8 Cardiovascular Conditions With Early Visual Warning Signs
The human eye serves as a remarkable diagnostic window into the cardiovascular system, offering healthcare professionals and individuals alike crucial early warning signs of potentially life-threatening heart conditions. This intimate connection between ocular health and cardiovascular wellness stems from the eye's unique vascular architecture, which mirrors the delicate blood vessel networks throughout the body. When cardiovascular disease begins to develop, the retinal blood vessels, optic nerve, and surrounding ocular structures often manifest visible changes that can precede traditional cardiac symptoms by months or even years. These visual indicators range from subtle alterations in blood vessel appearance to more pronounced changes in vision quality, eye pressure, and ocular surface characteristics. Understanding these eight critical cardiovascular conditions and their associated visual warning signs empowers individuals to seek timely medical intervention, potentially preventing heart attacks, strokes, and other serious complications. The retina, being the only place in the human body where blood vessels can be directly observed without invasive procedures, provides an invaluable opportunity for early detection and monitoring of systemic cardiovascular health, making regular comprehensive eye examinations an essential component of preventive healthcare.
1. Hypertensive Retinopathy - The Silent Blood Pressure Indicator

Hypertensive retinopathy represents one of the most common and diagnostically significant cardiovascular conditions detectable through eye examination, occurring when chronically elevated blood pressure damages the delicate retinal blood vessels. This condition manifests through a progressive spectrum of visual changes, beginning with arterial narrowing and arteriovenous nicking, where arteries compress adjacent veins at crossing points, creating a characteristic "copper wire" or "silver wire" appearance. As hypertension persists and worsens, patients may notice gradual vision changes, including blurred vision, difficulty focusing, and reduced peripheral vision, though many individuals remain asymptomatic in early stages. Advanced hypertensive retinopathy can produce more dramatic visual symptoms, including sudden vision loss, double vision, and the appearance of floaters or flashing lights, indicating retinal hemorrhages, exudates, or papilledema. The severity of retinal changes often correlates directly with the degree of systemic hypertension and the risk of cardiovascular complications, making ophthalmoscopic examination a valuable tool for assessing overall cardiovascular risk. Early detection of hypertensive retinopathy can prompt immediate blood pressure management, potentially preventing stroke, heart attack, and kidney disease, while also preserving vision and preventing irreversible retinal damage that could lead to permanent visual impairment.
2. Diabetic Retinopathy - Microvascular Damage Visualization
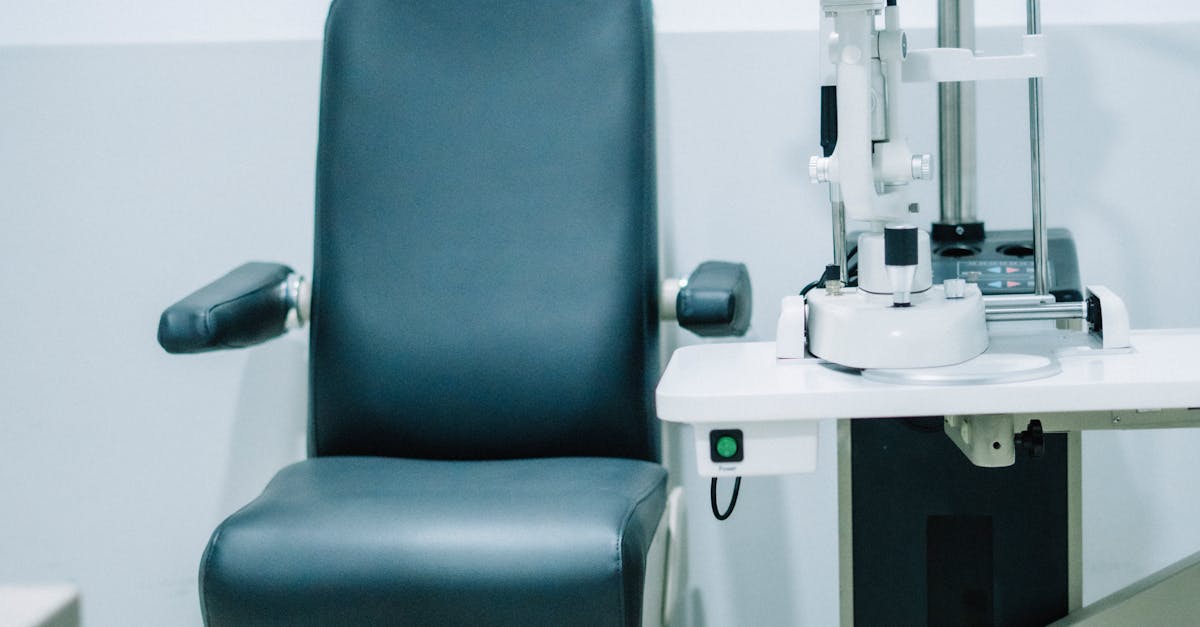
