12 Bleeding Pattern Variations That Signal Clotting and Platelet Disorders
The human body's hemostatic system represents one of nature's most sophisticated biological mechanisms, orchestrating a delicate balance between bleeding and clotting that maintains vascular integrity while preventing life-threatening hemorrhage. When this intricate system malfunctions, it communicates through a complex vocabulary of bleeding patterns that serve as diagnostic windows into underlying platelet and coagulation disorders. These bleeding manifestations are not merely symptoms but rather precise indicators that reflect specific defects in platelet function, coagulation cascade abnormalities, or vascular integrity compromises. Understanding these bleeding pattern variations is crucial for healthcare professionals, as early recognition can mean the difference between timely intervention and potentially catastrophic outcomes. From the subtle appearance of petechiae suggesting thrombocytopenia to the dramatic presentation of deep tissue hematomas indicating severe coagulation factor deficiencies, each bleeding pattern tells a unique story about the underlying pathophysiology. This comprehensive exploration will examine twelve distinct bleeding pattern variations that serve as critical diagnostic markers, providing healthcare providers and patients with essential knowledge to recognize, interpret, and respond appropriately to these important clinical signs that may herald serious hematological disorders requiring immediate medical attention.
1. Petechial Bleeding - The Pinpoint Indicators of Platelet Dysfunction
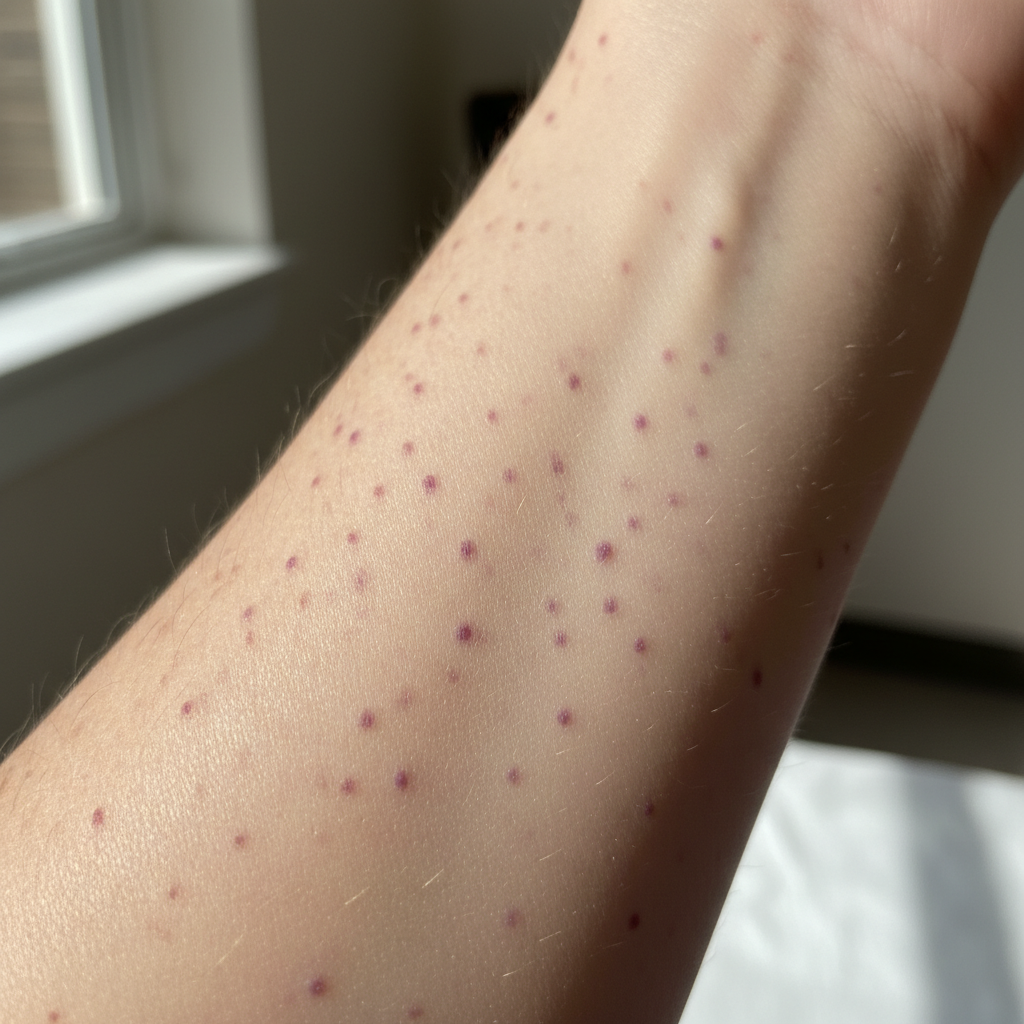
Petechial bleeding represents one of the most characteristic and diagnostically significant bleeding patterns associated with platelet disorders, manifesting as tiny, pinpoint-sized hemorrhages that appear as red or purple spots measuring less than 2 millimeters in diameter on the skin and mucous membranes. These minute bleeding points occur when capillaries rupture due to inadequate platelet plug formation, typically indicating thrombocytopenia (low platelet count) or qualitative platelet dysfunction. The distribution pattern of petechiae provides valuable diagnostic clues, with gravity-dependent areas such as the lower extremities, ankles, and feet commonly affected first, followed by areas of increased pressure or trauma. Unlike larger purpuric lesions, petechiae do not blanch with pressure and represent actual extravasation of red blood cells into the surrounding tissue. The density and progression of petechial bleeding often correlates with the severity of the underlying platelet disorder, with platelet counts below 50,000 per microliter typically associated with spontaneous petechial formation. Common causes include immune thrombocytopenic purpura (ITP), drug-induced thrombocytopenia, bone marrow disorders, and inherited platelet function defects. The presence of petechiae, particularly when accompanied by other bleeding manifestations, warrants immediate hematological evaluation including complete blood count with platelet assessment, peripheral blood smear examination, and potentially bone marrow biopsy to determine the underlying etiology and guide appropriate therapeutic intervention.
