10 Abdominal Pain Quadrant Locations and What Each Area Typically Suggests
Understanding abdominal pain requires a systematic approach that begins with anatomical mapping, as the location of discomfort often provides the first crucial clue in determining its underlying cause. Medical professionals divide the abdomen into distinct quadrants and regions, creating a diagnostic framework that has proven invaluable for centuries. The traditional four-quadrant system divides the abdomen into right upper quadrant (RUQ), left upper quadrant (LUQ), right lower quadrant (RLQ), and left lower quadrant (LLQ), while more detailed approaches include additional central regions such as the epigastric, umbilical, and suprapubic areas. Each quadrant houses specific organs and structures, making the location of pain a powerful diagnostic tool that can help differentiate between conditions ranging from simple digestive issues to life-threatening emergencies. This systematic approach to abdominal pain assessment not only guides healthcare providers toward appropriate diagnostic tests and treatments but also helps patients better communicate their symptoms. By understanding what each area typically suggests, both medical professionals and patients can work together more effectively to identify potential causes and determine the urgency of medical intervention required.
1. Right Upper Quadrant - The Liver and Gallbladder Territory
The right upper quadrant encompasses some of the body's most metabolically active organs, primarily the liver, gallbladder, and portions of the pancreas, making pain in this region particularly significant from a diagnostic standpoint. Gallbladder-related conditions represent the most common cause of RUQ pain, with cholecystitis (gallbladder inflammation) and cholelithiasis (gallstones) leading the list of potential diagnoses. Patients experiencing gallbladder issues typically describe a sharp, cramping pain that may radiate to the right shoulder blade or between the shoulder blades, often triggered by fatty meals and accompanied by nausea and vomiting. Hepatitis, whether viral, alcoholic, or drug-induced, can also manifest as RUQ pain, usually presenting as a dull, constant ache accompanied by jaundice, fatigue, and changes in urine color. Additionally, this quadrant can be affected by conditions such as liver abscesses, hepatic tumors, or even referred pain from pneumonia affecting the right lower lung lobe. The proximity of the duodenum and head of the pancreas to this region means that peptic ulcers and pancreatitis can also present with RUQ discomfort, making careful clinical evaluation essential for accurate diagnosis.
2. Left Upper Quadrant - Spleen, Stomach, and Pancreatic Concerns
The left upper quadrant houses critical digestive and immune system organs, including the spleen, stomach, tail of the pancreas, and splenic flexure of the colon, each capable of producing distinct pain patterns when affected by disease or injury. Splenic conditions, though less common than other abdominal pathologies, can present with LUQ pain that may radiate to the left shoulder, particularly in cases of splenic rupture following trauma or splenic infarction in patients with blood disorders. Gastric conditions frequently manifest in this region, with peptic ulcers, gastritis, and gastric outlet obstruction producing pain that typically correlates with meal timing and may be accompanied by nausea, vomiting, or changes in appetite. Pancreatitis affecting the body and tail of the pancreas often presents with severe LUQ pain that radiates straight through to the back, creating a characteristic "boring" sensation that patients find difficult to relieve with position changes. The pain from pancreatitis is often described as constant and severe, frequently accompanied by nausea, vomiting, and fever. Other conditions that may present with LUQ pain include splenic flexure syndrome, where gas trapped in the colon creates significant discomfort, and referred pain from cardiac conditions, making this quadrant particularly challenging for differential diagnosis.
3. Right Lower Quadrant - Appendix and Reproductive Organ Considerations
The right lower quadrant is perhaps most famous for housing the appendix, making appendicitis the most well-known cause of RLQ pain, though numerous other conditions can affect this anatomically complex region. Classic appendicitis typically begins with periumbilical pain that migrates to the RLQ over several hours, localizing at McBurney's point, approximately one-third of the distance from the anterior superior iliac spine to the umbilicus. However, appendicitis presentations can vary significantly, particularly in elderly patients, pregnant women, or those with atypical appendix positions, making clinical suspicion and imaging studies crucial for accurate diagnosis. In women of reproductive age, RLQ pain may indicate ovarian pathology such as ovarian cysts, ovarian torsion, or ectopic pregnancy, conditions that require immediate evaluation due to their potential for serious complications. Inflammatory bowel diseases, particularly Crohn's disease affecting the terminal ileum, commonly present with RLQ pain accompanied by diarrhea, weight loss, and systemic symptoms. Other considerations include cecal diverticulitis, which can mimic appendicitis, kidney stones affecting the right ureter, and hernias involving the inguinal region. The complexity of potential diagnoses in this quadrant necessitates careful history-taking, physical examination, and often advanced imaging to differentiate between these various conditions.
