10 Jaw and Facial Pain Patterns That Extend Beyond Dental Causes
When facial pain strikes, the immediate assumption often points toward dental issues – a cavity, an abscess, or perhaps wisdom teeth complications. However, the intricate network of nerves, muscles, joints, and blood vessels throughout the head and neck region creates a complex web where pain can originate from numerous non-dental sources. The trigeminal nerve, the largest cranial nerve responsible for facial sensation, branches extensively throughout the face, making it possible for pain to radiate and manifest in patterns that can easily mislead both patients and healthcare providers. Understanding these alternative pain sources is crucial because misdiagnosis can lead to unnecessary dental procedures, prolonged suffering, and inadequate treatment of the underlying condition. The jaw and facial region serves as a convergence point where neurological, muscular, vascular, and structural systems intersect, creating a sophisticated pain network that extends far beyond the realm of dentistry. This comprehensive exploration will unveil ten distinct pain patterns that masquerade as dental problems, providing insight into their origins, characteristics, and proper management approaches to help individuals and healthcare providers navigate this complex diagnostic landscape.
1. Temporomandibular Joint Disorders (TMJ/TMD) - The Great Mimicker

Temporomandibular joint disorders represent one of the most common non-dental causes of facial pain, affecting millions of individuals worldwide and frequently masquerading as dental pathology. The temporomandibular joint functions as a complex hinge mechanism that connects the jawbone to the skull, incorporating a sophisticated system of muscles, ligaments, and cartilage that enables speaking, chewing, and yawning. When this system becomes dysfunctional due to factors such as teeth grinding, jaw clenching, trauma, arthritis, or structural abnormalities, it can generate pain patterns that closely mimic dental problems. Patients with TMJ disorders often experience aching pain in the jaw area, difficulty opening the mouth, clicking or popping sounds during jaw movement, and pain that radiates to the teeth, ears, neck, and shoulders. The pain typically worsens with jaw movement and may be accompanied by muscle tension headaches. What makes TMJ disorders particularly deceptive is their ability to cause referred pain to specific teeth, leading patients to seek dental treatment for what appears to be a tooth problem. The condition can be triggered or exacerbated by stress, poor posture, excessive gum chewing, or dental work that alters the bite. Proper diagnosis requires a comprehensive evaluation of jaw function, muscle palpation, and sometimes imaging studies to assess joint structure and movement patterns.
2. Trigeminal Neuralgia - Electric Shock Pain Phenomenon

Trigeminal neuralgia stands as one of the most excruciating pain conditions known to medicine, characterized by sudden, severe, electric shock-like pain episodes that can be easily mistaken for acute dental emergencies. This neurological disorder affects the trigeminal nerve, which carries sensation from the face to the brain, and typically manifests as brief but intensely painful episodes lasting from seconds to minutes. The pain usually follows the distribution of one or more branches of the trigeminal nerve, commonly affecting areas around the upper jaw, lower jaw, or cheek, making it particularly likely to be confused with dental pathology. Patients often describe the pain as feeling like an electric shock, stabbing sensation, or burning that can be triggered by light touch, speaking, chewing, or even a gentle breeze across the face. The condition predominantly affects individuals over 50 years of age and is more common in women than men. What distinguishes trigeminal neuralgia from dental pain is its characteristic pattern of sudden onset and offset, the triggering nature of light stimuli, and the presence of trigger zones on the face where minimal contact can precipitate an attack. The pain is typically unilateral and follows specific nerve pathways, unlike the more diffuse or localized nature of dental pain. Between episodes, patients are usually completely pain-free, which contrasts with the continuous or throbbing nature of most dental conditions.
