12 Voice Change Symptoms Associated With Thyroid and Neurological Conditions
The human voice serves as a remarkable barometer of our overall health, particularly when it comes to thyroid and neurological conditions that can profoundly impact vocal function. Voice changes often represent the earliest and most noticeable symptoms of underlying systemic disorders, making them crucial diagnostic indicators that healthcare professionals and patients alike should never ignore. The complex interplay between hormonal regulation, neurological control, and muscular coordination required for normal voice production creates multiple vulnerability points where disease processes can manifest. Thyroid disorders, ranging from hyperthyroidism to hypothyroidism, can alter vocal cord structure, muscle tension, and respiratory support, while neurological conditions affecting the brain, cranial nerves, or peripheral nervous system can disrupt the precise neural coordination necessary for speech and voice production. Understanding these voice-related symptoms not only aids in early detection and diagnosis but also provides valuable insights into disease progression and treatment effectiveness. This comprehensive exploration will examine twelve distinct voice change symptoms that commonly occur in thyroid and neurological conditions, offering both patients and healthcare providers essential knowledge for recognizing when voice alterations signal more serious underlying health concerns.
1. Hoarseness and Vocal Roughness - The Primary Warning Signal
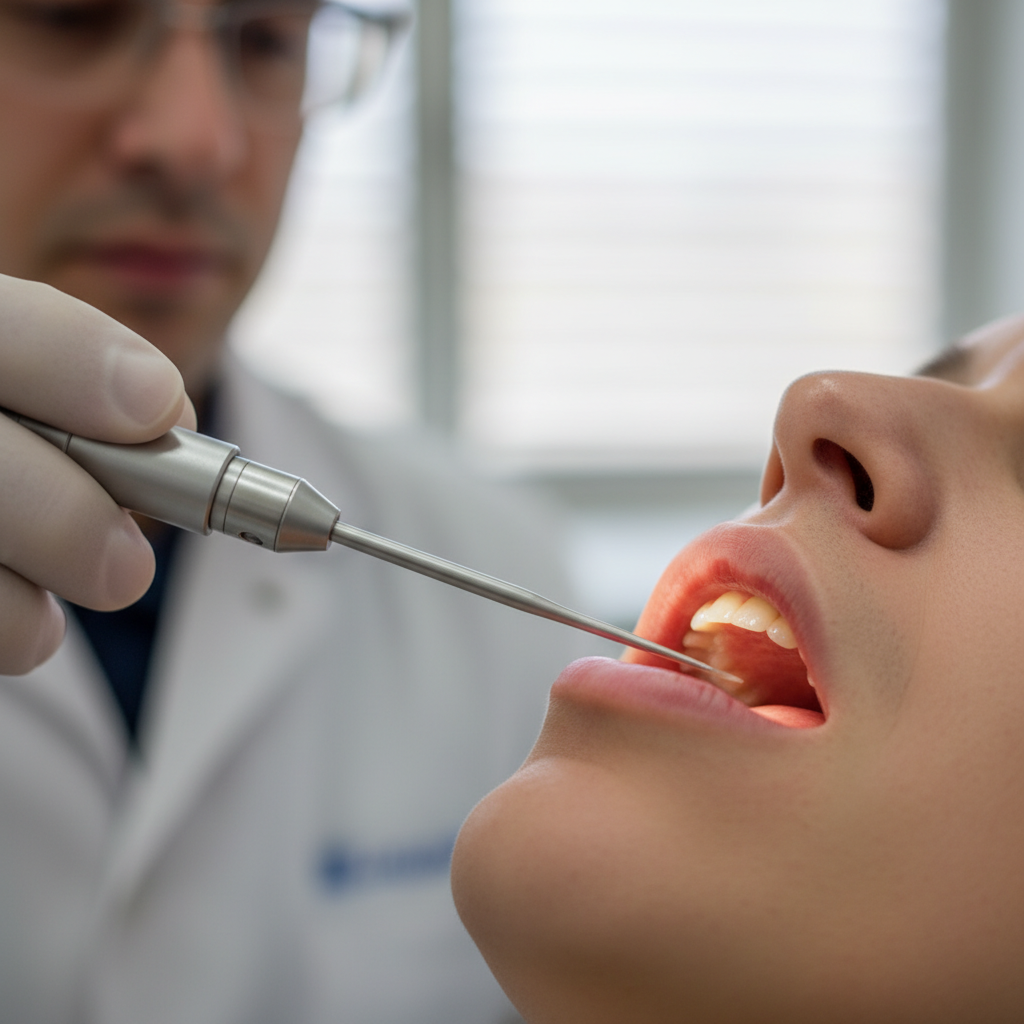
Hoarseness represents one of the most common and recognizable voice changes associated with both thyroid and neurological disorders, characterized by a rough, breathy, or strained vocal quality that deviates significantly from an individual's normal speaking voice. In thyroid conditions, particularly hypothyroidism, hoarseness often develops gradually as the vocal cords become swollen and thickened due to mucopolysaccharide deposits, a consequence of decreased thyroid hormone production that affects tissue metabolism throughout the body. This swelling reduces the vocal cords' ability to vibrate smoothly, creating the characteristic rough, gravelly sound that many patients describe as feeling like they have a persistent cold or laryngitis. Neurological conditions can produce hoarseness through different