8 Joint Pain Locations and Their Associated Conditions
# 8 Joint Pain Locations and Their Associated Conditions: A Comprehensive Guide to Understanding Your Body's Warning Signals
Joint pain represents one of the most common yet complex health complaints affecting millions of people worldwide, serving as a crucial indicator of underlying conditions that range from temporary inflammation to chronic degenerative diseases. Understanding the specific location of joint pain and its associated symptoms can provide invaluable insights into potential diagnoses, enabling both patients and healthcare providers to develop more targeted treatment approaches. Each joint in the human body has unique anatomical structures, biomechanical functions, and vulnerability patterns that influence the types of conditions that commonly affect them. From the weight-bearing responsibilities of knee and hip joints to the intricate movements of finger and wrist joints, different locations experience distinct stressors and wear patterns throughout our lives. This comprehensive exploration examines eight critical joint pain locations, delving into the specific conditions commonly associated with each area, their underlying mechanisms, risk factors, and the interconnected nature of joint health throughout the musculoskeletal system. By recognizing these patterns and understanding the relationship between location-specific pain and potential conditions, individuals can better advocate for their health and work collaboratively with medical professionals to achieve optimal outcomes.
1. Knee Joint Pain - The Weight-Bearer's Burden
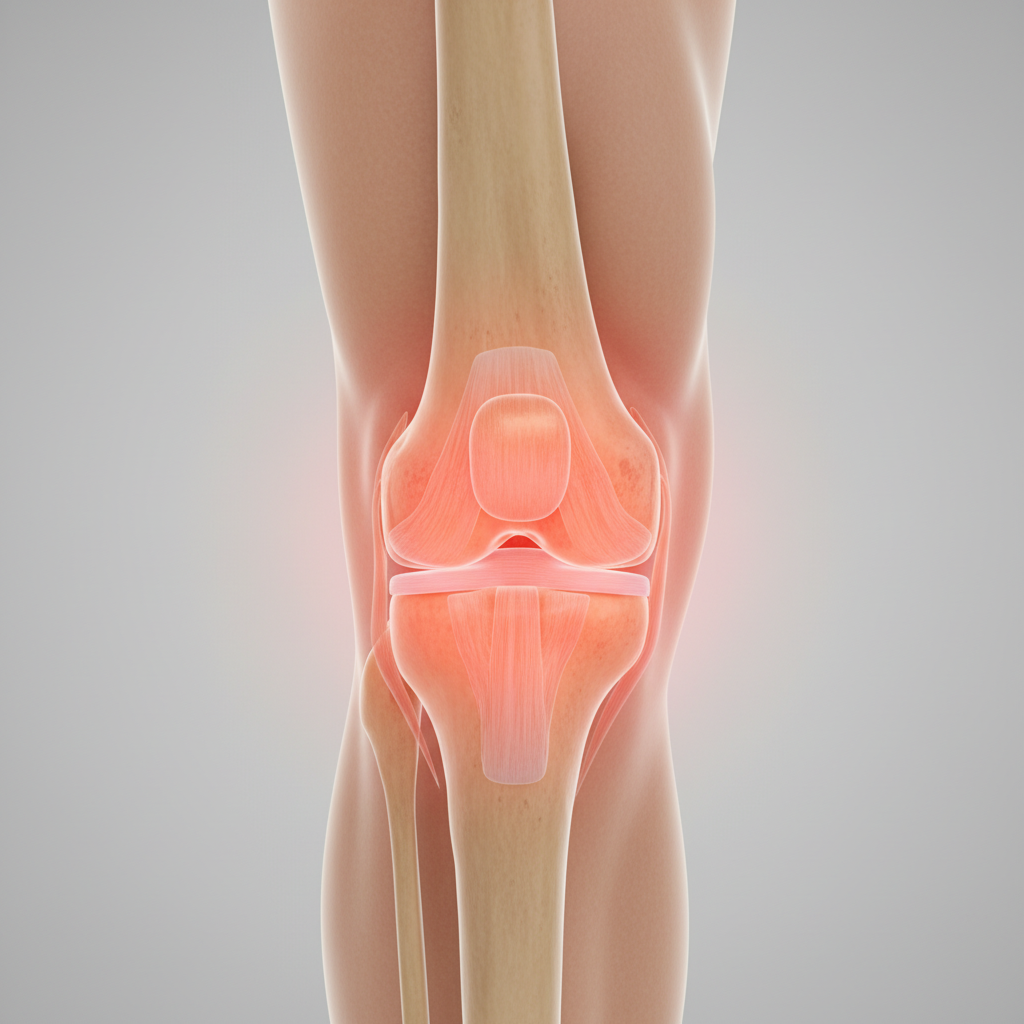
The knee joint, being the largest and most complex joint in the human body, bears the brunt of our daily activities and is consequently susceptible to a wide array of painful conditions that can significantly impact mobility and quality of life. Osteoarthritis stands as the most prevalent condition affecting the knee, particularly in individuals over 50, where the gradual breakdown of cartilage leads to bone-on-bone contact, resulting in pain, stiffness, and reduced range of motion. Athletes and active individuals frequently encounter meniscal tears, where the C-shaped cartilage discs that cushion the joint become damaged through sudden twisting motions or degenerative changes over time. Patellofemoral pain syndrome, commonly known as "runner's knee," affects the area around the kneecap and often results from muscle imbalances, overuse, or biomechanical issues that alter the tracking of the patella during movement. Rheumatoid arthritis can also target the knee joint, causing inflammatory pain, swelling, and potential joint deformity if left untreated. Additionally, conditions such as bursitis, ligament injuries (including ACL and MCL tears), and Baker's cysts can contribute to knee pain, each presenting with distinct symptom patterns and requiring specific diagnostic approaches and treatment strategies.