2. Purpuric Lesions - The Bridge Between Platelet and Vascular Disorders
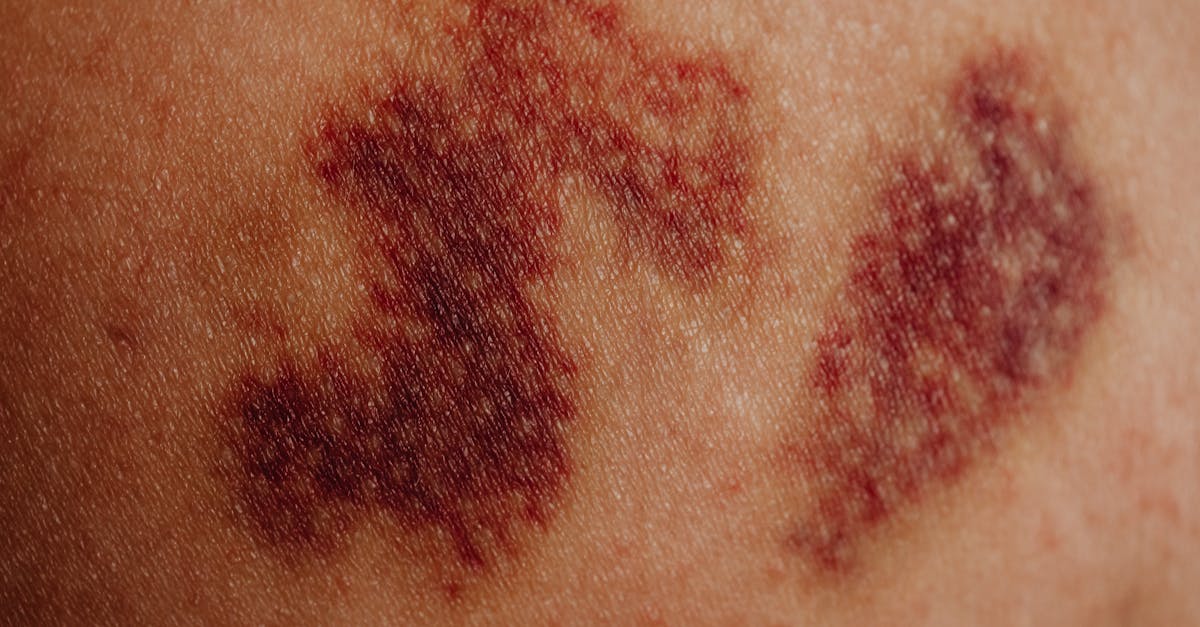
Purpuric lesions represent a more extensive form of bleeding than petechiae, characterized by purple or red discoloration of the skin measuring between 2-10 millimeters in diameter, resulting from bleeding into the skin from damaged capillaries or small blood vessels. These lesions serve as important indicators of both platelet disorders and vascular abnormalities, often appearing in conjunction with other bleeding manifestations to create a comprehensive clinical picture of hemostatic dysfunction. The morphology and distribution of purpuric lesions can provide significant diagnostic information, with palpable purpura suggesting vasculitic processes, while non-palpable purpura typically indicates platelet or coagulation abnormalities. Age-related changes in vascular integrity can contribute to purpura formation, particularly in elderly patients where skin fragility and decreased subcutaneous tissue support make vessels more susceptible to minor trauma. Senile purpura, commonly observed on the dorsal surfaces of hands and forearms in older adults, represents a benign form related to age-related vascular changes and chronic sun exposure. However, the sudden appearance of purpuric lesions, especially when accompanied by other bleeding symptoms, may indicate serious underlying conditions such as thrombotic thrombocytopenic purpura (TTP), hemolytic uremic syndrome (HUS), or disseminated intravascular coagulation (DIC). The evaluation of purpuric lesions requires careful assessment of their characteristics, distribution, associated symptoms, and temporal relationship to potential triggers, making them valuable diagnostic markers in the comprehensive evaluation of bleeding disorders.
