, can also cause bilateral ptosis that develops gradually over time, often accompanied by limitations in eye movement. In thyroid eye disease, ptosis may develop secondary to superior rectus muscle fibrosis and restriction, or from mechanical factors related to eyelid swelling and inflammation. The degree of ptosis can range from barely perceptible to complete coverage of the pupil, significantly impacting visual function and requiring compensatory head positioning or eyebrow elevation to maintain adequate vision. Patients often develop characteristic facial expressions, including raised eyebrows and tilted head positions, as they attempt to compensate for the visual obstruction caused by the drooping eyelids.
6. Eyelash and Eyebrow Changes - Hair Loss and Texture Alterations
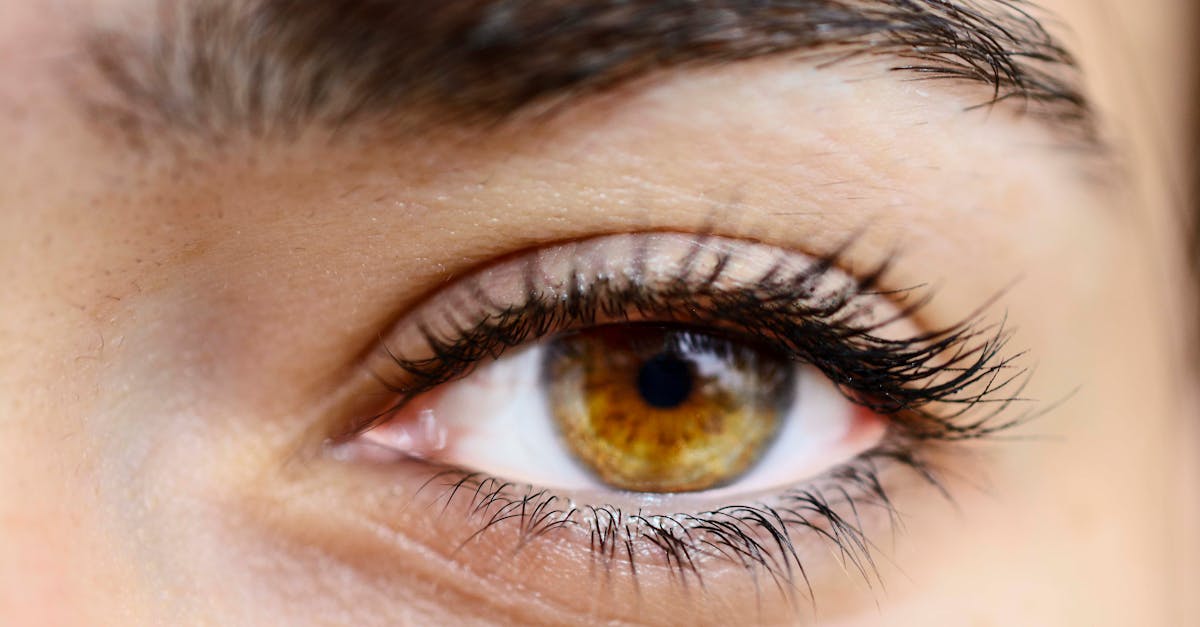
The hair follicles of the eyelashes and eyebrows are particularly sensitive to the hormonal and inflammatory changes associated with autoimmune and thyroid conditions, often serving as early indicators of systemic disease. Alopecia areata, an autoimmune condition targeting hair follicles, can cause patchy or complete loss of eyelashes and eyebrows, creating distinctive bare areas that can be psychologically distressing for patients. The hair loss typically occurs in well-demarcated patches and may be accompanied by characteristic "exclamation point" hairs at the borders of affected areas. Thyroid disorders significantly impact hair growth cycles, with hypothyroidism commonly causing thinning, brittle, and slow-growing eyelashes and eyebrows, while hyperthyroidism may lead to fine, fragile hair that breaks easily. The outer third of the eyebrows is particularly susceptible to thyroid-related hair loss, a finding known as the "Queen Anne sign" that has been recognized as a classic indicator of hypothyroidism. Systemic lupus erythematosus and other autoimmune conditions can cause diffuse hair thinning around the eyes, often accompanied by changes in hair texture and pigmentation. Some patients notice that their eyelashes become lighter in color, shorter, or grow in different directions than normal. These changes can significantly impact appearance and self-esteem, and may require specialized cosmetic approaches or medical treatments to address both the underlying condition and its aesthetic consequences.
7. Eyelid Erythema and Rash - Inflammatory Skin Manifestations
Inflammatory skin changes affecting the eyelids represent common and often diagnostically significant manifestations of various autoimmune conditions, presenting as erythema, rashes, and other distinctive dermatologic patterns. Systemic lupus erythematosus frequently involves the periorbital area as part of the characteristic malar rash, creating redness and inflammation that may extend from the cheeks to involve the lower eyelids and surrounding skin. The lupus-related eyelid erythema often demonstrates photosensitivity, becoming more pronounced after sun exposure and potentially leading to permanent pigmentation changes if left untreated. Contact dermatitis, which can be triggered by autoimmune hypersensitivity reactions, may cause acute eyelid swelling, redness, and vesicle formation, particularly in response to specific allergens or irritants. Seborrheic dermatitis, more common in patients with certain autoimmune conditions, creates characteristic scaling and erythema along the eyelid margins and eyebrow areas, often accompanied by itching and burning sensations. Rosacea, which has autoimmune components, can cause persistent redness and inflammatory papules around the eyes, leading to chronic discomfort and cosmetic concerns. The pattern, distribution, and associated symptoms of eyelid erythema can provide important diagnostic clues, helping to differentiate between various autoimmune conditions and guide appropriate treatment strategies. Some patients develop chronic, low-grade inflammation that creates a persistent pink or red tint to their eyelids, while others experience acute flares with intense erythema and associated symptoms.