mechanisms, including vocal cord paralysis from cranial nerve damage, muscle weakness affecting respiratory support, or coordination problems that prevent proper vocal cord closure during phonation. Patients with Parkinson's disease frequently experience hoarseness as one of their earliest symptoms, often years before motor symptoms become apparent, due to the progressive deterioration of neural pathways controlling fine motor movements of the laryngeal muscles. The severity and progression pattern of hoarseness can provide valuable diagnostic clues, with sudden onset suggesting acute neurological events like stroke, while gradual development over months typically indicates progressive conditions like thyroid dysfunction or neurodegenerative diseases.
2. Voice Tremor and Vocal Instability

Voice tremor manifests as involuntary oscillations in vocal pitch, loudness, or quality, creating a characteristic quavering or shaking sound that can significantly impact communication effectiveness and social confidence. This symptom commonly appears in essential tremor, Parkinson's disease, and other movement disorders where the fine motor control required for stable voice production becomes compromised due to abnormal neural firing patterns in the brain circuits responsible for motor coordination. In thyroid disorders, particularly hyperthyroidism, voice tremor may develop as part of a broader tremor syndrome affecting multiple body systems, reflecting the heightened metabolic state and increased sympathetic nervous system activity that characterizes overactive thyroid function. The tremor typically becomes more pronounced during periods of stress, fatigue, or emotional intensity, when the already compromised neural control systems face additional demands. Patients often report that their voice sounds "shaky" or "nervous" even when they feel calm, and the tremor may be more noticeable during sustained vowel sounds or when speaking at higher volumes. Neurological voice tremor can vary in frequency and amplitude, with some patients experiencing rapid, fine oscillations while others develop slower, more pronounced wavering that makes speech difficult to understand. The impact on daily communication can be profound, leading many individuals to avoid speaking situations or develop compensatory strategies like speaking more softly or in shorter phrases to minimize the tremor's visibility.