4. Left Lower Quadrant - Diverticular Disease and Gynecological Factors

The left lower quadrant commonly presents diagnostic challenges due to the convergence of gastrointestinal, urological, and gynecological structures, with diverticular disease representing one of the most frequent causes of pain in this region, particularly in older adults. Sigmoid diverticulitis, often called "left-sided appendicitis," typically presents with cramping LLQ pain accompanied by fever, changes in bowel habits, and localized tenderness, though the presentation can range from mild discomfort to severe complications including perforation or abscess formation. The sigmoid colon's location in this quadrant also makes it susceptible to other inflammatory conditions, including inflammatory bowel disease, particularly ulcerative colitis, which may present with bloody diarrhea and cramping pain. In women, LLQ pain frequently stems from gynecological causes, including ovarian cysts, mittelschmerz (ovulation pain), endometriosis, or pelvic inflammatory disease, each requiring specific diagnostic approaches and treatments. Urological conditions such as kidney stones affecting the left ureter or urinary tract infections can also manifest as LLQ pain, often accompanied by urinary symptoms such as dysuria, frequency, or hematuria. The interconnected nature of pelvic anatomy means that conditions affecting one organ system may present with pain that seems to originate from another, making comprehensive evaluation essential for accurate diagnosis and appropriate treatment planning.
5. Epigastric Region - The Upper Central Abdominal Hub
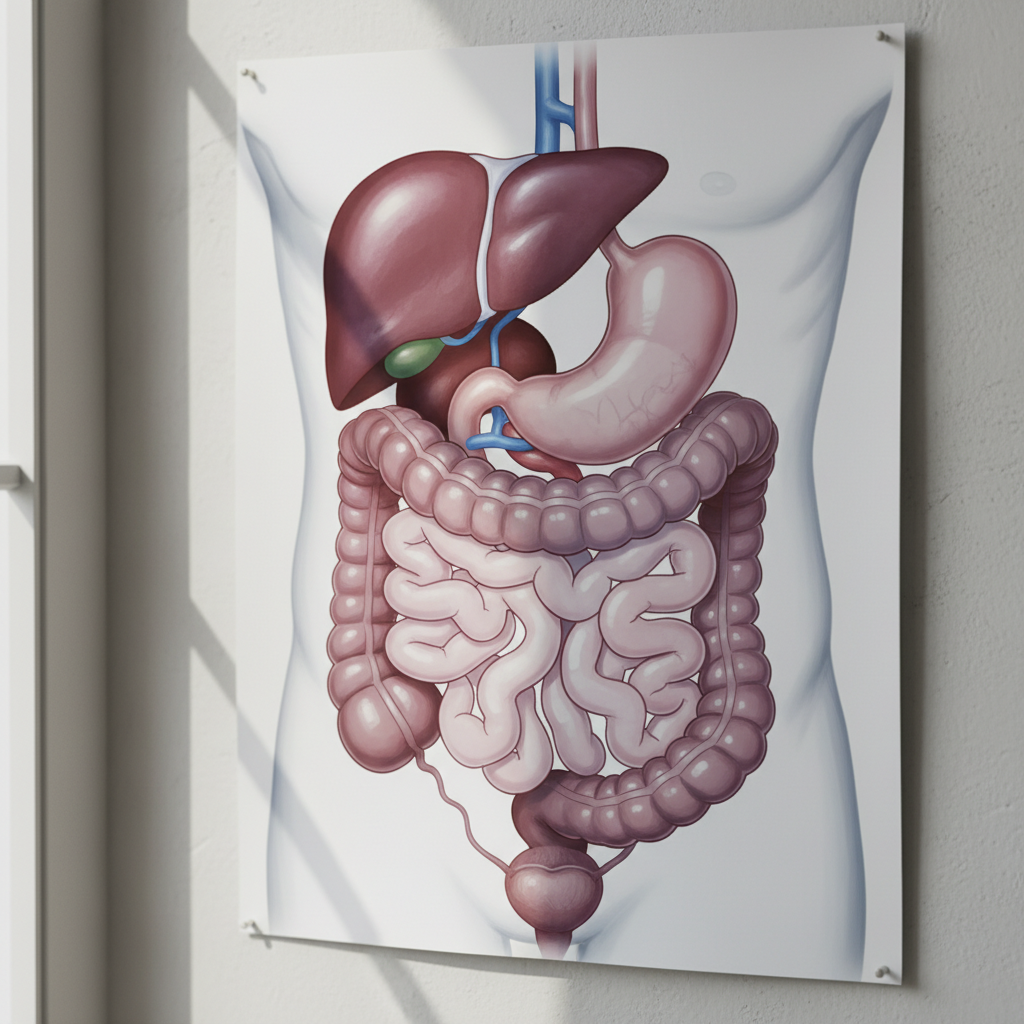
The epigastric region, located in the upper central portion of the abdomen just below the xiphoid process, serves as a crucial diagnostic area where pain often indicates conditions affecting the stomach, duodenum, pancreas, or even the heart. Peptic ulcer disease represents one of the most common causes of epigastric pain, with gastric ulcers typically producing pain that worsens with eating, while duodenal ulcers often improve with food intake and worsen several hours after meals. The character of ulcer pain is usually described as burning or gnawing, and may be accompanied by nausea, bloating, or early satiety. Acute pancreatitis frequently presents with severe epigastric pain that radiates to the back, creating an intense, constant discomfort that patients often describe as the worst pain they have ever experienced. This pain is typically accompanied by nausea, vomiting, and systemic signs of inflammation including fever and elevated inflammatory markers. Gastroesophageal reflux disease (GERD) can also