8 Gum Appearances Associated with Systemic Health Conditions
# 8 Gum Appearances Associated with Systemic Health Conditions: A Comprehensive Guide to Oral-Systemic Health Connections
The human mouth serves as far more than just the gateway for nutrition and communication—it functions as a remarkable diagnostic window that can reveal critical insights into our overall systemic health. The gingival tissues, commonly known as gums, are particularly telling indicators of underlying health conditions, often manifesting visible changes that precede or accompany serious medical disorders. Modern medical research has established compelling connections between periodontal health and systemic diseases, with gum appearance serving as an early warning system for conditions ranging from cardiovascular disease to autoimmune disorders. The rich vascular supply of gingival tissues, combined with their constant exposure to oral bacteria and inflammatory mediators, makes them uniquely positioned to reflect systemic inflammatory processes and metabolic disturbances. Healthcare professionals increasingly recognize that certain gum appearances—including color changes, texture alterations, bleeding patterns, and structural modifications—can provide valuable diagnostic clues that warrant further medical investigation. This comprehensive exploration examines eight distinct gum appearances that have been scientifically linked to systemic health conditions, offering both healthcare providers and patients crucial knowledge for early detection and intervention strategies that can significantly impact long-term health outcomes.
1. Pale or White Gums - Indicators of Anemia and Blood Disorders
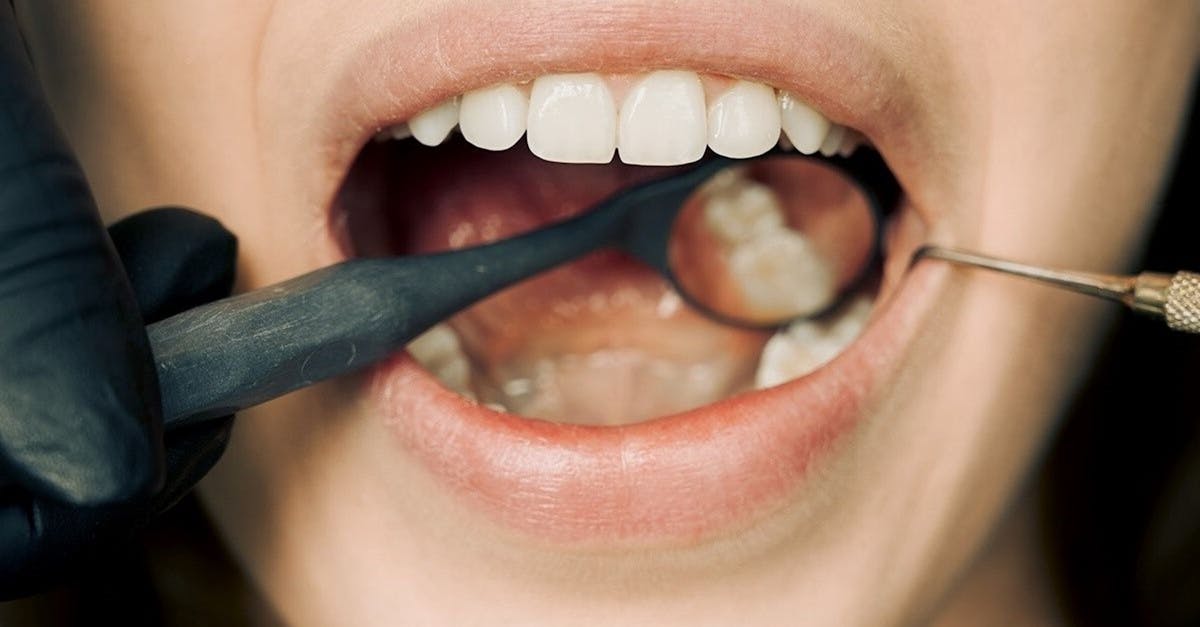
Pale or unusually white gums represent one of the most clinically significant oral manifestations of systemic health problems, particularly those affecting blood composition and circulation. Healthy gums typically display a coral pink coloration due to adequate blood flow and normal hemoglobin levels, but when gums appear noticeably pale, white, or grayish, this often indicates underlying anemia or other hematological disorders. Iron-deficiency anemia, the most common form of anemia worldwide, frequently presents with pale gingival tissues as one of its earliest visible signs, occurring when reduced hemoglobin levels diminish the characteristic pink coloration of well-vascularized tissues. Additionally, other forms of anemia, including vitamin B12 deficiency anemia, folate deficiency anemia, and chronic disease-related anemia, can similarly manifest through gum pallor. Beyond anemia, pale gums may indicate more serious blood disorders such as leukemia, where abnormal white blood cell production can affect normal tissue coloration and health. Certain autoimmune conditions, including systemic lupus erythematosus, can also cause gum pallor through their effects on circulation and tissue inflammation. The clinical significance of pale gums extends beyond simple color changes, as this appearance often accompanies other symptoms such as fatigue, weakness, shortness of breath, and cold intolerance, creating a constellation of findings that can guide healthcare providers toward appropriate diagnostic testing and treatment interventions.