3. Ecchymoses - The Telltale Signs of Coagulation Factor Deficiencies
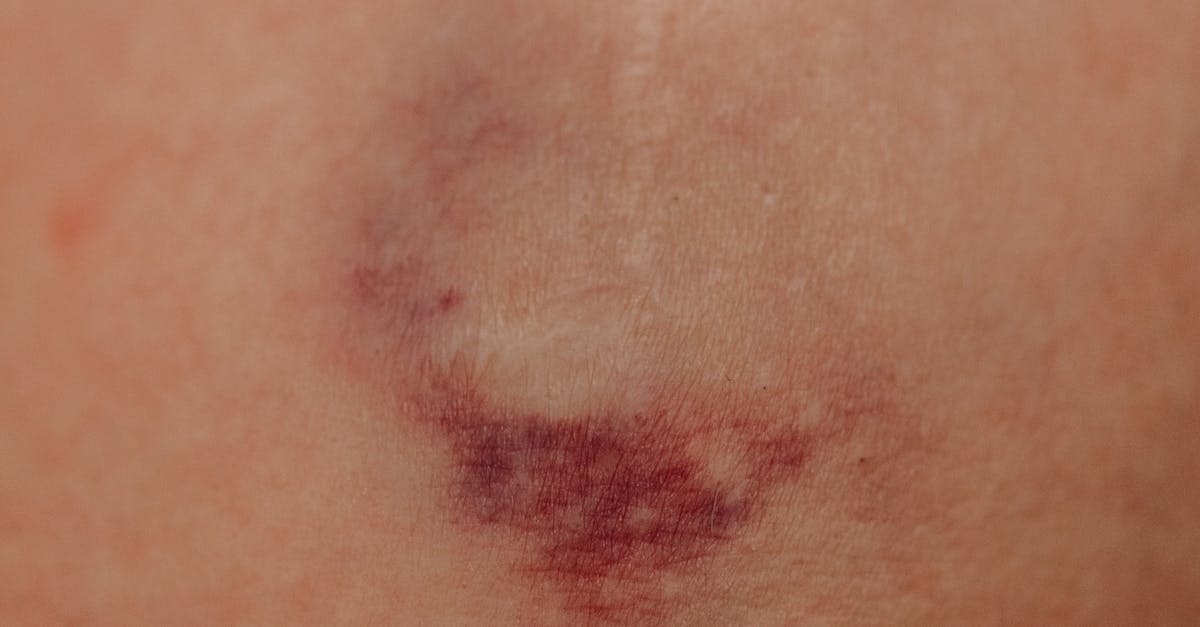
Ecchymoses, commonly known as bruises, represent larger areas of bleeding into the skin and subcutaneous tissues, typically measuring greater than 10 millimeters in diameter and appearing as blue, purple, or greenish discoloration that evolves through characteristic color changes as the extravasated blood is metabolized. These lesions are particularly significant in the context of coagulation disorders, as they often indicate deficiencies in clotting factors or abnormalities in the coagulation cascade that prevent effective hemostasis following minor trauma or even spontaneous bleeding. The size, location, and frequency of ecchymoses provide important diagnostic clues about the underlying hemostatic abnormality, with large, deep bruises in unusual locations such as the trunk, back, or areas not typically subject to trauma suggesting serious coagulation factor deficiencies like hemophilia A or B. The temporal evolution of ecchymoses follows a predictable pattern, beginning as red or purple lesions that gradually transition through blue, green, and yellow colors as hemoglobin breakdown products are processed by tissue macrophages. Spontaneous ecchymoses or those resulting from minimal trauma may indicate severe factor deficiencies, anticoagulant medication effects, or acquired coagulopathies such as liver disease or vitamin K deficiency. The assessment of ecchymoses should include evaluation of their size, number, location, relationship to trauma, and associated bleeding symptoms, as these factors help differentiate between inherited bleeding disorders, acquired coagulopathies, and medication-related bleeding complications that require different therapeutic approaches.
