15 Nose and Nasal Skin Changes Associated With Rosacea and Autoimmune Conditions
# 15 Nose and Nasal Skin Changes Associated With Rosacea and Autoimmune Conditions: A Comprehensive Guide
The nose, prominently positioned at the center of our face, serves as more than just a respiratory organ—it functions as a diagnostic window into our overall health, particularly when examining inflammatory and autoimmune conditions. Rosacea and various autoimmune disorders frequently manifest their earliest and most distinctive signs through characteristic changes in nasal and perinasal skin. These manifestations range from subtle vascular alterations to dramatic structural modifications that can significantly impact both appearance and function. Understanding the intricate relationship between nasal skin changes and systemic conditions is crucial for healthcare providers, as early recognition can lead to prompt diagnosis and treatment, potentially preventing progression to more severe complications. The nose's rich vascular supply, combined with its exposure to environmental factors and its unique anatomical structure, makes it particularly susceptible to inflammatory processes. This comprehensive exploration will examine fifteen distinct nasal and perinasal skin changes associated with rosacea and autoimmune conditions, providing healthcare professionals and patients with essential knowledge for recognition, understanding, and management of these often interconnected manifestations.
1. Persistent Erythema and Vascular Dilation
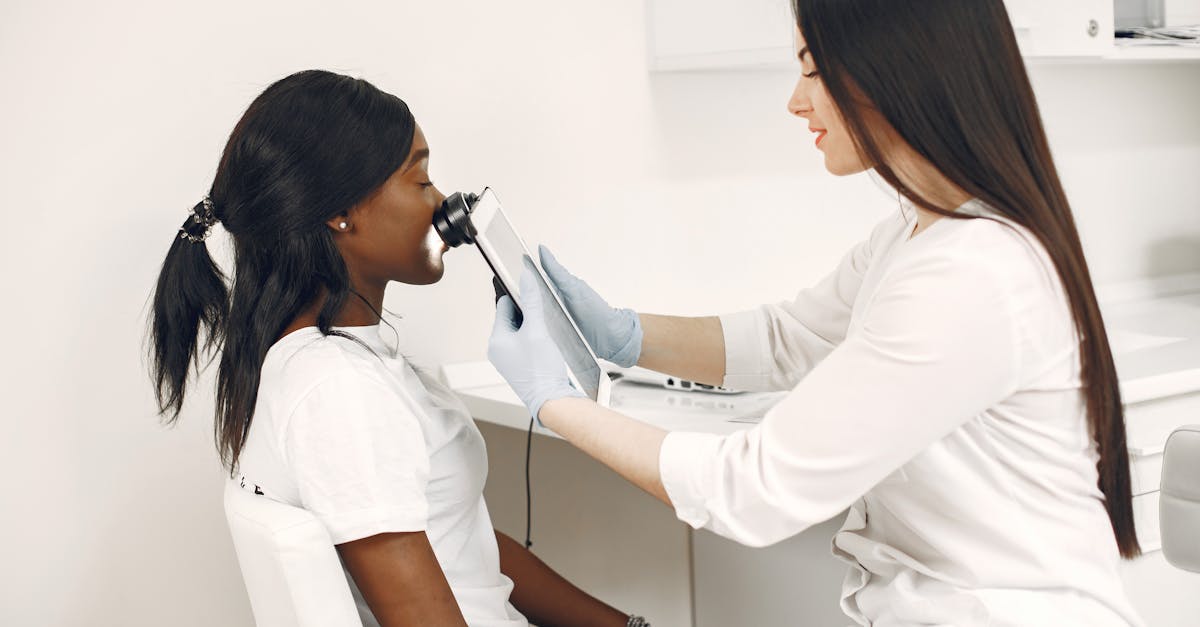
Persistent erythema, characterized by chronic redness of the nasal skin, represents one of the most common and earliest manifestations of both rosacea and certain autoimmune conditions. This persistent redness occurs due to chronic vasodilation of the superficial capillaries and venules within the nasal skin, creating a characteristic flushed appearance that distinguishes it from temporary redness caused by environmental factors or emotions. In rosacea, this erythema typically begins on the central nose and may extend to the nasal alae and surrounding areas, often accompanied by a burning or stinging sensation. The underlying pathophysiology involves dysregulation of the neurovascular system, increased expression of inflammatory mediators such as tumor necrosis factor-alpha and interleukin-1, and abnormal responses to normal stimuli including temperature changes, certain foods, or stress. In autoimmune conditions like systemic lupus erythematosus, the erythema may present as part of the classic malar rash, extending across the nasal bridge and cheeks in a butterfly pattern. The persistence of this redness, lasting weeks to months without resolution, helps differentiate pathological erythema from benign causes and warrants further investigation for underlying inflammatory or autoimmune processes.