3. Vocal Fatigue and Reduced Endurance

Vocal fatigue represents a debilitating symptom characterized by rapid voice deterioration during speaking tasks, often accompanied by throat discomfort, increased effort required for phonation, and progressive voice quality decline throughout the day. In thyroid disorders, particularly hypothyroidism, vocal fatigue frequently occurs due to the generalized muscle weakness and reduced metabolic efficiency that affects all body systems, including the complex musculature involved in voice production. The laryngeal muscles, respiratory muscles, and articulatory structures all require optimal energy metabolism to maintain coordinated function during extended speaking periods, and thyroid hormone deficiency can significantly compromise this energy production at the cellular level. Neurological conditions affecting motor neuron function, such as amyotrophic lateral sclerosis (ALS) or myasthenia gravis, can produce severe vocal fatigue as the neural signals controlling muscle contraction become progressively weaker or less reliable throughout periods of use. Patients typically notice that their voice starts strong in the morning but becomes increasingly weak, breathy, or strained as the day progresses, often requiring frequent rest periods or voice conservation strategies to maintain functional communication. The psychological impact of vocal fatigue can be substantial, as individuals may begin to limit their social interactions, professional activities, or recreational pursuits that involve extensive speaking, leading to isolation and reduced quality of life that extends far beyond the physical voice symptoms themselves.
4. Pitch Changes and Vocal Range Limitations
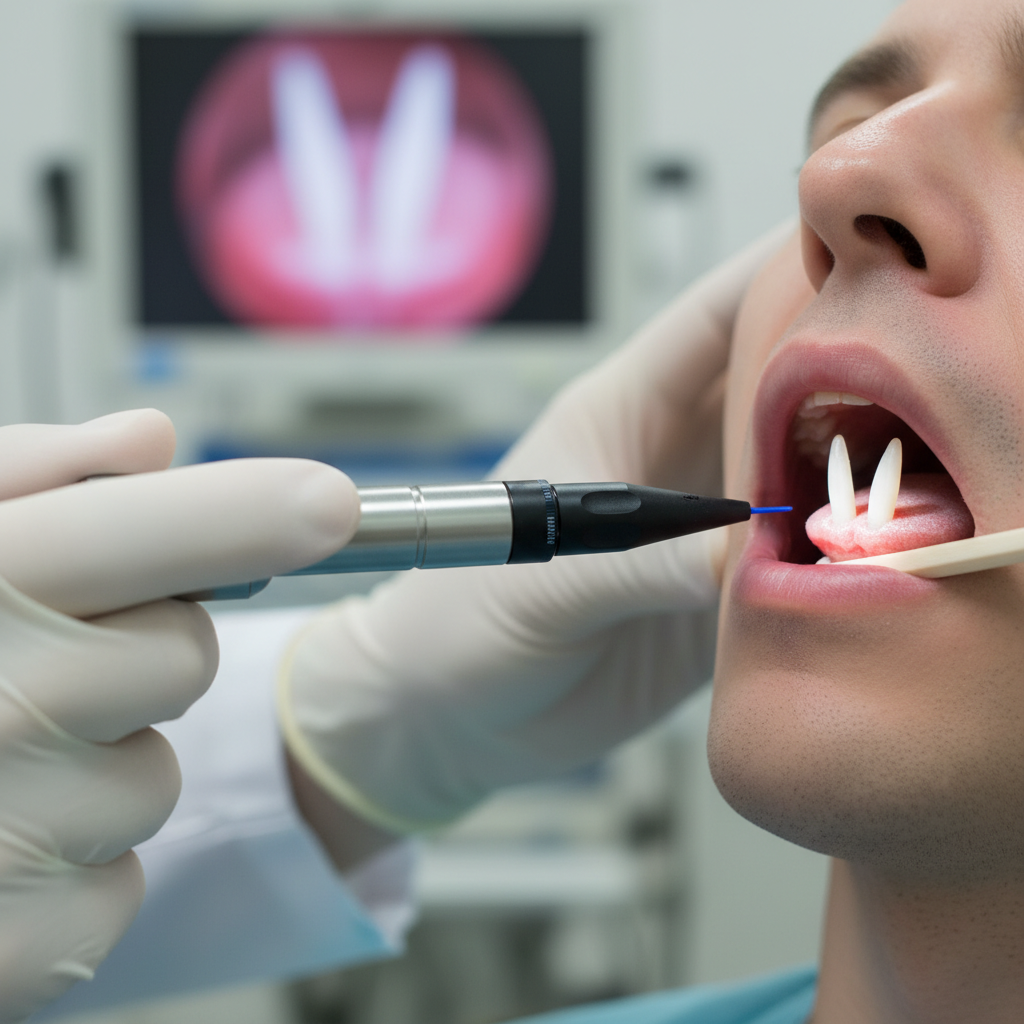
Alterations in vocal pitch and reduced vocal range represent significant voice changes that can profoundly impact both the functional and aesthetic aspects of communication, often serving as early indicators of underlying thyroid or neurological pathology. Thyroid disorders frequently cause characteristic pitch changes, with hypothyroidism typically leading to a lower, deeper voice due to vocal cord thickening and increased mass, while hyperthyroidism may produce a higher, more strained vocal quality as metabolic hyperactivity affects muscle tension and coordination. These pitch changes often develop gradually over months or years, making them particularly insidious as patients and their families may not immediately recognize the alteration until it becomes quite pronounced. Neurological conditions affecting the recurrent laryngeal nerve, such as