2. Bright Red or Deep Red Gums - Signs of Diabetes and Inflammatory Conditions
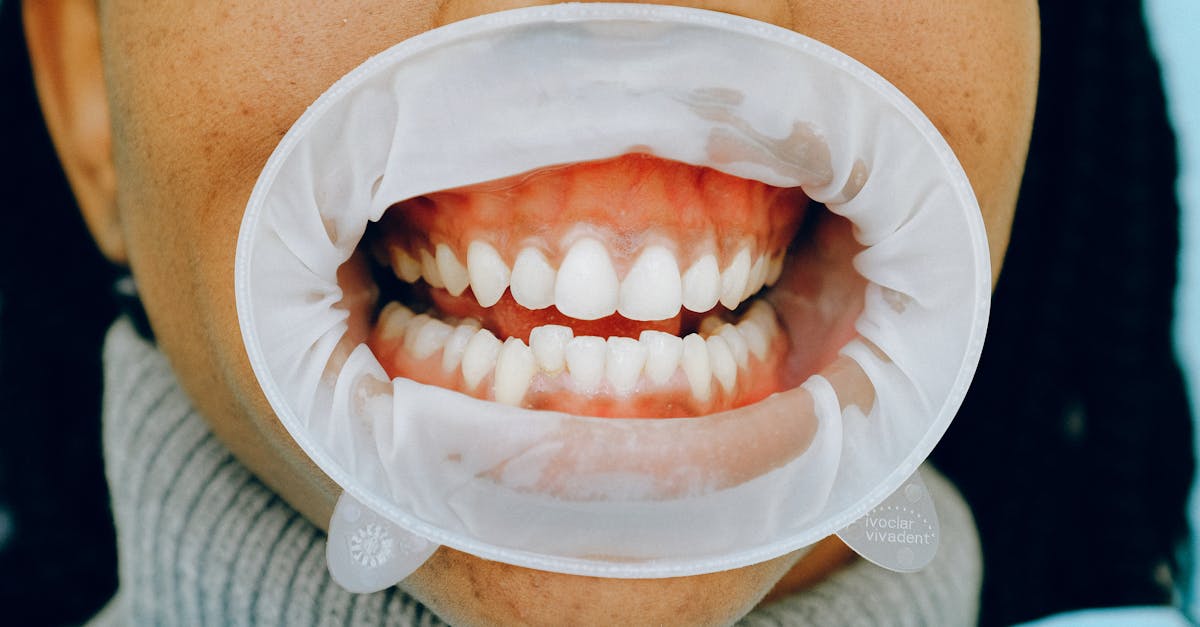
Intensely red or deep crimson gums serve as important indicators of systemic inflammatory processes and metabolic disorders, with diabetes mellitus representing the most significant associated condition. The characteristic bright red appearance results from increased blood flow, vascular engorgement, and inflammatory mediator release that occurs when systemic conditions affect periodontal tissues. Diabetes, particularly when poorly controlled, creates a complex interplay between elevated blood glucose levels, compromised immune function, and enhanced inflammatory responses that manifest prominently in gingival tissues. The chronic hyperglycemia associated with diabetes leads to advanced glycation end products formation, which triggers inflammatory cascades and compromises the body's ability to fight periodontal infections effectively. This results in gums that appear not only bright red but also swollen, tender, and prone to bleeding even with minimal provocation. Beyond diabetes, other systemic inflammatory conditions such as rheumatoid arthritis, inflammatory bowel disease, and certain cardiovascular conditions can produce similar gingival redness through their effects on systemic inflammation and immune function. The intensity and persistence of gum redness often correlate with the severity of the underlying systemic condition, making regular oral examinations valuable for monitoring disease progression and treatment effectiveness. Research has demonstrated that individuals with bright red, inflamed gums have significantly higher risks of cardiovascular events, stroke, and diabetic complications, emphasizing the critical importance of addressing both oral and systemic health simultaneously.