Diabetic retinopathy emerges as a critical cardiovascular warning sign, reflecting the widespread microvascular damage that characterizes diabetes mellitus and significantly increases the risk of heart disease, stroke, and peripheral vascular complications. This condition develops when chronically elevated blood glucose levels damage the tiny blood vessels within the retina, leading to a cascade of pathological changes that mirror similar processes occurring throughout the cardiovascular system. Early-stage diabetic retinopathy, known as non-proliferative diabetic retinopathy, presents with microaneurysms, dot and blot hemorrhages, and hard exudates that may cause subtle vision changes, including mild blurring, difficulty with night vision, and problems with color discrimination. As the condition progresses to proliferative diabetic retinopathy, patients may experience more severe visual symptoms, including significant vision loss, the appearance of dark spots or strings in their visual field, and sudden flashes of light, indicating the growth of abnormal blood vessels and potential retinal detachment. The presence and severity of diabetic retinopathy serve as powerful predictors of cardiovascular risk, with studies demonstrating that individuals with advanced retinal changes face dramatically increased risks of heart attack, stroke, and cardiovascular death. Regular dilated eye examinations for diabetic patients not only preserve vision but also provide crucial information about overall vascular health and the need for aggressive cardiovascular risk factor modification.
3. Retinal Artery Occlusion - Stroke's Ocular Manifestation
Retinal artery occlusion represents a true ocular emergency that serves as both a cardiovascular warning sign and a predictor of imminent stroke risk, occurring when blood clots or emboli block the central retinal artery or its branches, causing sudden, painless vision loss. This condition, often described as a "stroke of the eye," typically results from the same underlying cardiovascular pathology that causes cerebral strokes, including carotid artery disease, atrial fibrillation, and systemic atherosclerosis. Patients experiencing retinal artery occlusion report sudden, dramatic vision loss in one eye, often described as a curtain or shadow descending across their visual field, and this vision loss may be preceded by episodes of temporary vision loss called amaurosis fugax. The visual symptoms can range from complete blindness in the affected eye to sectoral vision loss, depending on whether the central retinal artery or branch arteries are involved, and the degree of vision recovery depends heavily on the speed of treatment and restoration of blood flow. Beyond the immediate threat to vision, retinal artery occlusion serves as a critical warning sign for systemic cardiovascular disease, with studies showing that affected individuals face significantly elevated risks of stroke, heart attack, and cardiovascular death in the months and years following the ocular event. Immediate medical evaluation following retinal artery occlusion should include comprehensive cardiovascular assessment, carotid imaging, cardiac rhythm monitoring, and aggressive risk factor modification to prevent future cardiovascular events and preserve both vision and life.