4. Mucosal Bleeding - The Internal Manifestations of Hemostatic Failure
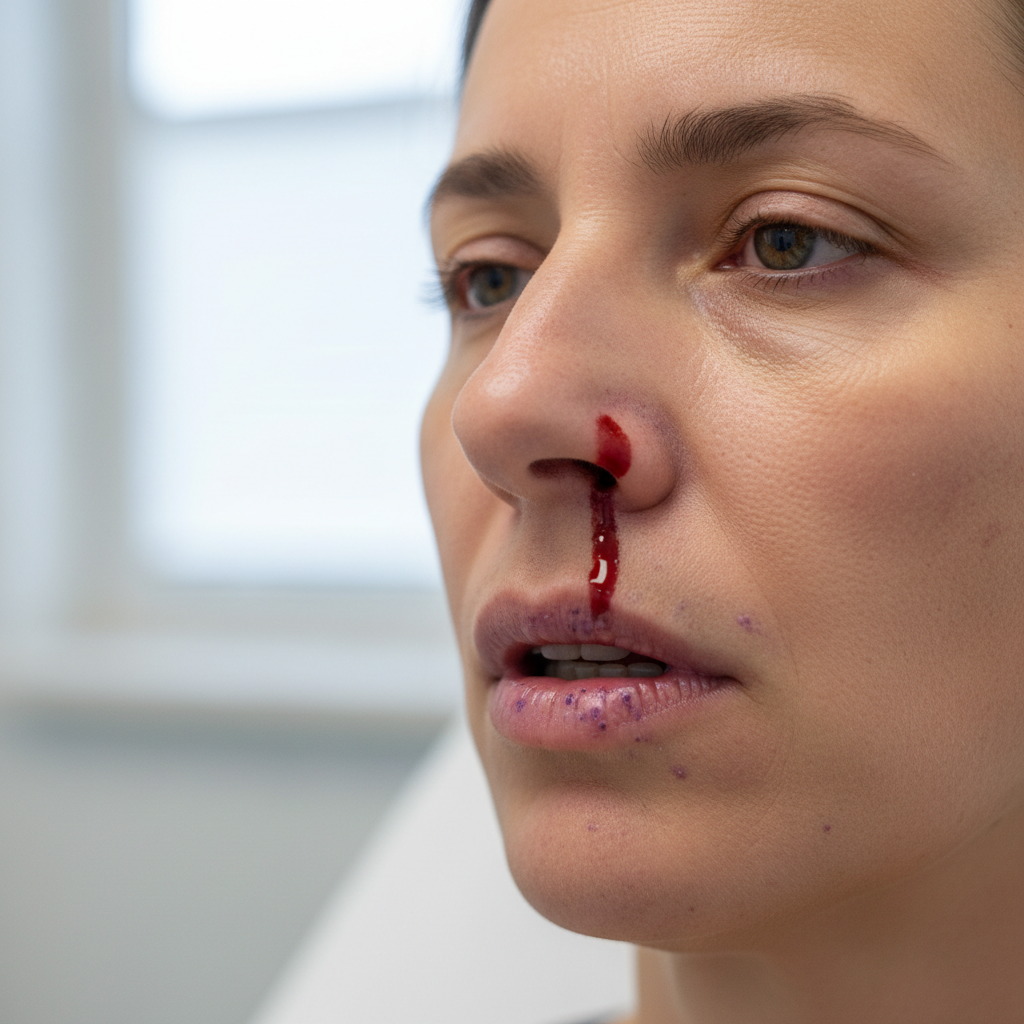
Mucosal bleeding represents a particularly concerning category of bleeding patterns that affects the mucous membranes lining various body cavities, including the oral cavity, nasal passages, gastrointestinal tract, and genitourinary system, often serving as early indicators of significant platelet or coagulation disorders. The mucous membranes are particularly vulnerable to bleeding due to their rich vascular supply, thin epithelial covering, and constant exposure to mechanical trauma from normal physiological functions such as eating, speaking, and breathing. Epistaxis, or nosebleeds, represents one of the most common forms of mucosal bleeding and can range from minor, self-limited episodes to severe, life-threatening hemorrhages requiring emergency intervention. The frequency, duration, and severity of nosebleeds provide important diagnostic information, with recurrent, prolonged, or difficult-to-control epistaxis suggesting underlying bleeding disorders such as von Willebrand disease, platelet function defects, or hereditary hemorrhagic telangiectasia. Oral mucosal bleeding, including gingival bleeding during routine dental hygiene or spontaneous bleeding from the tongue, cheeks, or lips, often indicates platelet disorders or coagulation abnormalities and may be among the earliest signs of hematological malignancies. Gastrointestinal mucosal bleeding can manifest as hematemesis, melena, or hematochezia, potentially indicating both local pathology and systemic bleeding disorders. The evaluation of mucosal bleeding requires careful assessment of the location, frequency, severity, and associated symptoms, as these patterns help differentiate between local anatomical abnormalities and systemic hemostatic disorders requiring comprehensive hematological investigation.
