10 Coordination and Balance Symptom Types Associated With Inner Ear and Brain Conditions
The human body's ability to maintain balance and coordination represents one of nature's most sophisticated engineering marvels, involving an intricate network of sensory systems, neural pathways, and motor responses that work in perfect harmony. At the center of this complex system lies the vestibular apparatus within the inner ear, working in concert with visual inputs, proprioceptive feedback from muscles and joints, and the central nervous system's processing centers in the brain. When these systems become compromised due to inner ear disorders, neurological conditions, or brain injuries, the resulting symptoms can profoundly impact an individual's quality of life, ranging from mild unsteadiness to severe debilitating vertigo. Understanding the various manifestations of balance and coordination disorders is crucial for both healthcare professionals and patients, as these symptoms often serve as early warning signs of underlying pathological conditions. The following exploration delves into ten distinct symptom types that emerge when the delicate equilibrium between inner ear function and brain processing becomes disrupted, each presenting unique challenges and requiring specialized approaches to diagnosis and treatment.
1. Vertigo - The Spinning Sensation That Disrupts Reality
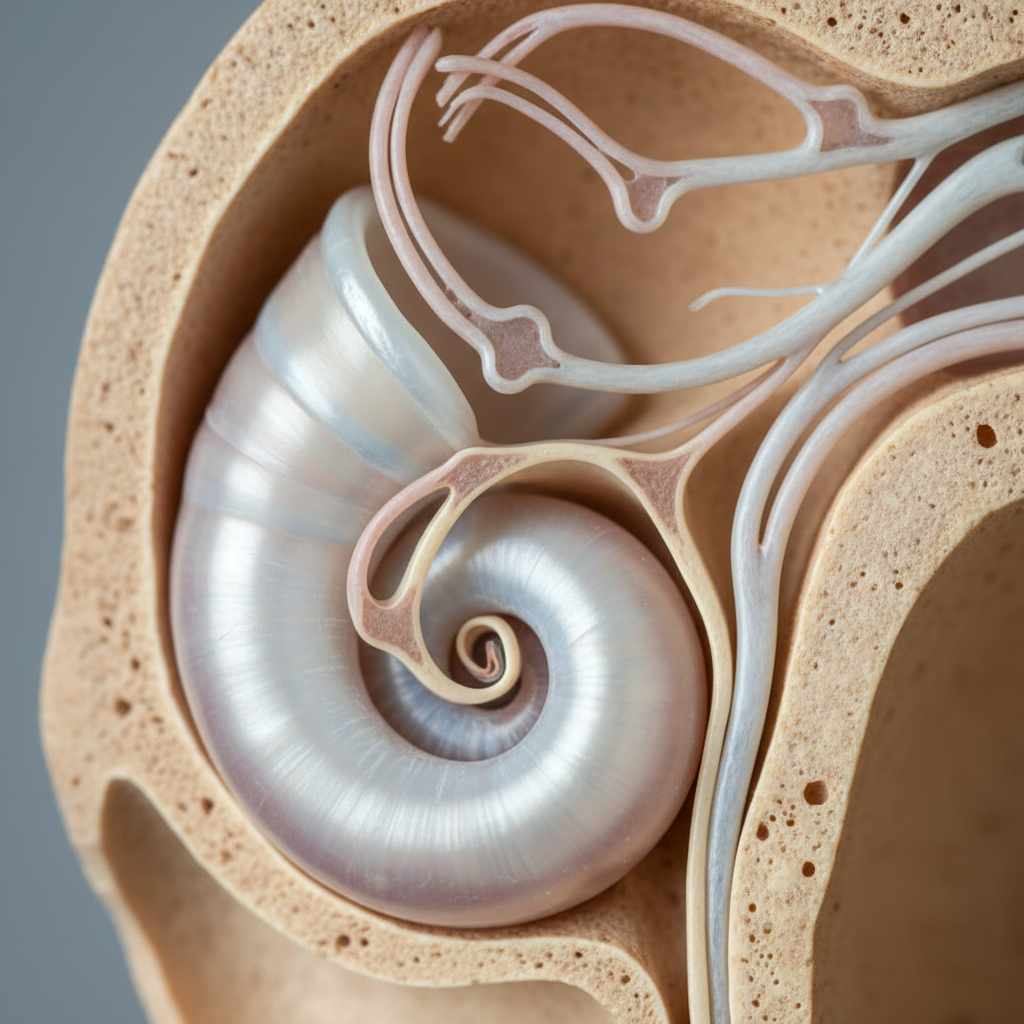
Vertigo stands as perhaps the most recognizable and distressing symptom associated with inner ear and brain disorders, characterized by the false sensation that either the individual or their surrounding environment is spinning, rotating, or moving when no actual movement is occurring. This phantom movement sensation stems from conflicting signals between the vestibular system, visual input, and proprioceptive feedback, creating a sensory mismatch that the brain struggles to reconcile. Peripheral vertigo, originating from inner ear dysfunction such as benign paroxysmal positional vertigo (BPPV), vestibular neuritis, or Meniere's disease, typically presents with intense spinning sensations accompanied by nausea, vomiting, and hearing changes. Central vertigo, arising from brainstem or cerebellar pathology, often manifests with additional neurological symptoms including diplopia, dysarthria, and limb ataxia. The duration and triggers of vertigo episodes provide crucial diagnostic clues, with BPPV causing brief episodes triggered by head movements, while vestibular migraine may produce prolonged episodes lasting hours to days. Treatment approaches vary significantly based on the underlying cause, ranging from canalith repositioning procedures for BPPV to vestibular rehabilitation therapy for chronic vestibular dysfunction, highlighting the importance of accurate diagnosis in managing this debilitating symptom.
2. Disequilibrium - The Persistent Feeling of Unsteadiness