2. Telangiectasia Formation and Vascular Proliferation
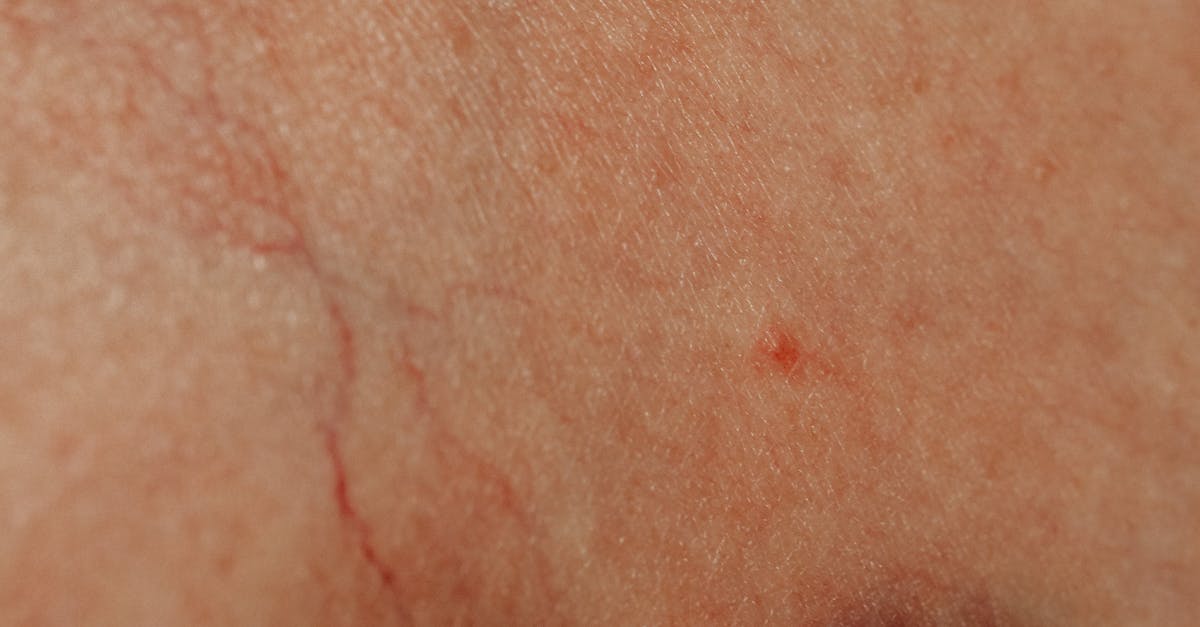
Telangiectasias, or dilated superficial blood vessels visible through the skin, frequently develop on the nose in patients with rosacea and certain autoimmune conditions, creating a characteristic spider-like or branching pattern of red or purple lines. These permanently dilated capillaries result from chronic inflammation and repeated cycles of vasodilation and vasoconstriction that ultimately damage the vessel walls and supporting connective tissue. In rosacea, telangiectasias typically appear on the nasal alae, tip, and dorsum, often becoming more prominent with disease progression and repeated inflammatory episodes. The development of these vascular changes involves multiple factors including genetic predisposition, environmental triggers, and inflammatory mediators that compromise the structural integrity of the microvasculature. In autoimmune conditions such as systemic sclerosis or dermatomyositis, telangiectasias may appear as part of a broader pattern of vascular involvement, often accompanied by other signs of microvascular disease. The presence of telangiectasias on the nose can significantly impact patients' quality of life due to cosmetic concerns, and their recognition is important for staging disease severity and monitoring treatment response. Advanced cases may require specialized treatments including laser therapy or intense pulsed light to address the cosmetic and functional implications of these vascular changes.