3. Cluster Headaches - The Suicide Headache's Dental Disguise

Cluster headaches, often referred to as "suicide headaches" due to their excruciating intensity, represent a primary headache disorder that can manifest with pain patterns closely resembling severe dental problems, particularly in the upper jaw and temple regions. These headaches occur in cyclical patterns or clusters, typically lasting 15 minutes to three hours and recurring multiple times per day during active periods that can span weeks to months. The pain is characteristically described as a severe, burning, or piercing sensation that centers around one eye but frequently radiates to the temple, upper jaw, and teeth on the affected side. This radiation pattern often leads patients to seek emergency dental care, convinced they have a severe tooth abscess or other dental emergency. Cluster headaches are accompanied by distinctive autonomic symptoms including eye redness, tearing, nasal congestion, and eyelid drooping on the affected side, which can help differentiate them from dental causes. The condition predominantly affects men and often follows a circadian rhythm, with attacks frequently occurring at the same time each day or night. Unlike dental pain, cluster headaches are not typically aggravated by chewing or biting pressure, and the pain quality is distinctly different from the throbbing or aching associated with dental pathology. The cyclical nature of cluster periods, followed by remission phases that can last months or years, provides another important diagnostic clue that distinguishes this condition from dental problems.
4. Sinusitis and Sinus-Related Pain - The Upper Tooth Imposter

Sinusitis represents a frequently overlooked cause of facial and dental pain that can perfectly mimic upper tooth problems, leading to unnecessary dental procedures and prolonged patient suffering. The maxillary sinuses, located directly above the upper teeth, share intimate anatomical relationships with the tooth roots, particularly the premolars and molars, creating a scenario where sinus inflammation can directly affect dental structures and vice versa. When sinuses become inflamed due to infection, allergies, or other causes, the resulting pressure and inflammation can create pain that radiates directly to the upper teeth, making patients convinced they have dental problems requiring immediate attention. This sinus-related dental pain typically affects multiple teeth simultaneously rather than a single tooth, and is often accompanied by characteristic sinus symptoms such as nasal congestion, postnasal drip, facial pressure, and sometimes fever. The pain tends to worsen when bending forward, lying down, or during changes in atmospheric pressure, which are not typical characteristics of dental pain. Additionally, sinus-related tooth pain often has a dull, aching quality that differs from the sharp, throbbing nature of dental infections. Chronic sinusitis can create persistent low-grade pain that mimics chronic dental conditions, while acute sinusitis may produce severe pain that resembles dental abscesses. Understanding this connection is crucial because treating the underlying sinus condition often resolves the dental symptoms completely, avoiding unnecessary dental interventions.
5. Migraine and Tension Headaches - Referred Pain Networks