manifest as epigastric discomfort, particularly when associated with gastritis or esophagitis, often accompanied by heartburn and regurgitation. Importantly, cardiac conditions, particularly inferior wall myocardial infarctions, can present with epigastric pain rather than classic chest pain, making this region critical for ruling out life-threatening cardiovascular events, especially in patients with cardiac risk factors.
6. Periumbilical Area - Early Warning Signs and Visceral Pain Patterns
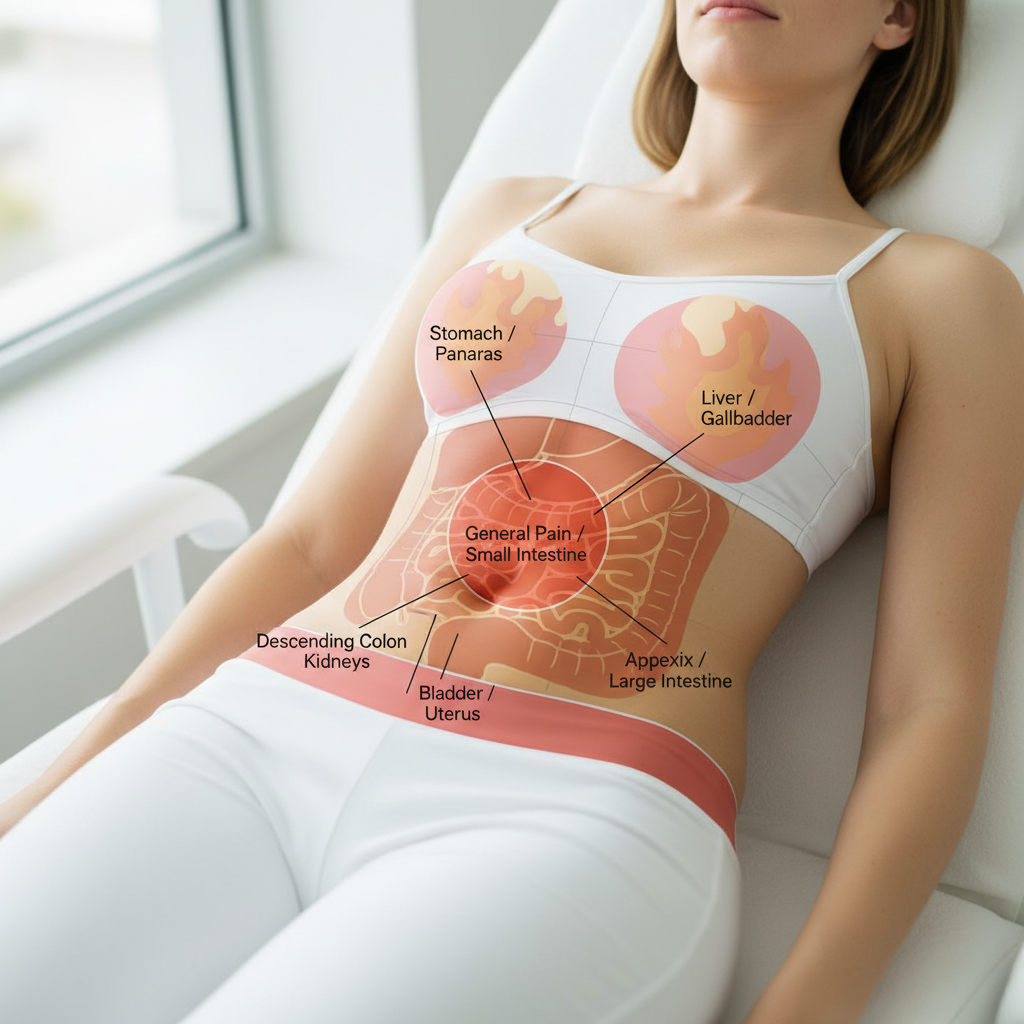
The periumbilical region, centered around the navel, represents a unique area where visceral pain from various abdominal organs often first manifests before localizing to more specific quadrants, making it an important early indicator of developing pathology. This phenomenon occurs because visceral pain fibers from many abdominal organs converge at the T10 dermatome level, corresponding to the umbilical area, before the pain becomes more localized as inflammation spreads to involve the parietal peritoneum. Early appendicitis classically begins with vague periumbilical pain that gradually migrates to the right lower quadrant as the inflammatory process progresses, though this classic presentation occurs in only about 50% of cases. Small bowel obstruction frequently presents with cramping periumbilical pain that comes in waves, corresponding to peristaltic waves attempting to overcome the obstruction, often accompanied by nausea, vomiting, and abdominal distension. Early pancreatitis may also begin with periumbilical discomfort before localizing to the epigastric region, while mesenteric ischemia can present with severe periumbilical pain that seems disproportionate to physical findings. Umbilical hernias, though often asymptomatic, can become incarcerated or strangulated, leading to localized periumbilical pain accompanied by a visible or palpable mass. The nonspecific nature of periumbilical pain requires careful clinical evaluation and often serial examinations to determine the underlying cause and appropriate treatment approach.
7. Suprapubic Region - Urological and Reproductive System Indicators
The suprapubic region, located in the lower central abdomen above the pubic symphysis, primarily reflects pathology involving the urinary bladder, reproductive organs, and lower gastrointestinal tract, making it a critical area for evaluating genitourinary complaints. Bladder conditions represent the most common cause of suprapubic pain, with urinary tract infections producing a characteristic burning sensation accompanied by urinary frequency, urgency, and dysuria. Bladder outlet obstruction, commonly caused by benign