10 Facial Sensation Changes That Prompt Neurological Evaluation
The human face serves as a remarkable neurological interface, containing one of the most densely innervated regions of the body through the trigeminal nerve system and its complex network of sensory pathways. When facial sensation begins to change—whether through numbness, tingling, pain, or altered perception—these symptoms often represent the earliest warning signs of significant neurological conditions that require immediate medical attention. The trigeminal nerve, cranial nerve V, carries sensory information from the face to the brain through three distinct divisions: the ophthalmic, maxillary, and mandibular branches, each responsible for specific facial regions. Changes in facial sensation can indicate everything from benign conditions like Bell's palsy to serious disorders such as multiple sclerosis, brain tumors, or stroke. Understanding these warning signs becomes crucial because early detection and intervention can dramatically improve outcomes for patients experiencing neurological decline. The face's rich sensory network makes it an exceptional diagnostic tool, as subtle changes in sensation patterns can provide neurologists with precise localization information about where nervous system damage or dysfunction may be occurring. This comprehensive exploration examines ten critical facial sensation changes that should prompt immediate neurological evaluation, offering both medical professionals and patients essential knowledge about recognizing these potentially serious symptoms before they progress to more severe neurological complications.
1. Unilateral Facial Numbness - The Classic Warning Sign
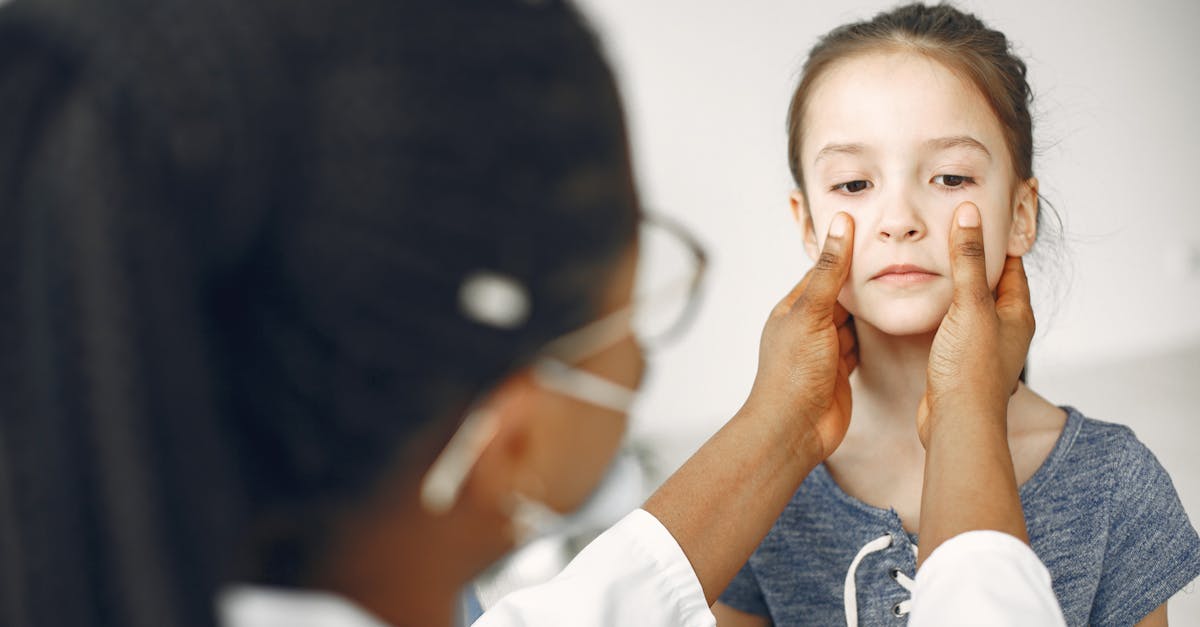
Unilateral facial numbness represents one of the most significant red flags in neurological medicine, as it typically indicates damage or dysfunction affecting specific neural pathways on one side of the nervous system. This condition manifests as a complete or partial loss of sensation affecting one half of the face, often following the precise anatomical distribution of trigeminal nerve branches. Patients frequently describe the sensation as feeling like their face has been injected with dental anesthetic, creating a profound disconnect between their visual perception of touch and their actual sensory experience. The underlying causes of unilateral facial numbness span a broad spectrum of neurological conditions, including stroke, transient