3. Purple or Blue-Tinged Gums - Cardiovascular and Circulatory Implications
Purple, blue, or cyanotic-appearing gums represent serious indicators of cardiovascular compromise and circulatory dysfunction that demand immediate medical attention and comprehensive evaluation. This distinctive coloration, known as gingival cyanosis, occurs when oxygen-depleted blood accumulates in periodontal tissues due to inadequate circulation or impaired oxygen exchange. Congestive heart failure represents one of the most common systemic conditions associated with purple-tinged gums, as the heart's reduced pumping capacity leads to poor circulation and venous congestion that becomes visible in highly vascularized oral tissues. Chronic obstructive pulmonary disease (COPD) and other respiratory conditions can similarly cause gum discoloration through their effects on blood oxygenation and circulation. Additionally, certain congenital heart defects, pulmonary hypertension, and severe anemia can manifest through purple or blue gum coloration. The appearance of purple gums often accompanies other cardiovascular symptoms such as shortness of breath, chest pain, fatigue, and peripheral edema, creating a clinical picture that requires urgent medical evaluation. Interestingly, some medications used to treat cardiovascular conditions, particularly certain calcium channel blockers and anticoagulants, can also contribute to gum color changes through their effects on blood flow and tissue metabolism. The recognition of purple or blue-tinged gums as a potential sign of serious cardiovascular compromise has led to increased collaboration between dental and medical professionals, emphasizing the importance of comprehensive health assessments that consider oral manifestations of systemic disease.
4. Swollen and Spongy Gums - Hormonal Imbalances and Endocrine Disorders
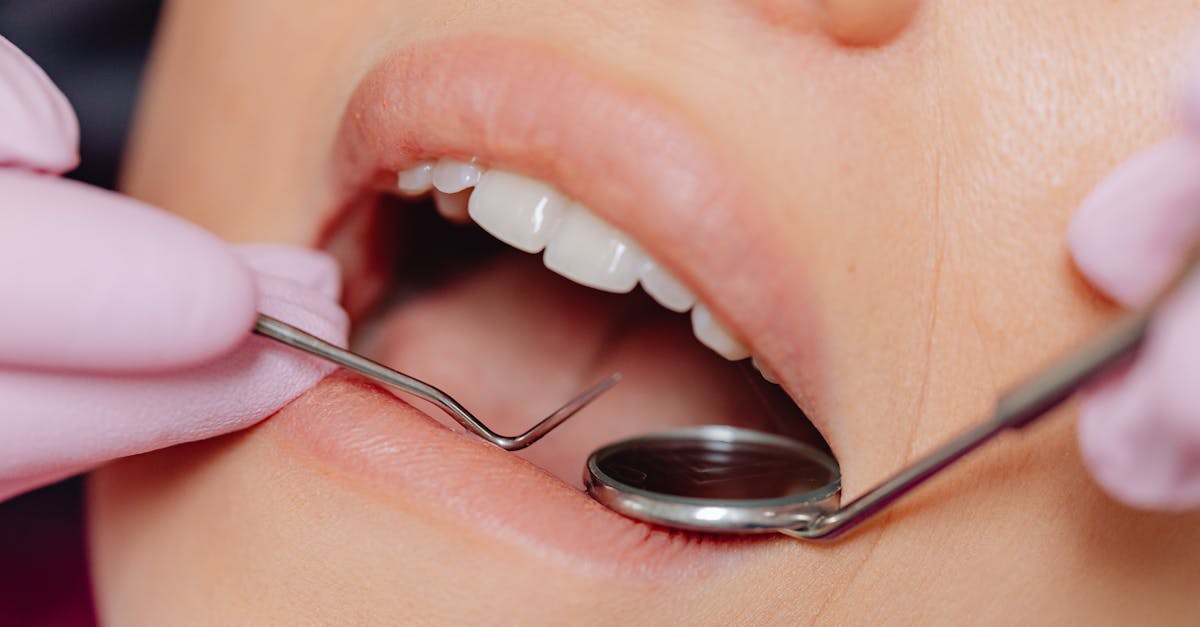
Chronically swollen, spongy, or puffy gums often indicate underlying hormonal imbalances and endocrine disorders that affect tissue metabolism, fluid retention, and inflammatory responses throughout the body. Pregnancy represents the most well-recognized condition associated with gum swelling, where elevated estrogen and progesterone levels increase vascular permeability and enhance inflammatory responses to bacterial plaque, resulting in the characteristic "pregnancy gingivitis" that affects up to 75% of pregnant women. However, gum swelling extends far beyond pregnancy-related changes, serving as an important indicator of various endocrine disorders including thyroid dysfunction, diabetes mellitus, and hormonal fluctuations