3. Papulopustular Eruptions and Inflammatory Lesions
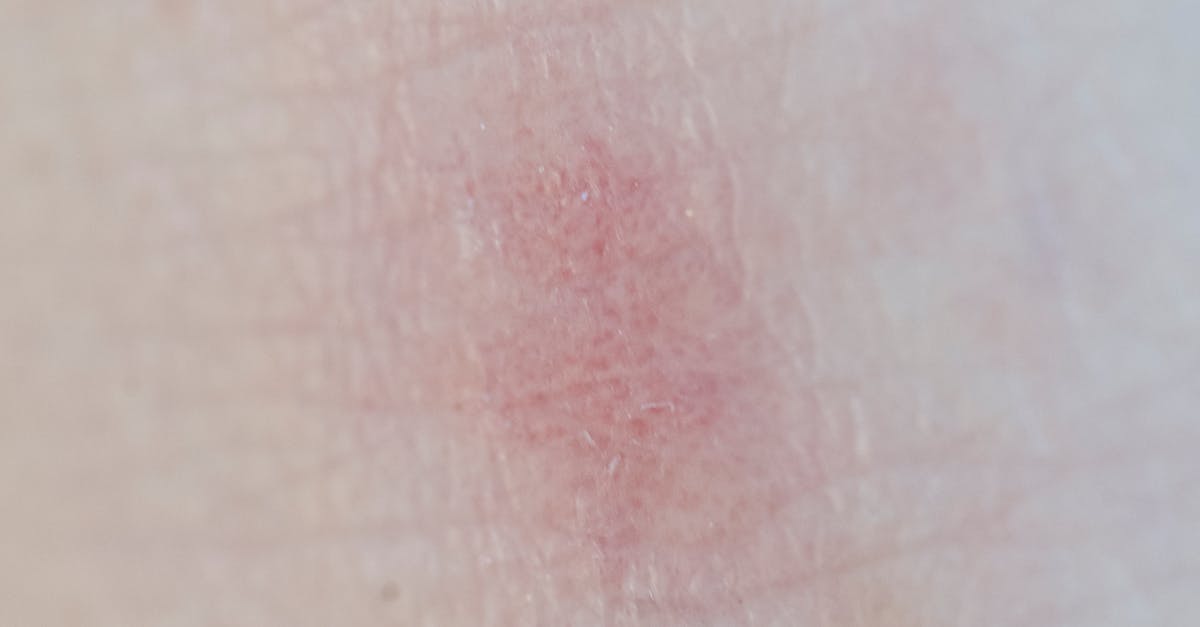
Papulopustular eruptions on the nose represent a more advanced stage of rosacea and can occasionally occur in certain autoimmune conditions, characterized by the development of inflammatory papules and pustules that distinguish this presentation from simple vascular rosacea. These lesions typically appear as small, red, dome-shaped bumps that may contain pus, often accompanied by surrounding erythema and edema that can cause significant discomfort and cosmetic concern. Unlike acne vulgaris, rosacea-associated papulopustular lesions lack comedones and tend to occur in a more central facial distribution, particularly affecting the nose, cheeks, and forehead in adults over thirty years of age. The pathogenesis involves a complex interplay of factors including abnormal innate immune responses, particularly involving toll-like receptor 2 activation, increased production of antimicrobial peptides like cathelicidin, and potential involvement of Demodex folliculorum mites that may trigger inflammatory responses. In some autoimmune conditions, similar papulopustular eruptions may occur as part of drug-induced lupus or as a manifestation of Behçet's disease, requiring careful differential diagnosis. The inflammatory nature of these lesions often responds to topical or systemic anti-inflammatory treatments, but proper identification and management are essential to prevent scarring and persistent inflammation that can lead to permanent textural changes in the nasal skin.