ischemic attacks, brain tumors, multiple sclerosis plaques, and trigeminal neuralgia. When stroke occurs in the brainstem or thalamic regions, facial numbness often appears as part of a constellation of symptoms that may include weakness, speech difficulties, or coordination problems. Brain tumors, particularly those affecting the cerebellopontine angle or brainstem, can compress trigeminal nerve pathways, producing progressive numbness that gradually worsens over weeks or months. Multiple sclerosis frequently presents with facial numbness as an early symptom, as demyelinating lesions can affect trigeminal pathways at various points along their course from the brainstem to the peripheral nerve branches. The critical nature of unilateral facial numbness lies in its potential to herald serious, treatable conditions where early intervention can prevent permanent neurological damage and significantly improve patient outcomes.
2. Progressive Facial Tingling - Early Neurodegeneration Signals
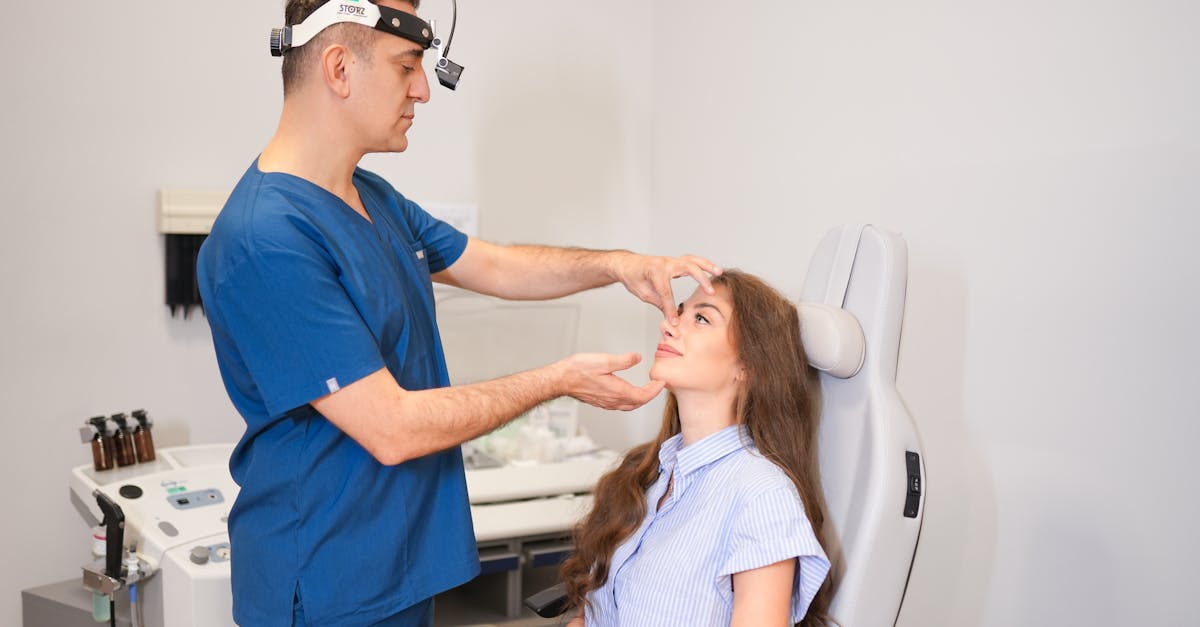
Progressive facial tingling, characterized by persistent pins-and-needles sensations that gradually intensify over time, often serves as an early harbinger of neurodegenerative processes affecting the central or peripheral nervous system. Unlike acute onset symptoms that might indicate vascular events, progressive tingling typically develops over weeks to months, creating a slowly evolving pattern of sensory disturbance that patients may initially dismiss as minor irritation. This symptom commonly manifests in conditions such as multiple sclerosis, where inflammatory demyelination affects nerve conduction, creating abnormal electrical activity that the brain interprets as tingling or paresthesias. The progression pattern provides crucial diagnostic information, as symmetric bilateral tingling might suggest systemic conditions like vitamin B12 deficiency or diabetes, while asymmetric or unilateral progression often points toward focal neurological lesions. Patients frequently report that the tingling sensation intensifies during periods of stress, fatigue, or temperature changes, reflecting the increased metabolic demands placed on already compromised neural tissue. In multiple sclerosis, facial tingling may be accompanied by Lhermitte's sign, where neck flexion produces electric shock-like sensations radiating down the spine and into the extremities. Brain tumors affecting sensory cortex regions can also produce progressive tingling as