15 Morning Symptom Patterns That Doctors Use to Differentiate Inflammatory Conditions
The early morning hours serve as a critical diagnostic window for physicians seeking to identify and differentiate various inflammatory conditions. During the transition from sleep to wakefulness, the human body undergoes complex physiological changes that can unmask or amplify symptoms of underlying inflammatory processes. This phenomenon occurs due to the natural circadian rhythm of cortisol production, which typically reaches its lowest point during the early morning hours before gradually rising. When cortisol levels are diminished, the body's natural anti-inflammatory mechanisms are temporarily reduced, allowing inflammatory symptoms to manifest more prominently. Medical professionals have long recognized that morning symptom patterns provide invaluable insights into the nature, severity, and specific type of inflammatory condition affecting a patient. These patterns can help distinguish between rheumatoid arthritis, osteoarthritis, fibromyalgia, inflammatory bowel disease, and numerous other conditions that share overlapping symptoms throughout the day. By carefully analyzing the timing, duration, intensity, and specific characteristics of morning symptoms, healthcare providers can make more accurate diagnoses, develop targeted treatment plans, and monitor disease progression more effectively. Understanding these morning diagnostic markers represents a cornerstone of modern inflammatory disease management and continues to evolve as medical research advances.
1. Morning Joint Stiffness Duration - The Rheumatoid Arthritis Signature

The duration of morning joint stiffness stands as one of the most reliable diagnostic indicators for differentiating rheumatoid arthritis from other inflammatory and degenerative joint conditions. In rheumatoid arthritis patients, morning stiffness typically persists for more than one hour, often extending for several hours after awakening, while osteoarthritis-related stiffness generally resolves within 30 minutes of movement. This prolonged stiffness occurs because inflammatory cytokines, particularly tumor necrosis factor-alpha and interleukin-1, accumulate in synovial fluid during periods of inactivity, creating a gel-like consistency that impedes joint movement. The inflammatory process in rheumatoid arthritis involves active synovial membrane inflammation, which produces excess synovial fluid rich in inflammatory mediators that literally "gum up" the joint mechanics