4. Rhinophyma and Progressive Nasal Enlargement
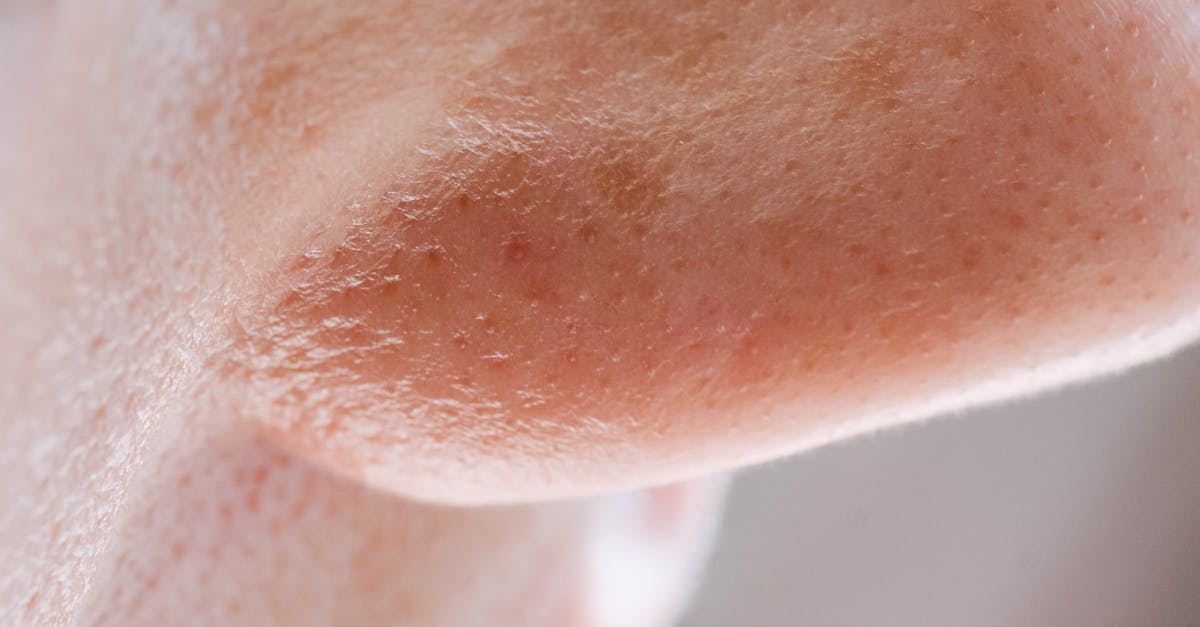
Rhinophyma represents the most severe and disfiguring manifestation of rosacea, characterized by progressive enlargement and distortion of the nose due to chronic inflammation, sebaceous gland hyperplasia, and connective tissue proliferation. This condition predominantly affects middle-aged to older men and develops through years of untreated or inadequately managed rosacea, progressing from simple erythema and telangiectasias to irreversible structural changes. The affected nose becomes bulbous, with a lobulated surface texture, prominent pores, and a characteristic "strawberry" or "potato" appearance that can significantly impact breathing function and psychological well-being. The pathophysiology involves chronic inflammation leading to fibroblast activation, increased collagen production, sebaceous gland hyperplasia, and vascular proliferation, creating the characteristic thickened, irregular nasal contour. While rhinophyma is primarily associated with rosacea, similar nasal enlargement can occasionally occur in other inflammatory conditions or as a result of chronic lymphedema in certain autoimmune disorders. The condition requires surgical intervention for correction, with various techniques including dermabrasion, laser resurfacing, electrosurgery, and excisional procedures available depending on the severity and extent of involvement. Early recognition and treatment of rosacea can prevent progression to this advanced stage, emphasizing the importance of prompt diagnosis and appropriate management of initial symptoms.
