10 Armpit and Groin Skin Changes That Signal Hormonal and Metabolic Issues
The skin in our armpits and groin areas serves as a remarkable diagnostic window into our body's internal hormonal and metabolic health, often revealing crucial information long before other symptoms manifest. These intimate areas, rich in apocrine glands and sensitive to hormonal fluctuations, frequently display the earliest signs of endocrine disruption, insulin resistance, and metabolic dysfunction. Unlike other parts of the body, the skin in these regions is particularly responsive to changes in hormones like insulin, androgens, cortisol, and thyroid hormones, making it an invaluable early warning system for underlying health issues. Medical professionals increasingly recognize that skin changes in these areas can precede more serious conditions such as diabetes, polycystic ovary syndrome (PCOS), thyroid disorders, and adrenal dysfunction by months or even years. Understanding these subtle yet significant changes empowers individuals to seek appropriate medical attention before conditions progress to more advanced stages. The following exploration delves into ten specific skin manifestations that serve as important indicators of hormonal and metabolic imbalances, providing insight into when these changes warrant medical evaluation and what they might reveal about your overall health status.
1. Acanthosis Nigricans - The Dark Velvet Warning Sign
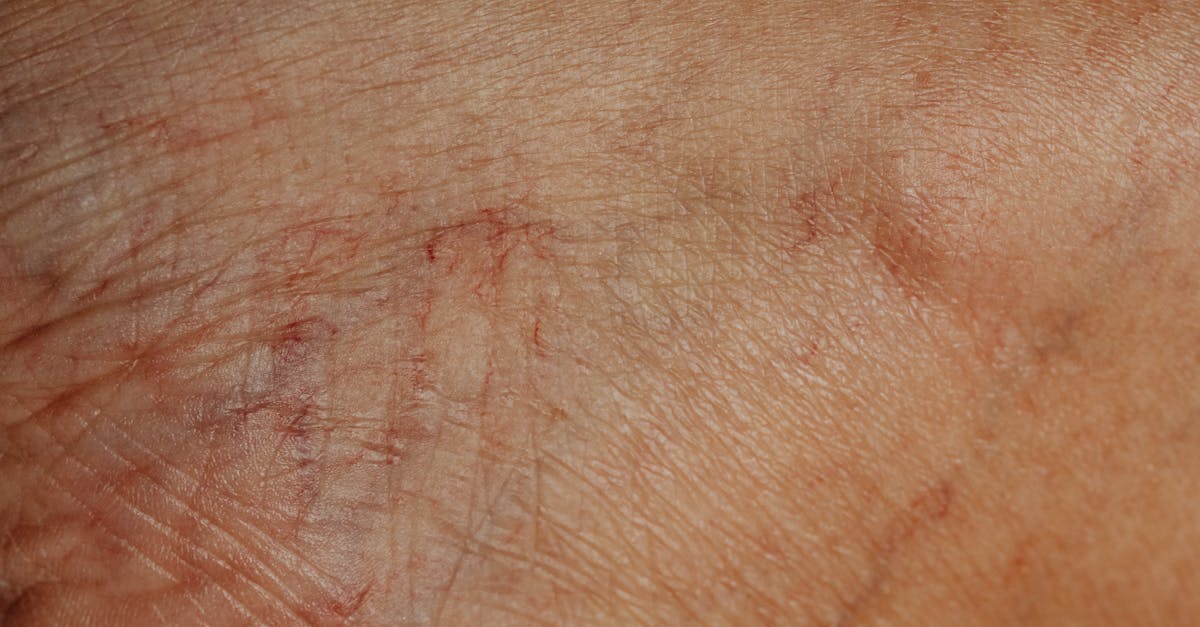
Acanthosis nigricans presents as dark, velvety patches of skin that commonly appear in the armpits, groin, and neck folds, serving as one of the most significant indicators of insulin resistance and metabolic dysfunction. This distinctive skin condition occurs when elevated insulin levels stimulate skin cell proliferation and melanin production, creating the characteristic hyperpigmented, thickened appearance that feels soft and velvety to the touch. Research consistently demonstrates that acanthosis nigricans is strongly associated with type 2 diabetes, with studies showing that up to 90% of individuals with this skin condition have some degree of insulin resistance. The condition is particularly prevalent among individuals with obesity, affecting nearly 75% of adults with a BMI over 30, and often appears years before diabetes is formally diagnosed. Beyond diabetes, acanthosis nigricans can signal other serious conditions including hypothyroidism, Cushing's syndrome, and certain cancers, particularly gastric adenocarcinoma. The severity and extent of the darkening often correlate with the degree of insulin resistance, making it not only a diagnostic marker but also a tool for monitoring metabolic health over time. Early recognition of acanthosis nigricans allows for timely intervention through lifestyle modifications, dietary changes, and medical treatment that can potentially prevent or delay the onset of type 2 diabetes and its associated complications.