overnight. Physicians use this timing distinction as a key criterion in the American College of Rheumatology classification criteria for rheumatoid arthritis diagnosis. Patients often describe this morning stiffness as feeling like their joints are "rusted" or "frozen," requiring significant time and gentle movement to regain normal flexibility. The severity and duration of morning stiffness also correlate with disease activity levels, making it an important marker for monitoring treatment effectiveness. Healthcare providers typically ask patients to track their morning stiffness duration over several weeks to establish patterns and assess response to anti-inflammatory medications or disease-modifying antirheumatic drugs.
2. Symmetrical vs. Asymmetrical Joint Involvement Patterns
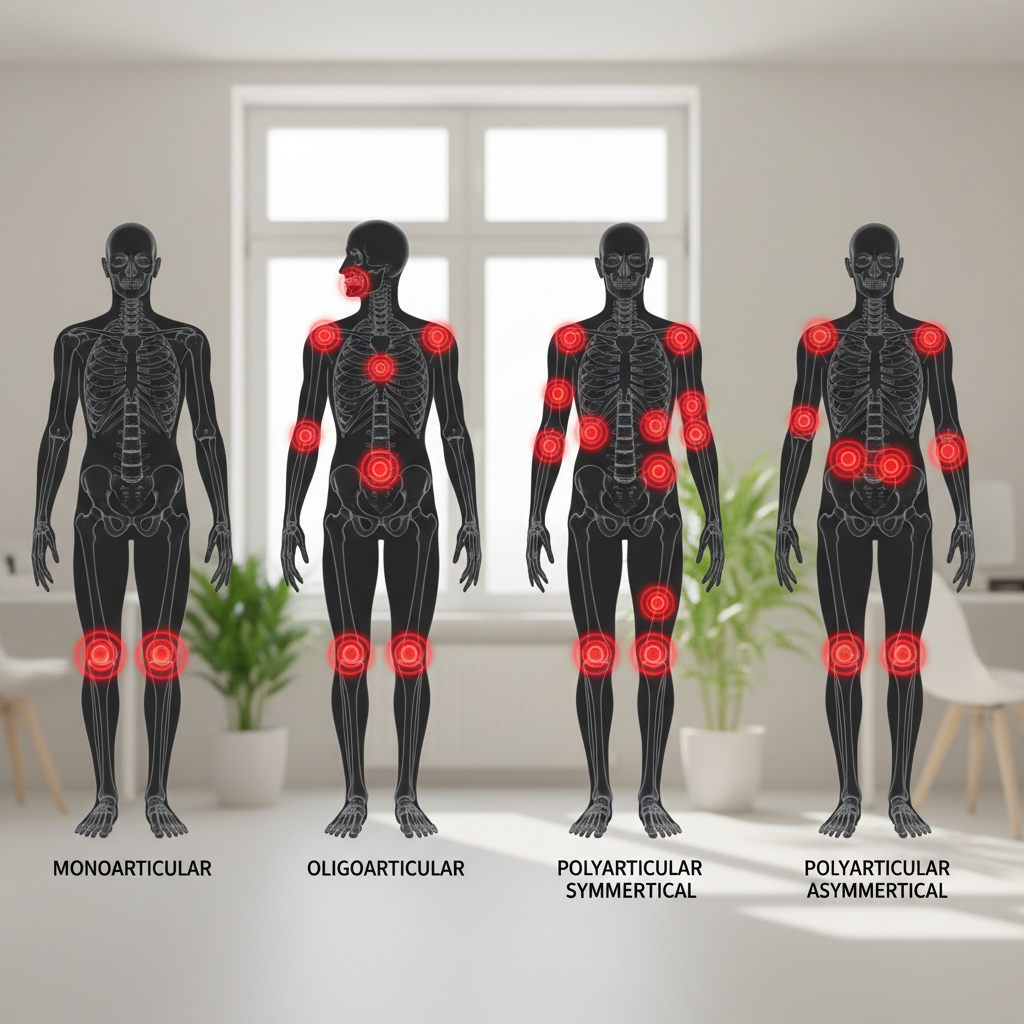
The pattern of joint involvement upon morning awakening provides crucial diagnostic information that helps physicians distinguish between various inflammatory arthropathies. Rheumatoid arthritis characteristically presents with symmetrical joint involvement, meaning that if the right wrist is affected, the left wrist will typically show similar symptoms, creating a mirror-image pattern of inflammation. This symmetrical presentation occurs because rheumatoid arthritis is a systemic autoimmune condition that affects joints through circulating antibodies and inflammatory mediators that target synovial tissue throughout the body. In contrast, psoriatic arthritis often presents with asymmetrical joint involvement, where inflammation may affect joints on one side of the body more severely than the other, or involve completely different joint groups on each side. Osteoarthritis, while not primarily inflammatory, can cause morning symptoms in weight-bearing joints and typically follows patterns related to previous injuries or mechanical stress rather than symmetrical distribution. Physicians conduct systematic joint examinations during morning appointments to document which specific joints are affected, noting swelling, tenderness, warmth, and range of motion limitations. The distribution pattern helps narrow differential diagnoses significantly, as conditions like ankylosing spondylitis primarily affect the axial skeleton, while reactive arthritis may show oligoarticular involvement affecting only a few joints. Understanding these patterns allows healthcare providers to order appropriate laboratory tests, imaging studies, and initiate targeted treatments more efficiently.
