8 Facial Asymmetries That Warrant Medical Attention
Facial symmetry has long been considered a hallmark of beauty and health across cultures, but beyond aesthetic considerations, significant facial asymmetries can signal underlying medical conditions that require professional evaluation. While minor asymmetries are completely normal and present in virtually every human face, pronounced or sudden changes in facial symmetry may indicate neurological disorders, developmental abnormalities, infections, or structural problems that demand immediate medical attention. The human face serves as a complex map of our internal health, with muscles, nerves, bones, and soft tissues working in intricate harmony to create our expressions and facilitate essential functions like eating, speaking, and breathing. When this delicate balance is disrupted, the resulting asymmetries can range from cosmetic concerns to life-threatening conditions. Understanding which facial asymmetries warrant medical evaluation is crucial for early detection and treatment of potentially serious underlying conditions. This comprehensive exploration examines eight specific types of facial asymmetries that should prompt immediate consultation with healthcare professionals, providing readers with the knowledge necessary to recognize when facial changes require urgent medical intervention rather than simple acceptance as natural variation.
1. Sudden Onset Facial Drooping - The Bell's Palsy Emergency

Sudden onset facial drooping represents one of the most urgent facial asymmetries requiring immediate medical attention, as it can indicate either Bell's palsy or the far more serious condition of stroke. Bell's palsy affects approximately 40,000 Americans annually and presents as rapid weakness or paralysis of facial muscles on one side, typically developing over 48 hours and reaching peak severity within 72 hours. The condition manifests as an inability to close the eye completely, drooping of the mouth corner, loss of the nasolabial fold, and difficulty with facial expressions on the affected side. While Bell's palsy is generally benign and often resolves within three to six months, the initial presentation is virtually indistinguishable from stroke-related facial paralysis, making immediate medical evaluation critical. Healthcare providers use specific diagnostic criteria, including the ability to wrinkle the forehead (preserved in Bell's palsy but lost in stroke), to differentiate between these conditions. Early treatment with corticosteroids within 72 hours of onset can significantly improve outcomes in Bell's palsy cases, while stroke requires emergency intervention to minimize permanent damage. The psychological impact of sudden facial asymmetry cannot be understated, as patients often experience significant distress, social anxiety, and concerns about permanent disfigurement, making prompt diagnosis and appropriate treatment essential for both physical and emotional well-being.
2. Progressive Jaw Deviation - Temporomandibular Joint Disorders and Beyond
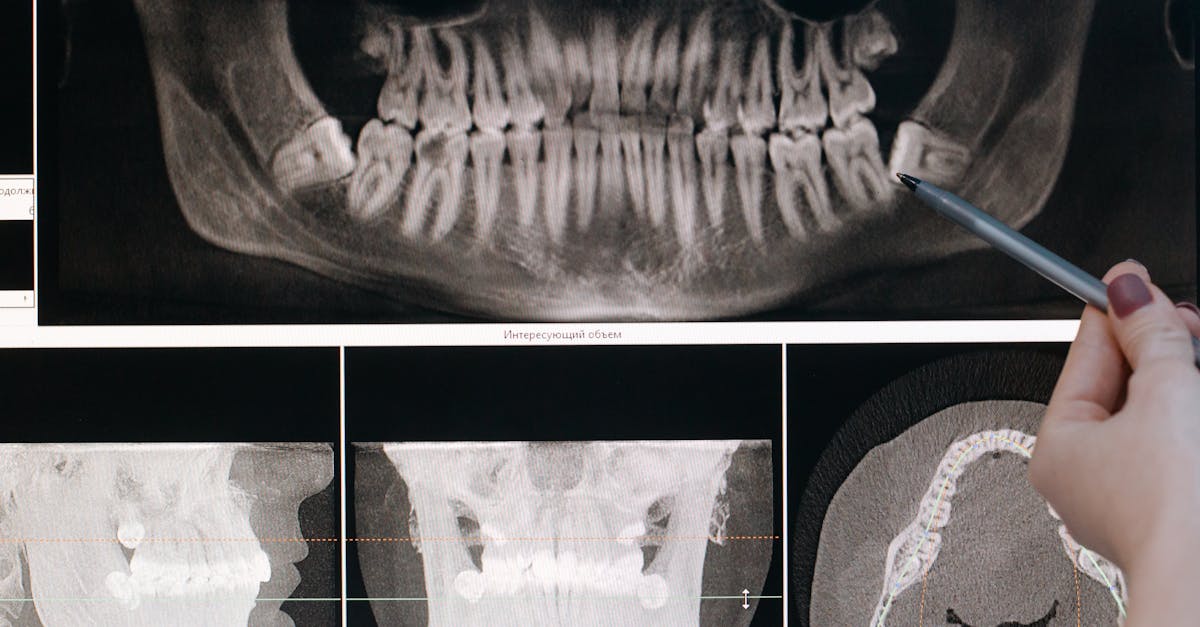
Progressive jaw deviation presents as a gradual shift in the jaw's position during opening, closing, or at rest, creating noticeable facial asymmetry that can indicate serious underlying conditions affecting the temporomandibular joint (TMJ) or surrounding structures. This asymmetry often begins subtly but becomes increasingly pronounced over time, potentially signaling TMJ disorders, arthritis, muscle imbalances, or even tumors affecting the jaw joint or surrounding tissues. Patients typically notice that their jaw shifts to one side when opening their mouth, their bite feels different, or their facial appearance becomes increasingly lopsided over weeks or months. The condition can be accompanied by clicking or popping sounds, jaw pain, headaches, and difficulty chewing or speaking properly. In severe cases, the asymmetry can affect dental occlusion, leading to uneven tooth wear, dental problems, and further complications. Medical evaluation is crucial because progressive jaw deviation can result from inflammatory conditions like rheumatoid arthritis affecting the TMJ, degenerative joint disease, muscle disorders, or space-occupying lesions such as tumors or cysts. Early intervention through proper diagnosis can prevent permanent joint damage and may involve treatments ranging from physical therapy and oral appliances to surgical intervention. The multidisciplinary approach often requires collaboration between oral and maxillofacial surgeons, rheumatologists, and dental specialists to address both the underlying cause and the resulting functional and aesthetic concerns.