those resulting from stroke, brain tumors, or progressive neurodegenerative diseases, can cause unilateral vocal cord paralysis that dramatically alters pitch control and eliminates the ability to produce certain frequencies within the normal vocal range. Patients may lose their ability to sing, speak in their professional voice (particularly problematic for teachers, singers, or public speakers), or modulate their voice for emotional expression, leading to a monotonous, flat speaking pattern that lacks the natural prosody essential for effective communication. The impact extends beyond mere acoustic changes, as pitch alterations can affect perceived gender identity, professional competence, and social interactions, making this symptom particularly distressing for many individuals experiencing voice changes related to systemic health conditions.
5. Breathiness and Air Loss During Speech

Breathiness in voice production manifests as excessive air escape during phonation, creating a whispered or airy quality that reduces vocal clarity and projection while often requiring increased effort to maintain audible speech volume. This symptom commonly occurs in neurological conditions affecting the cranial nerves responsible for vocal cord movement, particularly when unilateral or bilateral vocal cord paralysis prevents complete glottal closure during voice production. In conditions such as vagal nerve injury, brainstem stroke, or progressive supranuclear palsy, the inability to bring the vocal cords together completely allows air to escape continuously during speech attempts, resulting in the characteristic breathy voice quality that many patients describe as feeling like they're "running out of air" while talking. Thyroid disorders can contribute to breathiness through multiple mechanisms, including vocal cord swelling that prevents proper closure, muscle weakness affecting respiratory support, or changes in tissue elasticity that alter vocal cord vibration patterns. The compensatory behaviors that patients develop to manage breathiness often exacerbate the problem, as increased respiratory effort and muscle tension can lead to additional voice strain and fatigue. Patients frequently report frustration with their inability to be heard in noisy environments, difficulty speaking on the telephone, or embarrassment about their weak, ineffective voice quality that may be misinterpreted by others as lack of confidence or authority. The social and professional implications of severe breathiness can be particularly challenging for individuals whose careers depend on effective vocal communication.
