10 Back Skin Changes That Correspond to Internal Organ Health Concerns
The human back represents one of the body's largest canvases of skin, serving as a remarkable diagnostic window into our internal organ health. Traditional Chinese Medicine has long recognized the back as a reflection of internal organ function, with specific zones corresponding to different organ systems. Modern dermatology and internal medicine have begun to validate many of these ancient observations, revealing that various skin changes on the back can indeed signal underlying health concerns. From acne patterns that may indicate hormonal imbalances to discoloration that could suggest liver dysfunction, the back's skin provides valuable clues about what's happening beneath the surface. This comprehensive exploration examines ten distinct back skin changes that medical professionals increasingly recognize as potential indicators of internal organ health issues. By understanding these connections, individuals can become more attuned to their body's subtle warning signs and seek appropriate medical attention when necessary. The integration of dermatological observation with internal medicine creates a holistic approach to health assessment that empowers both patients and healthcare providers to identify potential problems before they become serious conditions.
1. Acne Along the Spine - Hormonal and Digestive System Indicators
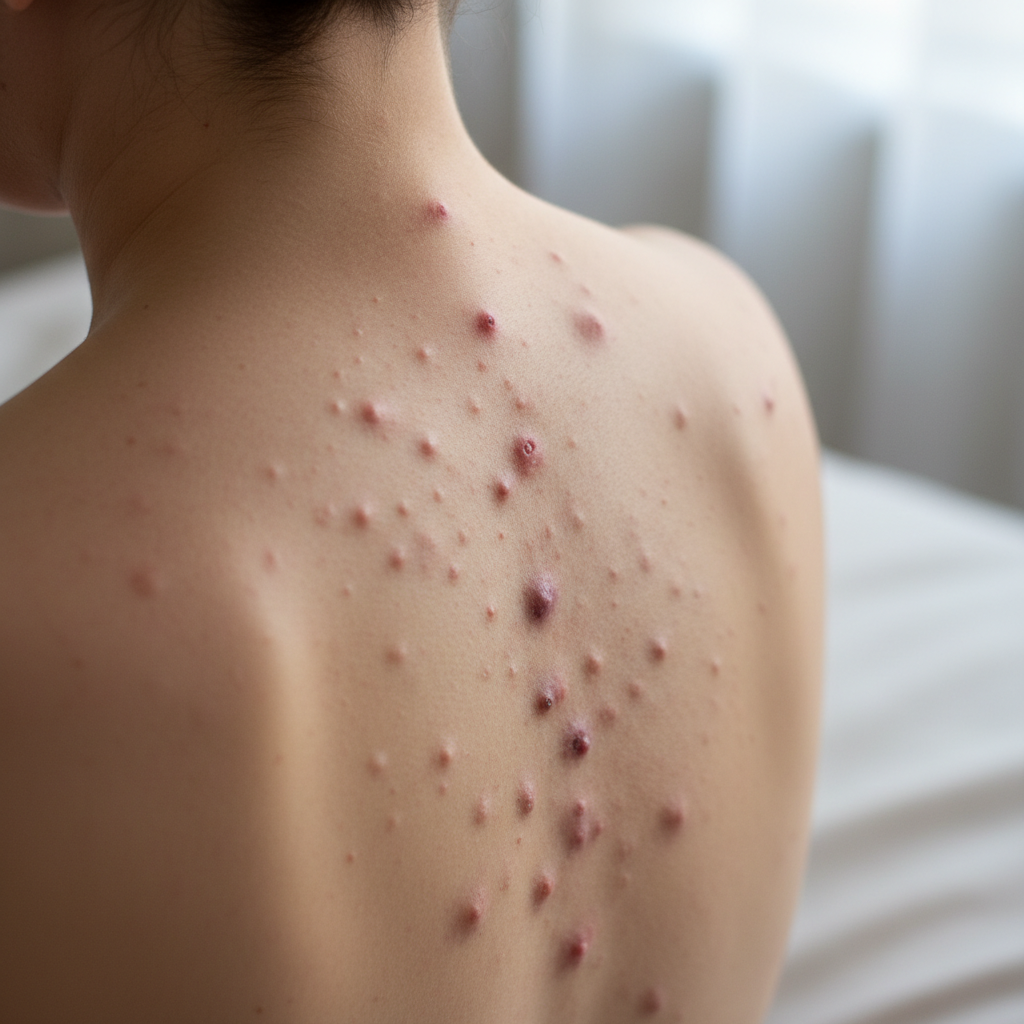
Acne formation along the spine, particularly in adults, often signals complex interactions between hormonal fluctuations and digestive system dysfunction. Research indicates that spinal acne frequently correlates with elevated androgen levels, insulin resistance, and compromised gut health. The sebaceous glands along the spine are particularly sensitive to hormonal changes, especially increases in dihydrotestosterone (DHT) and insulin-like growth factor-1 (IGF-1). When the digestive system struggles with inflammation or bacterial overgrowth, it can trigger systemic inflammatory responses that manifest as persistent acne along the vertebral column. Additionally, food sensitivities and poor dietary choices can exacerbate this condition by promoting inflammatory cytokine production. Women experiencing spinal acne may have underlying polycystic ovary syndrome (PCOS) or other endocrine disorders, while men might be dealing with testosterone imbalances or metabolic syndrome. The location and severity of spinal acne can provide healthcare providers with valuable insights into which specific hormonal pathways or digestive issues require attention, making this skin change a crucial diagnostic indicator for internal health assessment.