2. Hidradenitis Suppurativa - Inflammatory Signals of Hormonal Chaos
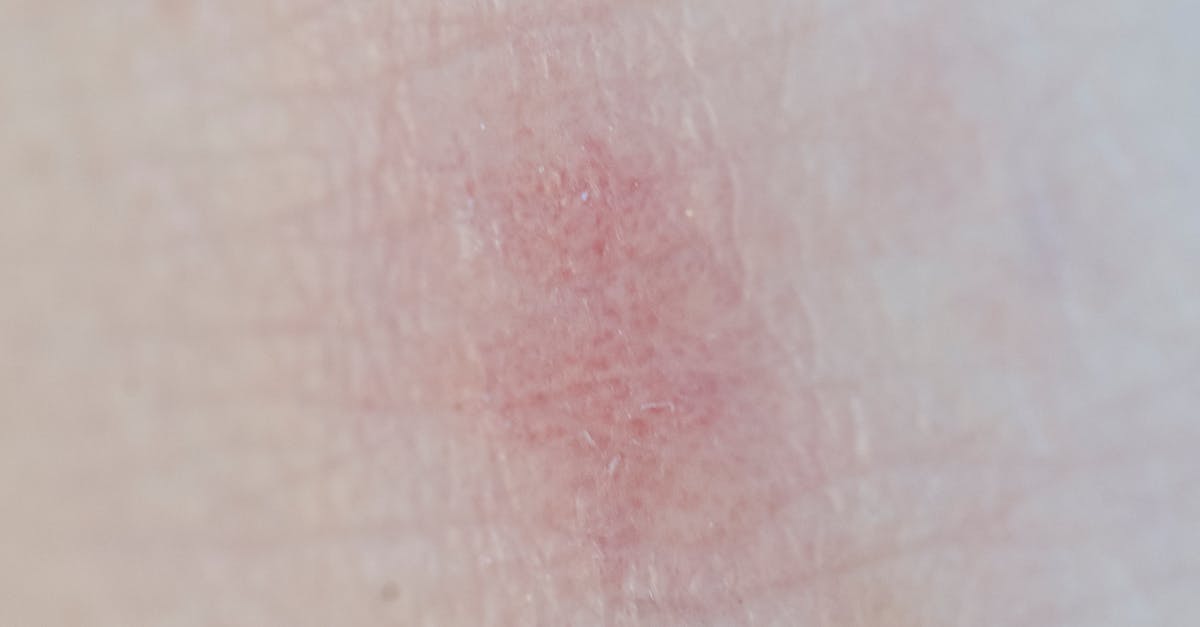
Hidradenitis suppurativa (HS) is a chronic inflammatory skin condition that primarily affects areas rich in apocrine glands, including the armpits and groin, manifesting as painful nodules, abscesses, and scarring that often indicates significant hormonal imbalances and metabolic dysfunction. This debilitating condition affects approximately 1-4% of the population, with women being disproportionately affected due to its strong association with hormonal fluctuations, particularly androgens and insulin. The pathophysiology of HS involves follicular occlusion and subsequent inflammation, which is exacerbated by hormonal imbalances, insulin resistance, and metabolic syndrome. Studies reveal that individuals with HS have significantly higher rates of diabetes, with some research indicating up to a 30% prevalence of type 2 diabetes among HS patients compared to 8% in the general population. The condition often worsens during hormonal changes such as menstruation, pregnancy, and menopause, highlighting its intimate connection with endocrine function. Additionally, HS is frequently associated with polycystic ovary syndrome (PCOS), thyroid disorders, and elevated inflammatory markers that suggest broader metabolic dysfunction. The chronic inflammation characteristic of HS can contribute to insulin resistance, creating a vicious cycle where metabolic dysfunction worsens the skin condition, which in turn promotes further metabolic imbalance. Recognition of HS as more than just a skin condition is crucial, as it often serves as an external manifestation of internal metabolic chaos requiring comprehensive medical evaluation and management.