5. Nasal Vestibulitis and Mucosal Involvement
Nasal vestibulitis, characterized by inflammation and irritation of the nasal vestibule and anterior nasal cavity, frequently occurs in patients with rosacea and certain autoimmune conditions, presenting as crusting, fissuring, and painful erosions at the nasal entrance. This condition involves the transition zone between the external nasal skin and the internal mucosal lining, an area particularly susceptible to irritation from environmental factors, mechanical trauma, and inflammatory processes. In rosacea patients, nasal vestibulitis often accompanies facial symptoms and may be exacerbated by the same triggers that worsen cutaneous manifestations, including certain skincare products, environmental irritants, and stress. The inflammatory process can lead to secondary bacterial colonization, particularly with Staphylococcus aureus, creating a cycle of infection and inflammation that perpetuates symptoms. In autoimmune conditions such as granulomatosis with polyangiitis (formerly Wegener's granulomatosis), nasal vestibulitis may represent early mucosal involvement that can progress to more serious complications including septal perforation and saddle nose deformity. The management of nasal vestibulitis requires gentle cleansing, appropriate moisturization, and sometimes topical or systemic antimicrobial therapy, while addressing underlying inflammatory conditions is essential for preventing recurrence and complications.
6. Sebaceous Hyperplasia and Glandular Changes

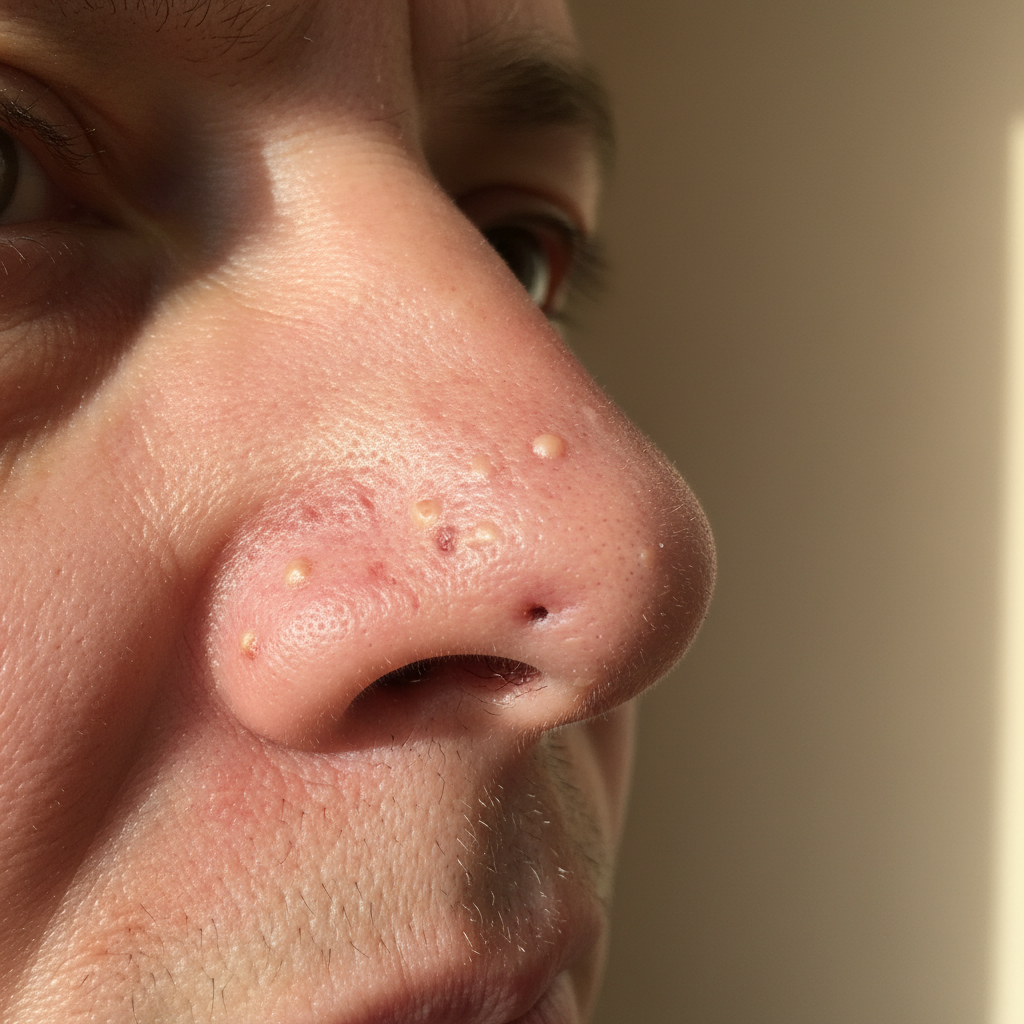
Sebaceous hyperplasia of the nasal skin represents a common finding in patients with rosacea and certain autoimmune conditions, characterized by enlarged sebaceous glands that create small, yellowish, dome-shaped papules with central umbilication. These benign growths result from the proliferation of sebaceous gland tissue in response to chronic inflammation, hormonal influences, and genetic predisposition, particularly affecting the nose where sebaceous glands are naturally more numerous and larger. In rosacea, sebaceous hyperplasia often accompanies other inflammatory changes and may contribute to the overall textural irregularities and cosmetic concerns associated with the condition. The enlarged glands can become more prominent with age and continued inflammatory stimulation, sometimes requiring differentiation from other conditions such as basal cell carcinoma or sebaceous adenoma. The pathophysiology involves increased sebocyte proliferation and altered sebaceous gland architecture in response to inflammatory mediators, particularly in areas of chronic erythema and vascular changes. In some autoimmune conditions, particularly those involving chronic inflammation or