Disequilibrium represents a chronic sensation of unsteadiness, imbalance, or feeling "off-balance" that persists even when sitting or lying down, distinguishing it from the episodic nature of vertigo. This symptom typically manifests as a constant awareness of instability, often described by patients as feeling like they're walking on a boat, standing on unstable ground, or experiencing a persistent "drunk-like" sensation. Unlike vertigo's spinning quality, disequilibrium creates a more generalized sense of spatial disorientation that can significantly impact daily activities and reduce confidence in movement. The underlying mechanisms often involve dysfunction in multiple balance systems simultaneously, including bilateral vestibular hypofunction, age-related changes in sensory processing, or central nervous system disorders affecting balance integration centers. Patients with disequilibrium frequently develop compensatory strategies such as widening their base of support, using visual cues more heavily, or avoiding challenging environments, which can lead to deconditioning and further balance deterioration over time. The psychological impact of chronic disequilibrium cannot be understated, as the persistent uncertainty about one's stability often leads to anxiety, depression, and social isolation. Comprehensive treatment approaches typically combine vestibular rehabilitation exercises, balance training, and sometimes pharmacological interventions to address both the physical symptoms and psychological consequences of this challenging condition.
3. Postural Instability - When Standing Becomes a Challenge

Postural instability manifests as difficulty maintaining an upright stance, particularly evident when standing still or making postural adjustments, and represents a complex interplay between vestibular, visual, and somatosensory systems. This symptom becomes particularly pronounced during challenging conditions such as standing on uneven surfaces, in darkness, or when visual and proprioceptive inputs are compromised. Patients often report feeling like they might fall backward, forward, or to one side, leading to compensatory behaviors such as holding onto furniture, walls, or other people for support. The Romberg test, where patients attempt to maintain balance with feet together and eyes closed, often reveals the extent of postural instability and helps differentiate between sensory and cerebellar causes. Age-related changes in vestibular function, combined with declining visual acuity and reduced proprioceptive sensitivity, contribute to increased postural instability in older adults, making them particularly vulnerable to falls and subsequent injuries. Neurological conditions such as Parkinson's disease, multiple sclerosis, and cerebellar disorders can exacerbate postural instability through different mechanisms, including altered muscle tone, delayed postural reflexes, and impaired central processing of balance information. Treatment strategies focus on improving postural control through specific exercises that challenge balance systems progressively, environmental modifications to reduce fall risk, and sometimes assistive devices to provide additional stability and confidence during daily activities.