5. Deep Tissue Hematomas - The Signature of Severe Coagulation Defects
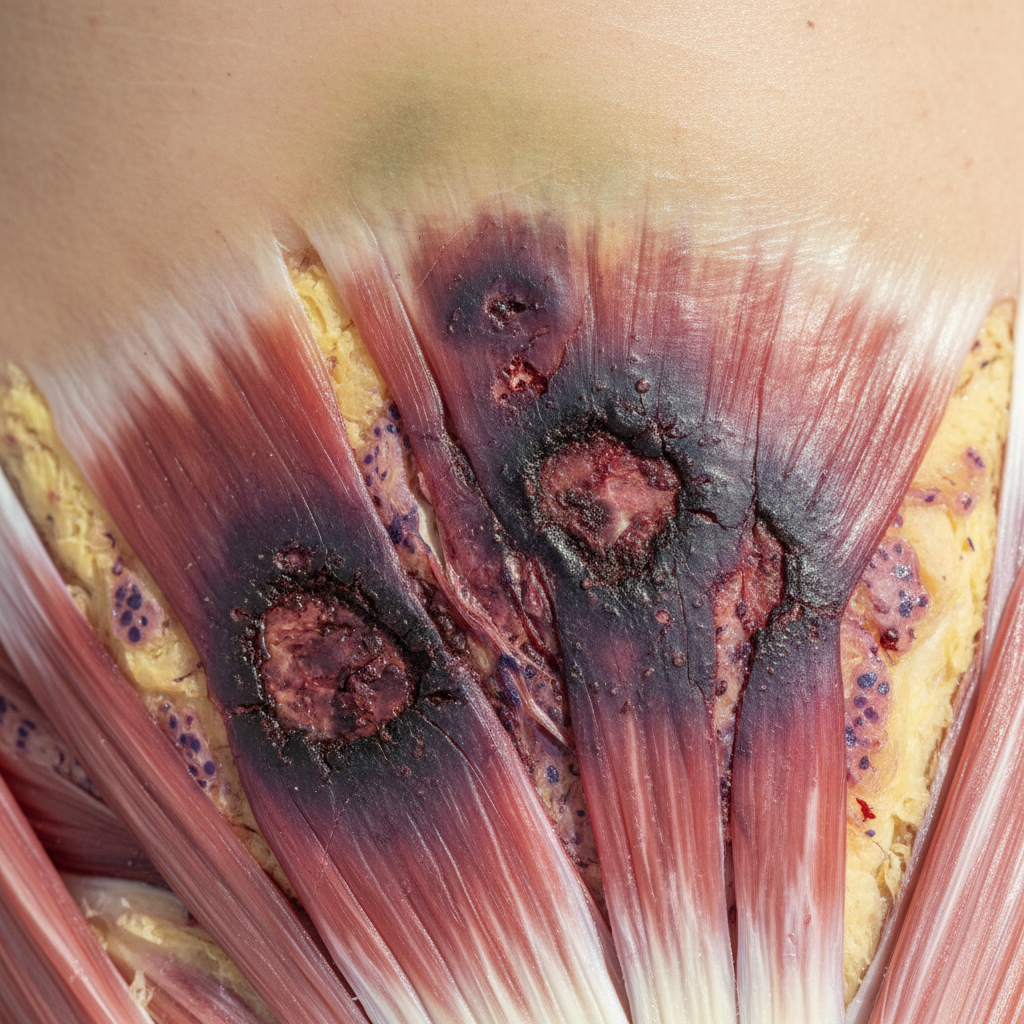
Deep tissue hematomas represent one of the most serious and characteristic bleeding patterns associated with severe coagulation factor deficiencies, manifesting as large collections of blood within muscle compartments, joints, or other deep anatomical spaces that can cause significant morbidity and potentially life-threatening complications. These bleeding episodes typically occur in patients with severe hemophilia A or B, where factor VIII or IX levels are less than 1% of normal, leading to inadequate thrombin generation and unstable clot formation that cannot withstand normal physiological stresses. Intramuscular hematomas commonly affect large muscle groups such as the psoas, quadriceps, gastrocnemius, and forearm flexors, often developing spontaneously or following minimal trauma that would not cause bleeding in individuals with normal hemostasis. The clinical presentation of deep tissue hematomas includes progressive swelling, pain, decreased range of motion, and potential neurovascular compromise due to compartment syndrome or compression of adjacent structures. Retroperitoneal hematomas represent particularly dangerous manifestations that can result in significant blood loss, hemodynamic instability, and compression of vital organs, requiring immediate recognition and aggressive management. The diagnosis of deep tissue hematomas often requires advanced imaging techniques such as ultrasound, computed tomography, or magnetic resonance imaging to assess the extent of bleeding and identify potential complications. Management typically involves immediate factor replacement therapy, immobilization, pain control, and monitoring for complications such as compartment syndrome, infection, or pseudotumor formation that can occur with recurrent bleeding episodes in the same location.