3. Skin Tags - Small Growths with Big Implications

Skin tags, medically known as acrochordons, are small, benign growths that commonly appear in friction-prone areas like the armpits and groin, serving as important markers of insulin resistance and metabolic dysfunction that are often overlooked by both patients and healthcare providers. These soft, flesh-colored or slightly darker growths typically measure 1-5 millimeters in diameter and hang from the skin on a thin stalk, developing most frequently in areas where skin rubs against skin or clothing. Research has established a strong correlation between the presence of multiple skin tags and insulin resistance, with studies showing that individuals with five or more skin tags have significantly higher insulin levels and are at increased risk for developing type 2 diabetes. The pathophysiology behind this association involves elevated insulin and insulin-like growth factor-1 (IGF-1) levels, which stimulate keratinocyte and fibroblast proliferation, leading to the formation of these benign growths. Interestingly, the number and size of skin tags often correlate with the severity of insulin resistance, making them a potential clinical marker for metabolic health assessment. Beyond diabetes risk, skin tags are also associated with obesity, dyslipidemia, and cardiovascular disease, reflecting their role as indicators of broader metabolic syndrome. While skin tags themselves are harmless, their presence, particularly when numerous, should prompt evaluation for underlying metabolic conditions and may serve as motivation for lifestyle interventions aimed at improving insulin sensitivity and overall metabolic health.
4. Intertrigo - When Moisture Meets Metabolic Dysfunction
Intertrigo is an inflammatory skin condition that occurs in skin folds, including the armpits and groin, where moisture, friction, and bacterial or fungal overgrowth create an environment that is often exacerbated by underlying hormonal and metabolic imbalances. This condition presents as red, raw, and sometimes malodorous patches of skin that can become secondarily infected, causing significant discomfort and serving as an indicator of compromised immune function and metabolic health. Individuals with diabetes are particularly susceptible to intertrigo due to elevated glucose levels in sweat and skin secretions, which create an ideal environment for pathogenic microorganisms to flourish. The condition is also more common in people with obesity, as excess weight creates deeper skin folds and increased friction, while also being associated with insulin resistance and altered immune function. Hormonal changes, particularly those involving cortisol and sex hormones, can affect skin barrier function and immune response, making individuals more prone to developing intertrigo during times of hormonal fluctuation. The chronic inflammation associated with intertrigo can contribute to insulin resistance through the release of pro-inflammatory cytokines, creating a cycle where metabolic dysfunction promotes skin problems, which in turn worsen metabolic health. Additionally, the stress and discomfort caused by recurrent intertrigo can elevate cortisol levels, further disrupting hormonal balance and potentially affecting glucose metabolism. Recognition of intertrigo as more than just a hygiene issue is important, as persistent or recurrent cases may warrant evaluation for underlying diabetes, immune dysfunction, or hormonal imbalances.
5. Excessive Hair Growth (Hirsutism) - Androgen Overload Manifestation

Hirsutism, characterized by excessive hair growth in typically male-pattern areas including the groin region and sometimes extending to the lower abdomen, represents one of the most visible signs of androgen excess and hormonal imbalance, particularly in women. This condition affects approximately 5-10% of women of reproductive age and is most commonly associated with polycystic ovary syndrome (PCOS), which affects up to 15% of women worldwide and is characterized by insulin resistance, elevated androgen levels, and metabolic dysfunction. The pathophysiology of hirsutism involves increased sensitivity to androgens or elevated androgen production, often triggered or worsened by insulin resistance, which stimulates ovarian and adrenal androgen production through complex hormonal pathways. Beyond PCOS, hirsutism can indicate other serious conditions including congenital adrenal hyperplasia, Cushing's syndrome, androgen-secreting tumors, and insulin resistance syndrome, making it an important clinical sign that warrants thorough evaluation. The psychological impact of hirsutism is significant, often leading to decreased quality of life, social anxiety, and depression, which can further disrupt hormonal balance through stress-induced cortisol elevation. Studies demonstrate that women with hirsutism have higher rates of metabolic syndrome, type 2 diabetes, and cardiovascular disease, reflecting the interconnected nature of hormonal and metabolic health. The severity of hirsutism often correlates with the degree of insulin resistance and metabolic dysfunction, making it not only a cosmetic concern but also a marker of overall health status. Early recognition and treatment of the underlying hormonal imbalances causing hirsutism can prevent progression to more serious metabolic complications while also addressing the distressing cosmetic aspects of the condition.