## Section 3: Darkened Patches (Acanthosis Nigricans) - Insulin Resistance and Metabolic Dysfunction
The appearance of dark, velvety patches on the back, medically known as acanthosis nigricans, serves as a significant early warning sign of insulin resistance and metabolic dysfunction. These hyperpigmented areas typically develop in skin folds and areas of friction, including the upper back, neck, and shoulder blade regions. The darkening occurs due to excessive insulin levels stimulating skin cell proliferation and melanin production, creating the characteristic thick, dark appearance. Research demonstrates that acanthosis nigricans often precedes the development of type 2 diabetes by several years, making it a crucial early intervention opportunity. The condition is strongly associated with obesity, metabolic syndrome, and various endocrine disorders including hypothyroidism and Cushing's syndrome. In some cases, the sudden appearance or rapid progression of these dark patches can indicate underlying malignancies, particularly gastric adenocarcinoma or other internal cancers that affect insulin signaling pathways. The severity and distribution of acanthosis nigricans correlate with the degree of insulin resistance, providing healthcare providers with a visual assessment tool for metabolic health. Early recognition and treatment of the underlying metabolic dysfunction can often lead to improvement or resolution of these skin changes.
2. Rashes and Hives on Upper Back - Liver Function and Detoxification Issues

Persistent rashes, hives, or unexplained skin eruptions on the upper back frequently indicate compromised liver function and impaired detoxification processes. The liver plays a crucial role in processing toxins, metabolizing hormones, and maintaining skin health through its detoxification pathways. When liver function becomes compromised due to conditions such as fatty liver disease, hepatitis, or excessive alcohol consumption, the body's ability to eliminate toxins through normal channels becomes impaired. Consequently, the skin, being the body's largest elimination organ, attempts to expel these accumulated toxins, resulting in various skin manifestations including rashes, hives, and inflammatory eruptions. The upper back is particularly susceptible to these manifestations due to its rich blood supply and proximity to major lymphatic drainage pathways. Additionally, liver dysfunction can lead to elevated histamine levels and altered immune responses, contributing to chronic urticaria and eczematous conditions. Certain medications that stress liver function, such as statins, antibiotics, or pain relievers, can exacerbate these skin changes. The pattern and persistence of upper back skin eruptions can provide valuable insights into the severity of liver compromise and guide appropriate diagnostic testing and treatment strategies.
3. Excessive Sweating and Heat Rashes - Thyroid and Adrenal Gland Dysfunction
Abnormal sweating patterns and recurrent heat rashes on the back often signal thyroid or adrenal gland dysfunction, representing the body's struggle to maintain proper temperature regulation and stress response. Hyperthyroidism frequently manifests as excessive sweating, particularly on the upper back and between the shoulder blades, accompanied by heat intolerance and skin that feels warm and moist. The thyroid's role in regulating metabolism directly impacts the body's thermoregulatory mechanisms, and when overactive, it can cause persistent hyperhidrosis even in cool environments. Conversely, adrenal dysfunction, whether from Addison's disease, Cushing's syndrome, or chronic stress, can disrupt the body's cortisol production and stress response systems, leading to altered sweating patterns and increased susceptibility to heat rashes. The sympathetic nervous system, which controls sweating, is intimately connected to both thyroid and adrenal function, creating a complex interplay that manifests on the skin. Chronic stress and adrenal fatigue can also compromise the skin's barrier function, making it more prone to irritation and rash formation. The location and timing of excessive sweating or heat rashes can provide diagnostic clues, with nighttime sweating often indicating hormonal imbalances while daytime episodes might suggest metabolic dysfunction.