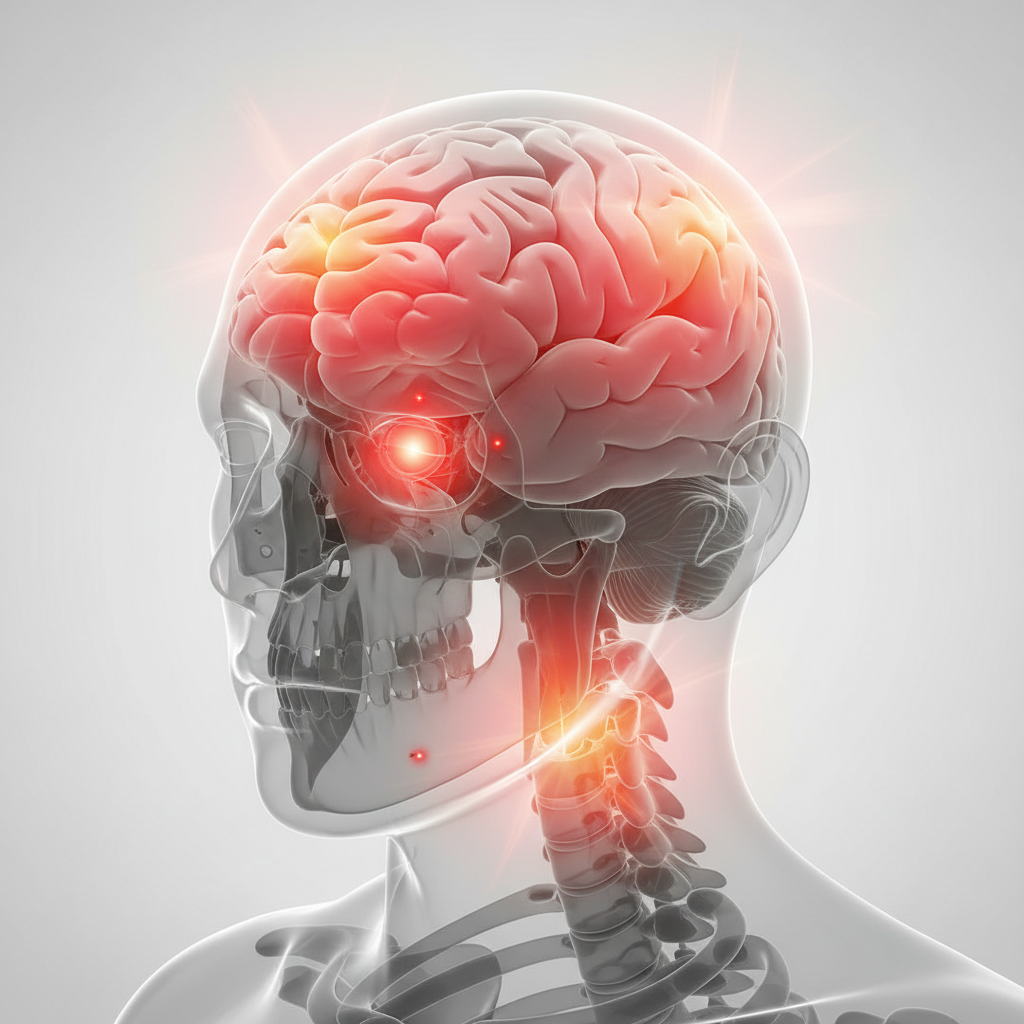
Migraine and tension-type headaches frequently generate referred pain patterns that can convincingly simulate dental problems, creating diagnostic challenges that require careful evaluation to distinguish neurological from odontological causes. Migraines, characterized by their complex neurological mechanisms involving trigeminal nerve activation and vascular changes, can produce pain that radiates to the jaw, teeth, and facial regions through shared neural pathways. The trigeminal-vascular system plays a central role in migraine pathophysiology, and when activated, can create pain sensations that seem to originate from dental structures. Patients experiencing migraine-related facial pain often report aching or throbbing sensations in the upper or lower jaw, tooth sensitivity, and sometimes even the sensation of dental pressure or looseness. Tension-type headaches, while typically associated with band-like head pressure, can also manifest with jaw and facial pain due to muscle tension and referred pain patterns. The muscles of mastication, including the temporalis and masseter muscles, often become tense during headache episodes, creating additional pain that can be perceived as dental in origin. What distinguishes headache-related facial pain from dental problems is the association with typical headache symptoms such as light sensitivity, sound sensitivity, nausea, and the characteristic headache pain patterns. Additionally, headache-related facial pain often responds to headache medications and treatments rather than dental interventions, providing an important therapeutic diagnostic clue.
6. Myofascial Pain Syndrome - Muscle Trigger Points and Referred Pain

Myofascial pain syndrome affecting the muscles of mastication and facial expression represents a significant source of non-dental facial pain that can create convincing dental-like symptoms through complex referred pain mechanisms. This condition involves the development of trigger points within muscle fibers – hyperirritable spots that, when stimulated, produce both local pain and referred pain to distant areas. The muscles most commonly involved include the masseter, temporalis, pterygoid muscles, and various neck muscles, all of which can refer pain to dental structures when trigger points become active. Patients with myofascial pain syndrome often experience deep, aching pain that may be constant or intermittent, accompanied by muscle stiffness, limited jaw opening, and tenderness to palpation over affected muscles. The referred pain patterns can be remarkably specific, with trigger points in the masseter muscle commonly referring pain to the posterior teeth, while temporalis trigger points may create pain that seems to originate from the upper teeth and temple region. This condition often develops secondary to factors such as stress, poor posture, teeth grinding, prolonged jaw clenching, or trauma to the head and neck region. The pain typically worsens with muscle use, such as chewing or speaking, which can further confuse the clinical picture by mimicking dental pain aggravated by function. Unlike dental pain, myofascial pain often responds to muscle relaxation techniques, trigger point therapy, and stress management, while dental treatments provide little relief.