4. Gait Ataxia - The Uncoordinated Walk

Gait ataxia presents as an uncoordinated, unsteady walking pattern characterized by irregular steps, variable stride length, and difficulty maintaining a straight path, often resembling the gait of someone who is intoxicated. This symptom reflects dysfunction in the complex neural networks responsible for coordinating movement, particularly involving the cerebellum, vestibular system, and sensory pathways that provide feedback about body position and movement. Patients with gait ataxia typically exhibit a wide-based stance, irregular timing of steps, and may veer to one side or appear to stagger while walking. The severity can range from subtle unsteadiness noticeable only during challenging tasks like tandem walking to severe impairment requiring assistive devices or making independent ambulation impossible. Cerebellar ataxia often produces a characteristic "drunken sailor" gait with lurching movements and difficulty with heel-to-toe walking, while sensory ataxia results from impaired proprioception and typically worsens in low-light conditions. Vestibular causes of gait ataxia may be accompanied by oscillopsia (visual jumping) and tend to improve with visual fixation or contact with stable surfaces. The functional impact of gait ataxia extends beyond mobility challenges, affecting independence, social participation, and overall quality of life. Rehabilitation approaches emphasize gait training, balance exercises, and adaptive strategies, while assistive devices such as canes or walkers may be necessary to ensure safety and maintain mobility independence.
5. Oscillopsia - When the Visual World Won't Stay Still

Oscillopsia represents the disturbing visual symptom where stationary objects appear to bounce, oscillate, or move rhythmically, creating a disorienting experience that significantly impacts visual function and spatial orientation. This phenomenon occurs when the vestibulo-ocular reflex (VOR), which normally stabilizes vision during head movements, becomes impaired or when pathological eye movements develop due to central nervous system dysfunction. Patients often describe the sensation as watching the world through a handheld camera with a shaky operator, making reading, driving, and other visually demanding tasks extremely challenging or impossible. The symptom can be constant or intermittent, triggered by head movements or occurring spontaneously, depending on the underlying cause. Bilateral vestibular hypofunction commonly produces oscillopsia during head movements as the VOR fails to compensate for head motion, while central nervous system disorders may cause spontaneous oscillopsia due to abnormal eye movements such as nystagmus. The functional consequences of oscillopsia are profound, often leading to reading difficulties, problems with depth perception, and challenges with activities requiring visual-motor coordination. Some patients develop compensatory strategies such as holding their head very still or using their hands to stabilize their head during visual tasks. Treatment approaches may include vestibular rehabilitation to improve gaze stability, prism glasses to reduce visual motion sensitivity, and in severe cases, surgical interventions to address underlying vestibular or ocular motor dysfunction.
6. Motion Sensitivity - When Movement Becomes the Enemy

Motion sensitivity, also known as visual motion sensitivity or space and motion discomfort, manifests as an abnormal response to visual motion stimuli or moving environments, often triggering symptoms of dizziness, nausea, and disorientation. This symptom commonly develops following vestibular disorders, head injuries, or migraine conditions, representing a maladaptive response where the visual system becomes hypersensitive to motion cues. Patients typically report feeling overwhelmed in visually complex environments such as grocery stores with busy patterns, crowded spaces with moving people, or while watching movies with rapid scene changes. The underlying mechanism involves altered processing of visual-vestibular interactions, where conflicting sensory information creates an exaggerated stress response and symptom production. Everyday activities that involve visual motion, such as riding in vehicles, using escalators, or even watching television, can become significant triggers for dizziness and discomfort. The condition often creates a cycle of avoidance behaviors, where patients limit their exposure to challenging environments, leading to increased sensitivity and reduced tolerance over time. Social and occupational functioning can be severely impacted, as many modern environments contain the visual motion stimuli that trigger symptoms. Treatment typically involves gradual exposure therapy through vestibular rehabilitation, where patients are systematically exposed to increasing levels of visual motion in a controlled manner. Optokinetic exercises, virtual reality therapy, and environmental modifications can help desensitize the visual system and restore normal motion tolerance, allowing patients to regain confidence in challenging visual environments.