3. Unilateral Facial Swelling - Infections and Inflammatory Conditions
Unilateral facial swelling that creates pronounced asymmetry demands immediate medical attention as it can indicate serious infections, inflammatory conditions, or allergic reactions that may compromise breathing or spread to vital structures. This type of asymmetry typically develops rapidly, often within hours or days, and may be accompanied by pain, warmth, redness, or systemic symptoms such as fever and malaise. Common causes include dental abscesses that can spread to facial spaces, salivary gland infections like parotitis or submandibular gland inflammation, cellulitis affecting facial tissues, or severe allergic reactions causing angioedema. Dental infections are particularly concerning as they can rapidly progress to life-threatening conditions such as Ludwig's angina, where swelling extends to the floor of the mouth and can compromise the airway. Salivary gland swelling may indicate bacterial or viral infections, autoimmune conditions like Sjögren's syndrome, or obstructive disorders caused by stones or tumors. The location and characteristics of the swelling provide important diagnostic clues: swelling in front of the ear suggests parotid gland involvement, while swelling under the jaw indicates submandibular gland issues. Prompt medical evaluation is essential because these conditions often require immediate antibiotic therapy, surgical drainage, or emergency airway management. Healthcare providers must quickly assess whether the swelling poses an immediate threat to vital functions and determine the appropriate level of intervention, which may range from outpatient antibiotic treatment to emergency hospitalization for intravenous medications and close monitoring.
4. Eyelid Asymmetry and Ptosis - Neurological and Muscular Concerns
Eyelid asymmetry, particularly when involving ptosis (drooping of the upper eyelid), represents a significant facial asymmetry that can indicate serious neurological or muscular disorders requiring immediate medical evaluation. Ptosis can be congenital or acquired, with acquired cases often signaling underlying pathology affecting the muscles that elevate the eyelid or the nerves that control them. The condition creates noticeable facial asymmetry and can range from mild drooping that affects appearance to severe cases that impair vision and daily functioning. Neurogenic ptosis may result from third cranial nerve palsy, Horner's syndrome, or myasthenia gravis, each requiring specific diagnostic approaches and treatments. Myasthenia gravis, an autoimmune condition affecting neuromuscular transmission, often presents initially with ptosis and can progress to involve other muscles, potentially affecting breathing and swallowing. Horner's syndrome, characterized by ptosis, miosis (small pupil), and anhidrosis (lack of sweating), can indicate serious underlying conditions such as lung tumors, carotid artery dissection, or brainstem lesions. Mechanical ptosis may result from tumors, inflammation, or trauma affecting the eyelid structures. The evaluation of eyelid asymmetry requires careful assessment of pupil size and reactivity, eye movements, and associated symptoms. Diagnostic testing may include blood tests for myasthenia gravis antibodies, imaging studies to evaluate for masses or vascular abnormalities, and specialized neurological testing. Early recognition and treatment are crucial because some underlying causes, such as carotid dissection or intracranial masses, can be life-threatening if not promptly addressed.
