12 Respiratory Conditions With Physical Signs Beyond Coughing
While coughing remains the most recognizable symptom of respiratory disease, the human respiratory system's complexity manifests through a diverse spectrum of physical signs that often precede or accompany traditional pulmonary symptoms. Healthcare professionals and patients alike must develop a keen awareness of these subtle yet significant indicators, as they frequently provide crucial diagnostic clues and may signal serious underlying conditions requiring immediate intervention. From the distinctive clubbing of fingertips that suggests chronic hypoxemia to the paradoxical breathing patterns that indicate respiratory muscle fatigue, these physical manifestations serve as windows into the intricate workings of our respiratory apparatus. Understanding these signs becomes particularly critical in early disease detection, as many respiratory conditions present with systemic symptoms before classic pulmonary signs emerge. This comprehensive exploration delves into twelve distinct respiratory conditions that demonstrate how the body's response to compromised breathing extends far beyond the lungs themselves, affecting cardiovascular function, neurological status, musculoskeletal alignment, and even dermatological appearance. By recognizing these interconnected physical signs, we can better appreciate the respiratory system's integral role in maintaining overall physiological homeostasis and identify potentially life-threatening conditions before they progress to irreversible stages.
1. Pulmonary Embolism - The Silent Cardiovascular Crisis

Pulmonary embolism represents one of the most deceptive respiratory emergencies, often presenting with cardiovascular and neurological signs that overshadow traditional respiratory symptoms. The classic triad of chest pain, dyspnea, and hemoptysis occurs in fewer than 20% of cases, making recognition challenging for even experienced clinicians. Instead, patients frequently exhibit tachycardia as the most consistent finding, with heart rates exceeding 100 beats per minute in approximately 70% of cases. The cardiovascular system responds to acute pulmonary vascular obstruction by increasing cardiac output, leading to palpitations, anxiety, and a sense of impending doom that patients describe as distinctly different from typical shortness of breath. Cyanosis may appear around the lips and fingertips, particularly during minimal exertion, while jugular venous distension becomes evident as right heart strain develops. Perhaps most significantly, many patients experience sudden onset of confusion, lightheadedness, or syncope due to decreased cardiac output and subsequent cerebral hypoperfusion. The skin may become diaphoretic and cool to touch, reflecting the body's sympathetic response to cardiovascular compromise. Lower extremity examination often reveals unilateral swelling, warmth, or tenderness, particularly in the calf region, indicating the source of the embolic material. These systemic manifestations underscore how pulmonary embolism affects multiple organ systems simultaneously, requiring healthcare providers to maintain high clinical suspicion even when classic respiratory symptoms are absent.
2. Pneumothorax - When Breathing Mechanics Fail

Spontaneous pneumothorax creates a unique constellation of physical signs that reflect the mechanical disruption of normal respiratory physiology, often manifesting through postural and movement-related symptoms that patients may not immediately associate with lung problems. The hallmark presentation involves sudden, sharp, unilateral chest pain that patients describe as "stabbing" or "tearing," typically occurring at rest or during minimal activity in young, tall, thin individuals. This pain characteristically worsens with deep inspiration and often radiates to the shoulder on the affected side due to phrenic nerve irritation. Patients instinctively adopt protective posturing, leaning toward the affected side and avoiding movements that expand the chest wall, creating an asymmetrical appearance during respiration. The affected hemithorax demonstrates reduced or absent chest wall movement during inspiration, while the unaffected side may show compensatory increased excursion. Tactile examination reveals decreased vocal fremitus and a hyperresonant percussion note over the pneumothorax, while auscultation demonstrates diminished or absent breath sounds. In larger pneumothoraces, tracheal deviation away from the affected side becomes apparent, and patients may develop subcutaneous emphysema, creating a distinctive crackling sensation under the skin around the neck and chest wall. The cardiovascular system responds with tachycardia and, in tension pneumothorax, signs of obstructive shock including hypotension, elevated jugular venous pressure, and paradoxical pulse. These mechanical disruptions highlight how pneumothorax affects not just gas exchange but the entire thoracic pump mechanism essential for both respiratory and cardiovascular function.