4. Hollenhorst Plaques - Embolic Warning Signals

Hollenhorst plaques, also known as retinal cholesterol emboli, appear as bright, refractile, yellow-orange deposits within retinal arterioles and serve as visible evidence of systemic atherosclerotic disease and significant cardiovascular risk. These microscopic cholesterol crystals originate from ulcerated atherosclerotic plaques, typically in the carotid arteries or aortic arch, and travel through the circulation to lodge in the small retinal vessels, where they can be directly observed during ophthalmoscopic examination. While Hollenhorst plaques themselves rarely cause significant visual symptoms, their presence indicates active atherosclerotic disease and a substantially increased risk of stroke, heart attack, and other cardiovascular events. Patients with these retinal emboli may occasionally report transient visual disturbances, including brief episodes of vision loss, flickering lights, or temporary blind spots, particularly if the emboli temporarily obstruct retinal blood flow before becoming permanently lodged. The detection of Hollenhorst plaques during routine eye examination should prompt immediate and comprehensive cardiovascular evaluation, including carotid duplex ultrasonography, echocardiography, and assessment of traditional cardiovascular risk factors. Studies have demonstrated that individuals with retinal cholesterol emboli face a dramatically increased risk of stroke within the first year after detection, making their identification a critical opportunity for preventive intervention. The presence of these plaques often indicates the need for antiplatelet therapy, statin treatment, and potentially surgical intervention such as carotid endarterectomy, depending on the degree of carotid stenosis and overall cardiovascular risk profile.
5. Papilledema - Intracranial Pressure and Cardiac Connections
Papilledema, characterized by optic disc swelling due to increased intracranial pressure, can serve as an important visual warning sign for several cardiovascular conditions, particularly those involving cerebral circulation and venous drainage abnormalities. This condition manifests as bilateral optic disc swelling visible during ophthalmoscopic examination and may be associated with various cardiovascular pathologies, including cerebral venous thrombosis, congestive heart failure with elevated central venous pressure, and hypertensive emergencies. Patients with papilledema typically experience gradual onset of visual symptoms, including transient vision loss lasting seconds (visual obscurations), peripheral vision defects, double vision due to sixth cranial nerve palsy, and headaches that worsen with position changes or Valsalva maneuvers. The visual changes associated