5. Nasal Deviation and Asymmetry - Structural and Functional Implications
Significant nasal deviation creating facial asymmetry can indicate structural abnormalities, trauma, or developmental disorders that require medical evaluation, particularly when accompanied by functional impairments such as breathing difficulties or recurrent sinus infections. While minor nasal asymmetries are common and often cosmetic in nature, pronounced deviations may signal septal deviations, nasal fractures, or underlying craniofacial abnormalities that can significantly impact quality of life. The nasal septum, which divides the nasal cavity into two chambers, can become severely deviated due to trauma, congenital abnormalities, or developmental issues, creating visible external asymmetry and internal obstruction. Patients with significant septal deviation often experience chronic nasal congestion, mouth breathing, snoring, sleep disturbances, and recurrent sinus infections that can lead to more serious complications if left untreated. External nasal deviation may also result from nasal bone fractures, cartilage damage, or soft tissue injuries that alter the nose's structural integrity and appearance. In some cases, nasal asymmetry can be associated with broader craniofacial syndromes or developmental abnormalities that require comprehensive evaluation and multidisciplinary treatment. The functional implications of nasal deviation extend beyond breathing difficulties to include effects on sleep quality, exercise tolerance, and overall well-being. Medical evaluation typically involves detailed examination of both external nasal anatomy and internal nasal structures using endoscopy, along with imaging studies when indicated. Treatment options range from conservative management with nasal decongestants and saline irrigation to surgical interventions such as septoplasty or rhinoplasty, depending on the severity of symptoms and the underlying cause of the deviation.
6. Asymmetric Muscle Weakness - Neuromuscular Disorders

Asymmetric facial muscle weakness that creates noticeable facial asymmetry can indicate serious neuromuscular disorders, stroke, or other neurological conditions that require immediate medical evaluation and intervention. This type of asymmetry typically manifests as weakness or paralysis affecting one side of the face, resulting in an inability to smile symmetrically, raise eyebrows evenly, or close the eyes completely on the affected side. The pattern and distribution of weakness provide important diagnostic clues about the underlying pathology. Upper motor neuron lesions, such as those caused by stroke, typically spare the forehead muscles due to bilateral innervation, while lower motor neuron lesions affect the entire side of the face uniformly. Conditions such as myasthenia gravis can cause fluctuating weakness that worsens with activity and improves with rest, often beginning with eyelid drooping and potentially progressing to involve other facial muscles. Muscular dystrophies and other inherited neuromuscular disorders may present with gradually progressive facial weakness that can be asymmetric in early stages. Inflammatory conditions such as polymyositis or dermatomyositis can also cause facial muscle weakness, often accompanied by other systemic symptoms. The evaluation of asymmetric facial weakness requires careful neurological examination, assessment of muscle strength and reflexes, and often specialized testing such as electromyography, nerve conduction studies, or blood tests for specific antibodies. Imaging studies of the brain may be necessary to rule out stroke or other central nervous system pathology. Early diagnosis and treatment are crucial because some causes of facial weakness, such as stroke or myasthenia gravis, can be life-threatening if not promptly addressed, while others may benefit from early intervention to prevent progression and optimize functional outcomes.