immunosuppressive therapy, sebaceous hyperplasia may develop as a secondary phenomenon. Treatment options include topical retinoids to normalize gland function, laser therapy for cosmetic improvement, and addressing underlying inflammatory conditions to prevent further glandular changes. Recognition of sebaceous hyperplasia is important for comprehensive management of nasal skin changes and patient counseling regarding realistic treatment expectations.
7. Phymatous Changes and Tissue Proliferation
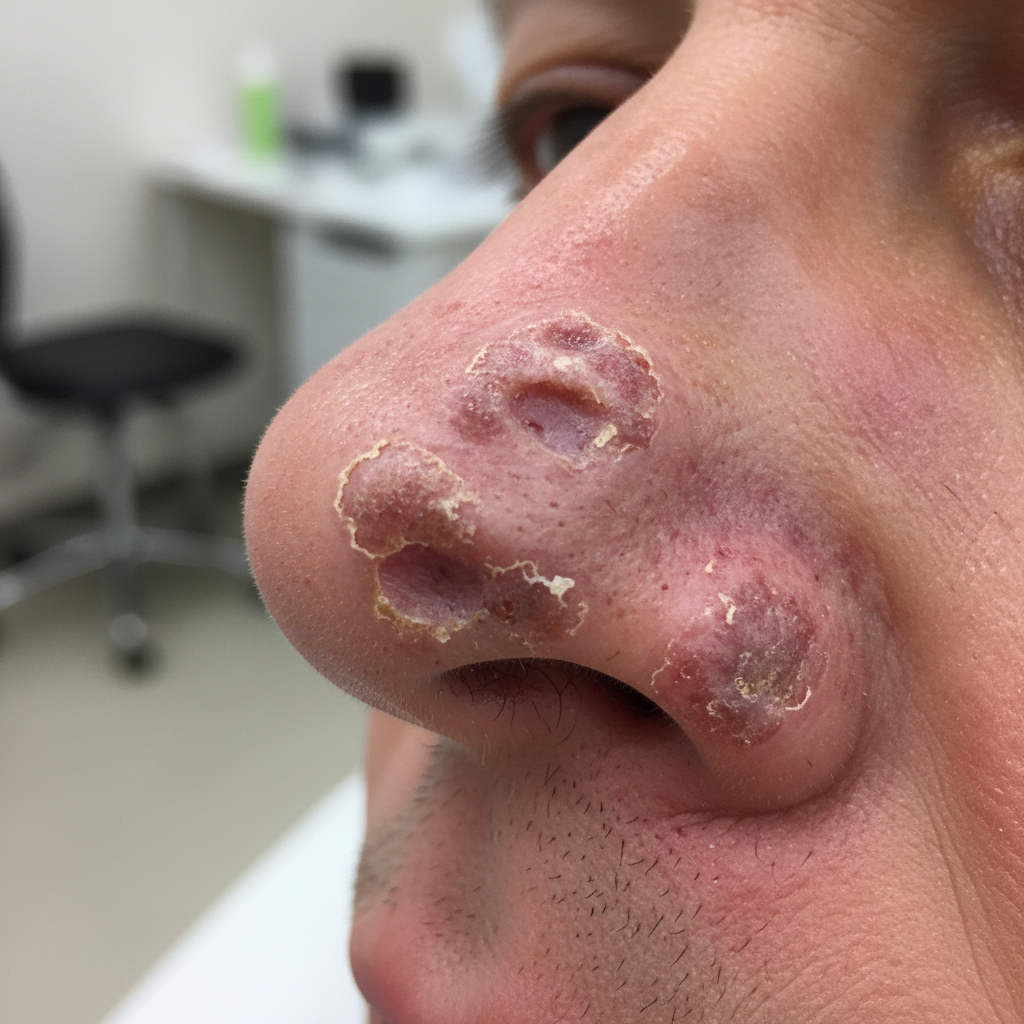
Phymatous changes represent advanced manifestations of rosacea characterized by progressive tissue thickening, irregular surface texture, and nodular proliferation that can affect various areas of the nose beyond the classic rhinophyma presentation. These changes involve hyperplasia of sebaceous glands, connective tissue proliferation, chronic inflammation, and vascular changes that combine to create characteristic lobulated, thickened skin with prominent follicular openings. While rhinophyma affecting the nasal tip and alae is the most recognized form, phymatous changes can also involve the nasal dorsum, sidewalls, and perinasal areas, creating asymmetric distortion and functional impairment. The development of phymatous changes typically occurs over years to decades of chronic inflammation, often in patients with inadequately treated or severe rosacea, and predominantly affects men over forty years of age. The underlying pathophysiology involves dysregulation of the extracellular matrix, increased collagen synthesis, sebaceous gland hyperplasia, and chronic inflammatory cell infiltration that leads to progressive tissue remodeling. In rare cases, similar phymatous changes may occur in other chronic inflammatory conditions or as a result of chronic lymphatic obstruction in certain autoimmune disorders. Early intervention with appropriate anti-inflammatory therapy can potentially slow or prevent progression to phymatous changes, while established lesions typically require surgical management including laser resurfacing, dermabrasion, or excisional techniques to restore normal nasal contour and function.
8. Lupus-Associated Nasal Lesions and Malar Involvement
Systemic lupus erythematosus frequently manifests with characteristic nasal and perinasal skin changes that can significantly impact diagnosis and disease monitoring, most notably the classic malar rash that extends across the nasal bridge and cheeks in a butterfly distribution. This distinctive eruption typically spares the nasolabial folds and presents as erythematous, sometimes scaly patches that may be photosensitive and can range from subtle pink discoloration to intense, edematous plaques. The nasal involvement in lupus often