associated with menopause and puberty. Hypothyroidism, in particular, can cause significant gum swelling due to mucopolysaccharide accumulation in tissues, reduced metabolic rate, and impaired immune function that allows bacterial overgrowth and inflammation. Cushing's syndrome and other adrenal disorders can similarly affect gum appearance through their effects on cortisol levels, immune function, and tissue healing capacity. The spongy texture of swollen gums results from increased fluid accumulation, collagen breakdown, and inflammatory cell infiltration that occurs when hormonal imbalances disrupt normal tissue homeostasis. Additionally, certain medications used to treat endocrine disorders, including some diabetes medications and hormone replacement therapies, can contribute to gum swelling through their effects on fluid retention and tissue metabolism. Recognition of chronically swollen gums as a potential sign of endocrine dysfunction has important implications for early disease detection and management, as addressing underlying hormonal imbalances often leads to significant improvements in both oral and systemic health outcomes.
5. Receding Gums with Exposed Roots - Osteoporosis and Bone Metabolism Disorders
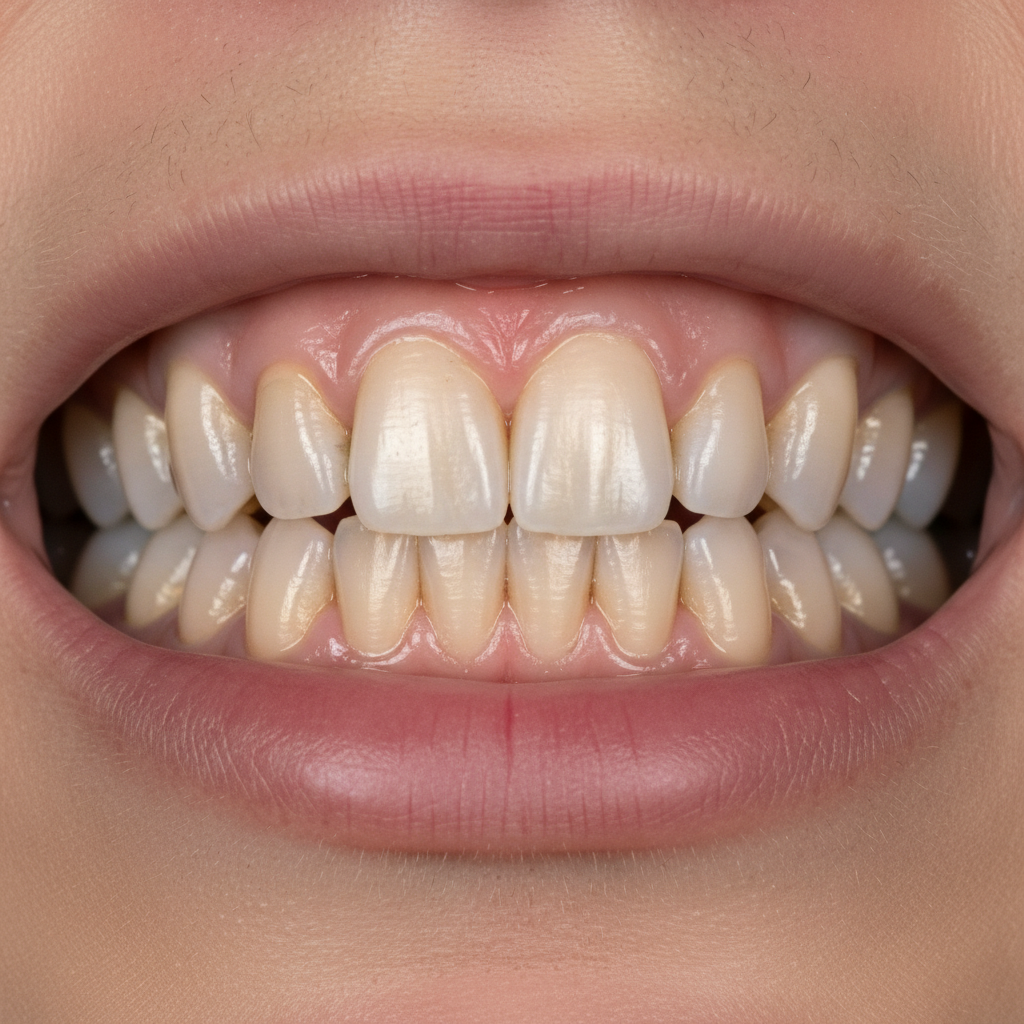
Gum recession accompanied by visible tooth root exposure represents a significant oral manifestation of systemic bone metabolism disorders, with osteoporosis serving as the most clinically relevant associated condition. The progressive loss of gingival tissue and underlying alveolar bone that characterizes gum recession often reflects broader skeletal changes occurring throughout the body, particularly in postmenopausal women and elderly individuals at risk for osteoporotic fractures. Research has established strong correlations between oral bone loss, as evidenced by gum recession and tooth mobility, and systemic bone density measurements, suggesting that periodontal changes may serve as early indicators of osteoporosis development. The biological mechanisms linking gum recession to osteoporosis involve shared risk factors including estrogen deficiency, calcium and vitamin D insufficiency, inflammatory cytokine activity, and genetic predisposition to bone resorption. Additionally, certain medications used to treat osteoporosis, particularly bisphosphonates, can paradoxically affect oral tissues and complicate dental treatment through their effects on bone remodeling and healing processes. Beyond osteoporosis, other conditions affecting bone metabolism such as hyperparathyroidism, chronic kidney disease, and malabsorption syndromes can