7. Orbital and Periorbital Asymmetry - Thyroid and Inflammatory Conditions

Orbital and periorbital asymmetry involving swelling, protrusion, or changes in the appearance of the eyes and surrounding tissues can indicate serious underlying conditions such as thyroid eye disease, orbital infections, or space-occupying lesions that require urgent medical evaluation. Thyroid eye disease, also known as Graves' ophthalmopathy, commonly presents with asymmetric orbital involvement, causing proptosis (eye protrusion), eyelid retraction, diplopia (double vision), and periorbital swelling that creates significant facial asymmetry. This condition can occur in patients with hyperthyroidism, hypothyroidism, or even those with normal thyroid function, and can be sight-threatening if severe. The inflammatory process affects the extraocular muscles and orbital tissues, leading to fibrosis and permanent changes if not treated promptly. Orbital cellulitis, a serious infection of the tissues surrounding the eye, can cause rapid onset of periorbital swelling, proptosis, and vision changes, potentially leading to blindness or intracranial complications if not treated emergently. Preseptal cellulitis, while less serious, can also cause significant asymmetric swelling and may progress to orbital involvement. Other causes of orbital asymmetry include tumors, vascular malformations, or inflammatory conditions such as orbital pseudotumor. The evaluation requires careful assessment of visual acuity, eye movements, pupil responses, and intraocular pressure, along with imaging studies such as CT or MRI to evaluate orbital structures. Laboratory testing may include thyroid function tests and inflammatory markers. Treatment varies depending on the underlying cause but may include corticosteroids for inflammatory conditions, antibiotics for infections, or surgical intervention for tumors or severe cases of thyroid eye disease. The multidisciplinary approach often involves collaboration between ophthalmologists, endocrinologists, and oculoplastic surgeons to optimize both functional and cosmetic outcomes.
8. Dental and Occlusal Asymmetries - Orthodontic and Surgical Considerations
Significant dental and occlusal asymmetries that affect facial appearance and function can indicate underlying skeletal abnormalities, developmental disorders, or pathological conditions that may require comprehensive medical and dental evaluation. These asymmetries often manifest as uneven tooth alignment, midline discrepancies, or differences in jaw size and position that create noticeable facial imbalance. While minor dental irregularities are common and primarily cosmetic concerns, severe asymmetries can indicate underlying issues such as hemifacial microsomia, condylar hyperplasia, ankylosis of the temporomandibular joint, or other craniofacial abnormalities that require multidisciplinary treatment. Hemifacial microsomia, the second most common facial birth defect after cleft lip and palate, causes underdevelopment of one side of the face, affecting the jaw, ear, and surrounding structures, resulting in significant facial asymmetry and functional impairments. Condylar hyperplasia involves excessive growth of one mandibular condyle, causing progressive facial asymmetry, dental midline shifts, and occlusal problems that can continue into adulthood if not properly managed. Dental asymmetries can also result from early loss of primary teeth, trauma, tumors, or infections that affect normal dental development and eruption patterns. The functional implications extend beyond appearance to include difficulties with chewing, speaking, and maintaining proper oral hygiene, potentially leading to dental decay, gum disease, and temporomandibular joint problems. Evaluation requires comprehensive dental and orthodontic examination, detailed medical history, and often specialized imaging such as cephalometric radiographs, CT scans, or 3D imaging to assess both dental and skeletal relationships. Treatment planning may involve orthodontic therapy, oral surgery, or combined orthodontic-surgical approaches to address both functional and aesthetic concerns. Early intervention is often crucial for optimal outcomes, particularly in growing patients where growth modification techniques may be employed to guide facial development.
9. The Importance of Early Recognition and Professional Evaluation

The recognition of significant facial asymmetries that warrant medical attention represents a critical aspect of healthcare awareness that can lead to early diagnosis and treatment of potentially serious underlying conditions. Throughout this comprehensive examination of eight distinct types of concerning facial asymmetries, the recurring theme emphasizes the importance of distinguishing between normal anatomical variation and pathological changes that require professional intervention. From sudden onset facial drooping that may indicate stroke or Bell's palsy to progressive jaw deviation suggesting temporomandibular joint disorders, each type of asymmetry provides valuable diagnostic clues about underlying health conditions that may otherwise go unrecognized until they reach advanced stages. The multidisciplinary nature of facial asymmetry evaluation highlights the complex interplay between various medical specialties, including neurology, ophthalmology, oral and maxillofacial surgery, endocrinology, and plastic surgery, emphasizing the need for comprehensive assessment and coordinated care. Early recognition and prompt medical evaluation can significantly impact treatment outcomes, prevent complications, and improve both functional and aesthetic results for patients experiencing these conditions. Healthcare providers and patients alike must maintain heightened awareness of facial changes, understanding that while minor asymmetries are normal, sudden onset changes, progressive worsening, or asymmetries accompanied by functional impairments warrant immediate professional evaluation. The psychological and social implications of facial asymmetry cannot be overlooked, as these conditions often significantly impact patients' self-esteem, social interactions, and overall quality of life, making timely and appropriate treatment essential for comprehensive patient care. By fostering greater understanding of these warning signs and promoting early intervention, we can improve outcomes for individuals affected by these conditions and ensure that serious underlying pathology is identified and treated before irreversible complications occur.