7. Cervical Spine Disorders - The Neck-Face Pain Connection
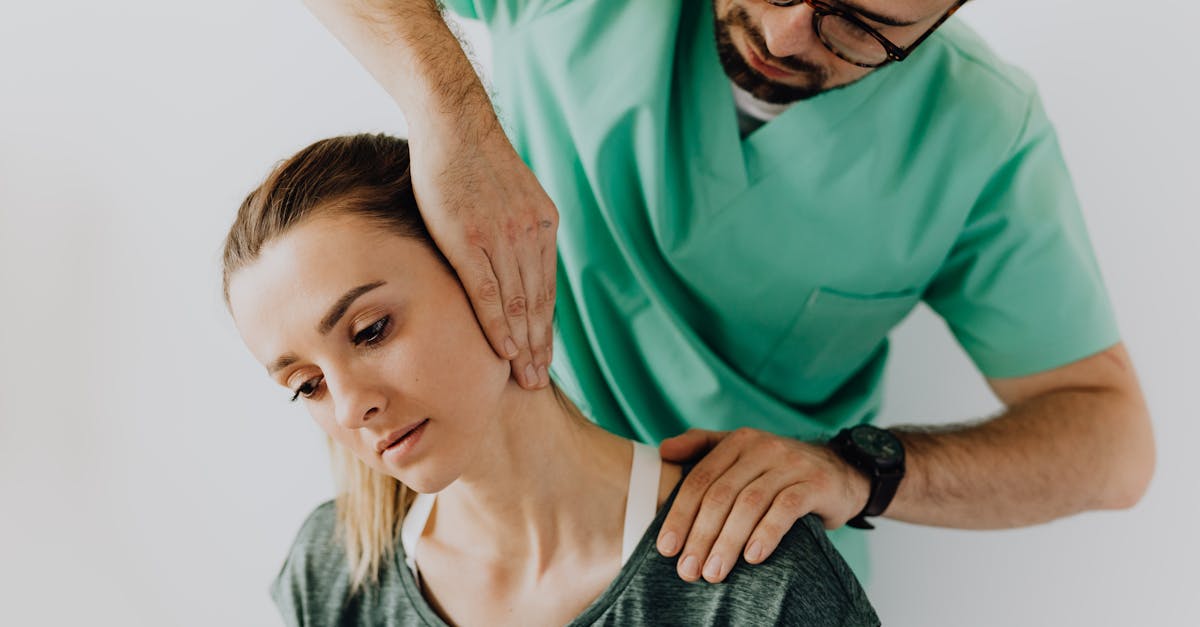
Cervical spine disorders create a fascinating and often overlooked source of facial and jaw pain through complex neurological connections that link the upper cervical segments with trigeminal nerve pathways. The upper cervical spine, particularly the C1-C3 vertebrae, shares neural connections with the trigeminal nerve through the trigeminocervical complex, creating pathways for referred pain from neck problems to manifest as facial and dental pain. Conditions such as cervical arthritis, herniated discs, muscle strain, or atlantooccipital joint dysfunction can generate pain that radiates to the jaw, temple, and even specific tooth regions through these shared neural pathways. Patients with cervical-related facial pain often experience a combination of neck stiffness, headaches, and facial pain that may worsen with neck movement or certain head positions. The pain quality is typically described as deep, aching, or burning, and may be accompanied by muscle tension in the neck and shoulders. What makes cervical spine disorders particularly deceptive as a source of facial pain is their ability to create symptoms that seem entirely unrelated to the neck, leading patients and healthcare providers to focus on local facial or dental causes. The pain patterns can be quite specific, with upper cervical problems commonly referring pain to the temple and upper jaw regions, while lower cervical issues may affect the lower jaw and ear areas. Proper diagnosis requires evaluation of neck mobility, muscle tension patterns, and sometimes advanced imaging to identify underlying cervical pathology.