6. Hyperpigmentation and Melasma - Hormonal Imprints on Skin
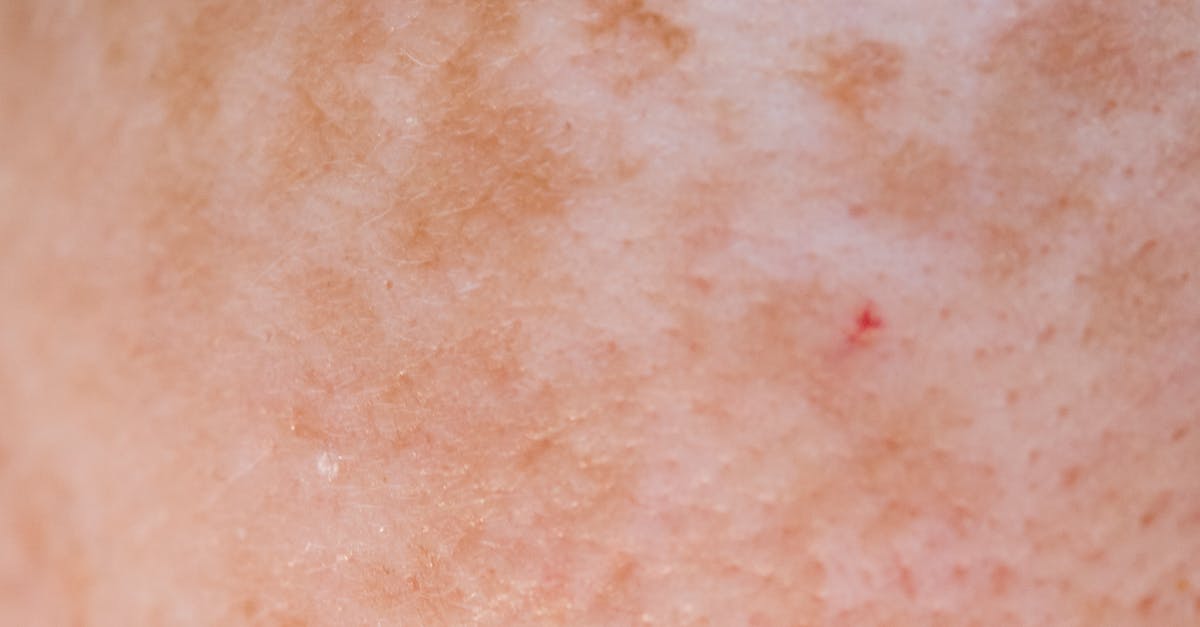
Hyperpigmentation in the armpit and groin areas, including conditions like melasma, represents a complex interplay of hormonal influences, particularly estrogen and progesterone fluctuations, that can signal underlying endocrine dysfunction and metabolic imbalances. While melasma typically affects facial areas, similar hyperpigmentation patterns can occur in body folds and intimate areas, particularly during pregnancy (chloasma), menopause, or with hormonal contraceptive use, indicating significant hormonal shifts that may have broader metabolic implications. The pathophysiology involves hormonal stimulation of melanocytes, the pigment-producing cells in the skin, with estrogen and progesterone playing key roles in regulating melanin synthesis and distribution. Insulin resistance can exacerbate hyperpigmentation through multiple mechanisms, including direct effects on melanocyte activity and indirect effects through inflammatory pathways and growth factor stimulation. Women with PCOS frequently experience hyperpigmentation in body folds, which often coincides with acanthosis nigricans, creating a complex pattern of skin changes that reflects the multifaceted nature of their hormonal and metabolic dysfunction. Thyroid disorders, particularly hypothyroidism, can also contribute to hyperpigmentation through alterations in hormone metabolism and skin cell turnover, while adrenal disorders may cause distinctive patterns of pigmentation that can help differentiate between various endocrine conditions. The persistence of hyperpigmentation after hormonal changes have resolved may indicate ongoing metabolic dysfunction or insulin resistance, making it an important marker for long-term health monitoring. Understanding these pigmentation changes as more than cosmetic concerns allows for earlier detection and treatment of underlying hormonal imbalances that could progress to more serious metabolic complications.