prostatic hyperplasia in older men, can lead to suprapubic discomfort associated with difficulty initiating urination, weak urinary stream, and incomplete bladder emptying. Interstitial cystitis, a chronic bladder condition more common in women, presents with persistent suprapubic pain that worsens with bladder filling and improves with voiding, often accompanied by urinary frequency and urgency without evidence of infection. In women, gynecological conditions such as uterine fibroids, endometriosis, or pelvic inflammatory disease can manifest as suprapubic pain, particularly during menstruation or sexual activity. Pregnancy-related conditions, including threatened abortion or ectopic pregnancy, may also present with suprapubic discomfort accompanied by vaginal bleeding or other reproductive symptoms. Gastrointestinal causes of suprapubic pain include sigmoid diverticulitis, inflammatory bowel disease affecting the rectosigmoid region, and occasionally, large bowel obstruction, making comprehensive evaluation essential for accurate diagnosis.
8. Right Flank and Costovertebral Angle - Renal and Retroperitoneal Pathology
The right flank region, extending from the costovertebral angle to the iliac crest, represents a critical diagnostic area for identifying renal, ureteral, and retroperitoneal pathology, with pain in this location often indicating conditions requiring urgent medical attention. Nephrolithiasis, or kidney stones, represents the most common cause of flank pain, typically presenting as severe, colicky pain that radiates from the flank to the groin as stones progress down the ureter. The pain from kidney stones is often described as excruciating and comes in waves, frequently accompanied by nausea, vomiting, and hematuria, with patients unable to find a comfortable position. Pyelonephritis, or kidney infection, presents with flank pain that is typically constant rather than colicky, accompanied by fever, chills, and urinary symptoms such as dysuria and frequency. Costovertebral angle tenderness is a classic finding in pyelonephritis and helps differentiate it from lower urinary tract infections. Renal infarction, though less common, can present with sudden onset of severe flank pain accompanied by hematuria and systemic signs of tissue death. Retroperitoneal bleeding, whether from trauma, anticoagulation complications, or ruptured abdominal aortic aneurysm, can manifest as flank pain accompanied by signs of hemodynamic instability. Other considerations include renal cell carcinoma, which may present with the classic triad of flank pain, hematuria, and palpable mass, though this complete presentation occurs in only a minority of cases.