includes the nasal bridge, dorsum, and sometimes the nasal tip, creating a characteristic pattern that helps differentiate lupus from other inflammatory conditions affecting the face. Histopathologically, lupus-associated nasal lesions demonstrate interface dermatitis with basal cell vacuolization, dermal mucin deposition, and perivascular lymphocytic infiltration that can be confirmed through skin biopsy when diagnosis is uncertain. In some patients, nasal lesions may present as discoid lupus erythematosus with well-demarcated, scaly plaques that can lead to scarring and permanent pigmentary changes if left untreated. The photosensitive nature of many lupus-associated nasal lesions emphasizes the importance of sun protection and may help explain the predilection for sun-exposed areas like the nose. Additionally, lupus patients may develop nasal mucosal ulcerations, particularly in the setting of active systemic disease, which can cause pain, crusting, and potential complications including septal perforation in severe cases.
9. Autoimmune Bullous Disease Nasal Manifestations

Autoimmune bullous diseases, including pemphigus vulgaris, bullous pemphigoid, and mucous membrane pemphigoid, can present with distinctive nasal manifestations that range from subtle mucosal erosions to dramatic blistering and scarring that significantly impacts both function and appearance. These conditions involve autoantibodies directed against structural proteins of the skin and mucous membranes, leading to loss of cellular adhesion and subsequent blister formation that can affect the nasal vestibule, external nasal skin, and internal nasal mucosa. In pemphigus vulgaris, nasal involvement often presents as painful erosions and crusting within the nasal vestibule and anterior nasal cavity, frequently preceding cutaneous manifestations and serving as an early diagnostic clue. The fragile nature of pemphigus blisters means that intact bullae are rarely seen, with patients typically presenting with erosions, crusts, and areas of denuded epithelium that heal slowly and may become secondarily infected. Mucous membrane pemphigoid can cause particularly severe nasal complications, including progressive scarring that may lead to nasal stenosis, synechiae formation, and functional impairment of breathing and smell. The diagnosis of autoimmune bullous disease affecting the nose requires careful clinical evaluation, often supplemented by skin or mucosal biopsy with direct immunofluorescence studies to identify characteristic autoantibody deposits. Treatment typically involves systemic immunosuppressive therapy to control the autoimmune process, along with supportive care to prevent secondary infection and minimize scarring that could compromise nasal function.