7. Chronic Infections and Poor Wound Healing - Metabolic Compromise Revealed
Recurrent bacterial, fungal, or yeast infections in the armpit and groin areas, along with poor wound healing in these regions, often serve as early indicators of compromised immune function associated with hormonal imbalances and metabolic dysfunction, particularly diabetes and insulin resistance. The warm, moist environment of these body areas naturally harbors various microorganisms, but when the body's immune system is compromised or when glucose levels are elevated, these normally harmless organisms can become pathogenic, leading to persistent or recurrent infections. Elevated blood glucose levels, even in prediabetic ranges, can impair white blood cell function and create an environment conducive to bacterial and fungal growth, as many pathogens thrive in glucose-rich environments. Hormonal imbalances, particularly those involving cortisol, can suppress immune function and delay wound healing, while insulin resistance can impair the cellular processes necessary for tissue repair and regeneration. Women with PCOS often experience recurrent vaginal and groin infections due to the combination of insulin resistance, elevated androgens, and altered immune function that characterizes this condition. Additionally, thyroid dysfunction can significantly impact immune system performance and wound healing capacity, with both hyperthyroidism and hypothyroidism associated with increased infection risk and delayed healing. The chronic inflammation associated with recurrent infections can further worsen insulin resistance and hormonal imbalances, creating a vicious cycle that perpetuates both the skin problems and the underlying metabolic dysfunction. Recognition of this pattern of recurrent infections and poor healing as potential indicators of metabolic disease allows for earlier intervention and prevention of more serious complications.
8. Unusual Sweating Patterns - Thermoregulatory Disruption
Abnormal sweating patterns in the armpit and groin areas, including excessive sweating (hyperhidrosis) or unusual odor changes, can indicate significant hormonal and metabolic disruptions affecting the body's thermoregulatory system and autonomic nervous function. The apocrine glands concentrated in these areas are particularly sensitive to hormonal influences, with androgens, estrogens, and stress hormones all playing roles in regulating sweat production and composition. Hyperthyroidism commonly causes excessive sweating as the elevated metabolic rate increases heat production, requiring enhanced cooling mechanisms, while the sweating pattern may be accompanied by other signs of metabolic acceleration such as weight loss and increased heart rate. Conversely, diabetes can cause both excessive sweating due to autonomic neuropathy and changes in sweat composition due to elevated glucose levels, creating an environment that promotes bacterial and fungal growth. Menopause and perimenopause frequently cause dramatic changes in sweating patterns due to estrogen fluctuations affecting the hypothalamic temperature regulation center, often resulting in sudden onset sweating episodes that can be particularly pronounced in the armpit and groin areas. Adrenal disorders, including Addison's disease and Cushing's syndrome, can significantly alter sweating patterns through their effects on cortisol levels and electrolyte balance, while also affecting the body's stress response and temperature regulation. The psychological stress associated with unusual sweating can further disrupt hormonal balance through elevated cortisol levels, creating a feedback loop that perpetuates both the sweating problem and the underlying hormonal dysfunction. Changes in sweat odor may also indicate metabolic changes, as certain conditions like diabetes can alter the chemical composition of sweat, producing distinctive odors that may be among the first noticeable signs of metabolic dysfunction.
9. Skin Texture Changes and Keratosis Pilaris - Cellular Metabolism Indicators
Changes in skin texture, including the development of keratosis pilaris (small, rough bumps) in the armpit and groin areas, can indicate underlying hormonal imbalances and metabolic dysfunction affecting cellular turnover and keratin production. Keratosis pilaris, commonly known as "chicken skin," occurs when keratin builds up in hair follicles, creating small, rough bumps that can be particularly noticeable in areas of friction like the armpits and inner thighs. This condition is often associated with insulin resistance, as elevated insulin levels can affect keratinocyte proliferation and differentiation, leading to abnormal keratin accumulation and follicular plugging. Hormonal changes, particularly those involving androgens and thyroid hormones, can significantly impact skin cell turnover rates and keratin production, with both hypothyroidism and PCOS commonly associated with keratosis pilaris and other texture changes. The condition often worsens during periods of hormonal fluctuation, such as puberty, pregnancy, and menopause, highlighting its sensitivity to endocrine changes and its potential value as a marker of hormonal health. Vitamin deficiencies, particularly vitamin A and essential fatty acids, which are often associated with metabolic dysfunction and malabsorption issues, can exacerbate keratosis pilaris and other texture changes. The chronic inflammation associated with keratosis pilaris may contribute to insulin resistance through inflammatory pathways, while the psychological impact of visible skin texture changes can increase stress levels and further disrupt hormonal balance. Additionally, the presence of keratosis pilaris in conjunction with other skin changes like acanthosis nigricans or skin tags may indicate more significant metabolic dysfunction requiring comprehensive evaluation and treatment. Understanding these texture changes as potential indicators of internal health issues allows for earlier intervention and may prevent progression to more serious metabolic complications.