6. Vocal Cord Paralysis and Movement Disorders
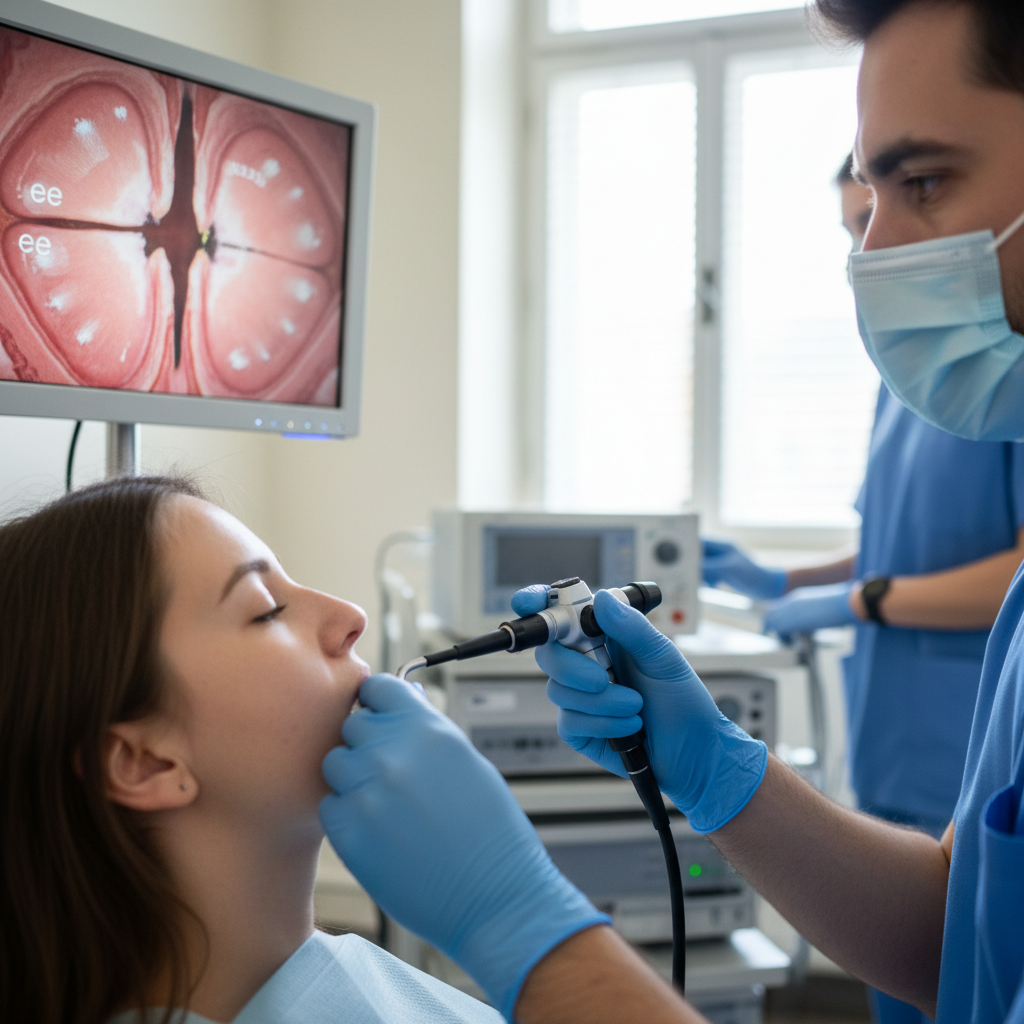
Vocal cord paralysis represents one of the most severe voice-related complications of neurological conditions, occurring when damage to the recurrent laryngeal nerve or vagus nerve prevents normal vocal cord movement during breathing and phonation. This condition can result from various neurological pathologies, including brainstem strokes, skull base tumors, neurodegenerative diseases, or surgical complications affecting the neural pathways that control laryngeal function. Unilateral vocal cord paralysis typically produces a weak, breathy voice with reduced loudness and poor vocal projection, as the paralyzed cord cannot meet the mobile cord at midline for effective voice production. Bilateral vocal cord paralysis, while less common, presents a more complex clinical picture that may compromise both voice production and breathing, potentially requiring emergency airway management in acute cases. The impact on daily communication can be devastating, as patients often struggle to make themselves heard in normal conversation, experience severe vocal fatigue with minimal voice use, and may develop compensatory behaviors such as throat clearing or excessive muscle tension that further compromise vocal function. Thyroid surgery complications represent a significant risk factor for recurrent laryngeal nerve injury and subsequent vocal cord paralysis, making post-operative voice monitoring essential for early detection and intervention. The psychological adjustment to vocal cord paralysis can be particularly challenging, as patients must adapt to a fundamentally altered communication ability that affects their personal identity, professional capabilities, and social interactions in profound and lasting ways.