9. Left Flank and Costovertebral Angle - Mirror Image Renal Considerations

The left flank region mirrors many of the diagnostic considerations of the right flank but includes some unique anatomical relationships that can influence pain presentation and diagnostic approaches. Similar to the right side, left-sided nephrolithiasis represents a common cause of left flank pain, with identical presentation patterns including severe colicky pain radiating to the groin, nausea, vomiting, and hematuria. However, the left kidney's slightly different anatomical position and the longer left ureter can sometimes lead to variations in pain patterns and stone passage times. Left-sided pyelonephritis presents similarly to right-sided infection but may be associated with different bacterial organisms or predisposing factors, particularly in patients with anatomical abnormalities or chronic kidney disease. The proximity of the left kidney to the spleen creates potential for diagnostic confusion, particularly in cases where splenic pathology may refer pain to the left flank region. Retroperitoneal pathology affecting the left side includes similar considerations to the right, including bleeding, infection, or malignancy, but the left retroperitoneum's relationship to the descending colon and sigmoid colon can create additional diagnostic complexity. Musculoskeletal causes of left flank pain, including rib fractures, muscle strains, or vertebral pathology, must also be considered, particularly in patients with recent trauma or chronic pain conditions. The evaluation of left flank pain requires the same systematic approach as right-sided pain, with careful attention to urinalysis, imaging studies, and clinical presentation to differentiate between various potential causes.
10. Diffuse Abdominal Pain - Systemic and Widespread Pathological Processes

Diffuse abdominal pain, affecting multiple quadrants or the entire abdomen, often indicates systemic pathological processes or conditions involving the peritoneum, requiring a different diagnostic approach than localized pain patterns. Peritonitis, whether from perforation of a hollow organ, postoperative complications, or spontaneous bacterial peritonitis in patients with ascites, typically presents with severe, diffuse abdominal pain accompanied by guarding, rigidity, and systemic signs of infection including fever and elevated white blood cell count. The pain from peritonitis is characteristically constant and worsens with movement, leading patients to lie still with knees drawn up to minimize discomfort. Gastroenteritis, whether viral, bacterial, or parasitic, commonly presents with diffuse cramping abdominal pain accompanied by nausea, vomiting, and diarrhea, though the pain is typically less severe than that seen with peritonitis. Bowel obstruction, particularly when involving multiple segments or when associated with ischemia, can present with diffuse abdominal pain that comes in waves, accompanied by vomiting, abdominal distension, and absence of bowel movements. Mesenteric ischemia, whether acute or chronic, often presents with severe diffuse abdominal pain that seems disproportionate to physical findings, particularly in elderly patients with cardiovascular risk factors. Other systemic conditions that may present with diffuse abdominal pain include diabetic ketoacidosis, uremia, inflammatory conditions such as systemic lupus erythematosus, and certain medications or toxins, making comprehensive evaluation essential for accurate diagnosis.
## Section 12: Clinical Integration and Diagnostic Approach - Synthesizing Location with Additional Clinical Factors
The integration of abdominal pain location with other clinical factors represents the cornerstone of effective diagnostic reasoning, as pain location alone, while highly informative, must be considered within the broader context of patient presentation, physical examination findings, and diagnostic test results. The timing and character of pain onset provide crucial diagnostic clues, with sudden, severe pain suggesting conditions such as perforation, vascular catastrophe, or torsion, while gradual onset pain may indicate inflammatory or infectious processes. Associated symptoms significantly enhance diagnostic accuracy, with fever suggesting infection or inflammation, nausea and vomiting indicating possible obstruction or visceral pathology, and urinary symptoms pointing toward genitourinary causes. Physical examination findings, including the presence or absence of guarding, rebound tenderness, masses, or organomegaly, help confirm or refute diagnostic hypotheses generated by pain location and associated symptoms. Patient demographics and medical history play crucial roles in diagnostic probability, with age, gender, surgical history, medication use, and comorbid conditions all influencing the likelihood of various diagnoses. Laboratory studies and imaging modalities should be selected based on the clinical presentation and suspected diagnoses, with basic studies such as complete blood count, comprehensive metabolic panel, and urinalysis providing initial screening, while more specific tests such as lipase, liver function tests, or imaging studies help confirm suspected diagnoses. The evolution of pain over time, response to initial treatments, and development of new symptoms all provide additional diagnostic information that may require reassessment and modification of the initial diagnostic approach, emphasizing the dynamic nature of clinical evaluation in patients with abdominal pain.