8. Vascular Disorders - Arterial and Venous Pain Patterns
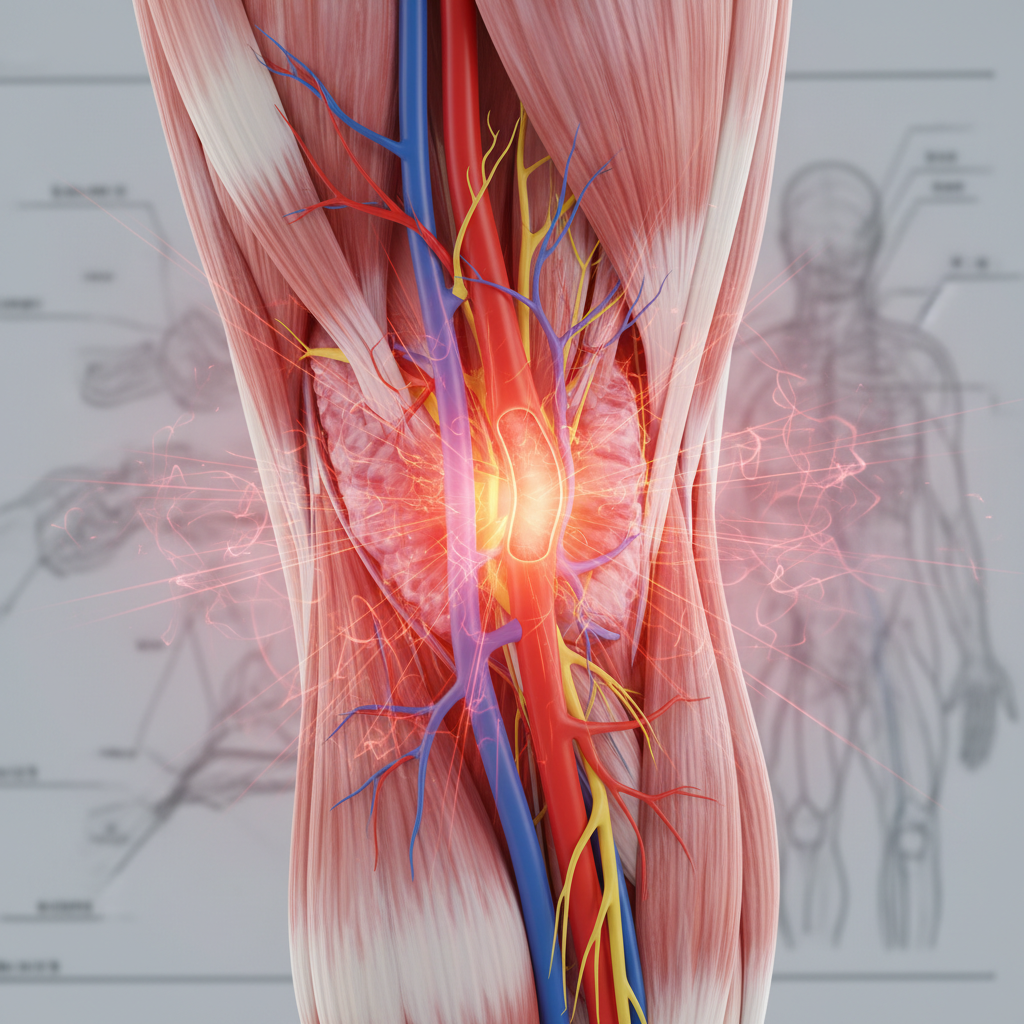
Vascular disorders affecting the head and neck region can create distinctive pain patterns that may be mistaken for dental problems, particularly when they involve blood vessels in close proximity to dental structures. Giant cell arteritis, also known as temporal arteritis, represents one of the most serious vascular causes of facial pain, typically affecting individuals over 50 years of age and creating severe, burning pain in the temple region that can radiate to the jaw and teeth. This inflammatory condition affects medium and large arteries and can lead to serious complications including vision loss if not promptly recognized and treated. The pain is often described as severe and constant, may worsen with chewing due to jaw claudication, and is frequently accompanied by systemic symptoms such as fever, weight loss, and elevated inflammatory markers. Carotid artery dissection, while less common, can create facial and neck pain that may be confused with dental or TMJ problems, particularly when the pain radiates to the jaw region. Venous disorders, including thrombosis of facial veins or cavernous sinus thrombosis, can also create facial pain and swelling that might initially suggest dental infection. Vascular malformations, such as arteriovenous malformations in the facial region, can create pulsatile pain that differs significantly from typical dental pain patterns. The key distinguishing features of vascular pain include its relationship to blood flow patterns, potential pulsatile quality, association with vascular risk factors, and often the presence of other vascular symptoms or signs.