they gradually expand and compress surrounding neural tissue. The insidious nature of progressive facial tingling makes it particularly concerning because patients may adapt to the sensation over time, potentially delaying medical evaluation until more severe neurological symptoms develop. Early recognition and neurological assessment of progressive facial tingling can lead to timely diagnosis and treatment initiation, potentially slowing or halting the underlying neurodegenerative process.
3. Sudden Onset Facial Pain - Vascular and Inflammatory Indicators

Sudden onset facial pain represents a neurological emergency that demands immediate medical attention, as it frequently indicates acute vascular events, inflammatory processes, or nerve compression syndromes requiring urgent intervention. This type of pain typically manifests as severe, sharp, or burning sensations that develop within minutes to hours, creating intense discomfort that significantly impacts patient quality of life and daily functioning. Trigeminal neuralgia, often called the "suicide disease" due to its excruciating nature, presents with sudden, electric shock-like pain episodes lasting seconds to minutes, typically triggered by light touch, chewing, or speaking. The pain follows specific trigeminal nerve distributions, most commonly affecting the maxillary or mandibular divisions, and can be so severe that patients avoid eating, speaking, or even gentle facial contact. Vascular causes of sudden facial pain include posterior circulation strokes affecting the brainstem, where damage to trigeminal pathways can produce both sensory loss and severe neuropathic pain. Inflammatory conditions such as herpes zoster affecting the trigeminal nerve create intense burning pain that may precede the characteristic vesicular rash by several days, making early diagnosis challenging but crucial for antiviral treatment effectiveness. Giant cell arteritis, a systemic inflammatory condition affecting medium and large arteries, can cause sudden facial pain when temporal arteries become inflamed, potentially leading to vision loss if left untreated. The sudden nature of facial pain onset distinguishes it from chronic conditions and suggests active pathological processes that may be reversible with appropriate treatment. Immediate neurological evaluation allows for rapid diagnostic workup including imaging studies and laboratory tests that can identify treatable causes before permanent nerve damage occurs.