7. Spatial Disorientation - Losing Your Place in Space
Spatial disorientation encompasses the disturbing experience of losing one's sense of position, direction, or relationship to the surrounding environment, creating confusion about spatial relationships and navigation abilities. This complex symptom involves dysfunction in the integration of vestibular, visual, and proprioceptive inputs that normally provide continuous information about body position and movement in three-dimensional space. Patients often describe feeling "lost" even in familiar environments, having difficulty judging distances, or experiencing confusion about which way is up or down, particularly in low-light conditions or when visual cues are limited. The phenomenon can manifest as difficulty navigating through doorways, misjudging the height of steps, or feeling disoriented when transitioning between different environments such as moving from indoors to outdoors. Spatial disorientation frequently accompanies vestibular disorders, traumatic brain injuries, and certain neurological conditions that affect spatial processing centers in the brain. The symptom can be particularly pronounced during head movements or when changing positions, as the disrupted spatial reference system fails to update accurately with body movement. Cognitive factors also play a role, as the brain's attempt to make sense of conflicting spatial information can lead to increased mental fatigue and concentration difficulties. Treatment approaches focus on spatial orientation training, environmental awareness exercises, and gradual exposure to challenging spatial environments. Occupational therapy interventions may include navigation training, spatial memory exercises, and the use of external cues or landmarks to improve spatial orientation and confidence in movement.
8. Lightheadedness - The Floating Sensation

Lightheadedness presents as a sensation of feeling faint, woozy, or as if one might pass out, often described as a "floating" or "swimming" feeling in the head that differs distinctly from the spinning sensation of vertigo. This symptom can arise from various causes including vestibular dysfunction, cardiovascular issues, medication effects, or anxiety disorders, making accurate diagnosis crucial for appropriate treatment. Unlike vertigo's rotational quality, lightheadedness typically involves a sense of detachment or unreality, where patients feel disconnected from their surroundings or experience a "foggy" mental state. The sensation may be accompanied by visual changes such as tunnel vision, seeing spots, or temporary dimming of vision, particularly when standing up quickly or during periods of stress. Vestibular causes of lightheadedness often involve dysfunction in the otolith organs, which detect linear acceleration and head position relative to gravity, leading to altered perception of spatial orientation and stability. The symptom can be triggered by specific head positions, rapid movements, or changes in environmental conditions such as temperature or lighting. Orthostatic hypotension, where blood pressure drops upon standing, can mimic or coexist with vestibular-related lightheadedness, requiring careful evaluation to distinguish between cardiovascular and vestibular causes. Anxiety and panic disorders frequently manifest with lightheadedness, creating a complex interplay between psychological and physiological factors that can perpetuate and worsen symptoms. Treatment approaches must address the underlying cause, whether through vestibular rehabilitation for inner ear dysfunction, cardiovascular management for blood pressure issues, or anxiety treatment for psychological components.