3. Chronic Obstructive Pulmonary Disease (COPD) - The Systemic Inflammatory Response
COPD exemplifies how chronic respiratory conditions extend their impact throughout the body, creating a complex web of physical manifestations that reflect both local pulmonary changes and systemic inflammatory processes. The characteristic "barrel chest" deformity develops gradually as chronic air trapping increases the anteroposterior diameter of the thorax, forcing patients to adopt accessory muscle breathing patterns that become increasingly evident during routine activities. Patients demonstrate pursed-lip breathing, a compensatory mechanism that creates positive end-expiratory pressure to prevent small airway collapse, while simultaneously exhibiting the classic "tripod position" – sitting forward with arms supported to optimize accessory muscle function. Digital clubbing, though more commonly associated with other respiratory conditions, may develop in advanced COPD, particularly when complicated by chronic hypoxemia or concurrent conditions like lung cancer. The neck muscles, particularly the sternocleidomastoid and scalene groups, become hypertrophied from chronic overuse, creating a distinctive muscular appearance in the neck and upper chest region. Peripheral edema often develops due to cor pulmonale, the right heart failure that results from chronic pulmonary hypertension, while jugular venous distension becomes apparent during exacerbations. Patients frequently exhibit weight loss and muscle wasting, particularly in the upper extremities and temporal regions, reflecting the increased metabolic demands of labored breathing and chronic systemic inflammation. The skin may appear dusky or cyanotic, especially around the lips and nail beds, while polycythemia secondary to chronic hypoxemia can create a ruddy facial complexion. These multisystem manifestations demonstrate how COPD functions as a systemic inflammatory disease rather than merely a localized pulmonary condition.
4. Asthma - The Dynamic Respiratory Response

Asthma presents with a unique pattern of physical signs that fluctuate dramatically based on disease severity and trigger exposure, creating diagnostic challenges when patients are evaluated between acute episodes. During acute exacerbations, patients exhibit visible accessory muscle use, with prominent contraction of the sternocleidomastoid, scalene, and intercostal muscles creating a characteristic appearance of respiratory distress. The suprasternal, supraclavicular, and intercostal spaces demonstrate prominent retractions during inspiration, particularly evident in children and thin adults. Patients often assume the classic "tripod position," sitting upright and leaning forward with hands on knees or a table to maximize mechanical advantage of accessory respiratory muscles. The expiratory phase becomes prolonged and labored, with patients demonstrating pursed-lip breathing and audible wheezing that may be heard without a stethoscope. Paradoxical pulse, defined as a drop in systolic blood pressure greater than 10 mmHg during inspiration, becomes pronounced during severe attacks and serves as an important indicator of attack severity. The skin may appear diaphoretic and pale, with circumoral cyanosis developing as hypoxemia progresses. Anxiety and agitation frequently accompany severe attacks, reflecting both the psychological stress of dyspnea and the physiological effects of hypoxemia and hypercarbia. Between attacks, patients may appear completely normal, though careful examination might reveal subtle signs such as allergic shiners (dark circles under the eyes), nasal polyps, or eczematous skin changes that suggest underlying atopic disease. The dynamic nature of these physical findings emphasizes the importance of recognizing asthma as a variable condition requiring assessment of both acute presentation and baseline functional status.
5. Interstitial Lung Disease - The Progressive Fibrotic Process

Interstitial lung diseases encompass a diverse group of conditions that share common physical manifestations reflecting the progressive scarring and stiffening of lung parenchyma, creating distinctive signs that often develop insidiously over months to years. Digital clubbing represents the most characteristic and earliest physical sign, occurring in approximately 50-70% of patients with idiopathic pulmonary fibrosis and serving as an important prognostic indicator. The clubbing typically develops gradually, beginning with loss of the normal angle between the nail and nail bed, progressing to increased curvature of the nails and eventual enlargement of the fingertip pulp. Fine, dry, inspiratory crackles, often described as "velcro-like," become audible at the lung bases and represent the sound of small airways and alveoli opening during inspiration against increased surface tension. These crackles characteristically persist despite coughing and may be the earliest auscultatory finding in disease progression. Patients develop a rapid, shallow breathing pattern as lung compliance decreases, with respiratory rates often elevated even at rest due to the increased work of breathing required to maintain adequate ventilation. The chest wall may appear to have reduced expansion, particularly in the lower regions where fibrosis typically predominates, while percussion reveals decreased resonance over affected areas. As the disease progresses, signs of pulmonary hypertension and cor pulmonale develop, including elevated jugular venous pressure, peripheral edema, and a prominent pulmonary component of the second heart sound. Patients often exhibit exercise intolerance that seems disproportionate to their apparent respiratory distress at rest, reflecting the inability of fibrotic lungs to increase gas exchange during periods of increased metabolic demand. The insidious nature of these physical changes often leads to delayed diagnosis, emphasizing the importance of recognizing subtle early signs in at-risk populations.