3. Temperature Variations and Inflammatory Heat Signatures
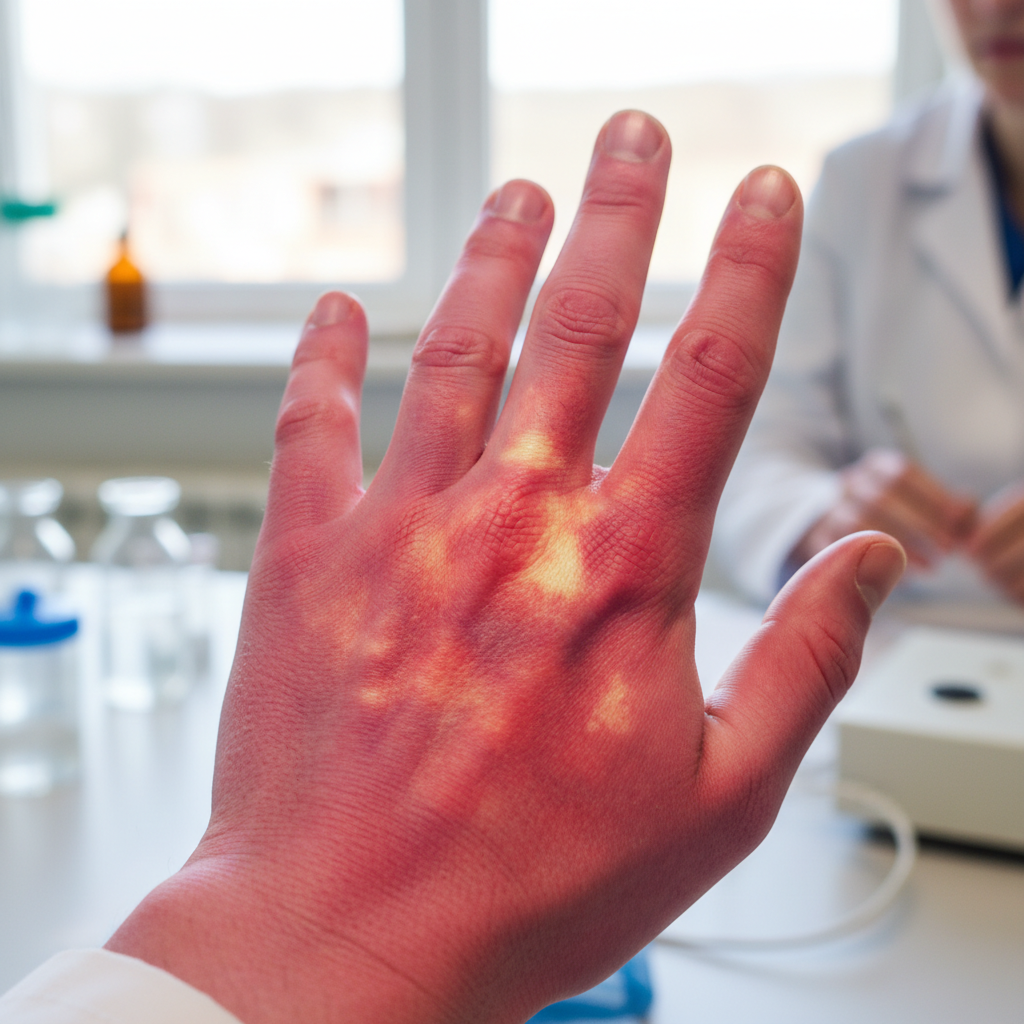
Morning temperature variations in affected joints and tissues provide valuable diagnostic clues that help physicians differentiate between various inflammatory conditions and their underlying pathophysiology. Inflammatory arthritis conditions, such as rheumatoid arthritis and psoriatic arthritis, often present with noticeably warm joints upon awakening, as increased blood flow and inflammatory mediator activity create localized hyperthermia. This warmth results from vasodilation caused by inflammatory cytokines like prostaglandin E2 and nitric oxide, which increase capillary permeability and blood flow to affected tissues. Patients with active inflammatory conditions may notice that their affected joints feel warm to the touch, particularly when compared to unaffected areas or when assessed by healthcare providers using clinical examination techniques. In contrast, osteoarthritis rarely produces significant joint warmth, as the degenerative process involves less active inflammation and more mechanical wear patterns. Fibromyalgia patients may actually experience the opposite phenomenon, with affected areas feeling cool or experiencing temperature sensitivity due to altered pain processing and autonomic nervous system dysfunction. Physicians use infrared thermography and clinical palpation to assess temperature differences, which can be particularly pronounced in the morning when circadian temperature variations are most apparent. The presence or absence of joint warmth, combined with other clinical findings, helps guide diagnostic workups and treatment decisions, as conditions requiring anti-inflammatory interventions can be distinguished from those needing alternative therapeutic approaches.