4. Dry, Scaly Patches - Kidney Function and Fluid Balance Disorders
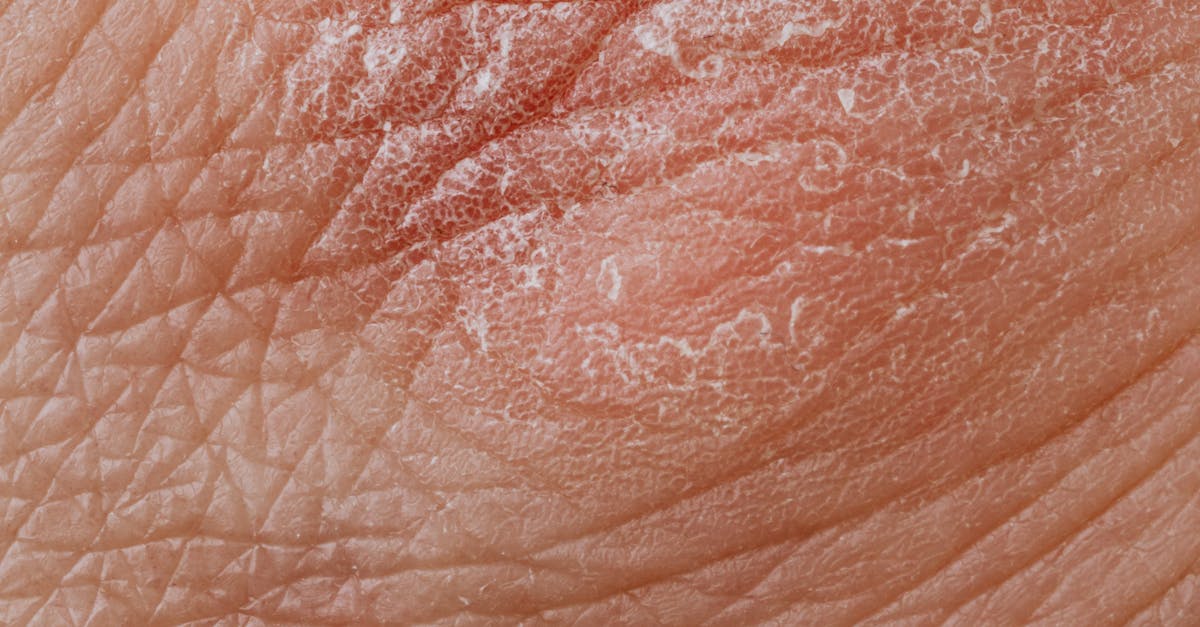
The development of persistently dry, scaly patches on the back can indicate underlying kidney dysfunction and fluid balance disorders that affect the body's ability to maintain proper hydration and electrolyte balance. The kidneys play a vital role in regulating fluid retention, electrolyte balance, and waste elimination, all of which directly impact skin health and appearance. When kidney function becomes compromised, the body's ability to maintain proper hydration levels diminishes, leading to chronically dry skin that may appear scaly, flaky, or rough to the touch. Additionally, kidney dysfunction can result in the accumulation of uremic toxins in the bloodstream, which can manifest as skin irritation, itching, and altered skin texture. Chronic kidney disease often presents with a condition called uremic frost, where crystallized urea appears on the skin surface, though this typically occurs in advanced stages. The back's large surface area makes it particularly susceptible to showing these systemic changes in skin hydration and texture. Electrolyte imbalances associated with kidney dysfunction, particularly alterations in sodium, potassium, and phosphorus levels, can further compromise skin barrier function and cellular regeneration processes, perpetuating the cycle of dry, scaly skin formation.
5. Unusual Moles and Pigmentation Changes - Liver Health and Hormonal Imbalances

Changes in mole appearance, new pigmentation patterns, or unusual discoloration on the back can reflect liver health issues and hormonal imbalances that affect melanin production and cellular regulation. The liver's role in hormone metabolism, particularly estrogen and testosterone processing, directly influences skin pigmentation patterns and cellular growth regulation. When liver function becomes impaired, hormonal imbalances can develop, leading to irregular melanin distribution and the formation of age spots, melasma, or other pigmentary disorders. Additionally, liver dysfunction can compromise the body's ability to process and eliminate cellular waste products, potentially contributing to abnormal cellular growth patterns including changes in existing moles or the development of new pigmented lesions. Hormonal fluctuations associated with liver dysfunction can also stimulate melanocyte activity, leading to hyperpigmentation in sun-exposed areas like the upper back and shoulders. The liver's role in vitamin D metabolism and antioxidant processing further impacts skin health and cellular protection mechanisms. While not all mole changes indicate serious health concerns, persistent or rapidly changing pigmentation patterns warrant medical evaluation, as they can sometimes signal more serious underlying conditions including metabolic disorders or, in rare cases, internal malignancies that affect hormone production or liver function.