6. Sleep Apnea - The Nocturnal Respiratory Disruption

Obstructive sleep apnea creates a distinctive pattern of physical signs that reflect both the mechanical obstruction of upper airways during sleep and the systemic consequences of chronic intermittent hypoxemia, often presenting with manifestations that patients and healthcare providers may not immediately connect to respiratory pathology. The most obvious physical characteristic involves upper airway anatomy, with patients typically demonstrating a thick neck (circumference >17 inches in men, >16 inches in women), retrognathia or micrognathia, macroglossia, and enlarged tonsils or uvula that contribute to airway narrowing during sleep. Facial morphology often includes a high, arched palate and crowded oropharynx, while nasal examination may reveal septal deviation, turbinate hypertrophy, or chronic congestion that forces mouth breathing. The cardiovascular system bears significant impact from repeated episodes of hypoxemia and arousal, leading to systemic hypertension that may be refractory to standard antihypertensive therapy, particularly elevated morning blood pressure readings. Patients frequently exhibit signs of right heart strain, including peripheral edema, elevated jugular venous pressure, and hepatomegaly, reflecting the development of pulmonary hypertension from chronic hypoxemic episodes. Neurological manifestations include morning headaches, cognitive impairment, and excessive daytime sleepiness that may be observed during clinical encounters as frequent yawning, difficulty maintaining attention, or actually falling asleep during conversations. The skin may appear chronically fatigued with dark circles under the eyes, while patients often demonstrate irritability, mood changes, and decreased libido reflecting the systemic effects of sleep fragmentation. Gastroesophageal reflux symptoms frequently accompany sleep apnea due to the negative intrathoracic pressures generated during obstructive episodes, creating additional physical discomfort that compounds the overall clinical picture.
7. Lung Cancer - The Malignant Respiratory Transformation
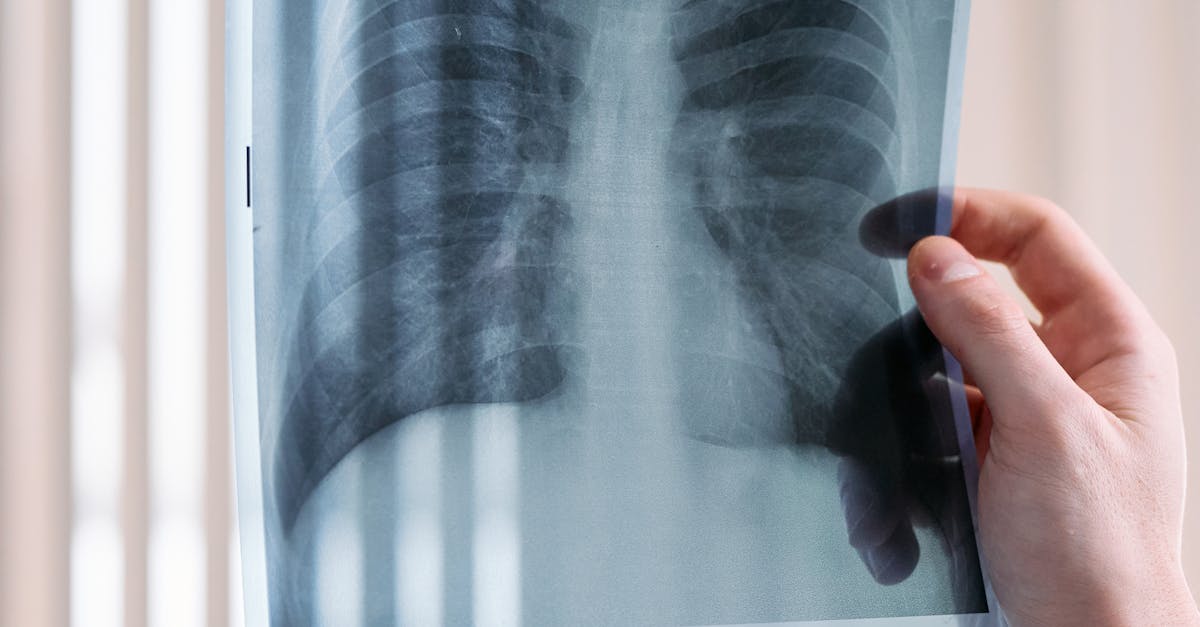
Lung cancer presents with an array of physical signs that extend far beyond the respiratory system, reflecting both local tumor effects and paraneoplastic syndromes that can affect virtually every organ system in the body. Superior vena cava syndrome, occurring in approximately 10-15% of lung cancer patients, creates a distinctive constellation of signs including facial and upper extremity edema, prominent superficial chest wall veins, and jugular venous distension that fails to vary with respiration. The face may appear plethoric and swollen, particularly around the eyes, while patients complain of a sensation of head fullness that worsens when bending forward or lying flat. Horner's syndrome, resulting from invasion of the sympathetic chain by apical tumors (Pancoast tumors), manifests as unilateral ptosis, miosis, and anhidrosis, often accompanied by severe shoulder and arm pain that radiates in an ulnar distribution. Digital clubbing develops in approximately 30% of lung cancer patients, typically appearing more rapidly than in benign conditions and sometimes accompanied by hypertrophic pulmonary osteoarthropathy, causing painful swelling of wrists, ankles, and knees. Paraneoplastic syndromes create diverse physical manifestations including the syndrome of inappropriate antidiuretic hormone secretion (SIADH), leading to hyponatremia with associated confusion, weakness, and altered mental status. Hypercalcemia from parathyroid hormone-related protein secretion causes muscle weakness, altered mental status, and cardiac arrhythmias, while Lambert-Eaton myasthenic syndrome produces proximal muscle weakness that improves with repeated muscle contraction. Skin manifestations may include acanthosis nigricans, dermatomyositis, or thrombophlebitis migrans, while neurological paraneoplastic syndromes can cause cerebellar ataxia, peripheral neuropathy, or limbic encephalitis. These diverse manifestations underscore the importance of maintaining high clinical suspicion for lung cancer in patients presenting with seemingly unrelated systemic symptoms.