10. Vasculitic Nasal Changes and Systemic Involvement
Systemic vasculitis can produce dramatic and potentially devastating nasal changes that serve as important diagnostic markers and indicators of disease activity, particularly in conditions such as granulomatosis with polyangiitis, eosinophilic granulomatosis with polyangiitis, and microscopic polyangiitis. These conditions involve inflammation of blood vessels that can affect the nasal mucosa, cartilage, and surrounding tissues, leading to a spectrum of manifestations ranging from chronic rhinosinusitis to complete nasal destruction. Granulomatosis with polyangiitis, formerly known as Wegener's granulomatosis, classically presents with upper respiratory tract involvement including chronic nasal congestion, bloody nasal discharge, crusting, and progressive destruction of nasal cartilage that can result in saddle nose deformity. The inflammatory process in vasculitic conditions involves necrotizing inflammation of small to medium-sized vessels, often accompanied by granulomatous inflammation that can destroy normal tissue architecture and lead to irreversible structural damage. Early nasal manifestations may include persistent rhinosinusitis, nasal crusting, epistaxis, and anosmia, which can precede systemic manifestations by months to years, emphasizing the importance of recognizing these early signs. The diagnosis of vasculitic nasal involvement requires a high index of suspicion, often supported by tissue biopsy demonstrating characteristic histopathologic features, serologic testing for antineutrophil cytoplasmic antibodies (ANCA), and comprehensive evaluation for systemic involvement. Prompt recognition and treatment with appropriate immunosuppressive therapy are essential to prevent irreversible nasal destruction and associated functional impairment.
11. Sarcoidosis and Granulomatous Nasal Infiltration
Sarcoidosis, a multisystem granulomatous disorder of unknown etiology, can present with distinctive nasal manifestations that may be among the earliest signs of systemic disease, characterized by granulomatous infiltration of nasal tissues that can cause both functional and cosmetic concerns. The nasal involvement in sarcoidosis typically presents as chronic nasal congestion, crusting, epistaxis, and sometimes visible external nasal lesions that appear as violaceous or erythematous papules, plaques, or nodules. These lesions result from the formation of non-caseating granulomas within the nasal mucosa and skin, composed of epithelioid cells, giant cells, and lymphocytes that create characteristic inflammatory infiltrates visible on histopathologic examination. The granulomatous inflammation can affect various structures within the nose, including the nasal mucosa, turbinates, septum, and external nasal skin, potentially leading to nasal obstruction, anosmia, and structural changes if left untreated. Lupus pernio, a specific form of chronic cutaneous sarcoidosis, has a predilection for the nose and can cause significant disfigurement through chronic granulomatous inflammation that creates violaceous, indurated plaques with a characteristic appearance. The diagnosis of nasal sarcoidosis requires correlation of clinical findings with histopathologic evidence of non-caseating granulomas, often supported by elevated serum angiotensin-converting enzyme levels, abnormal chest imaging, and exclusion of other granulomatous conditions. Treatment typically involves topical or systemic corticosteroids, with additional immunosuppressive agents sometimes required for refractory cases or to minimize steroid-related side effects.
12. Dermatomyositis Perinasal and Heliotrope Changes

Dermatomyositis, an inflammatory myopathy with characteristic cutaneous manifestations, frequently involves the perinasal area as part of its distinctive facial eruption, creating diagnostic clues that can facilitate early recognition and treatment of this potentially serious autoimmune condition. The perinasal involvement in dermatomyositis often presents