4. Temperature Sensation Loss - Spinothalamic Tract Dysfunction
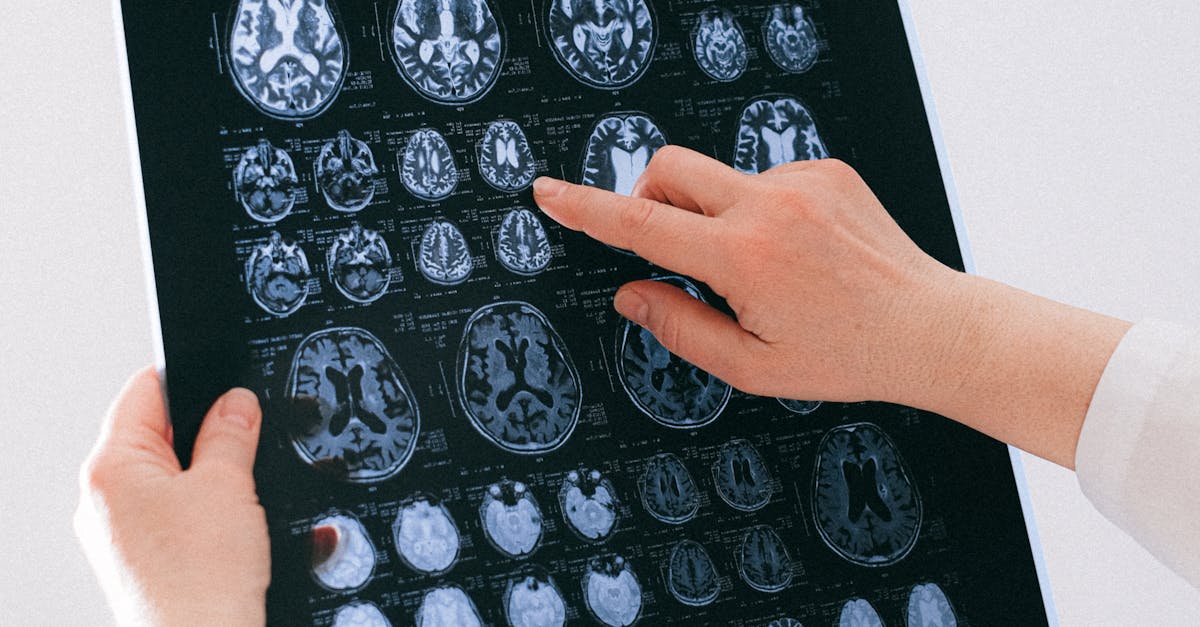
The loss of temperature sensation in facial regions represents a highly specific neurological finding that indicates dysfunction within the spinothalamic tract system, providing neurologists with precise localization information about central nervous system lesions. This sophisticated sensory modality relies on specialized thermoreceptors and unmyelinated nerve fibers that transmit temperature information through distinct pathways from other sensory modalities, making isolated temperature loss a valuable diagnostic sign. Patients experiencing temperature sensation loss often report inability to distinguish between hot and cold objects touching their face, creating potential safety hazards as they may inadvertently burn themselves on hot surfaces or fail to recognize dangerous temperature extremes. The anatomical organization of temperature pathways makes this symptom particularly useful for localizing brainstem lesions, as temperature fibers cross the midline shortly after entering the central nervous system and travel in specific brainstem regions. Lateral medullary syndrome, also known as Wallenberg syndrome, classically presents with ipsilateral facial temperature loss combined with contralateral body temperature loss, creating a distinctive crossed sensory pattern that helps neurologists pinpoint the exact location of brainstem damage. Syringobulbia, a rare condition involving cyst formation within the brainstem, can selectively affect temperature pathways while sparing other sensory modalities, producing the characteristic "dissociated sensory loss" pattern. Multiple sclerosis plaques affecting brainstem regions can also disrupt temperature sensation, often as part of more complex symptom patterns including coordination difficulties and cranial nerve dysfunction. The preservation of light touch and vibration sensation in the presence of temperature loss creates a distinctive clinical picture that guides diagnostic imaging toward specific brainstem regions. Recognition of temperature sensation loss requires careful clinical examination using warm and cold stimuli, as patients may not spontaneously report this subtle but significant neurological finding.