10. Stretch Marks and Skin Elasticity Changes - Hormonal Impact on Connective Tissue
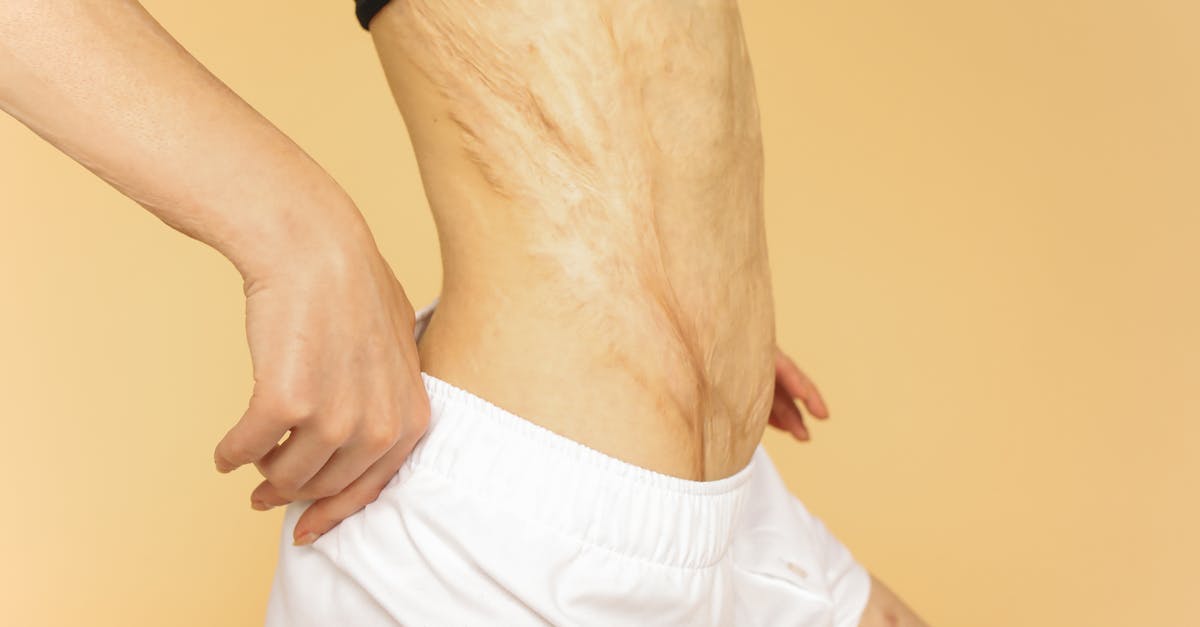
The development of new stretch marks (striae) or changes in existing ones in the armpit and groin areas can indicate significant hormonal fluctuations and metabolic changes affecting collagen production and skin elasticity, particularly when they appear outside of typical growth periods or pregnancy. Stretch marks form when the skin is stretched beyond its elastic capacity, causing tears in the dermis that initially appear red or purple before fading to white or silver, but their development can be accelerated by hormonal imbalances that affect collagen synthesis and skin structure. Cushing's syndrome, characterized by excess cortisol production, commonly causes the development of wide, purple stretch marks in unusual locations, including the armpits and groin, as cortisol inhibits collagen formation and weakens skin structure. Rapid weight gain associated with insulin resistance and metabolic syndrome can contribute to stretch mark formation, while the underlying hormonal imbalances may make the skin more susceptible to stretching and less capable of repair. Adolescents experiencing growth spurts may develop stretch marks in these areas, but when they appear in adults without obvious causes like pregnancy or significant weight changes, they may indicate underlying endocrine disorders such as thyroid dysfunction or adrenal abnormalities. The color, width, and pattern of stretch marks can provide clues about their underlying cause, with certain characteristics being more suggestive of hormonal disorders versus mechanical stretching. Changes in skin elasticity and the appearance of new stretch marks may also indicate nutritional deficiencies or malabsorption issues that commonly accompany metabolic dysfunction, particularly deficiencies in vitamin C, zinc, and protein that are essential for collagen synthesis. The psychological impact of visible stretch marks can contribute to stress and body image issues, potentially affecting hormonal balance through stress-induced cortisol elevation and creating a cycle that may worsen both the skin condition and underlying metabolic health.