2. Hip Joint Pain - The Foundation of Movement
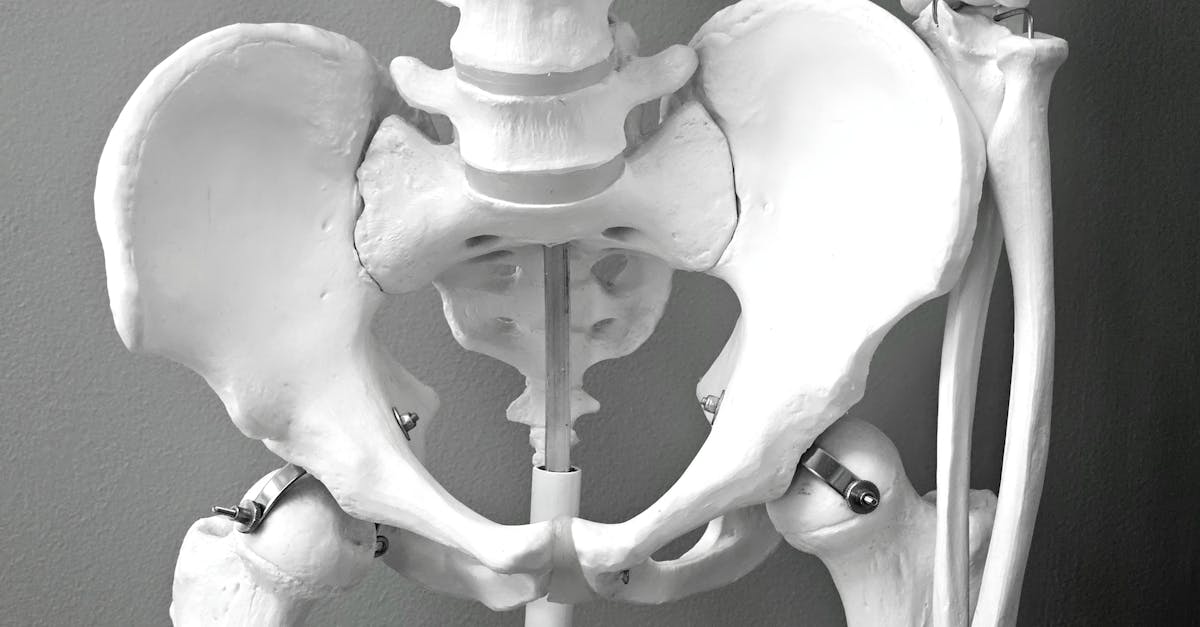
Hip joint pain represents a complex diagnostic challenge due to the joint's deep anatomical location and its critical role in supporting body weight while facilitating a wide range of movements essential for daily activities. Osteoarthritis of the hip typically develops gradually, causing deep, aching pain in the groin area that may radiate to the buttock or thigh, often accompanied by morning stiffness and difficulty with activities such as putting on shoes or getting in and out of cars. Hip impingement syndrome, also known as femoroacetabular impingement (FAI), occurs when abnormal bone growth creates friction between the femoral head and acetabulum, leading to pain during hip flexion and potentially contributing to early arthritis development. Trochanteric bursitis affects the fluid-filled sacs on the outer aspect of the hip, causing sharp, burning pain that worsens with lying on the affected side or climbing stairs. Labral tears, involving the ring of cartilage that surrounds the hip socket, can cause catching sensations, deep groin pain, and clicking sounds during movement. Hip fractures, particularly common in elderly individuals with osteoporosis, present as severe pain and inability to bear weight, requiring immediate medical attention. Other conditions such as avascular necrosis, where blood supply to the femoral head is compromised, and various forms of inflammatory arthritis can also manifest as hip pain with distinct clinical presentations.