5. Altered Taste Perception - Cranial Nerve Integration Issues

Altered taste perception affecting facial regions represents a complex neurological symptom that reflects dysfunction in the intricate network of cranial nerves responsible for gustatory sensation, including the facial nerve (VII), glossopharyngeal nerve (IX), and their central processing pathways. This symptom extends beyond simple taste changes to encompass the broader concept of flavor perception, which integrates taste, smell, and trigeminal sensations to create the complete sensory experience of eating and drinking. Patients may report metallic tastes, complete taste loss (ageusia), or distorted taste perception (dysgeusia), symptoms that can significantly impact nutrition, social interactions, and overall quality of life. The facial nerve carries taste sensation from the anterior two-thirds of the tongue through the chorda tympani, making facial nerve dysfunction a common cause of taste alterations that may accompany other facial symptoms. Bell's palsy, the most common cause of acute facial nerve dysfunction, frequently produces taste changes alongside facial weakness and altered facial sensation, creating a constellation of symptoms that can be particularly distressing for patients. Central nervous system lesions affecting the brainstem gustatory nuclei or their connections to higher cortical areas can produce more complex taste disturbances that may be accompanied by other neurological symptoms. Brain tumors, particularly those affecting the temporal lobe or brainstem regions, can disrupt taste processing pathways and create persistent taste alterations that serve as early warning signs of neurological disease. Stroke affecting specific brainstem regions can produce sudden onset taste changes that may be overlooked in the acute setting but provide important diagnostic information about lesion location. The integration of taste with facial sensation makes altered taste perception a valuable component of comprehensive neurological assessment, as it can provide additional evidence of cranial nerve dysfunction that might otherwise be missed. Understanding the relationship between taste changes and facial sensation helps clinicians develop more complete diagnostic pictures and treatment plans for patients experiencing complex neurological symptoms.
6. Facial Muscle Weakness with Sensory Changes - Motor-Sensory Integration

The combination of facial muscle weakness with concurrent sensory changes represents a particularly concerning neurological presentation that suggests extensive damage to neural pathways controlling both motor and sensory functions of the face. This dual symptom complex often indicates lesions affecting multiple cranial nerves or central nervous system regions where motor and sensory pathways are anatomically adjacent, making it a high-priority finding requiring immediate neurological evaluation. Facial nerve palsy, whether from Bell's palsy, Ramsay Hunt syndrome, or other causes, typically produces weakness of facial muscles on the affected side while potentially disrupting taste sensation and causing altered facial sensation due to the complex anatomy of the facial nerve and its branches. The pattern of weakness combined with sensory loss provides crucial diagnostic information, as peripheral facial nerve lesions produce different patterns compared to central nervous system lesions affecting the facial motor cortex or brainstem nuclei. Brainstem strokes affecting the facial nucleus or its connections can produce both facial weakness and sensory disturbances, often accompanied by other brainstem signs such as coordination difficulties, eye movement abnormalities, or swallowing problems. Cerebellopontine angle tumors, including acoustic neuromas and meningiomas, frequently compress both facial and trigeminal nerves as they grow, creating progressive weakness and numbness that may develop slowly over months or years. Multiple sclerosis can affect both motor and sensory pathways simultaneously when demyelinating plaques involve brainstem regions containing facial motor and sensory nuclei. The temporal relationship between motor and sensory symptom onset provides additional diagnostic clues, as simultaneous onset suggests acute lesions like stroke, while sequential development might indicate progressive conditions like tumors or degenerative diseases. Comprehensive neurological examination of patients presenting with combined motor and sensory facial symptoms requires careful assessment of all cranial nerves, as the involvement of multiple cranial nerves can help localize lesions and guide appropriate diagnostic imaging studies.