4. Swelling Patterns and Fluid Accumulation Timing
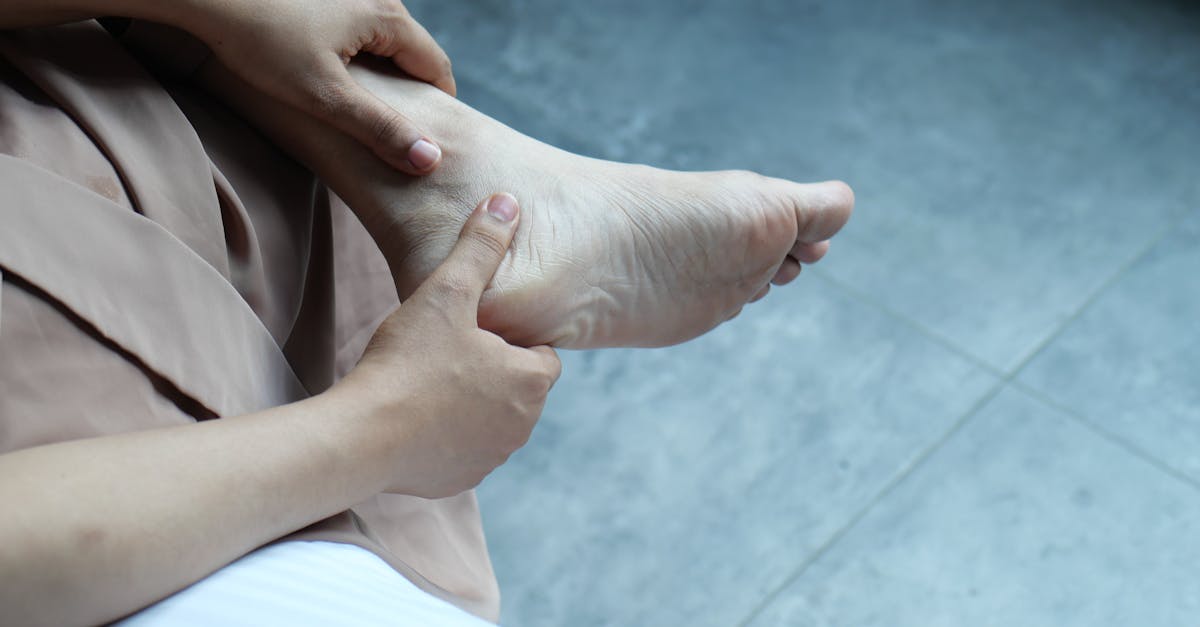
The timing and pattern of joint swelling upon morning awakening serve as critical diagnostic indicators that help physicians differentiate between various inflammatory conditions and understand their underlying mechanisms. In rheumatoid arthritis, morning joint swelling typically appears as soft, boggy tissue around affected joints, particularly in the small joints of the hands and feet, resulting from inflammatory synovial fluid accumulation and synovial membrane thickening. This swelling often feels warm and may be accompanied by visible joint deformity in advanced cases, as the inflammatory process damages cartilage and bone structures over time. The swelling in inflammatory conditions tends to be more pronounced in the morning due to prolonged immobility during sleep, which allows inflammatory mediators to accumulate and fluid to pool in joint spaces without the mechanical pumping action that movement provides. Osteoarthritis may also cause morning swelling, but it typically presents as harder, bony enlargements around joint margins rather than the soft tissue swelling characteristic of inflammatory arthritis. Physicians use specific measurement techniques, including joint circumference measurements and ultrasound imaging, to quantify and monitor swelling patterns over time. The response of morning swelling to movement and activity also provides diagnostic information, as inflammatory swelling often improves with gentle activity, while mechanical swelling may worsen with use. Healthcare providers teach patients to monitor and document their morning swelling patterns, as changes in these patterns can indicate disease flares or treatment responses.
5. Pain Intensity Fluctuations from Sleep to Waking

The characteristic pattern of pain intensity changes from sleep through the early morning hours provides physicians with essential diagnostic information for differentiating inflammatory conditions from other pain syndromes. Inflammatory arthritis pain typically follows a distinct pattern where patients may experience relatively comfortable sleep periods, only to awaken with intense joint pain and stiffness that gradually improves with movement and activity throughout the morning. This pattern occurs because inflammatory mediators accumulate during periods of inactivity, and the natural circadian rhythm of cortisol production reaches its nadir in the early morning hours, reducing the body's natural anti-inflammatory response. Patients with rheumatoid arthritis often describe waking up feeling as though they have been "hit by a truck," with pain levels significantly higher than when they went to bed. In contrast, osteoarthritis pain typically worsens throughout the day with activity and may actually be less severe in the morning after a period of rest. Fibromyalgia presents yet another pattern, where patients may experience disrupted sleep due to pain and awaken feeling unrefreshed, with widespread muscle pain and tenderness that doesn't follow typical joint distribution patterns. Physicians use validated pain assessment scales and ask patients to maintain pain diaries that track intensity levels at specific times, particularly focusing on the transition from sleep to waking. The timing and character of morning pain, combined with its response to movement, anti-inflammatory medications, and other interventions, helps guide diagnostic decisions and treatment planning.