6. Hemarthrosis - The Joint-Specific Bleeding Pattern of Factor Deficiencies
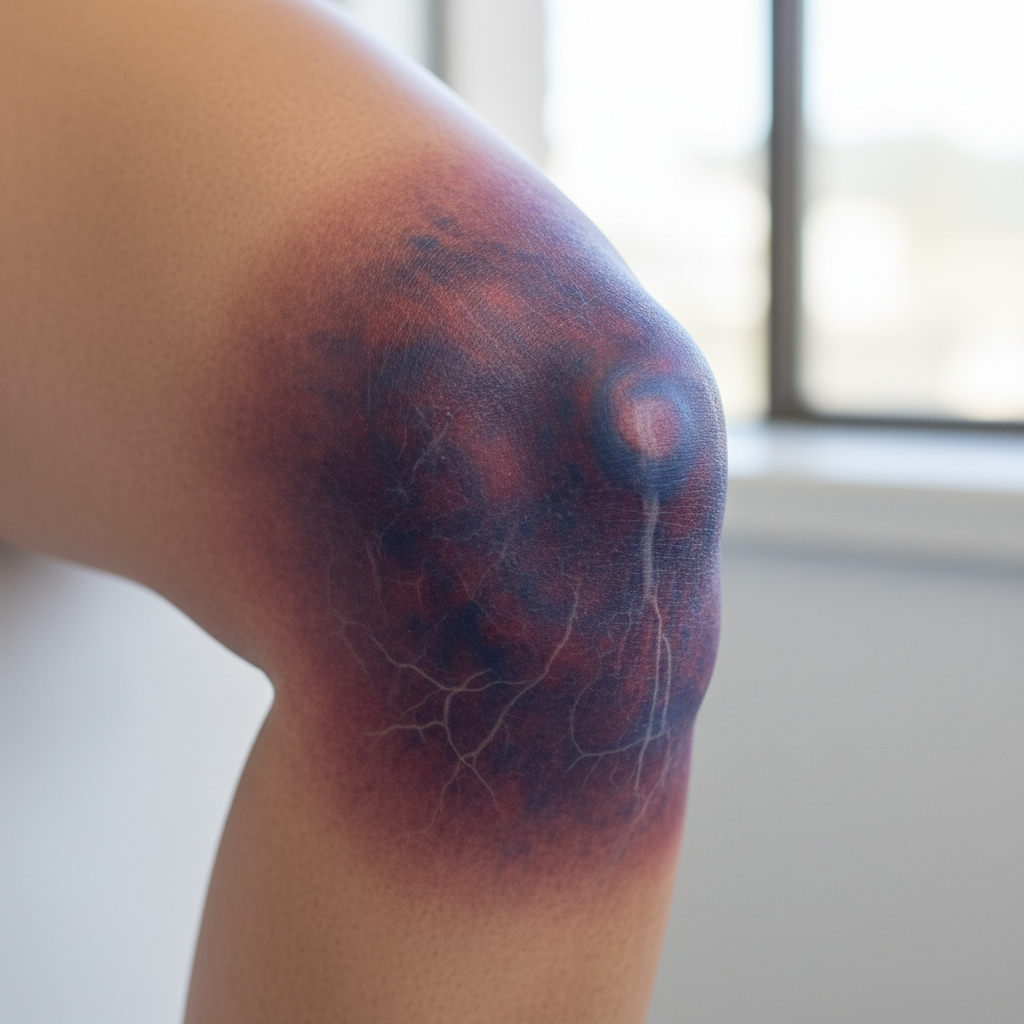
Hemarthrosis, or bleeding into joint spaces, represents a pathognomonic bleeding pattern most commonly associated with severe hemophilia A and B, characterized by spontaneous or trauma-induced bleeding into synovial joints that can lead to progressive joint destruction and chronic arthropathy if not properly managed. The knee, ankle, and elbow joints are most frequently affected due to their weight-bearing function and susceptibility to minor trauma during normal daily activities, though any synovial joint can be involved in severe coagulation factor deficiencies. The pathophysiology of hemarthrosis involves bleeding from the highly vascularized synovial membrane, which lacks the structural support of surrounding tissues and is particularly vulnerable to bleeding when adequate hemostasis cannot be achieved. Acute hemarthrosis presents with rapid onset of joint swelling, pain, warmth, and decreased range of motion, often accompanied by a characteristic feeling of tightness or pressure within the affected joint that patients with hemophilia learn to recognize as an early warning sign. The synovial fluid in hemarthrosis appears bloody or xanthochromic, and aspiration may be necessary for both diagnostic and therapeutic purposes, particularly when infection is suspected or when the joint effusion is causing significant discomfort or functional impairment. Recurrent hemarthrosis episodes lead to chronic synovitis, cartilage destruction, and eventual joint deformity through a process involving iron deposition, inflammatory mediator release, and progressive structural damage that can result in severe disability if prophylactic factor replacement therapy is not implemented. The management of hemarthrosis requires prompt factor replacement therapy, joint immobilization during the acute phase, followed by gradual mobilization and physical therapy to maintain joint function and prevent contracture formation.