7. Muscle Tension and Vocal Strain
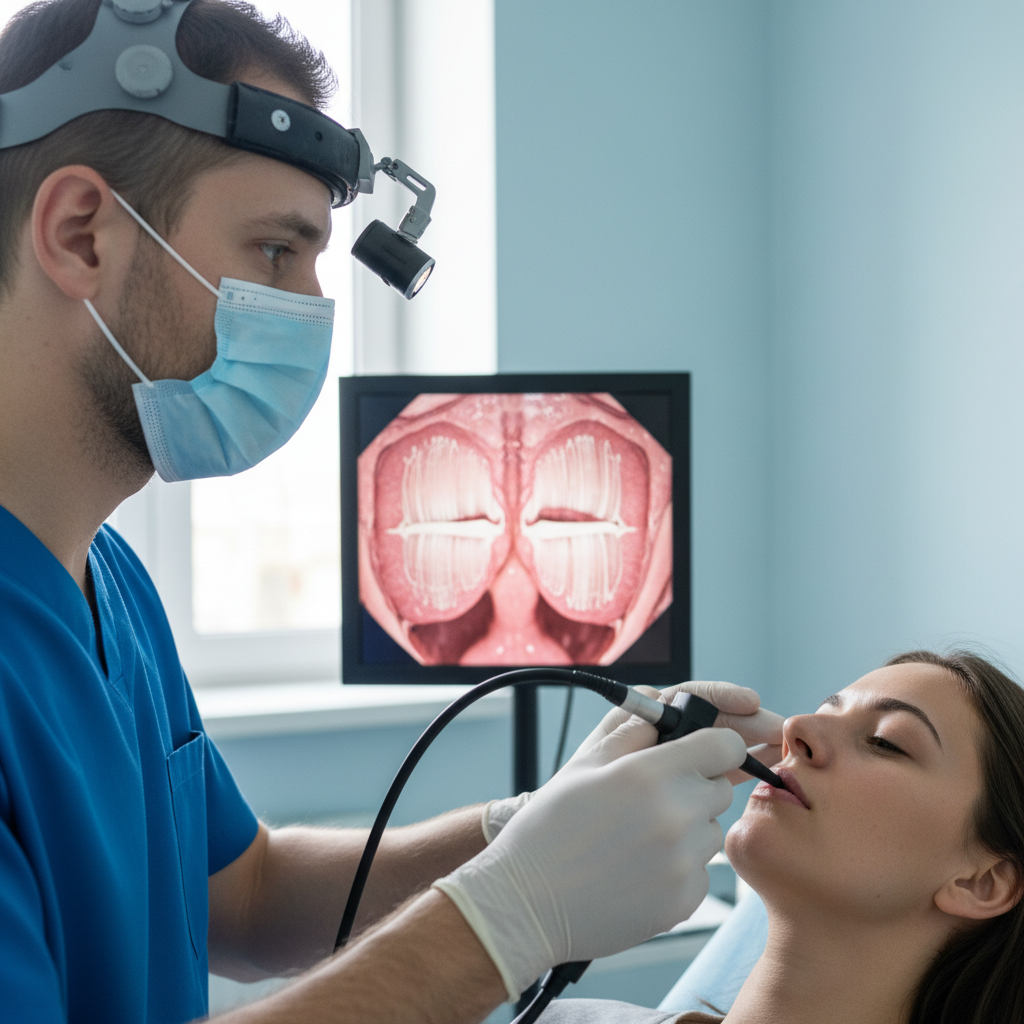
Excessive muscle tension affecting the laryngeal, respiratory, and articulatory muscles represents a common manifestation of both thyroid and neurological disorders that can significantly compromise voice quality and speaking comfort. In hyperthyroidism, increased metabolic activity and sympathetic nervous system stimulation often lead to generalized muscle tension that particularly affects the delicate balance of forces required for optimal voice production. Patients frequently develop a strained, effortful vocal quality as they unconsciously increase muscle tension in an attempt to maintain voice control, creating a vicious cycle where increased effort leads to greater tension and progressively worsening voice function. Neurological conditions such as dystonia, essential tremor, or Parkinson's disease can produce focal muscle tension in the laryngeal area, resulting in spasmodic dysphonia or other voice disorders characterized by involuntary muscle contractions that interrupt smooth voice production. The sensation of vocal strain often extends beyond the throat to include neck, shoulder, and jaw tension, as the body attempts to compensate for compromised laryngeal function through recruitment of accessory muscles not typically involved in voice production. Patients commonly report feeling like they need to "push" or "force" their voice, experiencing throat pain or discomfort after speaking, and noticing that their voice becomes increasingly strained throughout the day as muscle fatigue accumulates. The chronic nature of muscle tension-related voice problems can lead to secondary complications including vocal nodules, polyps, or other structural changes that further compromise voice function and may require specialized treatment approaches combining medical management with voice therapy techniques.