9. Neurological Conditions - Beyond Trigeminal Neuralgia
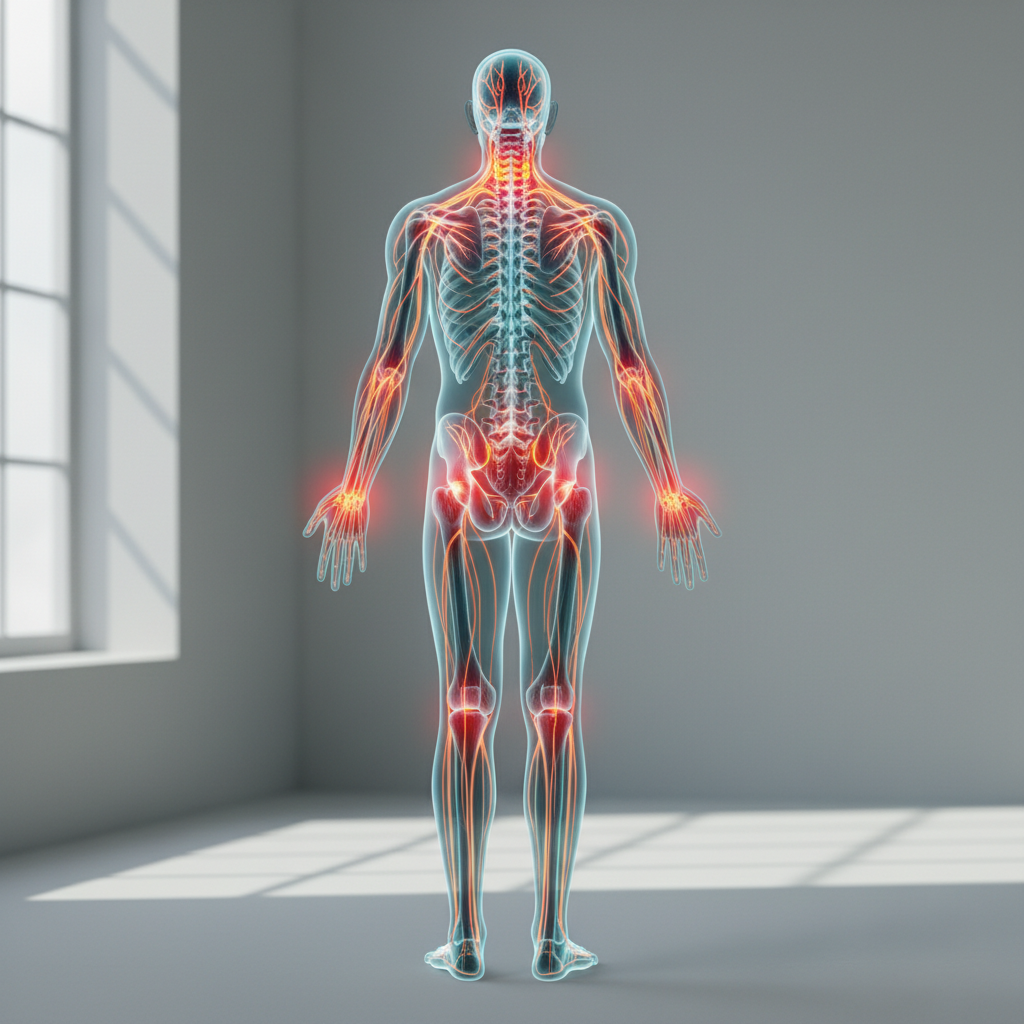
While trigeminal neuralgia represents the most well-known neurological cause of facial pain, numerous other neurological conditions can create pain patterns that mimic dental problems through various mechanisms involving nerve dysfunction, inflammation, or damage. Atypical facial pain, also known as persistent idiopathic facial pain, creates a constant, burning, or aching sensation that differs from the sharp, electric quality of classical trigeminal neuralgia but can still be mistaken for dental pathology. This condition often affects a broader area than classical trigeminal neuralgia and may not follow specific nerve distributions, making diagnosis particularly challenging. Post-herpetic neuralgia following herpes zoster infection of the trigeminal nerve can create persistent, burning pain in the distribution of the affected nerve branch, potentially affecting areas that include dental regions. Multiple sclerosis can occasionally present with trigeminal nerve involvement, creating facial pain that may be confused with dental problems, particularly in younger patients where MS might not be immediately suspected. Glossopharyngeal neuralgia, while primarily affecting the throat and ear regions, can sometimes create referred pain to the jaw and lower teeth through shared neural pathways. Brain tumors, particularly those affecting the cerebellopontine angle or trigeminal nerve pathways, can create facial pain that gradually develops and may initially be attributed to dental causes. The distinguishing features of these neurological conditions often include their specific pain qualities, associated neurological symptoms, and response patterns to neurological medications rather than dental treatments.