with papilledema can progress from subtle peripheral vision loss to significant central vision impairment if left untreated, and the condition may be accompanied by other neurological symptoms such as headache, nausea, and altered mental status. In the context of cardiovascular disease, papilledema may indicate cerebral venous thrombosis, a serious condition that can result from hypercoagulable states, dehydration, or underlying cardiac conditions that promote clot formation. Additionally, severe hypertensive crises can cause papilledema as part of hypertensive encephalopathy, representing a medical emergency requiring immediate blood pressure reduction and cardiovascular stabilization. Recognition of papilledema should prompt urgent neurological and cardiovascular evaluation, including neuroimaging, lumbar puncture when appropriate, and comprehensive assessment of cardiac function and coagulation status.
6. Retinal Vein Occlusion - Venous Circulation Compromise
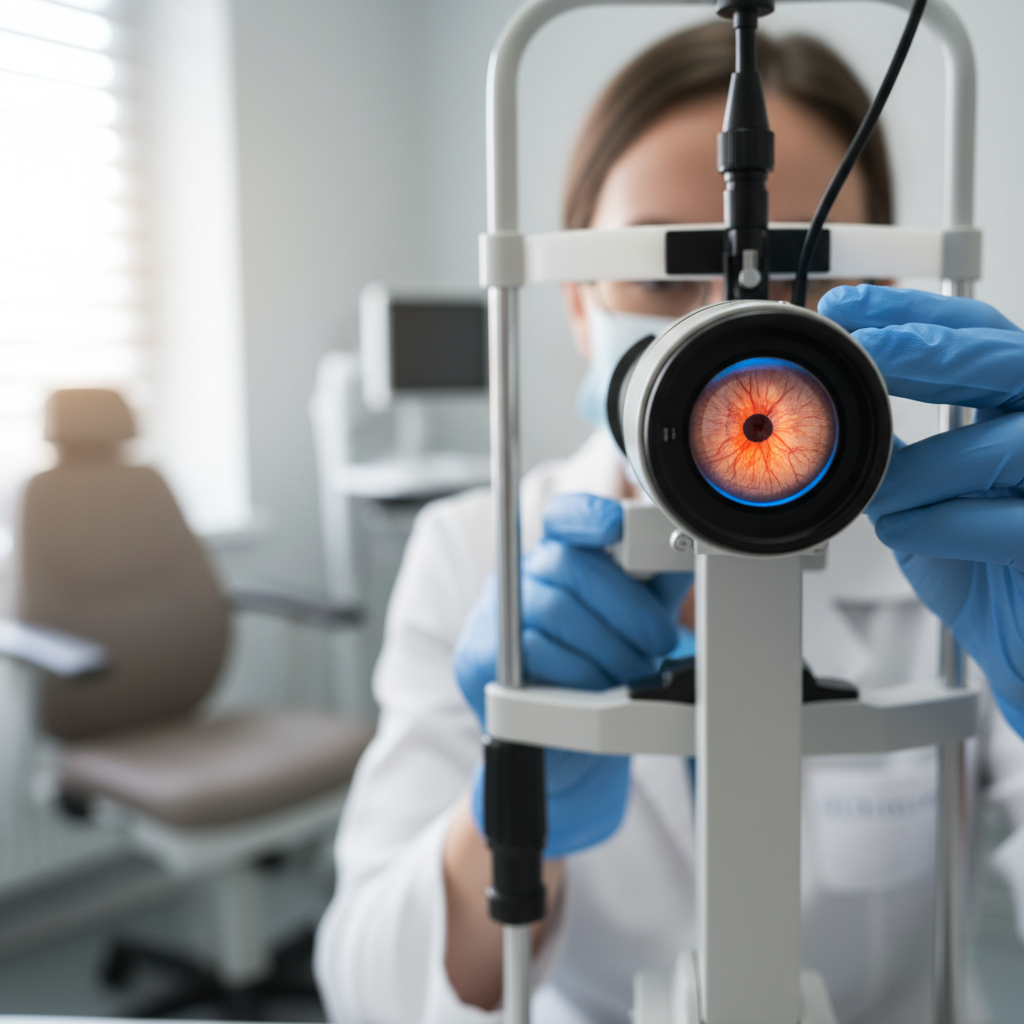
Retinal vein occlusion occurs when blood clots block the central retinal vein or its branches, causing sudden vision loss and serving as an important indicator of underlying cardiovascular disease and thrombotic risk. This condition typically affects individuals with cardiovascular risk factors such as hypertension, diabetes, hyperlipidemia, and hypercoagulable states, and its occurrence often signals the need for comprehensive cardiovascular evaluation and risk stratification. Patients with retinal vein occlusion experience sudden, painless vision loss that may range from mild blurring to severe visual impairment, depending on the location and extent of the venous blockage, and the affected eye may show characteristic findings including retinal hemorrhages, cotton wool spots, and macular edema. The visual symptoms can include central vision loss, peripheral vision defects, distorted vision, and difficulty with reading or detailed visual tasks, and recovery depends on the promptness of treatment and the development of collateral circulation. Central retinal vein occlusion typically causes more severe vision loss than branch retinal vein occlusion, and both conditions can lead to serious complications including neovascular glaucoma and retinal detachment if left untreated. The occurrence of retinal vein occlusion significantly increases the risk of future cardiovascular events, including stroke and myocardial infarction, making it essential to evaluate and treat underlying cardiovascular risk factors aggressively. Treatment may include intravitreal injections to reduce macular edema, laser therapy to prevent neovascularization, and systemic interventions to address cardiovascular risk factors and prevent future thrombotic events.