6. Muscle Stiffness vs. Joint-Specific Limitations
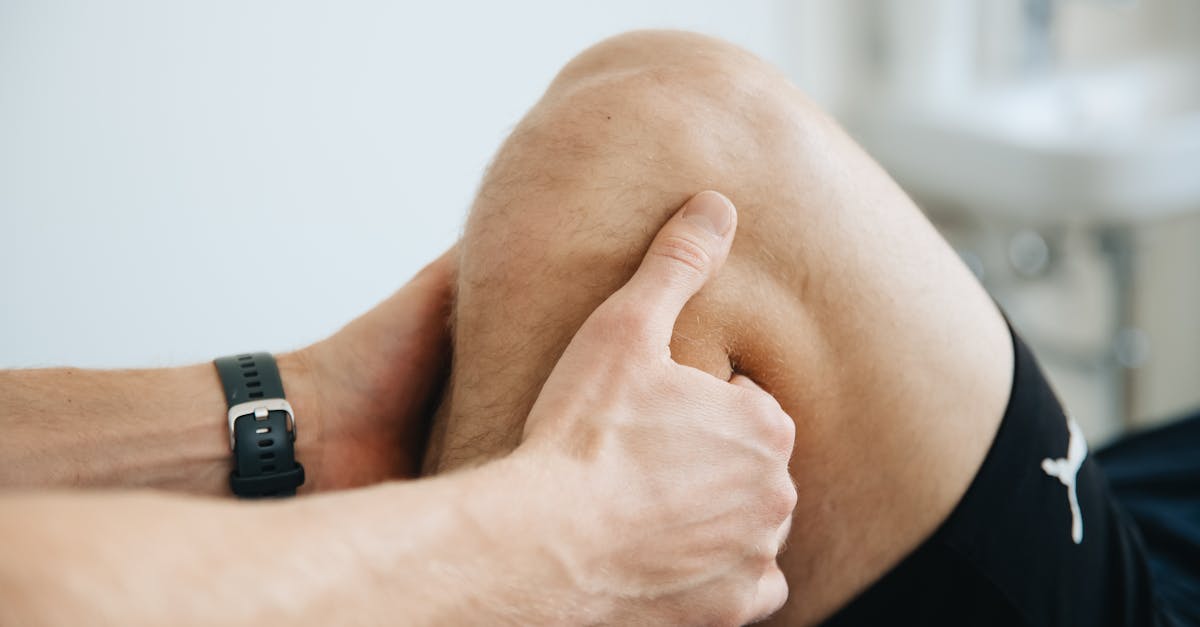
The distinction between generalized muscle stiffness and specific joint limitations upon morning awakening provides crucial diagnostic information that helps physicians differentiate between various inflammatory and non-inflammatory conditions. Inflammatory arthritis conditions primarily affect synovial joints, creating specific limitations in joint range of motion that patients can often localize to particular joints such as the wrists, knees, or ankles. These joint-specific limitations result from synovial inflammation, fluid accumulation, and eventual structural damage that mechanically restricts movement in predictable patterns. Patients with rheumatoid arthritis typically describe difficulty with specific tasks like making a fist, turning doorknobs, or climbing stairs, which correspond to inflammation in particular joint groups. In contrast, conditions like fibromyalgia or polymyalgia rheumatica present with more generalized muscle stiffness and aching that affects broad muscle groups rather than specific joints. Polymyalgia rheumatica, an inflammatory condition affecting older adults, characteristically causes severe morning stiffness in the shoulders, neck, and hip girdle muscles, making it difficult for patients to get out of bed or raise their arms above their heads. Physicians conduct detailed musculoskeletal examinations to differentiate between joint-specific limitations and muscle-related stiffness, using specific range of motion tests and palpation techniques. The pattern of limitation helps guide further diagnostic testing, as joint-specific problems may require imaging studies like X-rays or MRI, while muscle-related conditions might need different laboratory tests or electromyographic studies.