8. Pneumonia - The Infectious Respiratory Response

Pneumonia demonstrates how infectious respiratory processes create systemic inflammatory responses that manifest through multiple organ systems, often presenting with physical signs that may overshadow traditional pulmonary symptoms, particularly in elderly or immunocompromised patients. The classic presentation includes fever, chills, and rigors, but the systemic inflammatory response syndrome (SIRS) can produce more subtle signs such as altered mental status, particularly confusion or delirium in elderly patients, which may be the primary presenting complaint. Cardiovascular manifestations include tachycardia that persists despite fever reduction, hypotension indicating possible septic shock, and signs of increased cardiac output such as bounding pulses and warm extremities in early sepsis. The skin may demonstrate poor capillary refill, mottling, or peripheral cyanosis as sepsis progresses, while some patients develop a characteristic heliotrope rash around the eyes or erythema migrans-like lesions with certain atypical pathogens. Gastrointestinal symptoms frequently accompany pneumonia, including nausea, vomiting, diarrhea, and abdominal pain that may lead to misdiagnosis as gastroenteritis, particularly with Legionella or atypical pneumonia. Neurological signs beyond altered mental status may include headache, neck stiffness (without true meningitis), and photophobia, while some patients develop seizures or focal neurological deficits due to septic emboli or metabolic derangements. Laboratory manifestations visible through physical examination include jaundice from hemolysis or hepatic dysfunction, petechiae or purpura from thrombocytopenia or disseminated intravascular coagulation, and lymphadenopathy in cases of atypical pneumonia. The musculoskeletal system may show signs of myositis with muscle tenderness and weakness, while joint pain and swelling can occur with certain pathogens, emphasizing how pneumonia functions as a systemic disease rather than merely a localized pulmonary infection.
9. Pulmonary Hypertension - The Elevated Pressure Syndrome
Pulmonary hypertension creates a distinctive pattern of physical signs that primarily reflect right heart adaptation to chronically elevated pulmonary vascular pressures, often developing insidiously over years before becoming clinically apparent. The cardiovascular examination reveals a prominent pulmonary component of the second heart sound (P2) that may be palpable over the pulmonary area, while a right ventricular heave becomes apparent along the left sternal border as right heart hypertrophy develops. Jugular venous pressure elevation with prominent 'a' waves reflects decreased right ventricular compliance, while the development of tricuspid regurgitation creates a holosystolic murmur that increases with inspiration and may be accompanied by hepatic pulsations. As right heart failure progresses, patients develop peripheral edema that typically begins in the ankles and progresses proximally, accompanied by hepatomegaly that may be tender and pulsatile. Ascites may develop in advanced cases, while hepatojugular reflux becomes positive as venous return increases with abdominal compression. The skin often appears dusky or cyanotic, particularly around the lips, fingertips, and nail beds, reflecting chronic hypoxemia and reduced cardiac output. Digital clubbing may develop, particularly in patients with congenital heart disease or chronic hypoxemic conditions causing pulmonary hypertension. Patients frequently exhibit exercise intolerance that seems disproportionate to their apparent respiratory status, with syncope or near-syncope occurring during exertion as cardiac output fails to increase appropriately. The neck veins may show prominent v waves if significant tricuspid regurgitation develops, while the liver may become enlarged and pulsatile. In severe cases, patients may develop signs of low cardiac output including cool extremities, delayed capillary refill, and altered mental status, particularly during exertion or stress when the fixed cardiac output cannot meet metabolic demands.
10. Sarcoidosis - The Multisystem Granulomatous Disease
Sarcoidosis exemplifies how respiratory conditions can manifest as multisystem diseases, with physical signs affecting virtually every organ system and often presenting with extrapulmonary manifestations that precede or overshadow pulmonary symptoms. Dermatological manifestations represent some of the most recognizable signs, including erythema nodosum, which appears as tender, raised, reddish nodules typically on the anterior