7. Prolonged Bleeding After Minor Trauma - The Subtle Warning Sign
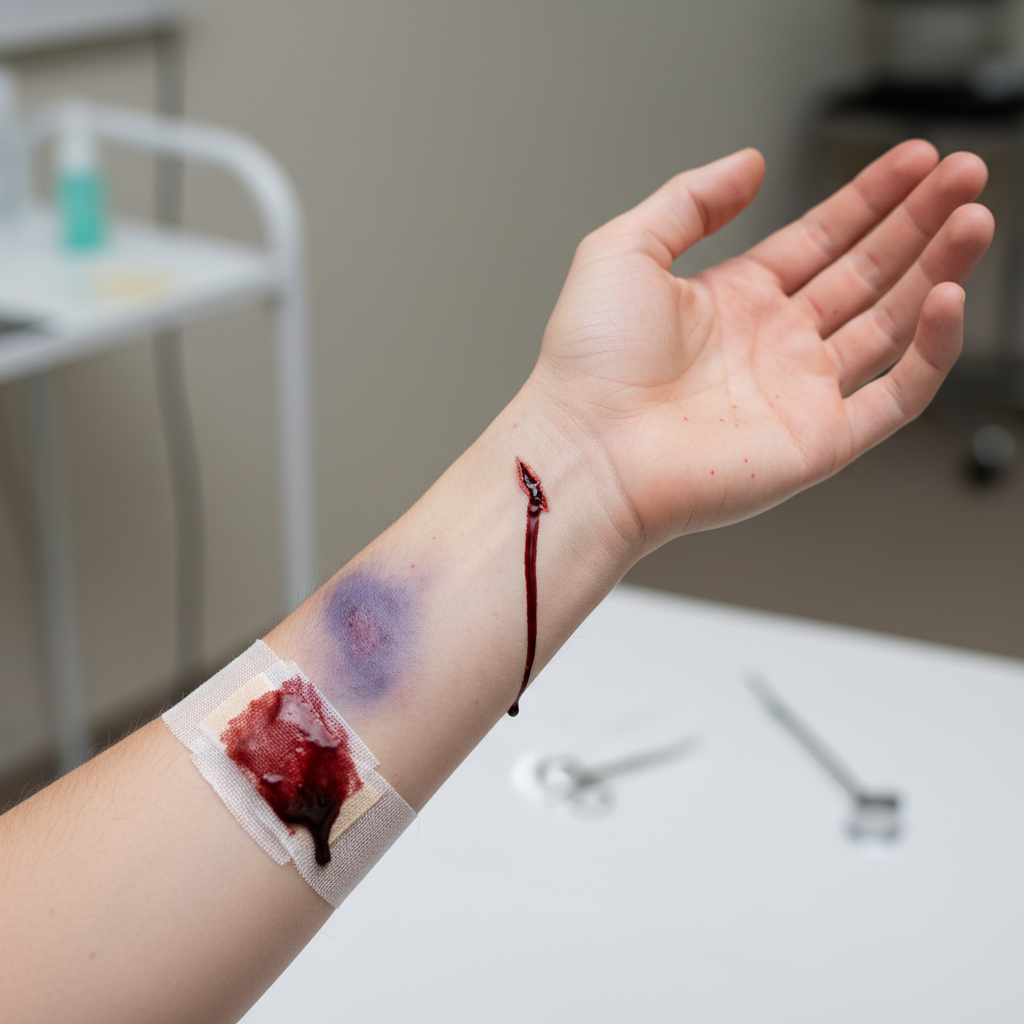
Prolonged bleeding following minor trauma represents a subtle but highly significant bleeding pattern that often serves as the first indication of an underlying bleeding disorder, characterized by bleeding that continues for an abnormally extended period after injuries that would typically stop bleeding within minutes in individuals with normal hemostasis. This bleeding pattern is particularly important because it may be the only manifestation of mild to moderate bleeding disorders, especially in patients with partial factor deficiencies or qualitative platelet disorders who may not experience spontaneous bleeding episodes. The definition of prolonged bleeding varies depending on the type and location of the injury, but generally refers to bleeding that continues for more than 15-20 minutes after minor cuts, dental procedures, or other minor surgical interventions, or bleeding that requires medical intervention to achieve hemostasis. Common scenarios where prolonged bleeding may be observed include dental extractions, minor surgical procedures, circumcision, tonsillectomy, and even routine blood draws or injections that continue to ooze for extended periods. The clinical significance of prolonged bleeding after minor trauma lies in its potential to unmask mild bleeding disorders that might otherwise go undiagnosed until more significant hemostatic challenges arise, such as major surgery or childbirth. Patients with von Willebrand disease, mild hemophilia, or platelet function disorders may present primarily with this bleeding pattern, making careful history-taking essential for identifying individuals at risk for bleeding complications. The evaluation of prolonged bleeding after minor trauma should include detailed bleeding history, family history of bleeding disorders, medication review, and appropriate laboratory testing including platelet count, coagulation studies, and potentially specialized tests for von Willebrand disease or platelet function assessment.