10. Systemic Conditions - The Whole-Body Connection

Systemic medical conditions can manifest with facial and jaw pain through various mechanisms, creating symptoms that may initially appear to be dental in origin but actually represent manifestations of broader health issues. Fibromyalgia, a chronic pain condition characterized by widespread musculoskeletal pain, frequently includes facial and jaw pain as part of its symptom complex, with patients experiencing tender points in the facial muscles and TMJ region. The pain associated with fibromyalgia is typically described as deep, aching, and constant, often accompanied by fatigue, sleep disturbances, and cognitive difficulties that help distinguish it from isolated dental problems. Autoimmune conditions such as rheumatoid arthritis can affect the temporomandibular joint, creating pain and dysfunction that may be mistaken for dental issues, while systemic lupus erythematosus can cause oral ulcers and facial pain through various mechanisms including vasculitis and nerve involvement. Temporal arteritis, as mentioned previously, represents a systemic inflammatory condition that can create severe facial pain mimicking dental emergencies. Cardiac conditions, particularly myocardial infarction, can occasionally present with referred pain to the jaw and teeth, especially in women, making it crucial to consider cardiac causes in appropriate clinical contexts. Thyroid disorders can affect muscle function and pain perception, potentially contributing to facial and jaw pain patterns. Vitamin deficiencies, particularly B12 deficiency, can cause neurological symptoms including facial pain and altered sensation that might be confused with dental nerve problems. Recognition of these systemic connections is essential for proper diagnosis and treatment, as addressing the underlying systemic condition often resolves the facial pain symptoms.
11. Diagnostic Strategies and Clinical Pearls - Navigating the Complexity
Successfully differentiating non-dental facial pain from genuine dental pathology requires a systematic approach that combines careful history-taking, physical examination, and appropriate use of diagnostic tools to unravel the complex web of potential causes. The clinical history provides crucial clues, with particular attention to pain quality, timing, triggers, associated symptoms, and response to previous treatments offering valuable diagnostic information. Sharp, electric-like pain suggests neurological causes, while deep, aching pain may indicate muscular or joint problems, and throbbing, pulsatile pain might suggest vascular involvement. The temporal pattern of pain – whether constant, intermittent, or episodic – provides additional diagnostic clues, with cluster patterns suggesting headache disorders and trigger-related episodes pointing toward neurological conditions. Physical examination should extend beyond the oral cavity to include palpation of facial muscles, assessment of jaw function, evaluation of neck mobility, and examination for trigger points or areas of referred pain. Dental examination remains important to rule out genuine dental pathology, but should be interpreted in the context of the broader clinical picture. Diagnostic imaging may include dental radiographs to exclude dental causes, but may also require CT or MRI imaging to evaluate sinuses, TMJ structures, or neurological pathways depending on clinical suspicion. Therapeutic trials can provide valuable diagnostic information, with response to specific medications or treatments helping to confirm suspected diagnoses. The key to successful diagnosis lies in maintaining a broad differential diagnosis, recognizing when symptoms don't fit typical dental patterns, and being willing to refer to appropriate specialists when non-dental causes are suspected, ultimately ensuring patients receive proper treatment for their underlying conditions rather than unnecessary dental procedures.