7. Burning Facial Sensations - Neuropathic Pain Syndromes

Burning facial sensations represent a distinct category of neuropathic pain that indicates damage or dysfunction within peripheral or central pain processing pathways, creating chronic discomfort that can be both physically and emotionally devastating for affected patients. This symptom typically manifests as constant or intermittent burning, searing, or hot sensations affecting specific facial regions, often accompanied by hypersensitivity to light touch or temperature changes that can make normal daily activities unbearable. Atypical facial pain, also known as atypical trigeminal neuralgia, produces deep, burning, or crushing pain that differs from the sharp, electric shock-like pain of classical trigeminal neuralgia, often affecting broader facial areas and lasting for longer periods. Post-herpetic neuralgia following herpes zoster infection of trigeminal nerve branches creates persistent burning pain that can continue for months or years after the acute infection resolves, representing one of the most challenging pain syndromes to treat effectively. Central pain syndromes resulting from brainstem strokes or other central nervous system lesions can produce burning facial sensations as part of broader pain syndromes affecting multiple body regions, reflecting damage to central pain processing pathways. The burning quality of facial pain often indicates small fiber neuropathy, where unmyelinated pain fibers are preferentially affected while larger myelinated fibers responsible for touch and vibration remain intact. Diabetic neuropathy can affect facial nerves, producing burning sensations that may be among the earliest signs of diabetic complications affecting the nervous system. Multiple sclerosis can cause burning facial pain through demyelination of trigeminal pathways, often fluctuating in intensity and potentially responding to disease-modifying treatments. The chronic nature of burning facial sensations can lead to secondary psychological effects including depression, anxiety, and social isolation, making comprehensive treatment approaches essential for optimal patient outcomes. Recognition of burning facial sensations as a neurological symptom rather than a psychological complaint is crucial for appropriate referral and treatment, as early intervention with neuropathic pain medications can significantly improve patient quality of life and prevent the development of chronic pain syndromes.
8. Facial Sensation Asymmetry - Comparative Neurological Assessment
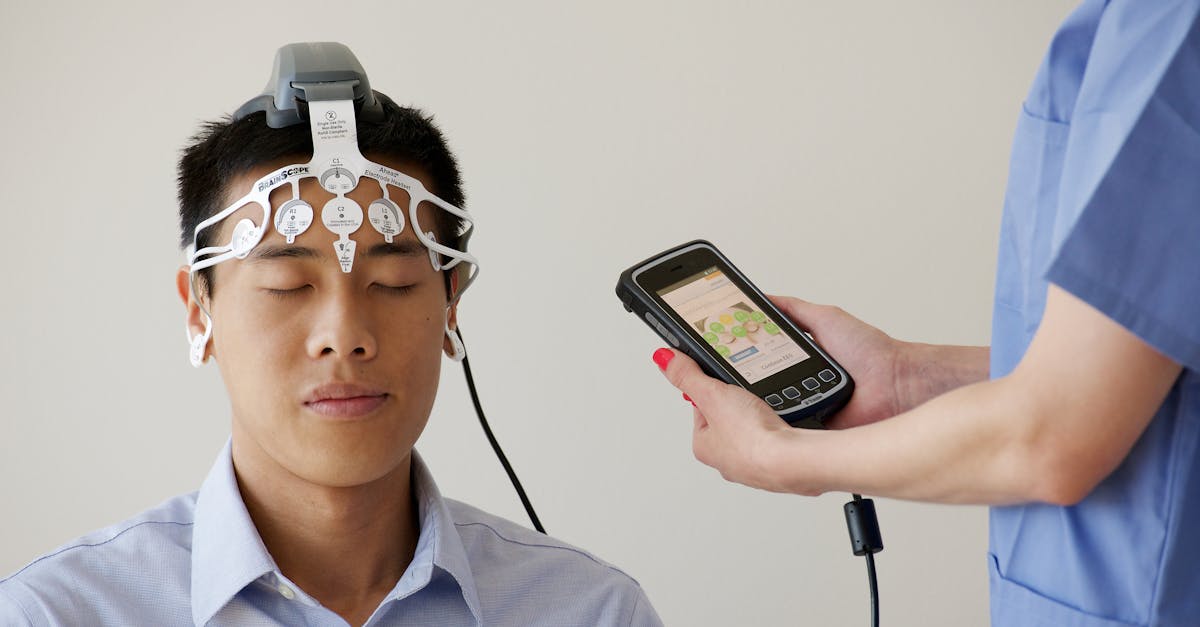
Facial sensation asymmetry, characterized by noticeable differences in sensory perception between the right and left sides of the face, provides neurologists with valuable lateralizing information that can help pinpoint the location and nature of underlying neurological conditions. This symptom requires careful comparative examination, as subtle differences in sensation between facial sides may be the only early indication of developing neurological disease. Patients may report that one side of their face feels "different," "heavy," or "strange" compared to the other side, descriptions that can be challenging to quantify but represent important subjective indicators of neurological dysfunction. Stroke affecting sensory pathways in the brainstem or thalamus commonly produces facial sensation asymmetry, often as part of broader sensory disturbances affecting the entire body on one side. The pattern of sensory loss can help distinguish between different stroke locations, as brainstem strokes may produce crossed sensory patterns while cortical strokes typically affect the face and body on the same side. Brain tumors growing near sensory pathways can produce gradually progressive sensation asymmetry that