8. Speech Rate and Rhythm Disturbances

Alterations in speech rate and rhythm represent significant neurological voice symptoms that can profoundly impact communication effectiveness and listener comprehension, often serving as early indicators of progressive neurodegenerative conditions. Parkinson's disease commonly produces a characteristic pattern of speech changes including rapid, rushed speech (tachyphemia) alternating with sudden stops or hesitations, creating an irregular rhythm that makes conversation difficult to follow and participate in naturally. The underlying pathophysiology involves disruption of the basal ganglia circuits responsible for motor timing and coordination, affecting not only the speed of speech production but also the natural prosodic patterns that give speech its musical quality and emotional expressiveness. Thyroid disorders can influence speech rate through their effects on overall metabolic function and nervous system activity, with hyperthyroidism often producing rapid, pressured speech that reflects the general acceleration of physiological processes, while hypothyroidism may result in slower, more labored speech patterns that mirror the generalized slowing of mental and physical functions. Patients with rhythm disturbances often struggle with social communication, as listeners may find their altered speech patterns distracting or difficult to understand, leading to frequent requests for repetition or clarification that can be embarrassing and frustrating. The impact extends beyond mere communication mechanics to affect the natural flow of conversation, making it challenging to maintain normal social interactions, participate effectively in professional meetings, or engage in the spontaneous verbal exchanges that characterize healthy human relationships.
9. Volume Control Problems and Loudness Variations

Difficulty controlling vocal volume represents a complex voice symptom that can manifest as either inability to speak loudly enough for effective communication or problems with excessive loudness that seems inappropriate for the social context. Neurological conditions affecting the brain regions responsible for motor control and sensory feedback often disrupt the sophisticated neural mechanisms required to monitor and adjust vocal intensity based on environmental demands and social cues. Parkinson's disease characteristically produces hypophonia, a condition where patients speak in an abnormally quiet voice that may be barely audible even in quiet environments, often without the patient's awareness of the volume reduction due to altered sensory feedback processing. This creates significant communication barriers as family members and colleagues struggle to hear and understand the patient's speech, leading to social isolation and frustration for all parties involved. Conversely, some neurological conditions or thyroid-related anxiety and agitation can produce inappropriate loudness where patients speak much more loudly than necessary, potentially creating social discomfort and misunderstandings about their emotional state or intentions. The inability to modulate volume appropriately also affects the natural emphasis and stress patterns that give speech its meaning and emotional content, resulting in a flat, monotonous delivery that lacks the dynamic range necessary for engaging communication. Patients often report feeling disconnected from their own voice, as if they cannot gauge how they sound to others, leading to self-consciousness and avoidance of speaking situations that further compounds the social and psychological impact of their voice disorder.