7. Anterior Ischemic Optic Neuropathy - Optic Nerve Circulation Crisis
Anterior ischemic optic neuropathy (AION) represents a serious cardiovascular-related condition where inadequate blood supply to the optic nerve head results in sudden, painless vision loss and serves as a marker for significant systemic vascular disease. This condition occurs in two primary forms: arteritic AION, associated with giant cell arteritis and requiring immediate treatment to prevent bilateral blindness, and non-arteritic AION, linked to cardiovascular risk factors such as hypertension, diabetes, and sleep apnea. Patients with AION typically experience sudden onset of painless vision loss upon awakening, often described as a curtain or shadow blocking part of their visual field, and this vision loss is usually permanent and may progress over days to weeks. The visual field defects in AION characteristically respect the horizontal meridian, creating superior or inferior visual field cuts that can significantly impact daily activities such as reading, driving, and navigating stairs. Non-arteritic AION often occurs in individuals with small, crowded optic discs and cardiovascular risk factors, suggesting that compromised microcirculation to the optic nerve head plays a crucial role in its development. The occurrence of AION, particularly the non-arteritic form, should prompt comprehensive cardiovascular evaluation, including assessment of blood pressure control, diabetes management, sleep apnea screening, and evaluation for other vascular risk factors. While treatment options for established AION are limited, aggressive management of cardiovascular risk factors is essential to prevent fellow eye involvement and reduce the risk of future cardiovascular events, as patients with AION face increased risks of stroke and other vascular complications.
8. Corneal Arcus - Lipid Metabolism and Vascular Risk

Corneal arcus, appearing as a white, gray, or yellowish ring around the corneal periphery, represents a visible accumulation of lipid deposits that can serve as an important early warning sign for cardiovascular disease, particularly in younger individuals. This condition, also known as arcus senilis when occurring in elderly patients, results from the deposition of cholesterol and other lipids in the corneal stroma and may indicate underlying dyslipidemia and increased cardiovascular risk. While corneal arcus is common in elderly individuals and may not carry significant cardiovascular implications in this population, its presence in individuals under 50 years of age strongly suggests underlying lipid metabolism disorders and warrants comprehensive cardiovascular risk assessment. Patients with corneal arcus typically do not experience visual symptoms related to the lipid deposits themselves, as the central cornea remains clear and visual acuity is preserved, but the condition may be accompanied by other signs of dyslipidemia such as xanthelasma or tendon xanthomas. The presence of corneal arcus in younger individuals has been associated with increased risks of coronary artery disease, stroke, and peripheral vascular disease, making it an important clinical finding that should prompt lipid screening and cardiovascular evaluation. Studies have demonstrated that individuals with premature corneal arcus often have elevated cholesterol levels, particularly LDL cholesterol, and may benefit from aggressive lipid-lowering therapy and lifestyle modifications to reduce cardiovascular risk. The detection of corneal arcus during routine eye examination provides an opportunity for early intervention and cardiovascular risk reduction, potentially preventing future heart attacks, strokes, and other cardiovascular complications through appropriate medical management and lifestyle changes.
9. Integrating Ocular Findings into Cardiovascular Care

The recognition and understanding of these eight cardiovascular conditions with early visual warning signs represents a paradigm shift in preventive healthcare, emphasizing the critical importance of comprehensive eye examinations as part of routine cardiovascular risk assessment and disease prevention strategies. The eye's unique anatomy provides an unparalleled window into the body's vascular health, allowing for direct visualization of blood vessels, detection of embolic phenomena, and assessment of microvascular damage that mirrors systemic cardiovascular pathology. Healthcare providers and patients alike must recognize that visual symptoms and ocular findings often precede traditional cardiovascular symptoms, providing crucial opportunities for early intervention and disease prevention that can save both sight and life. The integration of ophthalmologic findings into cardiovascular risk stratification enhances our ability to identify high-risk individuals, guide treatment decisions, and monitor the effectiveness of therapeutic interventions, ultimately improving patient outcomes and reducing the burden of cardiovascular disease. Regular comprehensive eye examinations, particularly for individuals with known cardiovascular risk factors such as diabetes, hypertension, and hyperlipidemia, should be considered an essential component of preventive healthcare rather than merely a vision screening tool. As our understanding of the eye-heart connection continues to evolve, emerging technologies such as retinal imaging, optical coherence tomography, and artificial intelligence-assisted diagnosis promise to further enhance our ability to detect and monitor cardiovascular disease through ocular examination. The future of cardiovascular medicine will likely see increased collaboration between ophthalmologists, cardiologists, and primary care physicians, working together to leverage the diagnostic power of the eye in the fight against heart disease, stroke, and other vascular conditions that continue to be leading causes of morbidity and mortality worldwide.