8. Eyelid Tightness and Restricted Mobility - Fibrotic Changes and Contractures

Progressive fibrotic changes in eyelid tissues represent a significant long-term complication of chronic autoimmune and thyroid conditions, leading to tightness, restricted mobility, and functional impairment that can severely impact quality of life. Scleroderma, a connective tissue disorder with prominent autoimmune features, commonly affects the periorbital area, causing progressive thickening and tightening of the eyelid skin that can eventually restrict normal eyelid closure and opening. This process, known as sclerosis, involves the excessive deposition of collagen and other fibrous proteins within the skin and subcutaneous tissues, creating a leather-like texture and appearance that becomes increasingly rigid over time. In advanced thyroid eye disease, chronic inflammation can lead to fibrotic changes in the eyelid muscles and supporting structures, resulting in mechanical restrictions that limit normal eyelid movement and function. Patients often describe a sensation of tightness or pulling around their eyes, and may notice difficulty with facial expressions that involve eyelid movement, such as squinting or winking. The restriction can be asymmetric, affecting one eye more than the other, or bilateral, involving both eyes to varying degrees. Functional consequences may include incomplete eyelid closure during sleep, leading to corneal exposure and dry eye complications, or difficulty with normal blinking patterns that can affect tear distribution and eye comfort. Physical therapy and specialized exercises may help maintain some degree of mobility, but severe cases may require surgical intervention to restore function and prevent complications.
9. Eyelid Asymmetry - Unilateral Disease Manifestations
Asymmetric eyelid changes represent a particularly challenging aspect of autoimmune and thyroid-related eye disease, as unilateral or markedly asymmetric presentations can create significant cosmetic concerns and diagnostic complexity. Thyroid eye disease frequently affects one eye more severely than the other, leading to noticeable differences in eyelid position, swelling, and overall appearance that can be psychologically distressing for patients. The asymmetry may involve any combination of the previously described changes—one eyelid may be more retracted while the other appears normal, or one side may demonstrate significant swelling while the other remains relatively unaffected. Myasthenia gravis commonly presents with asymmetric ptosis, where one eyelid droops significantly more than the other, and this asymmetry may fluctuate throughout the day or with fatigue. Autoimmune conditions such as linear scleroderma can cause unilateral eyelid changes, creating a distinctive appearance where one side of the face appears normal while the other shows characteristic thickening, discoloration, or restriction. The psychological impact of eyelid asymmetry can be profound, as facial symmetry is closely associated with perceived attractiveness and normal social interaction. Patients may develop compensatory behaviors, such as tilting their head or adjusting their hair to minimize the appearance of asymmetry, and may experience significant anxiety or depression related to their altered appearance. Treatment approaches must address both the underlying medical condition and the cosmetic concerns, often requiring a multidisciplinary approach involving ophthalmologists, oculoplastic surgeons, and mental health professionals.
10. Eyelid Nodules and Masses - Inflammatory and Autoimmune Growths
The development of nodules, masses, or other growths on or within the eyelids can represent important manifestations of autoimmune conditions and their associated inflammatory processes. Rheumatoid arthritis can cause the formation of rheumatoid nodules around the eyes, presenting as firm, movable masses that may be tender or asymptomatic depending on their location and size. These nodules represent areas of chronic inflammation and tissue necrosis surrounded by inflammatory cells, and their presence often correlates with more severe systemic disease activity. Sarcoidosis, a multisystem inflammatory condition with autoimmune features, can cause granulomatous infiltration of eyelid tissues, leading to the formation of firm, non-tender nodules that may be skin-colored or slightly hyperpigmented. Chalazions and hordeolums may occur more frequently in patients with autoimmune conditions due to altered immune function and chronic inflammation of the meibomian glands, creating recurrent eyelid swellings that can become chronic and require medical or surgical intervention. Thyroid eye disease can occasionally cause the development of lacrimal gland enlargement or orbital masses that may be palpable through the upper eyelid, creating asymmetric swelling or fullness that differs from typical inflammatory edema. Some autoimmune conditions predispose patients to the development of certain types of eyelid malignancies, making careful evaluation and monitoring of any new growths particularly important. The characteristics of these masses—including their size, consistency, mobility, and associated symptoms—can provide important diagnostic information and help guide appropriate evaluation and treatment strategies.
11. Eyelid Texture Changes - Surface Alterations and Skin Quality

Subtle but significant changes in eyelid skin texture represent important indicators of underlying autoimmune and thyroid conditions, often providing early clues to systemic disease before more obvious symptoms develop. Hypothyroidism commonly causes characteristic skin changes that are particularly noticeable in the thin, delicate skin of the eyelids, including dryness, roughness, and a distinctive waxy or puffy texture that reflects underlying metabolic changes. The skin may feel thicker than normal and demonstrate reduced elasticity, with fine lines and wrinkles becoming more pronounced due to decreased collagen production and altered skin metabolism. Autoimmune conditions such as dermatomyositis can cause distinctive skin texture changes around the eyes, including a characteristic scaling or roughening that may be accompanied by the pathognomonic heliotrope rash. Scleroderma progressively alters skin texture, causing the eyelid skin to become increasingly tight, shiny, and leather-like as collagen deposition progresses and normal skin architecture is disrupted. Some patients with systemic lupus erythematosus develop chronic skin changes around the eyes, including areas of atrophy, hyperpigmentation, or hypopigmentation that create a mottled or uneven appearance. The rate of texture change can vary significantly between conditions and individuals—some changes develop rapidly over weeks or months, while others progress slowly over years. Patients may notice that their usual skincare products no longer work effectively, or that makeup application becomes more difficult due to altered skin