may be subtle initially but becomes more pronounced as the tumor enlarges and compresses surrounding neural tissue. Multiple sclerosis frequently causes asymmetric neurological symptoms due to the random distribution of demyelinating plaques throughout the central nervous system, making facial sensation asymmetry a common early finding in this condition. Peripheral nerve conditions such as trigeminal neuralgia or facial nerve disorders typically produce unilateral symptoms, creating obvious asymmetry that can be readily detected during clinical examination. The assessment of facial sensation asymmetry requires systematic testing of all trigeminal nerve divisions using standardized techniques including light touch, pinprick, temperature, and vibration testing to create a comprehensive sensory map. Quantitative sensory testing methods can detect subtle asymmetries that might be missed during routine clinical examination, providing objective measurements that can be tracked over time to monitor disease progression or treatment response. Documentation of facial sensation asymmetry patterns helps guide appropriate diagnostic imaging studies and can provide baseline measurements for monitoring neurological conditions over time.
9. Intermittent Facial Sensory Episodes - Paroxysmal Neurological Events

Intermittent facial sensory episodes, characterized by sudden onset and resolution of sensory symptoms that occur in distinct attacks or paroxysms, represent a unique category of neurological symptoms that can provide important diagnostic clues about underlying conditions affecting neural excitability and conduction. These episodes typically last from seconds to hours, creating dramatic changes in facial sensation that may include numbness, tingling, pain, or altered perception before returning to baseline function between attacks. Trigeminal neuralgia exemplifies this pattern with its characteristic brief, severe pain episodes triggered by light touch or movement, followed by complete pain resolution between attacks, creating a distinctive temporal pattern that aids in diagnosis. Multiple sclerosis commonly produces intermittent neurological symptoms due to the inflammatory nature of the disease, where episodes of demyelination can temporarily disrupt nerve conduction before remyelination allows function to recover partially or completely. Patients may experience facial numbness or tingling episodes lasting days to weeks during multiple sclerosis relapses, followed by periods of symptom improvement or resolution. Migraine with aura can produce transient facial sensory symptoms as part of the aura phenomenon, typically lasting 20-60 minutes and often accompanied by visual disturbances or other neurological symptoms that help distinguish it from other conditions. Transient ischemic attacks affecting brainstem regions can cause brief episodes of facial numbness or altered sensation that resolve completely within 24 hours, representing warning signs of potential future stroke risk. The episodic nature of these symptoms can make diagnosis challenging, as patients may present during asymptomatic periods when neurological examination appears normal. Detailed history-taking becomes crucial for documenting the temporal patterns, triggers, associated symptoms, and duration of sensory episodes to guide appropriate diagnostic workup. Video recording or patient diaries can help capture the characteristics of intermittent episodes that may not be witnessed during medical visits. Understanding the paroxysmal nature of certain neurological conditions helps clinicians recognize that normal examination findings between episodes do not rule out significant underlying pathology requiring further investigation and treatment.
10. Facial Hypersensitivity - Altered Pain Processing Mechanisms