## Section 8: Persistent Itching Without Visible Rash - Blood Sugar Irregularities and Circulation Issues
Chronic itching on the back without visible rash or skin changes often indicates blood sugar irregularities and circulation problems that affect nerve function and skin sensitivity. Diabetes and prediabetes can cause peripheral neuropathy, which manifests as altered sensation, tingling, or persistent itching, particularly in areas with rich nerve supply like the back. Elevated blood glucose levels can damage small blood vessels and nerve endings, leading to compromised circulation and altered skin sensation. The resulting poor circulation reduces the skin's ability to maintain proper moisture levels and cellular regeneration, contributing to chronic itching sensations. Additionally, diabetic individuals are more susceptible to fungal and bacterial infections that may not always present with visible symptoms initially, causing persistent itching as an early warning sign. Blood sugar fluctuations can also affect the body's inflammatory response and immune function, leading to heightened skin sensitivity and itching. Poor circulation associated with cardiovascular disease or peripheral vascular disease can similarly cause itching due to inadequate oxygen and nutrient delivery to skin tissues. The back's extensive network of sensory nerves makes it particularly susceptible to these circulation-related changes, often serving as an early indicator of systemic vascular or metabolic problems that require medical attention.
6. Skin Tags and Growths - Metabolic Syndrome and Insulin Resistance
The proliferation of skin tags and small growths on the back, particularly around the shoulder blades and upper back region, frequently correlates with metabolic syndrome and insulin resistance. Skin tags, medically known as acrochordons, develop when elevated insulin levels stimulate excessive skin cell growth and proliferation. Research has established strong associations between skin tag formation and various components of metabolic syndrome, including obesity, hypertension, dyslipidemia, and glucose intolerance. The insulin-like growth factor pathways become hyperactivated in insulin-resistant states, promoting not only skin tag formation but also increasing the risk of other skin growths and cellular abnormalities. The number and size of skin tags often correlate with the severity of metabolic dysfunction, making them useful clinical markers for assessing metabolic health. Additionally, skin tags may indicate underlying hormonal imbalances, particularly in women with polycystic ovary syndrome (PCOS) or men with low testosterone levels. The mechanical friction common in back areas, combined with the metabolic factors, creates an ideal environment for skin tag development. While generally benign, the sudden appearance of multiple skin tags or rapid changes in existing growths should prompt evaluation for underlying metabolic disorders and, in rare cases, internal malignancies that can stimulate growth factor production.
7. Color Changes and Jaundice - Liver Disease and Bile Duct Disorders
Subtle color changes in back skin, including yellowing, bronze discoloration, or unusual pallor, can indicate serious liver disease and bile duct disorders that affect bilirubin processing and circulation. Jaundice, characterized by yellowing of the skin and sclera, occurs when bilirubin levels become elevated due to liver dysfunction, bile duct obstruction, or excessive red blood cell breakdown. The back's large surface area often shows these color changes more subtly than other body areas, making careful observation crucial for early detection. Hepatitis, cirrhosis, gallbladder disease, and pancreatic disorders can all manifest with skin color changes that may first become apparent on the back. Bronze discoloration might indicate hemochromatosis, a condition involving excessive iron accumulation that primarily affects the liver. Additionally, certain liver diseases can cause changes in skin texture and appearance beyond color alterations, including spider angiomata, palmar erythema, and altered skin elasticity. The liver's role in producing proteins essential for skin health means that chronic liver disease often presents with multiple skin manifestations simultaneously. Early recognition of these color changes can be crucial for timely diagnosis and treatment of potentially serious liver conditions, making regular skin observation an important component of health monitoring.
8. Integrating Back Skin Observations into Holistic Health Assessment
The intricate connections between back skin changes and internal organ health underscore the importance of viewing the body as an interconnected system where external manifestations often reflect internal dysfunction. Healthcare providers and individuals alike can benefit from understanding these relationships, using skin observations as valuable diagnostic tools that complement traditional medical assessments. The ten skin changes discussed represent just a fraction of the complex ways our largest organ communicates about internal health status. Regular self-examination of the back, though challenging due to its location, becomes crucial for early detection of potential health issues. The integration of dermatological observations with internal medicine principles creates opportunities for earlier intervention and better health outcomes. However, it's essential to remember that skin changes should always be evaluated by qualified healthcare professionals who can distinguish between benign variations and clinically significant findings. The holistic approach to health assessment, incorporating both external observations and internal evaluations, represents the future of preventive medicine. By remaining attentive to these subtle body signals and seeking appropriate medical guidance when changes occur, individuals can take proactive steps toward maintaining optimal health and catching potential problems before they progress to more serious conditions.