3. Shoulder Joint Pain - The Price of Mobility
The shoulder joint's remarkable range of motion comes at the cost of stability, making it particularly vulnerable to a diverse spectrum of painful conditions that can severely limit upper extremity function and impact daily activities. Rotator cuff injuries, including tears and tendinitis, represent the most common source of shoulder pain, typically manifesting as deep, aching discomfort that worsens with overhead activities and may disturb sleep when lying on the affected side. Frozen shoulder, or adhesive capsulitis, involves progressive stiffening of the joint capsule, leading to severe pain and dramatic loss of range of motion that can persist for months or even years without proper treatment. Shoulder impingement syndrome occurs when tendons become compressed between bone structures during arm elevation, causing pain and weakness that particularly affects reaching and lifting motions. Glenohumeral arthritis, whether osteoarthritic or inflammatory in nature, can cause deep joint pain, stiffness, and grinding sensations during movement. Acromioclavicular (AC) joint arthritis affects the connection between the collarbone and shoulder blade, typically causing localized pain at the top of the shoulder that worsens with cross-body movements. Biceps tendinitis and labral tears can also contribute to shoulder pain, each presenting with characteristic symptoms and requiring specific diagnostic techniques and treatment approaches to achieve optimal outcomes.
4. Lower Back Joint Pain - The Spine's Silent Struggle

Lower back pain involving the facet joints and sacroiliac joints represents one of the most prevalent and debilitating musculoskeletal complaints, affecting millions of individuals and serving as a leading cause of disability worldwide. Facet joint arthritis, also known as spondylosis, develops when the small joints that connect adjacent vertebrae become inflamed and degenerated, causing localized back pain that typically worsens with extension and rotation movements. Sacroiliac joint dysfunction affects the connection between the spine and pelvis, often presenting as unilateral lower back pain that may radiate into the buttock and posterior thigh, frequently mimicking sciatica symptoms. Degenerative disc disease, while primarily affecting the intervertebral discs, can lead to secondary facet joint problems as the spine attempts to compensate for lost disc height and stability. Spondylolisthesis, where one vertebra slips forward over another, can cause both mechanical back pain and nerve compression symptoms, depending on the degree of slippage and associated spinal stenosis. Inflammatory conditions such as ankylosing spondylitis can affect the spine's joints, causing morning stiffness, pain that improves with movement, and potential fusion of spinal segments over time. Muscle spasms, ligament strains, and myofascial pain syndromes can also contribute to lower back discomfort, often developing as secondary responses to underlying joint dysfunction or as primary conditions resulting from overuse, poor posture, or acute injury.
5. Wrist and Hand Joint Pain - Precision Under Pressure

The intricate network of joints in the wrist and hand enables the fine motor control essential for countless daily activities, making pain in these areas particularly disruptive to functional independence and occupational performance. Carpal tunnel syndrome, caused by compression of the median nerve as it passes through the wrist, typically produces numbness, tingling, and pain in the thumb, index, middle, and half of the ring finger, often worsening at night or with repetitive hand activities. Rheumatoid arthritis commonly affects the small joints of the hands and wrists, causing symmetrical pain, swelling, and morning stiffness that can progress to joint deformity and functional impairment if not adequately treated. Osteoarthritis of the hand frequently targets the base of the thumb (carpometacarpal joint), the proximal interphalangeal joints, and the distal interphalangeal joints, leading to pain, stiffness, and the development of characteristic bony enlargements called Heberden's and Bouchard's nodes. De Quervain's tenosynovitis affects the tendons on the thumb side of the wrist, causing pain that worsens with thumb movement and gripping activities. Trigger finger involves inflammation of the tendon sheaths in the fingers, leading to catching or locking sensations during finger flexion and extension. Ganglion cysts, while typically benign, can cause pain and functional limitations when they compress nearby nerves or interfere with joint movement, requiring careful evaluation to distinguish them from other more serious conditions.
6. Ankle Joint Pain - Stability Meets Mobility

The ankle joint complex, consisting of the tibiotalar joint and subtalar joint, must balance the competing demands of providing stable weight-bearing support while maintaining sufficient mobility for walking, running, and navigating uneven terrain. Ankle sprains, particularly involving the lateral ligaments, represent the most common ankle injury, often resulting in acute pain, swelling, and instability that can lead to chronic problems if not properly rehabilitated. Post-traumatic arthritis frequently develops following ankle fractures or severe sprains, causing ongoing pain, stiffness, and functional limitations that may require surgical intervention in severe cases. Achilles tendinitis and tendon ruptures affect the powerful tendon connecting the calf muscles to the heel bone, causing posterior ankle pain that worsens with activity and may present as a sudden, severe pain with complete ruptures. Tarsal tunnel syndrome involves compression of the posterior tibial nerve as it passes behind the medial malleolus, causing burning pain, numbness, and tingling in the sole of the foot that may worsen with prolonged standing or walking. Subtalar joint arthritis can develop following calcaneal fractures or as part of systemic inflammatory conditions, causing deep, aching pain in the hindfoot that worsens with walking on uneven surfaces. Peroneal tendon disorders, including tendinitis and tears, can cause lateral ankle pain and instability, particularly in athletes involved in cutting and pivoting sports.