7. Fatigue Patterns and Energy Level Assessment

Morning fatigue patterns provide significant diagnostic insights that help physicians distinguish between various inflammatory conditions and understand their systemic impact on patients' overall health and functioning. Inflammatory conditions like rheumatoid arthritis and systemic lupus erythematosus often cause profound morning fatigue that extends beyond normal sleep inertia, leaving patients feeling exhausted despite adequate sleep duration. This fatigue results from the systemic inflammatory response, where cytokines like interleukin-1 and tumor necrosis factor-alpha affect the central nervous system and disrupt normal sleep architecture, preventing restorative sleep phases. Patients with active inflammatory disease often describe waking up feeling as tired as when they went to bed, with energy levels that may not improve significantly throughout the morning despite movement and activity. The inflammatory fatigue differs qualitatively from depression-related fatigue or simple sleep deprivation, as it often correlates with other inflammatory markers and responds to anti-inflammatory treatments. Fibromyalgia presents a unique fatigue pattern characterized by non-restorative sleep and morning exhaustion combined with cognitive symptoms often described as "fibro fog." Physicians use standardized fatigue assessment scales and sleep quality questionnaires to quantify and monitor these symptoms over time. The relationship between morning fatigue and disease activity levels helps guide treatment decisions, as addressing underlying inflammation often leads to improvements in energy levels and overall quality of life. Healthcare providers also assess for sleep disorders that may compound inflammatory fatigue, ensuring comprehensive treatment approaches.
8. Gastrointestinal Morning Symptoms in Systemic Inflammation

Morning gastrointestinal symptoms serve as important diagnostic markers that help physicians identify systemic inflammatory conditions and differentiate them from localized joint problems. Inflammatory bowel diseases like Crohn's disease and ulcerative colitis characteristically present with morning abdominal cramping, diarrhea, and urgency that may awaken patients from sleep or occur immediately upon rising. These symptoms result from increased inflammatory activity in the intestinal tract during early morning hours, when circadian rhythms influence immune system activity and inflammatory mediator production. The morning pattern occurs because inflammatory cytokines in the gut follow circadian variations, with peak activity often coinciding with early morning hours. Patients with inflammatory bowel disease may also develop extraintestinal manifestations including inflammatory arthritis, which creates a complex diagnostic picture requiring careful evaluation of both gastrointestinal and joint symptoms. Systemic inflammatory conditions like rheumatoid arthritis can also cause morning nausea and gastrointestinal discomfort, particularly when patients take medications on an empty stomach or when systemic inflammation affects gut function. Physicians conduct comprehensive reviews of gastrointestinal symptoms, including timing, character, and associated features, to identify patterns that suggest inflammatory bowel disease or systemic inflammatory conditions. The presence of morning gastrointestinal symptoms may prompt additional diagnostic testing including inflammatory markers, stool studies, and endoscopic procedures. Understanding these connections helps healthcare providers develop integrated treatment approaches that address both gastrointestinal and musculoskeletal manifestations of systemic inflammatory diseases.
9. Skin Manifestations and Morning Inflammatory Changes
Morning skin changes and manifestations provide valuable diagnostic clues that help physicians identify inflammatory conditions with dermatological components and distinguish them from purely articular diseases. Psoriatic arthritis often presents with characteristic morning skin symptoms including increased scaling, redness, and itching of psoriatic plaques that may be more pronounced upon awakening due to overnight accumulation of inflammatory mediators in affected skin areas. The inflammatory process in psoriasis follows circadian patterns, with cytokines like interleukin-17 and tumor necrosis factor-alpha showing peak activity during certain times of day, often correlating with symptom severity. Patients may notice that their psoriatic lesions appear more inflamed, thicker, or more symptomatic in the morning, particularly after periods of immobility during sleep. Systemic lupus erythematosus can present with morning facial rashes, particularly the characteristic malar rash, which may be more prominent upon awakening due to increased photosensitivity and inflammatory activity. The morning assessment of skin symptoms helps physicians identify patterns that suggest specific inflammatory conditions and monitor disease activity over time. Dermatomyositis, an inflammatory muscle disease, often presents with characteristic morning skin changes including heliotrope rash around the eyes and Gottron's papules over the knuckles, which may be more pronounced after overnight inflammation. Healthcare providers conduct systematic skin examinations during morning appointments to document inflammatory changes and correlate them with joint and muscle symptoms. The timing and character of skin manifestations, combined with other clinical findings, guide diagnostic testing and treatment decisions for complex inflammatory conditions.