9. Coordination Difficulties - When Precise Movements Become Impossible

Coordination difficulties manifest as impaired ability to perform smooth, precise, and purposeful movements, affecting both gross motor skills like walking and fine motor tasks such as writing or buttoning clothes. These symptoms reflect dysfunction in the complex neural networks responsible for motor planning, execution, and refinement, particularly involving the cerebellum, basal ganglia, and their connections to motor and sensory cortices. Patients often report clumsiness, difficulty with tasks requiring bilateral coordination, and problems with timing and sequencing of movements. Simple activities like reaching for objects, pouring liquids, or using utensils become challenging and may result in spills, drops, or inaccurate movements. The cerebellum plays a crucial role in motor learning and adaptation, so cerebellar dysfunction often produces characteristic signs including dysmetria (overshooting or undershooting targets), dysdiadochokinesia (difficulty with rapid alternating movements), and intention tremor that worsens as the hand approaches a target. Vestibular contributions to coordination involve the vestibulo-spinal reflexes that help maintain posture and coordinate head and body movements during locomotion and reaching tasks. When these systems are disrupted, patients may experience difficulty coordinating eye and head movements, problems with dynamic balance during multi-tasking, and reduced ability to perform activities that require integration of visual and motor systems. The functional impact extends to occupational performance, recreational activities, and independence in daily living tasks. Rehabilitation focuses on task-specific training, progressive motor skill development, and compensatory strategies to improve coordination and restore functional abilities.
10. Head Movement Intolerance - When Turning Your Head Triggers Symptoms

Head movement intolerance represents a debilitating symptom where normal head movements trigger intense dizziness, vertigo, nausea, or other vestibular symptoms, severely limiting daily activities and quality of life. This condition often develops following vestibular disorders, head trauma, or viral infections affecting the inner ear, where the vestibular system becomes hypersensitive to motion stimuli. Patients typically report that simple head movements such as looking up, turning to check blind spots while driving, or rolling over in bed can trigger severe symptoms lasting minutes to hours. The underlying mechanism involves dysfunction in the vestibulo-ocular reflex and vestibulo-spinal reflexes, which normally allow for smooth coordination between head movements and eye/body responses. When these reflexes are impaired, head movements create conflicting sensory signals that the brain interprets as motion sickness or spatial disorientation. The condition often leads to adaptive behaviors such as moving the entire body instead of just the head, using slow deliberate movements, or avoiding certain positions altogether. This movement restriction can result in neck stiffness, muscle tension, and secondary musculoskeletal problems from altered movement patterns. The psychological impact is significant, as patients often develop kinesiophobia (fear of movement) and may become increasingly sedentary to avoid triggering symptoms. Social and occupational functioning suffers as activities requiring head mobility become impossible or severely limited. Treatment typically involves graduated vestibular rehabilitation exercises designed to slowly desensitize the vestibular system to head movements, starting with small, slow movements and progressively increasing speed and range of motion as tolerance improves.
11. Integrating Understanding for Comprehensive Care
The ten coordination and balance symptom types explored in this comprehensive examination represent the diverse and complex manifestations that emerge when the intricate systems governing human equilibrium become disrupted. From the spinning sensations of vertigo to the persistent unsteadiness of disequilibrium, each symptom type reflects specific patterns of dysfunction within the vestibular, visual, proprioceptive, and central nervous systems that work together to maintain our sense of balance and spatial orientation. Understanding these distinct presentations is crucial for healthcare providers, as accurate symptom recognition forms the foundation for appropriate diagnostic testing, treatment planning, and patient education. The interconnected nature of these symptoms often means that patients may experience multiple manifestations simultaneously, requiring comprehensive assessment approaches that consider the full spectrum of balance and coordination disorders. Modern treatment strategies emphasize the importance of individualized care plans that address not only the physical symptoms but also the psychological and social impacts of these conditions. Vestibular rehabilitation therapy has emerged as a cornerstone of treatment, offering evidence-based interventions that can significantly improve symptoms and functional outcomes for many patients. However, the complexity of balance disorders necessitates multidisciplinary approaches involving otolaryngologists, neurologists, physical therapists, occupational therapists, and other specialists working collaboratively to optimize patient care. As our understanding of vestibular and balance disorders continues to evolve through ongoing research, new diagnostic tools and treatment modalities offer hope for improved outcomes and quality of life for individuals affected by these challenging conditions. The key to successful management lies in early recognition, accurate diagnosis, and prompt initiation of appropriate therapeutic interventions tailored to each patient's specific symptom profile and functional needs.