similarly manifest through gum recession and alveolar bone loss. The clinical significance of gum recession extends beyond cosmetic concerns, as exposed tooth roots increase susceptibility to decay, sensitivity, and tooth loss, while also indicating increased fracture risk and need for bone density evaluation. Early recognition of gum recession patterns associated with systemic bone disorders enables healthcare providers to implement comprehensive treatment strategies that address both oral health and fracture prevention, potentially preventing serious complications and improving long-term quality of life.
6. Bleeding Gums and Easy Bruising - Blood Clotting Disorders and Liver Disease
Spontaneous gum bleeding, excessive bleeding during routine oral care, and easy gingival bruising represent important oral manifestations of systemic blood clotting disorders and liver dysfunction that require careful medical evaluation and management. While mild gum bleeding commonly results from local periodontal inflammation, persistent or excessive bleeding often indicates underlying coagulopathy, platelet dysfunction, or liver disease that impairs normal hemostatic mechanisms. Liver disease, including hepatitis, cirrhosis, and fatty liver disease, frequently manifests through gum bleeding due to reduced production of clotting factors, decreased platelet function, and portal hypertension that affects oral circulation. The liver's central role in producing essential clotting proteins means that even mild hepatic dysfunction can result in prolonged bleeding times and easy bruising that becomes apparent during routine dental procedures or oral hygiene activities. Additionally, blood disorders such as thrombocytopenia, hemophilia, von Willebrand disease, and leukemia can present with characteristic gum bleeding patterns that may precede other systemic symptoms. Certain medications, particularly anticoagulants like warfarin and newer direct oral anticoagulants, as well as antiplatelet agents such as aspirin and clopidogrel, can significantly increase gum bleeding tendency and complicate dental treatment. The clinical assessment of gum bleeding patterns, including frequency, severity, and response to local treatment, provides valuable information about systemic hemostatic function and can guide appropriate laboratory testing and medical referrals. Recognition of abnormal gum bleeding as a potential indicator of serious systemic disease has led to improved coordination between dental and medical care providers, emphasizing the importance of comprehensive bleeding assessments that consider both local and systemic factors.