7. Elbow Joint Pain - The Hinge Under Stress

The elbow joint's primary function as a hinge joint, combined with its role in forearm rotation, subjects it to repetitive stresses that can lead to various overuse injuries and degenerative conditions affecting both recreational and occupational activities. Lateral epicondylitis, commonly known as tennis elbow, involves inflammation of the tendons that attach to the lateral epicondyle, causing pain on the outside of the elbow that worsens with gripping activities and wrist extension. Medial epicondylitis, or golfer's elbow, affects the tendons on the inside of the elbow, typically causing pain that radiates down the forearm and worsens with wrist flexion and pronation movements. Olecranon bursitis, often called "student's elbow" or "draftsman's elbow," involves inflammation of the bursa at the tip of the elbow, causing swelling and pain that may be associated with prolonged leaning on hard surfaces. Cubital tunnel syndrome occurs when the ulnar nerve becomes compressed as it passes around the medial aspect of the elbow, causing numbness and tingling in the ring and little fingers, along with potential weakness in hand grip strength. Elbow arthritis, whether post-traumatic or degenerative, can cause pain, stiffness, and loss of range of motion that particularly affects reaching and lifting activities. Radial tunnel syndrome involves compression of the posterior interosseous nerve, causing deep, aching pain in the forearm that may be mistaken for lateral epicondylitis but typically does not respond to standard tennis elbow treatments.
8. Neck Joint Pain - The Delicate Balance of Support and Movement

The cervical spine's complex arrangement of facet joints, intervertebral discs, and supporting structures must provide both stability for the head and remarkable mobility for visual and auditory orientation, making it susceptible to various painful conditions that can significantly impact daily function. Cervical facet joint arthritis commonly develops with age or following whiplash injuries, causing localized neck pain that may radiate to the shoulders and upper back, typically worsening with neck extension and rotation movements. Cervical disc herniation can cause not only local neck pain but also radicular symptoms extending into the arms and hands, depending on which nerve roots are affected by the protruding disc material. Cervical spinal stenosis involves narrowing of the spinal canal, potentially causing myelopathy symptoms such as hand clumsiness, gait difficulties, and neck pain that may be accompanied by neurological deficits. Atlantoaxial joint dysfunction affects the specialized joint between the first and second cervical vertebrae, often causing suboccipital headaches and neck pain that worsens with head rotation. Torticollis, whether acute or chronic, involves involuntary muscle contractions that cause painful neck positioning and limited range of motion. Cervical muscle strain and myofascial pain syndromes can develop from poor posture, stress, or acute injury, causing widespread neck and shoulder pain that may be accompanied by headaches and upper extremity symptoms. Inflammatory conditions such as rheumatoid arthritis can also affect the cervical spine, potentially causing serious complications if atlantoaxial instability develops.
9. Integrating Knowledge for Better Joint Health Management

Understanding the intricate relationship between joint pain locations and their associated conditions provides a foundation for more effective healthcare decision-making and improved quality of life outcomes for individuals experiencing musculoskeletal discomfort. Each joint's unique anatomical structure, biomechanical function, and vulnerability patterns create distinct clinical presentations that, when properly recognized and understood, can guide appropriate diagnostic workups and treatment strategies. The interconnected nature of the musculoskeletal system means that dysfunction in one area often influences other regions, emphasizing the importance of comprehensive evaluation and holistic treatment approaches that address both local symptoms and systemic factors. Early recognition of joint pain patterns and their potential underlying conditions can facilitate timely intervention, potentially preventing progression to more severe or chronic states that may require more invasive treatments. Healthcare providers and patients alike benefit from this knowledge, as it enables more informed discussions about symptoms, realistic treatment expectations, and appropriate lifestyle modifications that can support long-term joint health. Furthermore, understanding these relationships empowers individuals to take proactive steps in preventing joint problems through appropriate exercise, ergonomic modifications, and risk factor management. As our understanding of joint pathology continues to evolve with advances in medical research and technology, this foundational knowledge of location-specific pain patterns remains crucial for navigating the complex landscape of musculoskeletal health and achieving optimal outcomes through personalized, evidence-based care approaches.