8. Excessive Menstrual Bleeding - The Gender-Specific Bleeding Disorder Indicator

Excessive menstrual bleeding, medically termed menorrhagia, represents a critical bleeding pattern that affects a significant proportion of women with underlying bleeding disorders, serving as both a diagnostic clue and a major source of morbidity that can significantly impact quality of life and overall health status. Heavy menstrual bleeding is defined as menstrual flow lasting longer than seven days, requiring change of sanitary protection every hour for several consecutive hours, flooding or gushing of flow, bleeding between periods, or passage of clots larger than a quarter, though these criteria must be interpreted in the context of individual baseline patterns. The prevalence of bleeding disorders among women presenting with heavy menstrual bleeding is substantially higher than in the general population, with studies indicating that 10-20% of women with menorrhagia have an underlying hemostatic disorder, most commonly von Willebrand disease, platelet function disorders, or mild factor deficiencies. The pathophysiology of excessive menstrual bleeding in bleeding disorders involves inadequate hemostasis at the level of the spiral arteries in the endometrium during menstruation, where normal clot formation and stabilization are essential for controlling blood loss as the functional layer of the endometrium is shed. The impact of menorrhagia extends beyond the bleeding episodes themselves, often leading to iron deficiency anemia, fatigue, decreased exercise tolerance, and significant interference with daily activities, work, and social functioning. Evaluation of women with excessive menstrual bleeding should include comprehensive bleeding history, assessment of menstrual patterns using standardized tools, laboratory evaluation including complete blood count, iron studies, and coagulation studies, with consideration of specialized testing for von Willebrand disease and platelet function disorders when indicated by clinical presentation or family history.
9. Post-Surgical Bleeding - The Stress Test of Hemostatic Function

Post-surgical bleeding represents a critical bleeding pattern that serves as a natural stress test of the hemostatic system, revealing bleeding disorders that may not be apparent under normal physiological conditions but become manifest when the coagulation system is challenged by the extensive tissue trauma and vascular injury associated with surgical procedures. This bleeding pattern is particularly significant because it can lead to serious complications including hemorrhagic shock, need for reoperation, prolonged hospitalization, and increased morbidity and mortality, making preoperative identification of bleeding risk factors essential for optimal surgical outcomes. The timing and characteristics of post-surgical bleeding provide important diagnostic information, with immediate post-operative bleeding often indicating surgical bleeding from inadequate hemostasis or vessel injury, while delayed bleeding occurring hours to days after surgery may suggest underlying coagulation disorders or medication effects. Primary hemostatic disorders, such as platelet dysfunction or thrombocytopenia, typically manifest as immediate, continuous oozing from surgical sites, while secondary hemostatic disorders involving coagulation factor deficiencies may present as delayed bleeding when initial platelet plugs begin to dissolve without adequate fibrin reinforcement. The risk of post-surgical bleeding varies significantly depending on the type and extent of surgery, with procedures involving highly vascularized tissues, extensive dissection, or anticoagulated patients carrying higher bleeding risk that requires careful perioperative management. Preoperative assessment should include detailed bleeding history, family history, medication review, and appropriate laboratory testing, with consideration of specialized coagulation studies in patients with suggestive clinical features or those undergoing high-risk procedures where bleeding complications could be life-threatening.
10. Spontaneous Bleeding Episodes - The Hallmark of Severe Hemostatic Disorders
Spontaneous bleeding episodes represent the most concerning bleeding pattern in the spectrum of hemostatic disorders, characterized by bleeding that occurs without any identifiable trauma or precipitating event, indicating severe dysfunction of the coagulation system that cannot maintain basic hemostatic integrity under normal physiological conditions. These bleeding episodes are pathognomonic of severe bleeding disorders, most commonly severe hemophilia A or B with factor levels less than 1% of normal, severe von Willebrand disease type 3, or severe acquired coagulopathies such as disseminated intravascular coagulation or massive transfusion coagulopathy. The clinical manifestations of spontaneous bleeding can affect virtually any organ system, including intracranial hemorrhage, gastrointestinal bleeding, retroperitoneal hematomas, hemarthrosis, and soft tissue bleeding, with the location and severity often correlating with the underlying hemostatic defect and the degree of factor deficiency or platelet dysfunction. Intracranial hemorrhage represents the most feared complication of spontaneous bleeding, occurring in approximately 2-8% of patients with severe hemophilia and carrying significant morbidity and mortality risk that necessitates immediate recognition and aggressive treatment with factor replacement therapy and neurosurgical consultation when indicated. The frequency of spontaneous bleeding episodes varies among individuals with severe bleeding disorders, influenced by factors such as activity level, joint health, presence of inhibitors, and adherence to prophylactic treatment regimens, with some patients experiencing multiple episodes per month while others may have longer intervals between bleeding events. Management of spontaneous bleeding requires immediate recognition, prompt initiation of appropriate factor replacement or other hemostatic therapy, careful monitoring for complications, and long-term strategies to prevent recurrent episodes through prophylactic treatment, lifestyle modifications, and comprehensive multidisciplinary care.
11. Delayed Bleeding Patterns - The Secondary Hemostatic Failure Indicators