7. Dry Mouth with Gum Changes - Autoimmune Conditions and Medication Effects
Chronic dry mouth accompanied by distinctive gum changes represents a significant oral manifestation of autoimmune conditions and medication-related side effects that can profoundly impact both oral and systemic health outcomes. Sjögren's syndrome, the most prominent autoimmune condition associated with oral dryness, affects salivary and lacrimal glands through immune-mediated destruction, resulting in severely reduced saliva production and characteristic gum changes including increased redness, sensitivity, and susceptibility to infection. The absence of adequate saliva flow eliminates the mouth's natural cleansing and antimicrobial mechanisms, leading to rapid bacterial overgrowth, increased plaque accumulation, and gum inflammation that appears more severe and persistent than typical gingivitis. Additionally, other autoimmune conditions such as rheumatoid arthritis, systemic lupus erythematosus, and scleroderma can cause secondary Sjögren's syndrome or directly affect salivary gland function through inflammatory processes and medication effects. The extensive list of medications that can cause dry mouth includes antidepressants, antihistamines, blood pressure medications, diuretics, and many others commonly prescribed for chronic conditions, making medication-induced xerostomia a widespread problem affecting millions of individuals. Gum changes associated with chronic dry mouth include increased erythema, tissue friability, altered texture, and enhanced susceptibility to fungal infections such as oral candidiasis. The clinical significance of dry mouth-related gum changes extends beyond oral discomfort, as reduced saliva flow significantly increases risks of dental decay, gum disease progression, and oral infections that can have serious systemic consequences, particularly in immunocompromised individuals. Management of dry mouth and associated gum changes requires comprehensive approaches that address underlying autoimmune conditions, optimize medication regimens when possible, and implement targeted oral care strategies to maintain gum health and prevent complications.
8. Yellow or Discolored Gums - Liver Dysfunction and Metabolic Disorders
Yellow or abnormally discolored gums serve as important visual indicators of liver dysfunction and various metabolic disorders that affect bilirubin metabolism and tissue pigmentation throughout the body. Jaundice, the clinical condition characterized by elevated bilirubin levels, often manifests initially in highly vascularized tissues such as the gums before becoming apparent in the sclera or skin, making oral examination a valuable early detection tool for hepatic disorders. Liver diseases including hepatitis, cirrhosis, biliary obstruction, and drug-induced hepatotoxicity can all produce characteristic yellow discoloration of gingival tissues through their effects on bilirubin processing and elimination. The intensity of gum yellowing often correlates with the severity of liver dysfunction and bilirubin elevation, providing healthcare providers with a readily observable indicator of disease progression or treatment response. Beyond liver-related causes, certain metabolic disorders such as Gilbert's syndrome, Crigler-Najjar syndrome, and hemolytic anemias can produce similar gum discoloration through their effects on bilirubin metabolism and red blood cell breakdown. Additionally, some medications, particularly those metabolized by the liver or those that can cause hepatotoxicity, may contribute to gum discoloration through their effects on liver function and bilirubin levels. Smoking and tobacco use can also cause gum discoloration, though this typically presents as brown or black pigmentation rather than the yellow coloration associated with systemic disease. The recognition of yellow gum discoloration as a potential sign of serious liver or metabolic dysfunction has important implications for early disease detection and intervention, as prompt identification and treatment of underlying conditions can prevent progression to more serious complications such as liver failure or severe metabolic derangement.
9. Integrating Oral Health Assessment into Comprehensive Healthcare
The recognition of gum appearances as valuable indicators of systemic health conditions represents a paradigm shift in healthcare delivery that emphasizes the interconnected nature of oral and overall health. The eight distinct gum manifestations explored in this comprehensive analysis—pale coloration indicating anemia, bright redness suggesting diabetes and inflammation, purple discoloration reflecting cardiovascular compromise, swelling associated with hormonal imbalances, recession linked to bone disorders, bleeding patterns indicating clotting dysfunction, dryness-related changes suggesting autoimmune conditions, and yellow discoloration pointing to liver dysfunction—collectively demonstrate the mouth's remarkable capacity to reveal systemic disease processes. This understanding has profound implications for healthcare providers across all specialties, emphasizing the importance of routine oral examinations as part of comprehensive health assessments and the need for enhanced collaboration between dental and medical professionals. The integration of oral health evaluation into routine medical care can facilitate early detection of serious systemic conditions, potentially improving treatment outcomes and reducing healthcare costs through preventive interventions. Furthermore, the bidirectional relationship between oral and systemic health means that addressing gum problems can have positive effects on overall health outcomes, while managing systemic conditions often leads to improvements in oral health status. As healthcare continues to evolve toward more integrated, patient-centered approaches, the recognition of oral-systemic health connections will likely play an increasingly important role in disease prevention, early detection, and comprehensive treatment strategies that optimize both oral and overall health outcomes for patients across all age groups and health conditions.