10. Neurological Symptoms and Morning Cognitive Changes

Morning neurological symptoms and cognitive changes provide important diagnostic information that helps physicians identify inflammatory conditions with central nervous system involvement and distinguish them from purely peripheral inflammatory diseases. Systemic lupus erythematosus can cause morning cognitive dysfunction, including difficulty with concentration, memory problems, and mental fogginess that patients often describe as "lupus fog." These symptoms result from inflammatory mediators crossing the blood-brain barrier and affecting neural function, with severity often correlating with overall disease activity. The morning presentation of cognitive symptoms may be particularly pronounced due to circadian variations in inflammatory cytokine production and their effects on neurotransmitter systems. Patients with inflammatory conditions may also experience morning headaches, which can result from systemic inflammation affecting cerebral blood vessels or from medication side effects. Giant cell arteritis, an inflammatory condition affecting large and medium-sized arteries, characteristically presents with severe morning headaches, jaw claudication, and visual symptoms that require urgent medical attention. Fibromyalgia patients often experience morning cognitive symptoms including difficulty with word finding, concentration problems, and feeling mentally "cloudy," which may persist throughout the morning hours. Physicians conduct detailed neurological assessments and cognitive screening tests to identify and monitor these symptoms over time. The presence of morning neurological symptoms may prompt additional diagnostic testing including brain imaging, cerebrospinal fluid analysis, or specialized cognitive assessments. Understanding the relationship between inflammatory activity and neurological symptoms helps guide treatment decisions and monitoring strategies for complex systemic inflammatory conditions.
11. Ocular Symptoms and Morning Eye Inflammation
Morning ocular symptoms serve as critical diagnostic indicators that help physicians identify inflammatory conditions with ophthalmological manifestations and assess the systemic extent of inflammatory diseases. Inflammatory arthritis conditions, particularly ankylosing spondylitis and reactive arthritis, commonly present with acute anterior uveitis, which may cause morning eye pain, photophobia, and blurred vision that can be more pronounced upon awakening. The inflammatory process in uveitis involves immune-mediated inflammation of the uveal tract, with symptoms often following circadian patterns that correlate with overall inflammatory activity. Patients may notice increased eye redness, tearing, and discomfort in the morning, particularly when exposed to bright light after the relative darkness of sleep. Sjögren's syndrome, an autoimmune condition that commonly accompanies other inflammatory arthritis conditions, causes morning dry eye symptoms including gritty sensation, burning, and difficulty opening the eyes upon awakening due to decreased tear production overnight. The morning assessment of ocular symptoms is particularly important because inflammatory eye conditions can lead to serious complications including vision loss if not promptly diagnosed and treated. Physicians conduct systematic ophthalmological examinations and may collaborate with ophthalmologists to evaluate inflammatory eye conditions. Rheumatoid arthritis can cause morning dry eye symptoms and occasionally more serious complications like scleritis or corneal perforation. The timing and character of morning eye symptoms, combined with other clinical findings, help guide diagnostic testing and urgent referrals when necessary. Healthcare providers educate patients about the importance of reporting new or worsening eye symptoms, as these may indicate disease flares or the development of serious complications requiring immediate attention.
12. Respiratory Symptoms and Morning Breathing Patterns

Morning respiratory symptoms provide valuable diagnostic information that helps physicians identify inflammatory conditions with pulmonary involvement and assess the systemic impact of inflammatory diseases on respiratory function. Rheumatoid arthritis can cause morning chest tightness, shortness of breath, and coughing due to inflammatory involvement of the pleura, lung parenchyma, or chest wall joints, with symptoms often more pronounced upon awakening when inflammatory mediators have accumulated overnight. The inflammatory process in rheumatoid lung disease involves immune complex