10. Swallowing Difficulties and Voice Coordination

The intimate relationship between swallowing function and voice production means that many thyroid and neurological conditions simultaneously affect both processes, creating complex symptom patterns that can significantly impact quality of life and safety. The shared anatomical structures and neural pathways involved in swallowing and phonation mean that disorders affecting one function frequently compromise the other, leading to voice changes that occur alongside dysphagia (swallowing difficulties). Neurological conditions such as stroke, amyotrophic lateral sclerosis, or multiple sclerosis can disrupt the precise coordination required for both safe swallowing and effective voice production, as the same cranial nerves and brainstem centers control both functions. Patients may notice that their voice quality changes after eating or drinking, becoming wet or gurgly due to residual food or liquid in the throat, or they may experience coughing and throat clearing that further irritates the vocal cords and compromises voice function. Thyroid enlargement (goiter) can create mechanical compression of the esophagus and trachea that affects both swallowing comfort and voice resonance, while thyroid hormone imbalances can alter muscle strength and coordination throughout the swallowing mechanism. The safety implications of combined voice and swallowing problems are significant, as aspiration of food or liquid into the lungs can lead to pneumonia and other serious complications, making early recognition and treatment of these symptoms essential for preventing life-threatening consequences. The social and nutritional impact of swallowing difficulties often compounds the communication challenges created by voice changes, as patients may avoid eating in social situations or restrict their diet in ways that affect their overall health and well-being.
11. Cognitive-Voice Integration Problems

The complex relationship between cognitive function and voice production becomes particularly apparent in neurological conditions that affect both mental processing and motor control, creating voice symptoms that reflect underlying changes in thinking, memory, and executive function. Conditions such as dementia, traumatic brain injury, or multiple sclerosis can disrupt the sophisticated cognitive processes required for planning, organizing, and executing complex speech tasks, resulting in voice changes that go beyond simple motor dysfunction to include problems with word-finding, sentence construction, and conversational flow. Patients may experience voice symptoms that fluctuate with their cognitive state, becoming more pronounced during periods of confusion, fatigue, or emotional stress when cognitive resources are already taxed. The integration of language formulation with voice production requires seamless coordination between multiple brain regions, and when this integration is compromised, patients may struggle with initiating speech, maintaining appropriate vocal parameters while focusing on message content, or adapting their voice to match the communicative demands of different social situations. Thyroid disorders can affect cognitive-voice integration through their impact on mental clarity, concentration, and processing speed, with both hyperthyroidism and hypothyroidism potentially creating brain fog or cognitive slowing that interferes with the mental effort required for effective voice use. The frustration and anxiety that often accompany cognitive-voice integration problems can create a secondary layer of difficulty, as patients become increasingly self-conscious about their communication abilities and may develop avoidance behaviors that further limit their opportunities for social interaction and cognitive stimulation.
12. Emotional Expression and Prosodic Changes

The ability to convey emotion through voice represents one of the most sophisticated aspects of human communication, involving precise modulation of pitch, rhythm, stress, and intonation patterns that can be significantly disrupted by thyroid and neurological conditions. Prosody, the musical quality of speech that carries emotional meaning and social cues, relies on complex neural networks that integrate emotional processing centers with motor control systems, making it particularly vulnerable to neurological dysfunction. Parkinson's disease characteristically produces a flat, monotonous speaking pattern with reduced emotional expressiveness, often leading to misunderstandings where patients are perceived as depressed, disinterested, or unfriendly despite having normal emotional experiences internally. This disconnect between internal emotional state and external vocal expression can be particularly distressing for patients and their families, as the voice no longer serves as an accurate reflection of the person's feelings and intentions. Thyroid disorders can affect emotional expression through their impact on mood regulation and anxiety levels, with hyperthyroidism potentially producing rapid, agitated speech patterns that may be misinterpreted as anger or aggression, while hypothyroidism can create a subdued, flat vocal quality that suggests depression even when